Research Article
Relevance of a Persistent Descending Mesocolon to Sigmoid Volvulus
Atsushi Tsuruta1*, Yusaku Watanabe1, Yasuo Oka1, Minoru Fujita2, Hiroshi Matsumoto2, Yoshinori Fujiwara1, Akiko Shiotani2 and Tomio Ueno1
1Department of Digestive Surgery, Kawasaki Medical School, Japan
2Department of Internal Medicine, Kawasaki Medical School, Japan
*Corresponding author: Atsushi Tsuruta, Department of Digestive Surgery, Kawasaki Medical School, Japan
Published: 01 Nov, 2018
Cite this article as: Tsuruta A, Watanabe Y, Oka Y, Fujita
M, Matsumoto H, Fujiwara Y, et al.
Relevance of a Persistent Descending
Mesocolon to Sigmoid Volvulus. Clin
Surg. 2018; 3: 2188.
Abstract
Purpose: Sigmoid Volvulus (SV) causes acute abdomen, but its mechanism of torsion still remains
unknown. Persistent Descending Mesocolon (PDM) is a congenital anomaly where the primitive
dorsal mesocolon fails to fuse with the parietal peritoneum in the 4th to the 5th month of gestation.
We evaluated the association of PDM with SV.
Materials and Methods: We conducted a retrospective study of 45 consecutive patients (male:
female=36:9, median age=77.8 years old) with SV who were treated at our hospital between 2009-
2016. Relationships among computed tomography findings (Coffee Bean sign (CB), Bird Beak sign
(BB), Whirl Sign (WS), and PDM), anamnesis, a history of endoscopic treatment, and grading of
pathological findings were analyzed.
Results: The ratio of PDM in SV cases was higher compared with the usual frequency of occurrence.
With regard to the grade of pathological findings, Univariate analysis showed significant differences
in PDM and the number of endoscopic treatments. Multivariate analysis showed that only PDM
was an independent factor for a low grading of inflammation of the colon.
Conclusion: PDM may be one of the causes of SV and should be one of determining factors of
surgery for SV.
Keywords: Sigmoid volvulus; Persistent descending mesocolon; Coffee bean sign; Bird beak
sign; Whirl sign
Introduction
The incidence of sigmoid volvulus (SV) is the largest number in volvulus of the gastrointestinal
tract [1]. The ratio of men to women with SV is 1.4 to 1 and the average age is 68 years old [2]. The
causes of SV are chronic fecal overloading and elongation of the sigmoid colon [3]. The predisposing
factors for formation of volvulus are an abnormally long, large intestine and a narrow mesentery
[4-6]. However, the etiology or mechanism of pathogenesis of SV still remains unclear. Congenital,
as well as acquired factors could become reasons for torsion [2].
The diagnosis of SV may not be difficult by plain abdominal radiography findings with a “Coffee
Bean Sign (CB)”. Computed Tomography (CT) scan findings sometimes provide impressive images
of “Whirl Sign (WS)” and “Bird’s Beak Sign (BB)” [7,8].
Persistent mesocolon is an embryological anomaly that occurs during the final process of
intestinal development in organogenesis. This condition is associated with an absence of fusion
between the descending or ascending colon mesentery and posterior, lateral parietal peritoneum.
Persistent mesocolon appears after 5 months of gestation during the developmental process [9].
Persistent Descending Mesocolon (PDM) develops as a result of failure of the primitive dorsal
mesocolon to fuse with the parietal peritoneum in the 5th month of gestation [10]. In the 1960s,
this abnormality was reported in the fields of radiology and gynecology [11,12]. A previous study
reported that the incidence of PDM confirmed in laparoscopic colorectal surgery was 2.4% (13/543)
at a representative Japanese cancer institute [13]. In our previous literature survey, only two case
reports described the relevance of PDM to SV [14,15]. Therefore, the present study aimed to
determine how the presence of PDM affects the occurrence of SV.
Materials and Methods
A total of 45 patients who were diagnosed and underwent treatment for SV in Kawasaki
Medical School Hospital from January 2000 to September 2016 were
investigated. Patients who did not undergo CT in clinical diagnosis
were excluded from the present study. This was a retrospective chart
review of a prospectively maintained database. The institutional
review boards of the Kawasaki Medical School approved the study
protocol.
Diagnosis
All of the patients were diagnosed based on clinical symptoms
together with blood tests, a plain abdominal radiograph, and CT scan
findings. Plain abdominal radiographs showed a CB, and abdominal
CT scans showed a WS and a BB in cases of acute abdominal
obstruction. PDM was diagnosed by the coronal plane or transverse
plane of CT scans. The CT findings showed that descending colon or
Sigmoid-Descending junction (SD junction) shifted to the midline as
a result of absence of fusion between the descending colon mesentery
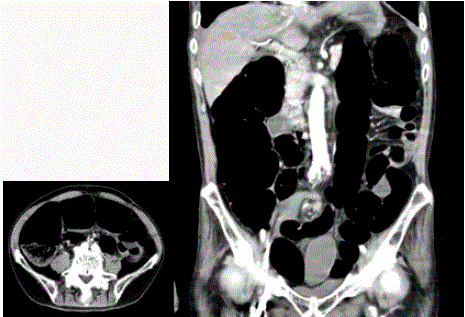
and posterior lateral parietal peritoneum. Figure 1 shows a case of 72
years-old male who was diagnosed as sigmoid volvulus having PDM.
Grading of inflammation by histopathological findings
Histological diagnosis was performed with all resected species.
Moreover, grading of inflammation was performed depending on
the degree of inflammation. We defined grading of inflammation
as follows. Grade 1 (G1) was no inflammation or a microcirculatory
disorder. Grade 2 (G2) was a mild ischemic change. Grade 3 (G3)
was a severe ischemic change or necrotic change. We categorized all
patients who underwent endoscopic therapy as G1 inflammation.
Patients who had more than G2 inflammation were regarded as cases
with a surgical indication.
Statistical analysis
Results are reported as mean ± SD. We used the chi-square test
and t-test for analysis. Multivariate analysis was performed using
logistic regression. Statistical significance was defined as a p value
<0.05. All analyses were performed using JMP software version 11.2
(SAS Institute, Inc., Cary, NC).
Figure 1
Figure 1
A case of sigmoid volvulus with PDM.
Abnormal dilatation of bowel was recognized (A). Entire descending colon
was shifted to the midline (B).
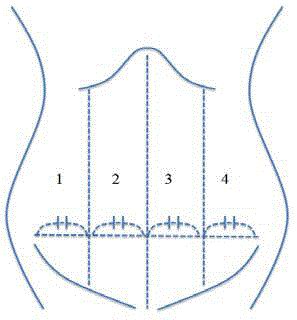
Figure 2
Figure 2
Four division of abdomen.
We studied which site WS or BB appeared in the coronal plane of CT scans
and divided the coronal image of CT into four parts.
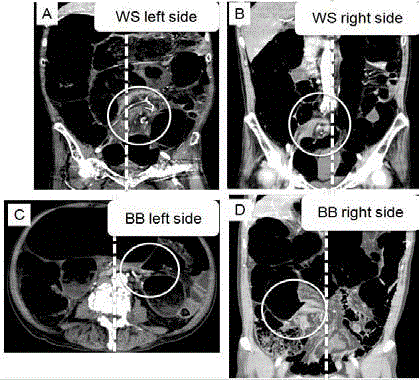
Figure 3
Figure 3
Positional relationship of whirl sign (WS) and bird’s beak sign (BB)
in abdominal CT.
WS placed in left side (A) and right side (B) in abdominal CT findings. BB
placed in left side (C) and right side (D) in abdominal CT findings.
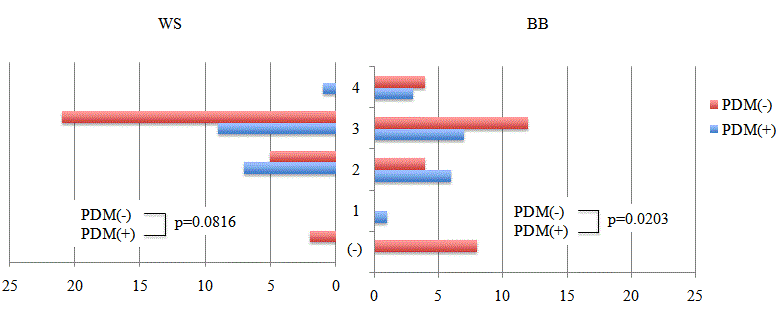
Figure 4
Figure 4
Frequency and localization of WS and BB.
WS and BB tended to be found in the left side of the abdomen. However,
in the PDM-positive (PDM(+)) group, WS and BB were observed more
frequently in the right side of the abdomen than in the left side compared with
the PDM negative (PDM(-)) group.
Results
Forty-five patients underwent endoscopic or surgical treatment
for SV during the study period. The ratio of males to females was 36
to 9. The median age of patients was 77.8 (47-97) years old. (Table
1) shows the patients’ characteristics. Preoperative representative
radiological findings showed that the ratios of CB, WS, and BB were
97.8% (44/45), 95.8% (43/45), and 82.2% (37/45), respectively. The
ratio of a PDM was 37.8% (17/45), which was much higher than that
reported previously [13]. The number of endoscopic treatment for SV
was as follows: one was 15 cases, two were two cases, three were six
cases, and four were three cases. The mean number of endoscopic
treatment was 1.10 ± 1.28. During the study, surgical intervention was
performed in 66.7% (30/45) of patients; in who open sigmoidectomy
was performed in nine, the open Hartmann procedure in 20, and
laparoscopic sigmoidectomy in one. For the grade of inflammation,
grade 1 was observed in 33 (73.3%) patients, grade 2 in (20.0%) seven,
and grade 3 in five (11.1%, Table 1).
Localization of WS, BB, and presence of PDM
We studied which site WS or BB appeared in the coronal plane
of CT scans. We divided the coronal image of CT into four parts
(Figure 2). Figure 3 shows the positional relationship of WS and BB
in abdominal CT.WS and BB tended to be found in the left side of the
abdomen. However, in the PDM-positive (PDM(+)) group, WS and
BB were observed more frequently in the right side of the abdomen
than in the left side compared with the PDM negative (PDM(-))
group (Figure 4). The presence of PDM would have possibility that
WS and BB could not occur in the left side of abdomen.
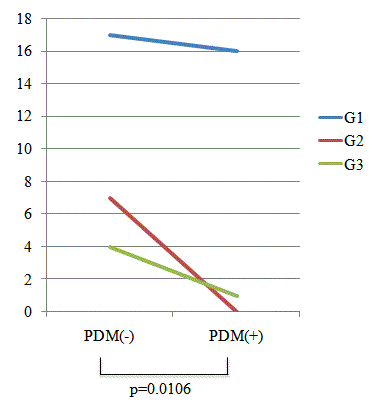
PDM and grading of inflammation
The causal relation between PDM and the grading of inflammation
was studied. In the PDM (-) group, G1 was observed in 17 patients,
G2 in seven, and G3 in four. In the PDM (+) group, G1 was observed
in 16 patients, G3 in one, and G2 in none. As a result, the grading of
inflammation in the PDM (+) group was significantly lower than that
in the PDM (-) group (p=0.0106) (Figure 5).
PDM and indication for surgery
We defined the Absolute Indication for Surgery (AIS) as grading
of inflammation greater than grade 2. Namely, AIS (-) meant relative
indication or maladaptation for surgery and indicated G1 as grading
inflammation. Moreover, AIS (+) indicated G2 or G3. Univariate
analysis showed that the number of endoscopic therapies (p=0.013)
and PDM (p=0.014) were significantly associated with AIS (Table 2).
In multivariate analysis, the presence of PDM was associated with
decreased odds of AIS (Table 3).
Figure 5
Figure 5
Causal relationship between PDM and grading of inflammation.
The causal relation between PDM and the grading of inflammation was
studied. In the PDM(-) group, G1 was observed in 17 patients, G2 in seven,
and G3 in four. In the PDM(+) group, G1 was observed in 16 patients, G3 in
one, and G2 in none. As a result, the grading of inflammation in the PDM(+)
group was significantly lower than that in the PDM(-) group (p=0.0106).
Table 1
Table 2
Table 3
Discussion
The present study is the first to report the association between SV
and PDM. In most cases of PDM, a descending or proximal sigmoid
colon is not adhered to the parietal peritoneum and a thin ligament
often exists between them. As a result, the left-sided colon is shifted
to the midline and an unusual mesenteric adhesion sometimes arises
between the mesocolon and mesentery. In our study, the incidence
of PDM in SV cases was more than 15 times that previously reported
[13]. Moreover, two case reports described that volvulus might occur
when PDM was present [14,15]. Therefore, PDM could be one of
the risk factors for SV. SV is defined as a twisting or rotation of the
sigmoid colon and mesocolon, leading to large bowel obstruction.
CB, BB, and WS are a typical clinical trial of SV. CB is shown in
plain radiographs of the abdomen and indicates that upstream and
downstream of an expanded sigmoid colon are in a horizontal line.
BB and WS are shown in abdominal CT scans and indicate twisting
of the bowel. These two signs appeared in the midline of body
(Figure 4). WS and BB in the right side of the body were observed
significantly more frequently in the PDM (+) group than in the
PDM (-) group. In the presence of PDM, the whole sigmoid colon
is often positioned towards the right side rather than the left side of
the abdomen. Furthermore, unusual adhesions by PDM sometimes
occur. Therefore, adhesions between the mesentery and mesocolon
sometimes occur in the left side of body and prevent twisting of the
sigmoid colon in the left side of the body. We considered that these
adhesions would affect grading of inflammation of the sigmoid colon.
Therefore, adhesion might make torsion incomplete. This possibility
was indicated by our finding that the grade of inflammation in the
PDM (+) group was significantly lower than that in the PDM (-)
group (Figure 5). Additionally, multivariate analysis showed that
patients with SV and PDM often recovered by endoscopic therapy,
and not surgery. Therefore, patients with PDM who underwent
surgery for SV were determined to have more of a relative indication
than absolute indication.
This study has limitations that are inherent to a retrospective
medical record review obtained at a single institution. More cases
need to be studied in the future. Further prospective studies on PDM
will hopefully identify an appropriate marker to provide information
that is useful for deciding the line of treatment of SV.
Conclusion
The association of PDM to SV, as proposed in this study, could be useful information for future treatment policies.
References
- Kabara JJ, Riggin RM, Kissinger PT. Abnormal levels of urinary catecholamines in dystrophic mice and hamsters. Proc Soc Exp Biol Med. 1976;151(1):168-72.
- Peña AS, Lems-van Kan PH, Kuiper I, van Duijn W, Lamers CB. Measurement of mucosa-specific antibodies against gliadin by a sensitive technique using the biotin-streptavidin system. Acta gastro-enterologicaBelgica.1986;49(4):423-26.
- Tegegne A. Cultural bowel patterns and sex difference in sigmoid volvulus morbidity in an Ethiopian hospital. Trop Geogr Med. 1995;47(5):212-15.
- Alatise OI, Ojo O, Nwoha P, Omoniyi-Esan G, Omonisi A. The role of the anatomy of the sigmoid colon in developing sigmoid volvulus: a cross-sectional study. Surg Radiol Anat. 2013;35(3):249-57.
- Grigg MM, Costanzo-Nordin MR, Celesia GG, Kelly MA, Silver MA, Sobotka PA, et al. The etiology of seizures after cardiac transplantation. Transplant Proc.1988;20(3):937-44.
- Bhatnagar BN, Sharma CL, Gupta SN, Mathur MM, Reddy DC. Study on the anatomical dimensions of the human sigmoid colon. Clin Anat. 2004;17(3):236-43.
- Fisher JK. Computed tomographic diagnosis of volvulus in intestinal malrotation. Radiology. 1981; 140(1):145-46.
- Levsky JM, Den EI, DuBrow RA, Wolf EL, Rozenblit AM. CT findings of sigmoid volvulus. AJR Am J Roentgenol. 2010;194(1):136-43.
- Balthazar EJ. Congenital positional anomalies of the colon: radiographic diagnosis and clinical implications. II. Abnormalities of fixation. Gastrointest Radiol. 1977;2(1):49-56.
- Tsuruta A, Kawai A, Oka Y, Okumura H, Matsumoto H, Hirai T, et al. Laparoscopic right hemicolectomy for ascending colon cancer with persistent mesocolon. World J Gastroenterol. 2014;20(18): 5557-60.
- Popky GL, Lapayowker MS. Persistent descending mesocolon. Radiology. 1966;86(2):327-31.
- Morgenstern L. Persistent descending mesocolon. Surg Gynecol Obstet. 1960;110:197-202.
- Okada I, Yamaguchi S, Kondo H, Suwa H, Tashiro J, Ishii T. Laparoscopic colectomy for persistent descending mesocolon: an experience of 13 patients. J Jpn Soc Endosc Surg. 2013;18:459-64 (Japanese).
- Shetty P, Nayak SB. Absence of transverse colon, persistent descending mesocolon, displaced small and large bowels: a rare congenital anomaly with a high risk of volvulus formation. Anat Cell Biol. 2014;47(4):279-81.
- Chen A, Yang FS, Shih SL, Sheu CY. Case report. CT diagnosis of volvulus of the descending colon with persistent mesocolon. AJR Am J Roentgenol. 2003;180(4):1003-6.