Research Article
Inflow Modulation in Adult Living Donor Liver Transplant to Reduce Risk of Small-for-Size Syndrome (SFSS)
Ling XS1, Koh YX1,2*, Teo JY1,2, Goh BKP1,2, Lee SY1,2, Cheow PC1,2, Chung AYF1,2, Chan CY1,2 and Prema Raj J1,2
1Department of Hepatopancreatobiliary and Transplant Surgery, Singapore General Hospital, Singapore
2Duke NUS Medical School, Singapore
*Corresponding author: Koh Ye Xin, Department of Hepatopancreatobiliary and Transplant Surgery, Singapore General Hospital, Singapore
Published: 01 Nov, 2018
Cite this article as: Ling XS, Koh YX, Teo JY, Goh BKP,
Lee SY, Cheow PC. Inflow Modulation
in Adult Living Donor Liver Transplant
to Reduce Risk of Small-for-Size
Syndrome (SFSS). Clin Surg. 2018; 3:
2180.
Abstract
Small for Size Syndrome (SFSS) is a specific problem in Living Donor Liver Transplant (LDLT)
where the pathogenesis in SFSS seems to be primarily linked to graft over perfusion. Various
methods of modulating portal inflow to reduce excessive flow to the liver without compromising
liver function has been described. We report the outcome of 4 LDLT cases in which the portal inflow
was modulated by performing a splenectomy and a temporary hemi-portocaval shunt.
Keywords: Liver transplant; SFSS; LDLT; DDLT
Introduction
Living Donor Liver Transplantation (LDLT) is an increasingly common modality of liver
transplantation in the East due to shortage of cadaveric grafts [1]. Improvements to the selection and
safety of LDLT has been improved over the past decades, making the contemporary results of LDLT
comparable to deceased donor liver transplantation (DDLT) However, specific problems arising
from living donor liver transplant (LDLT), such as size mismatch between donor and recipient are
still significant challenges to overcome [2].
Small for Size Syndrome (SFSS) was recognised in the early days of LDLT where liver failure
was observed in patients who received small grafts relative to their body weight. A Small for Size
Graft (SFSG) was later defined as a liver graft with a Graft Weight Ratio (GWR) of <0.8 [3]. This
was a significant issue overcome as SFSS was reported to be as high as 40% in LDLT [4]. Sugawara
et al. [5] described the problems of SFSG in a series of 80 LDLT observing that hyperbilirubinemia
and prolonged Prothrombin Time (PT) persisted longer in the group with SFSG [5]. Subsequently,
SFSS was defined as graft dysfunction in the first postoperative week characterized by the presence
of hyperbilirubinemia, coagulopathy or ascites on 3 consecutive days [6]. Even though not fully
understood, pathogenesis of SFSS seems to be primarily linked to graft over perfusion [2]. Various
methods of modulating portal inflow to reduce excessive flow to the liver without compromising
liver function have been described. However, there is no consensus as to which method is superior
[3]. In our centre, our technique of choice to modulate the inflow of the grafts in ALDLT with
GWR <0.8 comprises of a splenectomy and a temporary hemi-portocaval shunt. Here, we report the
outcome of 4 ALDLT cases with inflow modulation as described above.
Patients and Methods
Recipients
From 2015 to 2017, we performed a total of 4 LDLT using liver grafts with a GWR <0.8 in a
single centre. All 4 recipients are male. Two patients had Non-Alcoholic Steatohepatitis (NASH)
related liver cirrhosis complicated with Hepatocellular Carcinoma (HCC), 1 patient had Hepatitis
B Virus (HBV) related liver cirrhosis complicated with HCC where the last patient had Hepatitis C
Virus (HCV) related liver cirrhosis complicated with HCC. All 4 patients had clinically significant
portal hypertension before transplant. After transplant, all donors were put on a standard protocol
of immunosuppressive agents comprising of Mycophenolate Mofetil (MMF), Basilixumab,
Tacrolimus and Prednisolone.
Grafts
Living donor right hepatectomy was performed for all 4 cases. In cases where the middle hepatic
vein was not harvested, reconstruction of the venous outflow for segments 5 and 8 was performed
with iliac vascular conduits. The actual graft weight was calculated for
all recipients. Graft characteristics are summarized in Table 1.
Surgical technique
All 4 recipients had a splenectomy and a temporary hemiportocaval
shunt created between the right branches of the portal
vein to the inferior vena cava. The hemi-portocaval shunt was ligated
after reconstitution of the graft hepatic venous outflow and portal
venous inflow. The portal pressure was measured before and after
portal inflow reconstruction. Hepatic artery reconstruction was
performed with end to end arterial anastomosis in all 4 recipients
under microscope by the plastic and reconstructive surgeons. Biliary
anastomosis was performed in an end-to-end fashion between the
donor and recipient bile ducts.
SFSS and encephalopathy
In our case series, we used the definition proposed by Dahm et
al. [7] for SFSS. Dahm et al. [7] proposed definition for small for size
dysfunction as dysfunction of a small partial liver graft (GWR <0.8%)
during the first postoperative week after the exclusion of other causes
like technical, immunological or infectious causes. Graft dysfunction
was defined as the presence of two of the following on three
consecutive days: bilirubin >100 μmol/l, INR >2, encephalopathy
grade 3 or 4.
Table 1
Figure 1
Results
Donors and grafts
All four donors recovered uneventfully, and no repeat
interventions were required. Length of Stay (LOS) for all donors
ranged from 6 to 8 days.
Outcomes of 4 recipients
Intraoperatively all liver grafts appeared well perfused with no
evidence of congestion after all anastomosis were completed. Portal
pressure measured before and after inflow modulation and completion
of anastomosis showed significant reduction. All 4 recipients were
discharged with a LOS ranging between 11-67 days. 1 patient had
complete thrombosis of the hepatic artery anastomosis and required
a re-operation for takedown of thrombosed arterial anastomosis
with re-do arterial anastomosis with left radial artery graft. He was
started on single agent anti-platelet and subsequently monitored with
ultrasound Doppler of the hepatic arterial anastomosis. No further
thrombosis occurred, and patient was discharged well.
Primary non-function of the liver graft did not occur in any
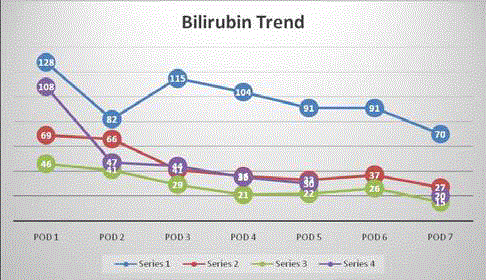
patients. Bilirubin was trended for the first postoperative week and
patients were observed clinically for development of encephalopathy
to detect early graft dysfunction and development of SFSS. All four
patients have down trending bilirubin as shown in Figure 1. None of
the recipients had encephalopathy.
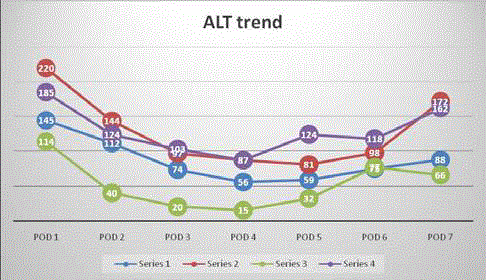
Acute biochemical rejection occurred in 3 patients, who presented
with elevated liver transaminases. They were otherwise clinically
asymptomatic. Liver biopsy performed in one patient showed features
consistent with acute rejection with a rejection activity index 5/9,
portal inflammation 2, bile duct inflammation damage 2 and venous
endothelial inflammation 1. Both acute rejection episodes were
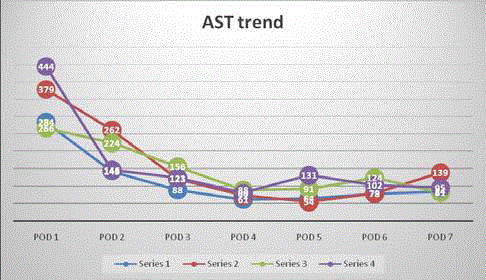
treated successfully with pulsed steroids. Trend of liver transaminases
is shown in Figure 2 and Figure 3. At the time of concluding our case
series, all four liver grafts were functioning well at an interval follow
up of 5-26 months.
Table 2
Figure 2
Discussion
Liver transplant is the only curative treatment for patients with
advanced liver failure and hepatocellular carcinoma [8]. With the
progress of surgical techniques and understanding of graft anatomy,
LDLT emerged as a mainstream modality of transplantation.
However, its expansion slowed down due to the occurrence of SFSS.
This was especially so in the Western countries where the donor
morbidity and risk of SFSS potentially outweigh the benefits of
performing LDLT with SFSG. Furthermore, because the deceased
donor pool is larger, LDLT with its attendant risks to the donor and
SFSS make it a controversial option [9].
Although SFSS can potentially be avoided by using the larger
right lobe graft, Umeshita et al. [10] reported a higher frequency of
complications in donors of the right liver lobe compared to donors
of lateral segment or left lobe [10]. Use of a smaller liver graft,
though reducing donor morbidity and mortality, is limited by risk
of developing SFSS and vulnerability to other insults such as sepsis
during recovery period [2,11].
Though not well understood, SFSS appears primarily linked to
graft hyperperfusion. Poor outcomes have been reported in LDLT
with SFSG likely due to excessive portal venous inflow which causes
a diffuse ischemic pattern with cellular ballooning noted on liver
biopsies [12,13]. To improve SFSG survival, many have proposed
to modulate portal inflow to prevent graft hyperperfusion. As portal
vein flow accounts for over 90% of total liver flow, [14] it is reasonable
to modulate portal inflow to prevent SFSS in recipients with GWR
<0.8. Troisi et al. [2] reported a poorer outcome in SFSG without
inflow modulation compared to those with inflow modulation [2].
The decision to perform inflow modulation relies on the clinical
judgment of the surgeon and the severity of portal hypertension at
transplantation. There is no fixed threshold of portal vein pressure
in deciding to perform portal inflow modulation to reduce portal
hyperperfusion. Troisi et al. [2] concluded in a study that PVF of
250 ml/min per 100 g liver is a suitable target level to prevent SFSS
[2]. Kyoto group described a retrospective series and concluded that
patients with a portal pressure of <15 mmHg demonstrated a better
survival rate that patients with portal pressure >15 mmHg [15].
Our unit’s practice is to modulate the inflow of all recipients with
a GWR of <0.8 to prevent SFSS. In our series, all four patients with
inflow modulation of portal flow did not develop SFSS or early graft
dysfunction requiring re-transplantation.
The use of Splenectomy or Splenic Artery Ligation (SAL) as a
simple and safe method to modulate portal flow has been reported
[2,16,17]. If this is insufficient to relieve portal hyperperfusion,
other techniques such as hemi-portocaval shunts, banding or portomesenteric
disconnection should be considered [14]. Troisi et al. [2]
reported excellent graft survival in using hemi-portocaval shunt to
modulate portal inflow in recipients with GWR <0.8 [9]. However,
significant concerns have been raised due to the worry that excessive
portal shunting carries a risk of hepatofugal flow which could lead
to graft dysfunction, portal thrombosis or impairment of graft
regeneration capabilities [18]. Yamada et al. proposed utilization of
a hemi-portocaval shunt based on portal vein pressure more than 20
mmHg at the time of transplant in recipients with GWR between 0.6-
0.8. In this study, there were no significant negative impacts of the
persistent shunt on graft regeneration capabilities.
In our centre, modulation of graft inflow of SFSG was achieved
by performing a splenectomy with a temporary hemi-portocaval
shunt for our recipients with a GWR <0.8. With the portal flow
modulated, there was a significant drop of portal pressure before
and after completion of anastomosis (Table 2), signifying successful
reduction of portal flow to the small partial liver grafts. This was a
durable procedure evidenced by the sustained reduction of portal
pressure even after ligation of the hemi-portocaval shunt. As our
patients did not develop SFSS, we concluded that this is a safe method
to modulate inflow of portal vein without further compromising the
graft regeneration capabilities.
In our series, we have demonstrated a safe and yet efficient way to
modulate the portal inflow in order to prevent development of SFSS
in SFSG. Maturation of this technique might lead to more ALDLT
cases with smaller liver grafts that could potentially benefit would be
recipients without compromising the safety of the donors.
Figure 3
References
- Lee SG. A complete treatment of adult living donor liver transplantation: a review of surgical technique and current challenges to expand indication of patients. Am J Transplant. 2015;15(1):17-38.
- Troisi R, Cammu G, Militerno G, De Baerdemaeker L, Decruyenaere J, Hoste E, et al. Modulation of the portal graft inflow: a necessity in adult living donor liver transplantation? Ann Surg. 2003;237(3):429-36.
- Kiuchi T, Tanaka K, Ito T, Oike F, Ogura Y, Fujimoto Y, et al. Small-for-size graft in living donor liver transplantation: how far should we go? Liver Transpl. 2003;9(9):S29-35.
- Troisi R, Berardi G, Tomassini F, Sainz-Barriga M. Graft inflow modulation in adult-to-adult living donor liver transplantation: A systematic review. Transplant Rev (Orlando). 2017;31(2):127-35.
- Sugawara Y, Makuuchi M, Takayama T. Small-for-size grafts in living-related liver transplantation. J Am Coll Surg. 2001;192(4):510-3.
- Mori S, Park M-S, Kim H, Choi Y, Hong G, Yi N-J, et al. Dysfunction in patients with small-for-size grafts after living donor liver transplantation. Int Surg. 2015;100(3):524-30.
- Dahm F, Georgiev P, Clavien PA. Small-for-size syndrome after partial liver transplantation: definition, mechanisms of disease and clinical implications. Am J Transplant. 2005;5(11):2605-10.
- Wertheim JA, Petrowsky H, Saab S, Kupiec-Weglinski JW, Busuttil RW. Major challenges limiting liver transplantation in the United States. Am J Transplant. 2011;11(9):1773-84.
- Troisi R, Ricciardi S, Smeets P, Petrovic M, Van Maele G, Colle I, et al. Effects of hemi-portocaval shunts for inflow modulation on the outcome of small-for-size grafts in living donor liver transplantation. Am J Transplant. 2005;5(6):1397-404.
- Umeshita K, Fujiwara K, Kiyosawa K, Makuuchi M, Satomi S, Sugimachi K, et al. Operative morbidity of living liver donors in Japan. Lancet. 2003;362(9385):687-90.
- Lahnborg G, Bracher M, Hickman R, Terblanche J. Disturbances of reticulo-endothelial function following experimental liver transplantation. Eur Surg Res. 1989;21(3-4):129-36.
- Emond JC, Renz JF, Ferrell LD, Rosenthal P, Lim RC, Roberts JP, et al. Functional analysis of grafts from living donors. Implications for the treatment of older recipients. Ann Surg. 1996;224 (4):544-54.
- Shimamura T, Tanigichi M, Jin MB, Suzuki T, Matsushita M, Furukawa H, et al. Excessive portal venous inflow as a cause of allograft dysfunction in small-for-size living donor liver transplantation. Transplant Proc. 2001;33(1-2):1331.
- Sainz-Barriga M, Reynyjens K, Costa MG, Scudeller L, Rogiers X, Wouters P, et al. Prospective evaluation of intraoperative hemodynamics in liver transplantation with whole, partial and DCD grafts. AM J Transplant. 2010;10(8):1850-60.
- Ogura Y, Hori T, El Moghazy WM, Toshizawa A, Oike F, Mori A, et al. Portal pressure <15 mmHg is a key for successful adult living donor liver transplantation utilizing smaller grafts than before. Liver Transpl. 2010;16(6):718-28.
- Ito T, Kiuchi T, Tamamoto H, Oike F, Ogura Y, Fujimoto Y, et al. Changes in portal venous pressure in the early phase after living donor liver transplantation: pathogenesis and clinical implications. Transplantation. 2003;75(8):1313-7.
- Sato Y, Yamamoto S, Oya H, Nakatsuka H, Tsukahara A, Kobayashi T, et al. Splenectomy for reduction of excessive portal hypertension after adult living-related donor liver transplantation. Hepatogastroenterology. 2002;49(48):1652-5.
- Sanada Y, Mizuta K, Urahashi T, Wakiya T, Ihara Y, Okada N, et al. Impact of posttransplant portosystemic shunts on liver transplantation. World J Surg. 2012;36(10):2449-54.