Editorial
Quality Parameters for Wedge Resections: Why not?
Federico Raveglia1, Alessandro Baisi1*, Matilde De Simone1 and Ugo Cioffi2
1Thoracic Surgery Unit, San Paolo Hospital, University of Milan, Italy
2Department of Surgery, University of Milan, Italy
*Corresponding author: Alessandro Baisi, Thoracic Surgery Unit, San Paolo Hospital, University of Milan, Italy
Published: 15 Oct, 2018
Cite this article as: Raveglia F, Baisi A, De Simone M,
Cioffi U. Quality Parameters for Wedge
Resections: Why not?. Clin Surg. 2018;
3: 2161.
Dear Editor,
For patients with early-stage Non–Small Cell Lung Cancer (NSCLC) not fit for lobectomy,
treatment options include surgery with sublobar resection. Its outcomes, indeed, despite worse
than lobectomy or any other anatomic resection, are satisfying. It is common opinion that sublobar
resections are affected by two main lacks. The first one is represented by margin that could be
interested by macroscopic or microscopic tumor foci. The second one is represented by a supposed
impossibility of satisfying nodal dissection. Moreover, for both these points, it is difficult to
determine if the actual problem concerns surgical technique or surgeons’ habits. Nowadays, correct
assessment of wedge resection efficacy for early-stage NSCLC is needed also during comparison
with Stereotactic Body Radiotherapy (SBRT) as alternative approach in patients with poor general
conditions. However, since wedge resection outcomes could be influenced, as reported above, by
technical aspects or surgeons’ habits, a definition of quality for non anatomic resection should be
encouraged; quite the opposite, data on the quality of non anatomic resection are limited. Recently,
Ajmani et al. [1] have published a study about this topic. The variables as quality indicators were
margins (R0 vs. R+) and numbers of Lymph Nodes (LNs) examined. This paper is interesting and
prompts to a vibrant discussion, indeed, with a population of 10.032 patients enrolled; it provides a
reliable “state of the art” about sub-anatomical resections in North America. Surprising, only 17.1%
of patients had correct operative nodal staging (>5 LNs examined), determining an overall upstage
of “only” 3% (primarily N1) versus 20% in literature. Whereas, negative margins were showed
in the most of cases (94.6%). These data could reveal that lymphadenectomy was intentionally
neglected rather than obstructed by technical difficulties. Since Authors results show that overall
survival worsen when surgical quality is low, their conclusions would suggest the need of common
recommendations about minimum objective to reach, when performing sub-anatomical resections.
This is even more desirable if we want to seriously support wedge resection versus SBRT. If nodal
statement is a real point in sub-anatomical resection, also margins are determinant as showed in
the paper. However, quality of margins assessment is more challenging. For example, Authors only
codified the positive or negative status of margins, despite many series reported that survival is
related to distance between tumor and margin [2] that should be at least 1.5 cm [3].
Moreover, discussion get more complicated if we consider that there are different ways
to measure ‘‘margin length’’. Our main concern about the possibility to classify wedges is their
heterogeneity. Apart of margins length, also the resection shape changes based on tumor position
and surgeons routine. Shape of parenchyma resected is also determined by open or closed approach
and number of ports. Unfortunately resection shape is hard to be described, but we think that this
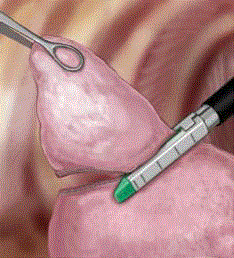
could be a critical parameter. In our opinion resection should be as
deep as possible toward the hilum, mimicking a segmentectomy.
Otherwise, if the resection is tangential to pleura it could involve
more parenchyma from healthy adjacent segments than from the
pathological one (Figure 1 and 2). To conclude, if high-quality wedge
appears to confer a significant survival advantage over lower-quality
wedge and stereotactic radiation, standards to determine quality
are still unclear. Negative margins and nodal dissection are surely
requested but perhaps more rigorous criteria about resection shape
and number of nodal stations sampled could be useful.
Figure 1
Figure 2
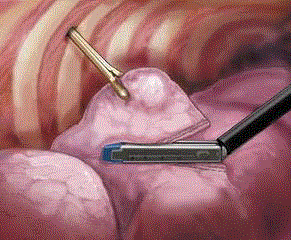
Figure 2
Parenchyma resection by staplers oriented quite tangential to
visceral pleura with straight line margin.
References
- Ajmani GS, Wang CH, Kim KW, Howington JA, Krantz SB. Surgical quality of wedge resection affects overall survival in patients with early stage non–small cell lung cancer. J Thorac Cardiovasc Surg. 2018;156(1):380-91.
- Baisi A, Raveglia F, De Simone M, Cioffi U. Do Margins Really Affect Prognosis in Wedge Resection for Early-Stage Lung Cancer? Ann Thorac Surg. 2016;101(4):1629.
- Sawabata N. Who should decide margin length in pulmonary excision of lung cancer? J Thoracic and Cardiovasc Surg. 2014;148(1):370-71.