Case Report
Hematospermia as Unknown Complication of Tension Free Mesh Repair of an Inguinal Hernia
Victoria Walter*, Jonas Roller and Matthias Glanemann
Department for General, Visceral, Vascular and Pediatric Surgery, University Hospital of the Saarland, Germany
*Corresponding author: Victoria Walter, Department for General, Visceral, Vascular and Pediatric Surgery, University Hospital of the Saarland, Homburg-Saar, Germany
Published: 10 Oct, 2018
Cite this article as: Walter V, Roller J, Glanemann
M. Hematospermia as Unknown
Complication of Tension Free Mesh
Repair of an Inguinal Hernia. Clin Surg.
2018; 3: 2150.
Abstract
Implantation of prosthetic meshes has become the gold standard in the repair of inguinal hernias. In
contrast to closure by suture, implantation of a mesh provides tension-free hernia repair, resulting
in decreased postoperative pain and significantly reduced recurrence rates. However, mesh
implantation may bear specific risks. In fact, mesh infection, migration of the mesh and seroma have
been recognized as mesh related complications. Here in, we describe a case with hematospermia as
a - to date unreported- complication of mesh repair of an inguinal hernia.
Keywords: Hematospermia; Tension free hernia repair; Mesh
Introduction
Hernia repair represents one of the most frequent operations in general surgery. Within
the last decades, tension free mesh implantation has become the gold standard in hernia repair.
During this time, material and shape of the implanted meshes developed significantly, resulting
in the modern light-weight, partly resorbable mesh materials that are commonly used for hernia
repair. Importantly and - in contrast to closure by suture - tension-free mesh implantation results
in reduced postoperative pain and significantly reduced recurrence rates [1-3]. Accordingly, about
62,500 of the inguinal hernias in 2015 underwent hernia repair by implantation with mesh [4].
However, implantation of a prosthetic mesh bears a numbers of risks including postoperative
seroma, mesh infection, fibrosis and mesh migration [5-7]. Moreover, as in inguinal hernia repair
the spermatic cord passes through the mesh material, affections of the spermatic cord have been
described as complications [8]. In this regard, symptoms may include chronic postoperative pain
and in the most severe cases, ischemic orchitis and testicular atrophy [5,9,10].
We herein describe a case of a 67 year old male patient after open inguinal hernia repair with
a mesh. The patient presents with the isolated symptoms of persistent hematospermia. To our
knowledge this is the first report of persistent hematospermia as a complication of open inguinal
hernia repair with a mesh.
Case Presentation
A 67-year old male patient presented with persistent hematospermia 4 months after open mesh repair of an inguinal hernia. At the time of presentation, the patient denied any scrotal or inguinal pain. Detailed urological investigations, including examination of the prostate and laboratory parameters to exclude a prostatitis and ultrasound examinations of the testis did not reveal possible urologic causes for the hematospermia. Accordingly Magnetic Resonance Imaging (MRI) of the pelvis and testis was arranged for continuative diagnostics. Herein, we found a solitary venous congestion of the spermatic vessels (Figure 1a) and a pronounced scar tissue in direct vicinity of the implanted inguinal mesh (Figure 1b). Arterial blood flow of the spermatic vessels was shown to be undisturbed and no other reasons for hematospermia could be detected. After discussing the MRI findings with the patient, he decided himself for further conservative treatment in order to wait for spontaneous healing of the venous affection. However, after persistence of the hematospermia for one year, the patient decided for operative treatment of the described findings. Accordingly in agreement with the patient, laparoscopic ligature and transection of the spermatic cord of the affected side was performed. The patient was dismissed two days postoperatively without any complications and reported about immediate absence of the hematospermia after surgery.
Review of the Literature
Hernia repair with prosthetic meshes represent a common procedure in the treatment of
inguinal hernias [2]. In fact, approximately 1,000,000 mesh repairs of
inguinal hernias are performed yearly worldwide [11]. In general, the
complication rate is low. The most frequent complications include
postoperative pain, seroma, mesh infection and mesh migration
[5,6]. However, severe complications by affection of the spermatic
cord have been described before. In fact, it was reported before that
herniorrhaphy with a mesh might cause inguinal vessel obstruction
with subsequent azoospermia, ischemic orchitis or testicular atrophy
[5,9,10,12]. Beyond vessel obstruction, also invasion of mesh edges
into the vas deference were described [13]. In this case, symptoms
included painful sperm granula four years after mesh repair of an
inguinal hernia. In our reported case the patient presented with
painless hematospermia 4 months after mesh repair of an inguinal
hernia. To our knowledge this is the first description of hematospermia
as a symptom of an affection of the spermatic cord by the mesh. MRI
diagnostic had shown that the hematospermia most likely was caused
by a venous congestion in direct vicinity of the ductus deferens.
Due to the increased pressure in the vein, collaterals with repetitive
bleedings into the ductus deferens might have occurred. Another
possibility is that the mesh might have caused a simultaneous erosion
of the vein and the ductus deferens with a subsequent fistula from the
vein into the ductus. Nevertheless the described case highlights the
importance of an adequate adjusting of the opening of the mesh for
the spermatic cord, in order to avoid a compression of the vascular
structures and the ductus deferens.
In conclusion, our case report shows that even with undisturbed
arterial blood perfusion within the spermatic cord, mesh related
complications can arouse from venous congestion. In this regard,
isolated hematospermia might be the leading symptom.
Figure 1
Figure 1
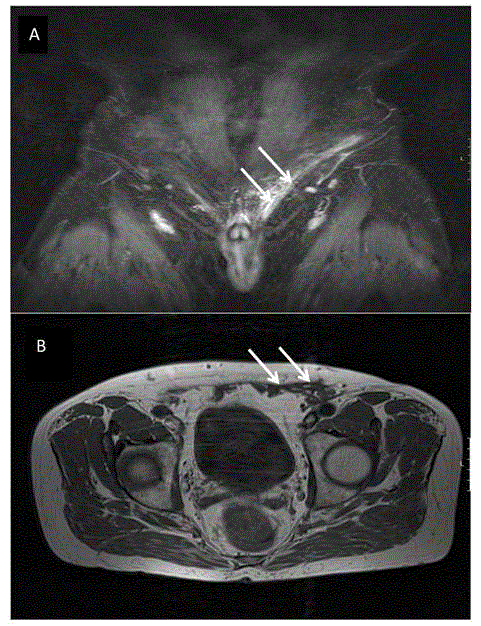
Representative MR - images (MRI) of the patient with
hematospermia after open inguinal hernia repair with a mesh. The coronar
(A; STIR-weighting) MR-image revealed a venous congestion of the
spermatic vessels (arrows) in direct vicinity of the implanted mesh material.
The transversal (B; T1 weighting) MR-image revealed a scar tissue in direct
vicinity of the implanted mesh material.
References
- Peiper Ch, Klinge U, Junge K, Schumpelick V. [Meshes in inguinal hernia repair]. Zentralbl Chir. 2002;127(7):573-7.
- Simons MP, Aufenacker T, Bay-Nielsen M, Bouillot JL, Campanelli G, Conze J, et al. European Hernia Society guidelines on the treatment of inguinal hernia in adult patients. Hernia. 2009;13(4):343-403.
- Israelsson LA, Smedberg S, Montgomery A, Nordin P, Spangen L. Incisional hernia repair in Sweden 2002. Hernia. 2006;10(3):258-61.
- Reinpold W. Aktuelle Leistenhernienchirurgie. Leitliniengerecht. Prävention und Management von Komplikationen. [Inguinal hernia up to date. Prevention and management of complications] Hamburger Ärzteblatt. 2015;17539:28-31.
- Amid PK. Lichtenstein tension-free hernioplasty: its inception, evolution, and principles. Hernia. 2004;8(1):1-7.
- Nienhuijs SW, Rosman C, Strobbe LJ, Wolff A, Bleichrodt RP. An overview of the features influencing pain after inguinal hernia repair. Int J Surg. 2008;6(4):351-6.
- Junge K, Binnebosel M, Rosch R, Ottinger A, Stumpf M, Muhlenbruch G, et al. Influence of mesh materials on the integrity of the vas deferens following Lichtenstein hernioplasty: an experimental model. Hernia. 2008;12(6):621-6.
- Al-Subaie S, Al-Haddad M, Al-Yaqout W, Al-Hajeri M, Claus C. A case of a colocutaneous fistula: A rare complication of mesh migration into the sigmoid colon after open tension-free hernia repair. Int J Surg Case Rep. 2015;14:26-9.
- Klinge U, Klosterhalfen B, Müller M, Schumpelick V. Foreign body reaction to meshes used for the repair of abdominal wall hernias. Eur J Surg. 1999;165(7):665-73.
- Lima Neto EV, Goldenberg A, Juca MJ. Prospective study on the effects of a polypropylene prosthesis on testicular volume and arterial flow in patients undergoing surgical correction for inguinal hernia. Acta Cir Bras. 2007;22(4):266-71.
- Puccio F, Solazzo M, Marciano P. Comparison of three different mesh materials in tension-free inguinal hernia repair: prolene versus Vypro versus surgisis. Int Surg. 2005;90(3 Suppl):S21-3.
- Shin D, Lipshultz LI, Goldstein M, Barme GA, Fuchs EF, Nagler HM, et al. Herniorrhaphy with polypropylene mesh causing inguinal vasal obstruction: a preventable cause of obstructive azoospermia. Ann Surg. 2005;241(4):553-8.
- Silich RC, McSherry CK. Spermatic granuloma. An uncommon complication of the tension-free hernia repair. Surg Endosc. 1996;10(5):537-9.