Case Report
Ileal Flap Duodenoplasty to Repair Large Duodenal Defects after R0 Resection for Malignant Tumor to Avoid a Complex Reconstruction: Experience with 6 Cases
Sami Hamed, TheophileGuilbaud, Jean Hardwigsen and Yves Patrice Le Treut
Department of Digestive Surgery and Liver Transplantation, Aix Marseille University, France
*Corresponding author: Yves Patrice Le Treut, Department of Digestive Surgery and Liver Transplantation, Aix Marseille University, APHM, Hôpital de la Timone, 264 rue St Pierre, 13005 Marseille, France
Published: 18 Sep, 2018
Cite this article as: Hamed S, Guilbaud T, Hardwigsen J,
Le Treut YP. Ileal Flap Duodenoplasty
to Repair Large Duodenal Defects after
R0 Resection for Malignant Tumor
to Avoid a Complex Reconstruction:
Experience with 6 Cases. Clin Surg.
2018; 3: 2110.
Abstract
Locally advanced malignant abdominal tumors of the right upper quadrant, as in colonic
carcinomas, can lead to a major resection of the duodenal sidewall to create free resection margins
(R0 resection). There is no standard surgical technique to manage this duodenal defect. We report
here our experience of a standardized duodenal reconstruction using an ileal flap. Following a right
colectomy with a major duodenal resection, the duodenal defect was covered with a pedicledileal
flap using the terminal ileum. This reconstruction is particularly suitable for performing a tensionfree
ileo-transverse anastomosis. Duodenal leakage did not occur in our study. Our experience as
well as a literature review shows that this technique is feasible and safe and is a reliable surgical
approach that avoids the need for a radical pancreaticoduodenectomy or a non-anatomical by-pass.
Keywords: Locally advanced tumors; Large duodenal defect; Ileal flap
Introduction
Approximately 10 percent of colonic carcinomas are locally advanced due to the involvement of adjacent organs [1]. Free resection margins (R0 resection) of locally advanced colonic cancer at the hepatic flexure can lead to a major en-bloc resection of the second duodenal sidewall, raising the issue of duodenal repair. A similar situation may be encountered with other malignant tumors of the upper right quadrant, such as liver, gallbladder, duodenal or retroperitoneal tumors. In cases of duodenal and pancreatic spread, there is no curative solution other than a Pancreaticoduodenectomy (PD). However, when invasion is limited to the duodenal sidewall, there is no standard surgical procedure for reconstructing the large duodenal defect after partial duodenectomy. Ileal flap duodenoplasty seems to be a safe but relatively unknown surgical procedure. We report here our case study experiences and a review of the literature on this topic.
Operative Technique
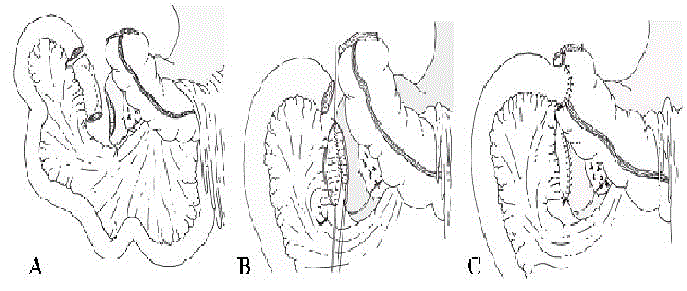
Following a Right Colectomy (RC) extending to a large portion of the duodenum, the duodenal defect can be covered with an ileal flap using the last loop of the ileum. A segment of the terminal ileum is isolated with a large pedicle of mesentery (it is better not to use a vascular section) (Figure 1a). The length of the ileal segment is adjusted to the size of the defect. The segment is opened along the antimesenteric border and then is easily transposed to the duodenum (Figure 1a) and sutured in isoperistaltic fashion on the duodenal defect using a continuous absorbable running suture (Figure 1b). A sealing test can be performed with air insufflation using a gastric probe. This reconstruction is particularly suitable for performing a tension-free ileo-transverse end-to-side anastomosis without torsion of the mesentery (Figure 1c). A gastric tube or gastrostomy tube can then be placed for gastric discharge.
Figure 1
Figure 1
Schematic representation of the procedure. A.Resection of the right colon with the duodenal sidewall resulted in a large duodenal defect. A segment of terminal ileum was isolated on a large vascular pedicle of mesentery, and the antimesenteric border of the lumen was opened. B. The duodenal defect was covered with the pedicledileal flap using a continuous running suture. C. An end-to-side anastomosis was done between the ileum and the mid-transverse colon.
Case Studies
We studied 6 cases with various kinds of tumors - adenocarcinoma of the right colon, gallbladder cancer, intrahepatic cholangiocarcinoma, and retroperitoneal sarcoma - macroscopically invading the sidewall of the first and/or second part of the duodenum (Table 1). Two cases have already been reported [2]. In all the cases, surgery allowed complete resection with safe margins (R0 resection) due to a major resection of the duodenal wall (duodenal defect measures 5 cm to 10 cm in length). In all the cases, we used an ileal flap to cover the duodenal defect. In one case that underwent a right hepatectomy extending to segment IV as well as bile duct confluence, a biliary-enteric anastomosis was done on the upstream end of the ileal segment, and the other end was used to cover the duodenal defect. An upper digestive tract X-ray series was done 7 days after surgery (Figure 2). Five patients had an uneventful course. One patient had a biloma in the bed of segmentectomy IV, which was treated with percutaneous drainage, and one patient died on day 25 from sepsis and hepatic failure without any sign of duodenal leakage.
Table 1
Discussion
Our experience shows that this technique is feasible to achieve
curative intent and is a safe and reliable surgical approach to avoid
radical PD and non-anatomical bypass.
In the presence of locally advanced colonic cancer, an aggressive
surgical approach can be effective and is associated with low
morbidity-mortality and a high survival rate [1,3]. In the case of a
right-sided colonic tumor, R0 resection extended “en bloc” to other
organs, such as the abdominal wall, gallbladder, small intestine,
kidney or ureter, can be safely performed. Regarding other duodenal
tumors such as stromal tumors, safe surgical margins are feasible,
with good survival rates. The severity of duodenal GIST appears to
be linked to particularly high rate of mitosis [4]. When either the
pancreas is involved or the duodenal invasion is massive, including
the papilla of Vater, the consensus is that it is desirable to achieve an
en bloc PD for curative intent. In contrast, when invasion is limited
to the duodenal sidewall, there is no consensus if the duodenal defect
does not allow for a simple closure. Several procedures can be used in
this rare instance: a PD [5] or a duodenal resection followed by Rouxen-
Y duodenojejunostomy [1], side-to-side duodenojejunostomy [6],
and a jejunal [3] or ileal flap [7]. Gastric pedicle patches have also
been described for duodenal stenosis [8].
A thorough literature review was conducted regarding locally
advanced malignant tumors of the right upper quadrant invading the
duodenum without pancreatic involvement. Cases of small resections
that may be simply closed as well as studies that did not describe the
surgical technique were not included (Table 2). Forty-seven patients
were collected, including our 6 cases. Most of the cases were those
of colonic cancer invading the duodenum (n=37); 4 cases were
duodenal GIST (with colonic invasion in 2 cases) and 6 cases were
other various diseases. Ileal flap was the most used technique (n=23),
followed by PD (n=9), Roux-en-Y duodenojejunostomy (n=9), lateral
duodenojejunostomy (n=3), and jejunal flap (n=3). Intraoperative
complexity and a high risk of postoperative complications for enbloc
RC plus PD often discourage surgeons from the procedure
[9]. Thus, the ileal flap avoids PD, which involves increased risk
of fistulas, especially when the pancreatic parenchyma is soft [9].
A duodenojejunostomy reconstruction can lead to difficulties in
moving the jejunal loop closer to the duodenal defect in the case
of a short mesentery, especially if an RC is not performed. Indeed,
RC associated with duodenal resection allows for easier lifting of
the ileal flap closer to the duodenal defect in anisoperistaltic fashion
immediately upstream from the ileo-transverse anastomosis. In
addition, the jejunal or ileal flap is the better anatomical solution
because there is no bypass or risk of reflux. In our case review,
no postoperative duodenal leakage was reported, and there was
only one case of postoperative death. In our case studies, the main
postoperative complication (bilioma, hepatic failure) were unrelated
to duodenoplasty.
Regarding the long-term results, the choice between RC plus PD
or RC with major duodenal resection remains unclear. In a recent
review, the 5-year survival rate was 52% after en bloc RC plus PD
vs. 25% and 0% in the cases of duodenal resection with correction
by direct suture or pedicledileal flap, respectively [9]. However, this
review included 10 cases of major duodenal resections only (vs. 38 in
our review), and survival rates were grossly estimated by the ratio of
patients living more than 5 years irrespective of shorter follow-ups. In the Kaplan Meir method based on the duration of survival specified
for each patient in each report. No follow-up was done in 9 of the 37
cases of colonic carcinomas. Among the remaining patients, the 3-year
survival rate of patients treated with RC with duodenal resection
(n=20) was 75%. This rate was comparable to the 3-year survival rate
of patients treated with RC plus DP (n=8, 70%). Regardless of the
treatment options, a complete R0 tumor removal remains the primary
prognostic factor [21]. In the case of exclusive duodenal invasion,
this goal is easier to achieve if the extent of duodenal resection is not
restricted by the underlying difficulties of the repair.
Table 2
Figure 2
Figure 2
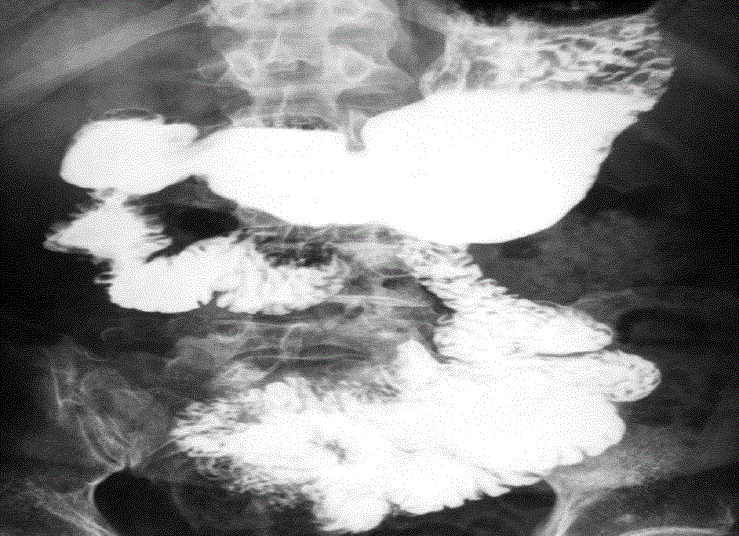
Postoperative day 7 upper gastrointestinal X-ray series. The arrow
shows the pedicled ileal flap. The passage through the “new duodenum” was
well maintained without stenosis or leakage.
Conclusion
Tumor invasion of the duodenum without pancreatic involvement is a rare and challenging condition. A radical approach is still possible by liberal resection of the lateral portion of the duodenum. Ileal flap duodenoplasty can then be ideally achieved with RC.
References
- Curley SA, Evans DB, Ames FC. Resection for cure of carcinoma of the colon directly invading the duodenum or pancreatic head. J Am Coll Surg. 1994;179(5):587-92.
- Richa H, Camerlo A, Campanile M, Hardwigsen J, Treut YPL. Ileal patch duodenoplasty after right colectomy extended to the duodenal wall. Hepatogastroenterology. 2008;55(85):1365-6.
- Koea JB, Conlon K, Paty PB, Guillem JG, Cohen AM. Pancreatic or duodenal resection or both for advanced carcinoma of the right colon: is it justified? Dis Colon Rectum. 2000;43(4):460-5.
- Colombo C, Ronellenfitsch U, Yuxin Z, Rutkowski P, Miceli R, Bylina E, et al. Clinical, pathological and surgical characteristics of duodenal gastrointestinal stromal tumor and their influence on survival: a multi-center study. Ann Surg Oncol. 2012;19(11):3361-7.
- Yang WL, Yan CQ, Zhang HG, Wang FJ, Ma YL. Surgical treatment and prognosis of cancer of hepatic flexure of colon invading the duodenum in 65 patients. Zhonghua Zhong Liu Za Zhi. 2009;31(11):873-6.
- Kapoor S, Das B, Pal S, Sahni P, Chattopadhyay TK. En bloc resection of right-sided colonic adenocarcinoma with adjacent organ invasion. Int J Colorectal Dis. 2006;21(3):265-8.
- Yuan L, Zhou J, Shu G, Liu D, Zhou J. Pedicled ileal flap for duodenal defect after right hemicolectomy. Hepatogastroenterology. 2010;57(100):493-6.
- Walley BD, Goco I. Duodenal patch grafting. Am J Surg. 1980;140(5):706-8.
- Cirocchi R, Partelli S, Castellani E, Renzi C, Parisi A, Noya G, et al. Right hemicolectomy plus pancreaticoduodenectomy vs partial duodenectomy in treatment of locally advanced right colon cancer invading pancreas and/or only duodenum. Surg Oncol. 2014;23(2):92-8.
- Mouaqit O, Chbani L, Maazaz K, Amarti A, Ait Taleb K, Oussaden A. A large gastrointestinal stromal tumor of the duodenum treated by partial duodenectomy with Roux-en-Y duodenojejunostomy: a case report. J Med Case Rep. 2013;7:184.
- Notani H, Kawamura T, Sato T, Hoshino A, Sato Y, Nakajima A. A patient treated with partial duodenectomy for invasive transverse colon cancer. Gan To Kagaku Ryoho. 2013;40(12):1738-40.
- Lee WS, Lee WY, Chun HK, Choi SH. En bloc resection for right colon cancer directly invading duodenum or pancreatic head. Yonsei Med J. 2009;50(6):803-6.
- Liyanage CA, Abeygunawardhana S, Kumarage S, Deen KI. Duodenum-preserving local excision of a gastrointestinal stromal tumor. Hepatobiliary Pancreat Dis Int. 2008;7(2):214-6.
- Goh BK, Chow PK, Ong HS, Wong WK. Gastrointestinal stromal tumor involving the second and third portion of the duodenum: treatment by partial duodenectomy and Roux-en-Y duodenojejunostomy. J Surg Oncol. 2005;91(4):273-5.
- Perez RO, Coser RB, Kiss DR, Iwashita RA, Jukemura J, Cunha JE, et al. Combined resection of the duodenum and pancreas for locally advanced colon cancer. Curr Surg. 2005;62(6):613-7.
- Ishiguro S, Moriura S, Kobayashi I, Tabata T, Yoshioka Y, Matsumoto T. Pedicled ileal flap to repair large duodenal defect after right hemicolectomy for right colon cancer invading the duodenum. Surg Today. 2004;34(4):386-8.
- Berrospi F, Celis J, Ruiz E, Payet E. En bloc pancreaticoduodenectomy for right colon cancer invading adjacent organs. J Surg Oncol. 2002;79(3):194-7.
- Fujiwara H, Yamasaki M, Nakamura S, Yasuda K, Tomiyoshi H, Teramura K. Reconstruction of a large duodenal defect created by resection of a duodenal tubulovillous adenoma using a double-tract anastomosis to a retrocolic roux-en-y loop: report of a case. Surg Today. 2002;32(9):824-7.
- Xenos ES, Halverson JD. Duodenocolic fistula: case report and review of the literature. J Postgrad Med. 1999;45(3):87-9.
- Cawthorn SJ, Bett NJ, Rutter KR. Malignant duodenocolic fistula: long-term survival following an extended right hemicolectomy with wide local excision of the duodenum. Br J Surg. 1985;72(3):211.
- Lehnert T, Methner M, Pollok A, Schaible A, Hinz U, Herfarth C. Multivisceral resection for locally advanced primary colon and rectal cancer: an analysis of prognostic factors in 201 patients. Ann Surg. 2002;235(2):217-25.