Research Article
Effect of Different Years of Resident Training on Complications and Stone Free Rate during Percutaneous Nephrolithotomy for Large Renal Stone Greater Than 20 mm: A Prospective Observational Study Using Balloon Dilator
Pao-Hwa Chen1, Meng-Yi Yan1, Heng-Chieh Chiang1*, Bai-Fu Wang1, Jesun Lin1, Chin-Pao Chang1, Sheng-Hsien Huang1, Chun-Chi Chen1, Hung-Jen Shih1,3,4, Chien-Hsiang Chang1, Jian-Ting Chen1 and Yao-Li Chen2
1Department of Surgery, Changhua Christian Hospital, Changhua, Taiwan
2Changhua Christian Hospital, Changhua, Taiwan
3School of Medicine, Chung Shan Medical University, Taichung, Taiwan
4School of Medicine, Kaohsiung Medical University, Kaohsiung, Taiwan
*Corresponding author: Heng-Chieh Chiang, Department of Surgery, Division of Urology, Changhua Christian Hospital, 135, Nanxiao St., Changhua City, Changhua County 500, Taiwan
Published: 11 Sep, 2018
Cite this article as: Chen P-H, Yan M-Y, Chiang H-C, Wang
B-F, Lin J, Chang C-P, et al. Effect of
Different Years of Resident Training on
Complications and Stone Free Rate
during Percutaneous Nephrolithotomy
for Large Renal Stone Greater Than 20
mm: A Prospective Observational Study
Using Balloon Dilator. Clin Surg. 2018;
3: 2098.
Abstract
Objective: The endoscopic management of urolithiasis has been the primary choice of treatment for
upper urinary tract urolithiasis. For large symptomatic renal calculi, Percutaneous Nephrolithotomy
(PCNL) provides the highest stone clearance rate. In this prospective study, we compared patients
undergoing PCNL using balloon dilator with sequential Amplatz dilator.
Methods: We started using balloon dilator for nephrostomy tract for PCNL since August 2014. From
August 2014 to July 2015, we performed 154 C-arm guided PCNL procedures with balloon dilator at
our hospital. We prospectively followed these patients and recorded peri - and post-operative data
and complications. We then compared the same data with 155 patients using Amplatz dilator in the
previous year.
Results: A total of 309 patients were included in this study (154 patients in balloon and 155 in the
Amplatz dilator). The average stone burden was larger in the Amplatz group (1189 vs. 771 mm2).
Balloon dilator group has a slightly better stone free rate (78% vs. 75%). Patients with residual stone
are the ones with higher stone burden on KUB (1734 and 1512 mm2). Surgeon's experience is also a
factor in stone free rate. Most of the complication is Clavien grade 1-2. There were 3 patients Clavien
grade 3 or higher in both group and no mortality.
Conclusion: Balloon dilator is non-inferior to sequential dilator in terms of complications.
Surgeon’s experience seems to influence stone-free rate and blood loss. Future randomized trials are
needed to establish the benefit of balloon dilator.
Keywords: Nephrolithotomy; PCNL; Percutaneous; Stone; Urolithiasis
Introduction
Due to improvements in technologies and equipment, the treatments for upper urinary tract
have shifted from the open and laparoscopic procedures to a more endourological approach. The
reported rate of open procedures for upper urinary tract urolithiasis has decreased from 5% to 6%
in the late 20th century to less than 1% in the beginning of the 21st century [1]. After Thomas Hillier
performed the first therapeutic percutaneous nephrostomy in 1865, Fernstrom and Johannson was
the first to report the use of percutaneous tract for stone removal in 1976 [2]. With the advancement
in technologies, the first decade of 21st century has seen a shift to miniature instrumentation (smaller
than 20 Fr.) in order to minimize wound to decrease complications and morbidities associated with
larger instruments [3]. Due to poor stone clearance in larger calculi, the miniature system (mini,
nano-perc) has stone size limitation [4]. With advancement in flexible ureterorenoscope (FURS),
FURS offers comparable stone clearance to small renal stones without the visible wound of miniature
PCNL. In current guidelines on urolithiasis, FURS is recommended
in complicated patient such as during pregnancy, patients with
urinary diversion, transplanted kidney, calculi in abnormal anatomy,
patients whom cannot discontinue anticoagulants, obese patients,
and renal diverticulum stone. In cases of large renal stone (>2 cm)
or staghorn stones, standard size (24 Fr. to 30 Fr.) PCNL is still the
preferred method of treatment. Therefore, the choice of treatment
modalities in patients with renal stones need to individualized and
a careful balance between stone free rate and minimal complications
need to be addressed. In this study, we prospectively observe patients
undergoing PCNL using balloon dilator and comparing to sequential
Amplatz dilator set. We wanted to identify risk factors for postoperative
complications and factors influencing stone free rate.
Statistical analysis
Patient demographics were expressed in mean values with
standard deviation and range for each variable. Fisher’s exact tests
were used to compare the complication between the 2 data set.
Variables with P<0.05 were considered significant.
Table 1
Method
Patients
After obtaining CCH IRB approval (IRB number: 140315), we
prospectively observed patients whom underwent PCNL using
balloon dilator at our department from August 2014 to July 2015.
Due to the balloon dilator’s ease of use and surgeon preference,
balloon dilators were the main method of percutaneous access in
all PCNL after August 2014. Prior to the introduction of balloon
dilator at our hospital, sequential Amplatz dilator set have been
used to establish PCNL tract. Therefore, we retrospectively identify
patients prior to introduction of balloon dilator (from July 2013 to
July 2014). To match up the patient numbers in both groups, an extra
month was added resulting in a total of 309 patients (155 patients
in Amplatz dilator group and 154 patients in balloon dilator group).
After reviewing the medical records, all post-operative complications,
lab data and culture results were recorded and analyzed.
Peri-operative preparation, operative method and postoperative
care
The patient preparation and stone extraction method was
identical in both group with the only difference being the dilatation
of nephrostomy tract (sequential Amplatz dilator set and BARD
X-Force® balloon dilator). In our urological training program,
residents start performing PCNL in the 4th year of training as the
main operator with a supervising senior staff looking over their work.
Therefore, most of PCNL (close to 90%) at our hospital is performed
by senior resident (4th year resident to fellow). All patients received
intravenous pre-operative prophylactic antibiotics with 1 gram of
cephalosporin. If the patient is more susceptible to infection (i.e.
poor nutrition, immune compromised, DM) or pre-operative urine
showed pyuria/bacteriuria then a 3rd generation cephalosporin will
then be used. After induction of anesthesia, the patient is placed on
lithotomy position for cystoscopy examination and insertion of 5 Fr.
retrograde ureteral catheter into the renal pelvis. Prone position is
used for the establishment of nephrostomy tract and proper care was
taken to protect the pressure points. With more than 90% of PCNL
cases using fluoroscopy in our department, adequate surgeon and
staff protections are mandatory during the operation (lead aprons,
neck shields, lead –containing gloves and lead goggles). The “eye-ofthe-
needle” technique used in establishing percutaneous access are
the same as described by Dr. Arthur Smith in the 2005 supplement of
BJU international [2,5]. Nephrostomy tract dilatations are performed
using either the sequential Amplatz dilator set or the BARD X-Force®
balloon dilator (BARD-Davol Inc., Cranston, RI USA). After dilating
the tract with the balloon dilator using 300 psi (20-22 ATM/bar) of
pressure, the balloon was left inflated for 1 to 3 minutes as a tamponade
effect in an attempt to minimize bleeding. A 24 Fr. Nephrostomy
sheath is routinely used after the establishment of the nephrostomy
tract, if the pre-operative image showed small collecting system then
a smaller size sheath (18 Fr or 20 Fr.) would be considered at the
discretion of the attending. A rigid 24 Fr. Nephroscope and ultrasonic
lithotripter with continuous suction was used to break up the stone
and a 2 or 3 prong grasper was used for extraction. A 6 Fr. Diameter
double-J ureteral stent is routinely used and nephrostomy tube (20-
22 Fr.) is placed at surgeon’s discretion. The external nephrostomy
tube (“tubeless” PCNL) is only omitted when the is no extensive
bleeding at the end of the stone extraction and the decision is left to
the primary surgeon’s discretion. After the placement of the double-J
stent and residual stone is checked with fluoroscopy, the patient is
turned back to supine position to wait for extubation. Post-operative
care includes adequate fluid hydration, use of tranexamic acid and
antibiotics for 1 to 3 days depending on the peri-operative finding.
Intensive care was mandated if the patient experience severe sepsis
with organ dysfunction.
Patient evaluation
A single fellow (P.H.C.) followed the patient after the operation
and evaluate medical records for any post-operative complications
(Clavien-Dindo classification used to grade severity). Amplatz dilator
group was reviewed and recorded in the same fashion.
Table 2
Table 3
Table 4
Results
Patient characteristics and peri-operative data
The patient characteristics from both groups are shown on Table
1. One hundred and fifty-four patients underwent PCNL using
balloon dilator from August 2014 to July 2015, while PCNL using
sequential Amplatz dilator was performed on one hundred fifty-five
patients from July 2013 to July 2014. The patient characteristics from
both groups are very similar with Amplatz dilator group exhibiting
larger stone burden on average. The post-operative data (Table 2)
from both groups were similar (change in hematocrit and creatinine,
stone-free rate and Clavien-Dindo grades. Most of the complications
are self-resolving Clavien-Dindo grade 1 and 2 (Table 3) with three
patients requiring further intervention. The sub-analysis of patients
with infectious complications and stone free rate are listed on table 4
and 5. A positive pre-operative urine routine does not correlate with
post-operative infectious complication (P=0.53), but a “dirty” urine
on first puncture is related to infectious complications (P<0.05). The
year of training does not correlate with post-operative infectious
complications. Previous hospital admission due to urinary tract
infection complications prior to PCNL does not seem to correlate
with post-operative infectious complications. Balloon dilator showed
slightly better stone free rate at 78% (compared to 75% in Amplatz
dilator group). Analysis of the patients with residual stones, we
noticed that the stone burden is almost twice the average. When
comparing between the form of dilatation, the stone free rate is
similar in both group (p= 0.59). But when breaking down to surgeon’s
experience, we found that Fellow surgeons had better stone free rate
using the balloon dilator. Fortunately, all of complications in these
two eras are manageable and there were no Clavien-Dindo grade 5
complications (death of patient). No patients require post-operative
blood transfusion.
Table 5
Figure 1
Discussion
In the rapid evolving field of endourology, the armamentarium
is growing and evolving with each passing year. With improved
instrumentation, endourological treatment of upper urinary tract
urolithiasis has made open/laparoscopic procedures obsolete (<1%)
[1]. Ever since the introduction of Donier HM3 extracorporeal
shockwave lithotripter (ESWL) in 1980’s, ESWL has been a
valuable tool in the treatment of urolithiasis but patient and stone
characteristics limit its use. Since the stone free rate for ESWL decrease
if the stone size exceeds 10 mm, guidelines suggest ESWL for stones
less than 10 mm and favoring endourological procedures for stones
greater than 10 mm. The improvement of FURS gives endourologist
another added option in treating renal stones up to 20 mm, but the
cost and durability of the scope is a major drawback. Miniature PCNL
were used to minimize PCNL complications, but stone burden is still
a major deciding factor in using miniature instruments [3,4,6,7].
Therefore, per guidelines, standard size (24 Fr to 30 Fr.) PCNL is the
first line of treatment for renal stones larger than 20 mm.
The most common complications associated with PCNL are
infection and hemorrhage [8-12]. A major roadblock in comparing
post-operative complication in PCNL from different studies and
hospital is the classification [13-15]. The use of Clavien-Dindo
classification for complication in urological surgeries has been used
and validated in several procedures such as prostatectomy (open
and laparoscopic), donor nephrectomy and several urological
laparoscopic procedures [14]. Numerous articles have investigated
the use of Clavien-Dindo post-PCNL complications including two
articles by Clinical Research Office of the Endourological Society
(CROES) group [13-15]. In the article by Dr. de la Rosette, the
agreement between different urologists is highest among higher
grade classifications (grade 4 and 5) and the agreement decreases
with decrease grades with the lowest among the lower grades (grade
1 and 2). There were high agreements for grade 3 and 4 but the
agreement is low among the subgroups (grade 3a, 3b, 4a, 4b), which
could be attributed to the use of anesthesia dividing the subgroups.
Even our departments depending on attending’s preference, same
procedures are performed using different anesthesia methods.
Therefore, reporting minor complications in different hospitals with
different cultures will vary significantly. In the article, a more specific
definition between the classifications is formulated for PCNL based
on expert opinions from 74 urologists [13]. Due to the high variable
in the reported complication rate, PCNL complications can be as high
as 83% [6]. Our complication rate of 50% for Amplatz dilator and
40% for balloon dilator includes transient fever and patients whom
experienced extreme pain not controlled with oral medication and
required intravenous or intramuscular injection for pain control
(Table 3). In our study, we combined the subgroups in grade 3 and
4. If we modify our complication per the article by Dr. de la Rosette,
more than 90% of our complications would be classified as grade 1
and only 1.9% (3 patients from each group) of our patients suffered
severe life-threatening complications (grade 4) with no grade 5
complications.
Our combined stone free rate for both group of 76% (75% in
Amplatz dilator and 78% in balloon dilator) is similar to the results
of previous studies [11]. When comparing between the two dilatation
methods, the stone free rate is slightly better for the balloon dilator
(78% and 75%, p=0.59). An explanation would be the stone burden
is much less on average in the balloon dilator group (771 mm2) than
the Amplatz dilator group (1189 mm2). Analyzing the data from the
residual stone patients (Table 5), we can see that the average stone
burden is almost twice than the average (1734 mm2 and 1513 mm2).
In theory, increase surgical experience will improve the stone-free rate
but surgeon’s experience is hard to quantity. Since most of our PCNL
are performed by senior residents, we decided to compare the stone
free rate among the different year of resident training. As the year
of training increases, the stone free rate increases and complication
decreases (Table 5). The improvement of stone-free rate and decrease
in complications could all be attributed to improved intra-operative
instrument manipulation. Previous studies have demonstrated the
importance of instrument manipulation during prone versus supine
PCNL [16,17]. Due to the increase range of instrument manipulation,
prone position resulted in a better stone free rate. An interesting data
in our study showed that surgeons in their Fellowship years had
better stone free rate using the balloon dilator compared to Amplatz
dilator (p<0.05), while the junior residents and attending had similar
stone free rate using either method. This finding seem contradictory
to the previous statement of increase experience will result in higher
stone free rate. But looking at the data closely, the Amplatz dilator
data showed that attending surgeons had the highest stone free rate
(86%). Since attending only has sequential dilators during their
training, the attending surgeons are more familiar with the sequential
Amplatz dilator. On the other hands, balloon dilator is only recently
covered by Taiwan’s National Healthcare Insurance (NIH) in 2014.
Due to the ease of use, the residents preferred dilatation with balloon
dilator which resulted in residents being more familiar with its use
than attending surgeons. The data from Table 5 seems to support
our explanation. NIH also limits the initial survey and follow-up
modality for urolithiasis. Even though guidelines suggest CT scan as
the standard initial image modality, the NIH in Taiwan only allow
intravenous pyelography and renal ultrasound as the initial image
modalities with KUB image as follow-up. All of our patients will have
at least 1 KUB image within 1 month after the procedure to check for
residual stone.
The reported rate of hemorrhagic complications after PCNL
needing blood transfusion ranged from 1% to 17% among different
studies, therefore numerous studies have been trying to identify
variables that increase the chance of hemorrhage [1,6,8,18-22]. In
the CROES global study investigating complications and outcomes
of PCNL, hemorrhagic complication requiring blood transfusion
was about 5% [10]. Variables that have been identified as risk factors
for severe hemorrhage requiring blood transfusion are multiple
punctures, stone burden, surgeon inexperience, operative time,
[8,19,21]. Studies comparing different dilatation methods have not
been able to determine which dilatation method results in higher
hemorrhagic complications [20-23]. In our study period, no patients
required blood transfusion and the hematocrit percentage in both
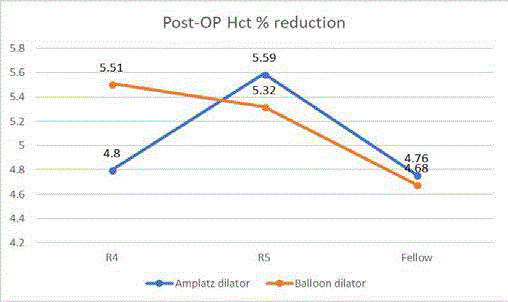
groups were similar (5.3% vs. 5.13%, P=0.81). We did notice a
decrease in hematocrit percentage as the year of training increases
(Figure 1). When creating the dilatation tract, the balloon dilator uses
a spreading force rather than lacerating or tearing the tissues [20,24].
An advantage of balloon dilator is the fast one step dilatation method,
rather than a series of 10-12 dilatations. This advantage is extremely
useful in patients with hypermobile kidney during dilatation. With
the help of the anesthesiology, hypermobility can be corrected but at
the cost of patients experiencing apnea conditions for the duration
of the dilatation process. This can be extremely dangerous in severe
obese patients whom are already in danger for cardiopulmonary
complication during prone position [25]. In our study, we were not
able to quantify that balloon dilator decreases time of tract dilatation
(the time from insertion of guide wire to insertion of working sheath)
but the feedbacks from the residents has been favorable toward
balloon dilator. The time difference between the dilator methods
could be an interesting data in the future studies. An explanation
for longer operative time in the balloon dilator group (95 min vs.
80 min) is surgeon experience. Nearly 50% of primary surgeons in
balloon dilator were 4th and 5th year resident, while 70% of primary
surgeons in the Amplatz dilator were Fellow or Attending. The value
of surgeon experience can be seen in our study by the higher rate
of residual stone, higher change of hematocrit percentage and longer
operative time in junior residents (4th and 5th year trainee) performing
PCNL (Figure 1).
In this prospective study, we demonstrated that balloon dilator
is non -inferior to traditional tract dilatation methods with similar
complication and stone-free rate. After the introduction of PCNL
procedure to our department in the early 2000’s, our case numbers
have progressed to average 150 cases per year from 2007 to 2015
(ranging from 120 to 177 cases/year) which coincide with the
definition of high volume center described in the CROES study (more
than 100 cases/year). Several points would be a good discussion topic
in the future large randomized control trial, such as tract dilatation
time from puncture to insertion of nephrostomy sheath or surgeon
comfort/preference. As endourologist, we need to keep our eyes and
mind open to these new technologies and have an unbiased view
to evaluate the usefulness of their uses to add them to our growing
armamentarium.
References
- Matlaga BR, Krambeck AE, Lingeman JE. Chapter 54: Surgical management of upper urinary tract calculi. Campbell-Walsh Urology. 2016:1260-90.
- Wolf JS. Chapter 47: Percutaneous approaches to the upper urinary tract collecting system. Campbell-Walsh Urology. 2012:1324-56.
- Ferakis N, Stavropoulos M. Mini Percutaneous Nephrolithotomy in the Treatment of renal and upper ureteral stones: Lessons learned from a review of the literature. Urology Annals. 2015;7(2):141-8.
- Desai J, Solanki R. Ultra-mini percutaneous nephrolithotomy (UMP): One more armamentarium. BJU Int. 2013;112(7):1046-9.
- Marcovich R, Smith AD. Percutaneous renal access: Tips and tricks. BJU Int. 2005;95:78-84.
- Michel MS, Trojan L, Rassweiler JJ. Complications in percutaneous nephrolithotomy. Eur Urol. 2007;51(4):899-906.
- Desai J, Zeng G, Zhao Z, Zhong W, Chen W, Wu W. A novel technique of ultra-mini-percutaneous nephrolithotomy: Introduction and an initial experience for treatment of upper urinary calculi less than 2 cm. BioMed Research Int. 2013;2013:6.
- Akman T, Binbay M, Sari E, Yuruk E, Tepeler A, Akcay M, et al. Factors affecting bleeding during PCNL: Single surgeon experience. J Endourol. 2011;25(2):327-33.
- Armitage JN, Irving SO, Burgess NA. British Association of Urological Surgeons Section of Endourology. Percutaneous nephrolithotomy in the United kingdom: Results of a prospective data registry. Eur Urol. 2012;61(6):1188-93.
- de la Rosette J, Assimos D, Desai M, Gutierrez J, Lingeman J, Scarpa R, et al. The Clinical Research Office of the Endourological Society PCNL global study: Indications, complications, and outcomes in 5803 pts. J Endourol. 2011;25(1):11-7.
- Kamphuis GM, Baard J, Westendarp M, de la Rosette JJ. Lessons learned from the CROES percutaneous nephrolithotomy global study. World J Urol. 2015;33(2):223-33.
- Yamaguchi A, Skolarikos A, Buchholz NP, Chomón GB, Grasso M, Saba P, et al. Operating times and bleeding complications in percutaneous nephrolithotomy: a comparison of tract dilation methods in 5,537 patients in the Clinical Research Office of the Endourological Society Percutaneous Nephrolithotomy Global Study. J Endourol. 2011;25(6):933-9.
- de la Rosette JJ, Opondo D, Daels FP, Giusti G, Serrano A, Kandasami SV, et al. Categorisation of complications and validation of the Clavien score for percutaneous nephrolithotomy. Eur Urol. 2012;62(2):246-55.
- Labate G, Modi P, Timoney A, Cormio L, Zhang X, Louie M, et al. The percutaneous nephrolithotomy global study: classification of complications. J Endourol. 2011; 25(8):1275-80.
- Tefekli A, Ali Karadag M, Tepeler K, Sari E, Berberoglu Y, Baykal M, et al. Classification of percutaneous nephrolithotomy complications using the modified clavien grading system: Looking for a standard. Eur Urol. 2008;53(1):184-90.
- Liu L, Zheng S, Xu Y, Wei Q. Systematic Review and Meta-analysis of percutaneous nephrolithotomy for patients in the supine versus prone position. J Endourol. 2010;24(12):1941-6.
- Valdivia JG, Scarpa RM, Duvdevani M, Gross AJ, Nadler RB, Nutahara K, et al. Supine versus prone position during percutaneous nephrolithotomy: A report from the clinical research office of the endourological society percutaneous nephrolithotomy global study. J Endourol. 2011;25(10):1619-25.
- el-Nahas AR, Eraky I, Shokeir AA, Shoma AM, el-Assmy AM, el-Tabey NA, et al. Factors affecting stone-free rate and complications of percutaneous nephrolithotomy for treatment of staghorn stone. Urology. 2012;79(6):1236-41.
- El-Nahas AR, Shokeir AA, El-Assmy AM, Mohsen T, Shoma AM, Eraky I, et al. Post-percutaneous nephrolithotomy extensive hemorrhage: A study of risk factors. J Urol. 2007;177(2):576-9.
- Gönen M, Istanbulluoglu OM, Cicek T, Ozturk B, Ozkardes H. Balloon dilatation versus Amplatz dilatation for nephrostomy tract dilatation. J Endourol. 2008;22(5):901-4.
- Keoghane SR, Cetti RJ, Rogers AE, Walmsley BH. Blood transfusion, embolisation and nephrectomy after percutaneous nephrolithotomy (PCNL). BJU Int. 2013;111(4):628-32.
- Lopes T, Sangam K, Alken P, Barroilhet BS, Saussine C, Shi L, et al. The Clinical Research Office of the Endourological Society Percutaneous Nephrolithotomy Global Study: Tract dilation comparisons in 5537 patients. J Endourol. 2011;25(5):755-62.
- Davidoff R, Bellman GC. Influence of technique of percutaneous tract creation on incidence of renal hemorrhage. J Urol. 1997;157(4):1229-31.
- Al-Kandari AM, Jabbour M, Anderson A, Shokeir AA, Smith AD. Comparative study of degree of renal trauma between amplatz sequential fascial dilation and balloon dilation during percutaneous renal surgery in an animal model. Urology. 2007;69(3):586-9.
- Fuller A, Razvi H, Denstedt JD, Nott L, Pearle M, Cauda F, et al. The CROES percutaneous nephrolithotomy global study: The influence of body mass index on outcome. J Urol. 2012;188(1):138-44.