Research Article
Chronic Mesenteric Ischemia: Long Term Results after Open Surgical Revascularization
Touloumtzidis A1*, Mamopoulos AT1, Lilien-Waldau V2, Zapenko A1, Gäbel G1 and Luther B2
1Department of Vascular Surgery, Helios Klinikum Krefeld, Germany
2Department of Vascular Surgery, Krankenhaus Maria Hilf, Germany
*Corresponding author: Aristotelis Touloumtzidis, Department of Vascular Surgery, Helios Klinikum Krefeld, Germany
Published: 20 Aug, 2018
Cite this article as: Touloumtzidis A, Mamopoulos AT,
Lilien-Waldau V, Zapenko A, Gäbel G,
Luther B. Chronic Mesenteric Ischemia:
Long Term Results after Open Surgical
Revascularization. Clin Surg. 2018; 3:
2080.
Abstract
Objectives: Open Surgical Revascularization (OR) as well as Endovascular Revascularization (ER)
is widely accepted therapeutic concepts concerning Chronic Mesenteric Ischemia (CMI). Nowadays
an increasing number of patients are administrated to ER. To evaluate the significance of OR we
analysed long-term outcomes in patients suffering from CMI in our hospital.
Methods: A retrospective single centre analysis of all patients, who underwent elective OR because
of CMI between 2004 and 2016, was conducted based on quality control data. Primary outcomes
were 30 day mortality and morbidity; secondary outcomes were survival, patency rates and symptom
free survival from digestive disorders.
Results: Eighty-six vessels in 52 patients were revascularized. Number of treated patients per year
remained similar during the observation period. The mean follow-up period amounted 58 ± 43
months. The 30 day mortality was 5,8%, the morbidity 21,1%. Five - year survival was 83,1%. The
primary and secondary patency rates at 5 years were 77,0% and 91,5% respectively. Freedom from
digestive symptoms at five years were achieved in 82,5% of the patients.
Conclusion: In accordance to international centre's OR offers improved rates of patency and
long-term relief from digestive symptoms but is accompanied by a deterioration of morbidity and
mortality. Nevertheless it remains necessary as a tailored approached therapy concept in a subgroup
of patients suffering from CMI.
Keywords: Chronic mesenteric ischemia; Open surgical revascularization; Coeliac trunk; Superior mesenteric artery
Introduction
Despite medical progress, the optimal treatment of Chronic Mesenteric Ischemia (CMI) remains controversial. Available options are the Open Surgical (OR) on the one hand and the Endovascular Revascularization (ER) on the other. Both therapy options are widely accepted in symptomatic patients, to avoid adverse complications like an acute mesenteric ischemia, which may cause bowel infarction and death. Nevertheless ER is rapidly rising due to its low in - hospital morbidity and mortality rates, while most centre's concerning OR a backup plan after failed interventional treatment. The international literature comprises a few series concerning the comparison between OR an ER for CMI, but large series studying long term outcomes associated with OR is rare. Recent meta analysis/reviews show lower in hospital complication rate after ER but decreased patency rates compared to OR, while both techniques comprises similar long - term survival rates [1-3]. Against this background we were lately wondering about the importance and necessity of OR nowadays. The purpose of this report was reviewing the experience with OR in patients suffering from CMI and its development in the course of time from a single centre view.
Methods
A retrospective analysis of all consecutive patients requiring surgical digestive revascularization for CMI between March 2004 and December 2016 was conducted. Patients’ characteristics and data from in - hospital stay and of the patients were analysed from medical records. Inclusion criteria were patients with typical symptoms (postprandial abdominal pain, food fear, weight loss) and/or endoscopic signs of gastric or intestinal ulcerations in combination with an at least 70% or higher significant stenosis of one or more digestive arteries. Grad of stenosis was assessed by duplex ultrasound and CT angiography or contrast - enhanced MR angiography, whenever the diagnosis was not clear additional digital subtraction angiography was performed. Preoperative demographic data, comorbidities and cardiovascular risk factors were recorded as well as performed surgical procedures. Peri - and postoperative complications were graded in accordance to Clavien - Dindo Classification [4]. Patients treated for arcuate ligament syndrome, non-occlusive visceral ischemia, acute or acute-on-chronic visceral ischemia and treatment in combination with another aortic procedure without CMI symptoms were excluded. Further exclusion criteria were prior operations of visceral arteries, high perioperative risk and contraindication for general anaesthesia. Follow-up examinations were conducted at 30 days, 6 months and annually thereafter. Duplex ultrasound was performed in each and CT angiography in non - conclusive cases. Survival, primary and secondary patency as well as freedom from digestive symptoms were analysed. The total statistical evaluation was performed with Microsoft Excel und SPSS® Version 24.0. For categorical data results are presented as frequency distribution and percentage, while continuous data are show as mean ± SD. Survival, primary patency, secondary patency and freedom from digestive symptoms rates were calculated by Kaplan - Meier - method.
Figure 1
Figure 2
Figure 3
Table 1
Results
Patients’ characteristics: Fifty-two patients, 30 women and 22
men with a median age of 62 ± 14 years were included. Mean follow
up was 58 ± 42 months; four patients were lost to follow-up. The
numbers of treated patients per year remained approximately equal
(~4 per year). Incidence of common cardiovascular risk factors were
hypertension in 38 patients (73,1%), hyperlipidemia in 23 patients
(44,2%), coronary artery disease in 18 patients (34,6%), cardiac
arrhythmia and peripheral vascular disease in 11 patients (21,2%),
chronic renal insufficiency in 10 patients (19,2%), diabetes mellitus
in 9 patients (17,3%), pulmonary disease in 8 patients (15,4%) and
current nicotine abuse in 7 patients (13,5%). Regarding typical
symptoms, postprandial pain was present in 44 patients (84,6%),
weight loss as well as food fear in 37 patients (71,2%) and gastric or
intestinal ulceration in 11 patients (21,2%). Mean weight loss was 13
± 8 kg. Mean preoperative body mass index amounted 21± 4 kg/m2.
An overview concerning demographic patient's data, symptoms and
risk factors can be derived from (Table 1).
Perioperative Data: Numbers of pathological digestive arteries
were one in 10 patients (19,2%), two in 30 patients (57,7%) and
three in 12 patients (23,1%). The amount of treated arteries were
one in 20 patients (38,4%), two in 30 patients (57,7%) and three in 2
patients (3,9%) an overall of 86 vessels were revascularized. Extend of
mesenteric disease and corresponding reconstruction are described in
(Table 2). Type of performed operation were an aorto-TC bypass in 23
cases (26,7%), aorto-SMA bypass in 21 cases (24,4%), reimplantation
of TC and SMA in 3 (3,6%) and 16 (18,6%) cases respectively, TC
and SMA thrombendarterectomy each in 10 cases (11,6%) and AMI
thrombendarterectomy in 2 cases (2,3%). One retrograde bypass was
performed due to heavy calcification of the celiac part of the aorta,
without technical possibility of safe clamping. Operation time was
136 ± 49 mins. Mean hospital stay and mean stay on the intensive care
unit were respectively 11 ± 8 and 1 ± 8 days. Overall postoperative
morbidity, according to the Clavien - Dindo - Classification stadium
III or higher, amounted 21,1%, whereas 30 - day - mortality was 5,8%
(Table 3). One patient died from bypass occlusion with consecutive
bowel infarction on day 18. One patient due to duodenal perforation
with massive gastrointestinal bleeding on day 20 and another one
from heart failure on day 24.
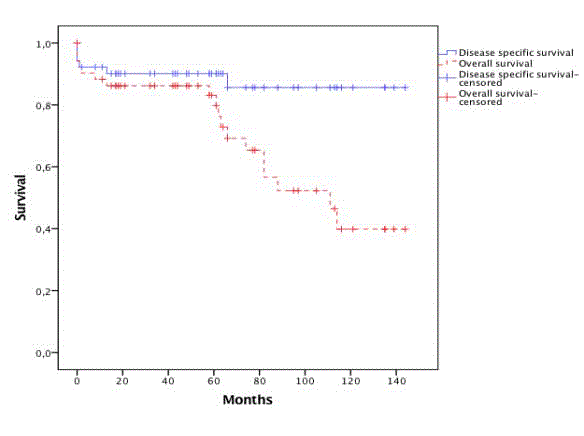
Long term results: Overall Survival rate was 83,1% at 5 years,
while disease specific survival rate (patients who have not died from
CMI or a perioperative complication) was 90,1% at 5 years (Figure
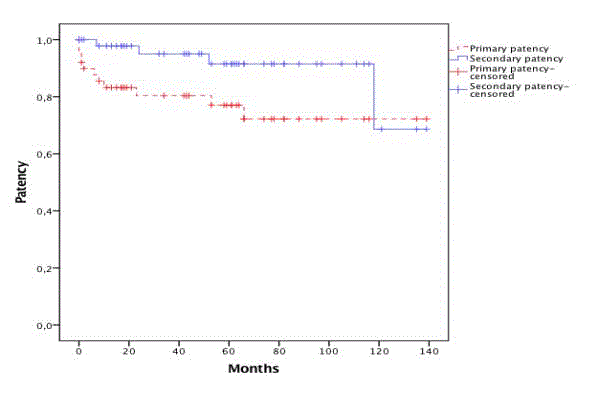
1). Primary patency rate was 77,0% at 5 years, secondary patency rate
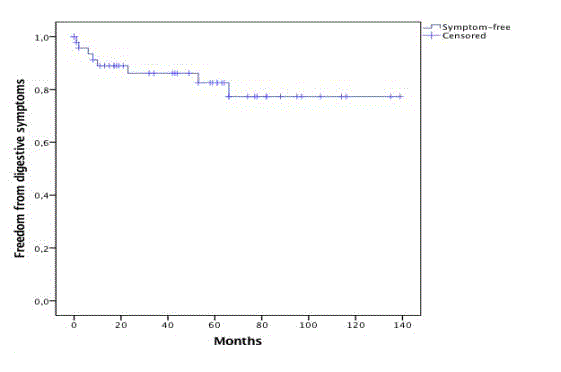
was 91,5% at 5 years (Figure 2). Freedoms from digestive symptoms
have been achieved in 82,5% at 5 years (Figure 3). Mean weight gain
was 6 ± 7 kg.
Table 2
Discussion
Diseases of the mesenteric arteries are relatively rare in comparison to other occlusive arterial entities. Therefore, prospective randomized controlled studies concerning open surgical therapy especially in a long - term follow-up setting are rare or surprises weak numbers of patients. Subsequently the decision - making process is not sustained by strong evidence and numerous question (vascular accesses, surgical technique, types of revascularisation, source of inflow - vessel) remain unanswered. Treatment strategies on diseases of the mesenteric arteries and veins have been recently publish in 2017 by the European Society of Vascular Surgery (ESVS) and also comprise recommendations regarding patients suffering from CMI [6]. Most of the studies on treatment of CMI, especially those containing large numbers of patients report in hospital outcomes, while just a few series comprises long term data of performed mesenteric revascularisation [7,8]. Concerning the comparison between OR and ER for CMI even recent reviews were inhomogeneous. While all meta - analysis shown decreased patency rates of ER compared to OR and both techniques comprises similar long - term survival rates there are divergent descriptions about the in hospital stay [1,3]. While Pecorar et al. [3] stated a lower in hospital complication rate after ER in contrast to the findings of Seadon et al. [1] and Can et al. [2], the study group of Tallarita et al. [9] showed, by using propensity score match comparisons, that 5 year patient survival was not influenced by the type of revascularization (OR or ER). Decision making of patient administration to either OR or ER consequently requires large prospective randomized studies but remains unrealistic due to low incidence of chronic mesenteric ischemia and patients suitable for both types of repair. Nevertheless the purpose of this study was not to compare OR versus ER or establish a new administration - process to the one or the other type of revascularization, but to evaluate the long - term results and preferred technique of OR, which is described below. Allocation of patients to either open OR or ER in this study was based on an interdisciplinary team approach; we were able to report an approximately equal number of treated patients over the last 13 year with over 80% classificated as ASA 3 or 4 and a mean age of 62 ± 14 years. Perioperative morbidity and mortality remains high after OR in comparison to ER amounting 13% to 42% and respectively 2% to 13%. The result a of the present study (morbidity 21,1% and mortality 5,8%) are therefore comparable to rates found in the international literature concerning outcomes of CMI after OR [9,11-25]. Even though they are hardly comparable towards morbidity given the fact, that their evaluation are inconsistent, because of heterogeneous classification systems or different cutoffs in the same classification system. Actually there is no doubt about the superior durability of OR in comparison to ER but controversy remains about the extent of performed OR (single or multiple vessel - revascularisation). While some authors pointed out an positive impact of multiple vessel revascularisation on long - time freedom from digestive symptoms others could not recognize any significant difference in primary or secondary patency rates type of revascularization [11,12]. Depending on our own experience, we recommend a multiple - vessel approach if both, the TC and the SMA are involved. Even though we could not observe a difference in long - term follow-up between single or multiple vessel - revascularisation, we had at least two patients after 2 - vessel - revascularisation with an re - occlusion of the SMA but still patent TC, which had no signs of recurrent digestive symptoms and therefore weren’t in need of any further interventions. Regarding the type of revascularization over the last years we have changed our concept from reimplantation of the TC or SMA to a mainly use of antegrade aorto - celiac/mesenterial - bypass implantation. Also there is no evidence in international literature, that the different types of revascularization have a significant influence on long - time patency rates, in the present study out of an overall of 11 occlusion 7 occurred in the reimplantation group (1x TC, 6x SMA) [11,12]. Which leads us to an primary patency rate of 77,0% at 5 years (72,2% at 10 years) and a secondary patency rate of 91,5% at 5 years (68,6% at 10 years). While international literature comprises primary and secondary patency - rates which vary between 57% and 88% for 5 - year primary and respectively 83% and 100% in terms of secondary patency rates [12-15,21,22,24]. Astonishingly in this study we could observe a detoriation of the secondary patency in comparison to the primary patency rate at 10 year, the cause was a late occlusion of an already operative revised reinserted TC 118 month after the initial operation. Also long-time - survival rates seems to be independent of type of revascularization. In this context several studies have reported long term results for CMI after OR with overall 5 - year - survival rates between 64% and 77% [9,11,12,14,15,22-25] and 5 - year - freedom from digestive symptoms in 57% to 92% [12,13,15,21,23,24] which are comparable to our own data. A review regarding in - hospital and long - term results after open surgical treatment of CMI can be established from (Table 4). The present study has several limitations like its retrospective non - randomized single - centre character. To mention is also the long study period with approximately 4 patients operated on every year, due to the low incidence of symptomatic CMI. During this period of time there has been significant progresses' concerning medical, surgical a perioperative therapy that possibly could have affected patients outcomes. Furthermore the significance is limited by the size of the patient collective only 52 patient's respectively 86 revascularized vessels could be analysed. In long term follow - up the numbers of patients at risk is even smaller and could lead to a severe falsification like we discussed it previously with regards to primary and secondary patency - rates.
Table 3
Table 4
Conclusion
In accordance to international centre's OR offers improved rates of patency and long - term relief from digestive symptoms but is accompanied by a deterioration of morbidity and mortality. Nevertheless it remains necessary as a tailored approached therapy concept in a subgroup of patients suffering from CMI, given the fact, that the numbers of patients per year, in need of an OR, remained approximately equal. Furthermore we recommend fit patients with suitable anatomy to be considered for OR instead of a categorical administration to ER at first presentation. In accordance to our own data we prefer a multiple vessel revascularization using an antegrade aorto - celiac/mesenterial - bypass technique whenever possible.
References
- Saedon M, Saratzis A, Karim A, Goodyear S. Endovascular Versus Surgical Revascularization for the Management of Chronic Mesenteric Ischemia. Vasc Endovascular Surg. 2015;49(1-2):37-44.
- Cai W, Li X, Shu C, Qiu J, Fang K, Li M, et al. Comparison of clinical outcomes of endovascular versus open revascularization for chronic mesenteric ischemia: a meta-analysis. Ann Vasc Surg. 2015;29(5):934-40.
- Pecoraro F, Rancic Z, Lachat M, Mayer D, Amann-Vesti B, Pfammatter T, Bajardi G, Veith FJ. Chronic mesenteric ischemia: critical review and guidelines for management. Ann Vasc Surg. 2013;27(1):113-22.
- Dindo D, Demartines N, Clavien PA. Classification of Surgical Complications: A New Proposal With Evaluation in a Cohort of 6336 Patients and Results of a Survey. Ann Surg. 2004; 240(2): 205-13.
- Fitz-Henry J. The ASA classification and peri-operative risk. Ann R Coll Surg Engl. 2011;93(3):185-7.
- Björck M, Koelemay M, Acosta S, Bastos Goncalves F, Kölbel T, Kolkman JJ, et al. Editor's Choice - Management of the Diseases of Mesenteric Arteries and Veins: Clinical Practice Guidelines of the European Society of Vascular Surgery (ESVS). Eur J Vasc Endovasc Surg. 2017;53(4):460-510.
- Schermerhorn ML, Giles KA, Hamdan AD, Wyers MC, Pomposelli FB. Mesenteric revascularization: management and outcomes in the United States, 1988-2006. J Vasc Surg. 2009;50(2):341-348.
- Indes JE, Giacovelli JK, Muhs BE, Sosa JA, Dardik A. Outcomes of endovascular and open treatment for chronic mesenteric ischemia. J Endovasc Ther. 2009;16(5):624-30.
- Tallarita T, Oderich GS, Gloviczki P, Duncan AA, Kalra M, Cha S, Misra S, Bower TC. Patient survival after open and endovascular mesenteric revascularization for chronic mesenteric ischemia. J Vasc Surg. 2013;57(3):747-55.
- Oderich GS1, Erdoes LS, Lesar C, Mendes BC, Gloviczki P, Cha S, et al. Comparison of covered stents versus bare metal stents for treatment of chronic atherosclerotic mesenteric arterial disease. Vasc Surg. 2013;58(5):1316-23.
- Wagenhäuser MU, Meyer-Janiszewski YK, Dueppers P, Spin JM, Floros N, Schelzig H, et al. Chronic Mesenteric Ischemia: Patient Outcomes Using Open Surgical Revascularization. Dig Surg. 2017;34(4):340-49.
- Lejay A, Georg Y, Tartaglia E, Creton O, Lucereau B, Thaveau F, et al. Chronic mesenteric ischemia: 20 year experience of open surgical treatment. Eur J Vasc Endovasc Surg. 2015;49(5):587-92.
- Arya S, Kingman S, Knepper JP, Eliason JL, Henke PK, Rectenwald JE. Open Mesenteric Interventions Are Equally Safe as Endovascular Interventions and Offer Better Midterm Patency for Chronic Mesenteric Ischemia. Ann Vasc Surg. 2016;30:219-26.
- Rawat N, Gibbons CP, Joint Vascular Research Group. Surgical or endovascular treatment for chronic mesenteric ischemia: a multicenter study. Ann Vasc Surg. 2010;24(7):935-45.
- Oderich GS, Bower TC, Sullivan TM, Bjarnason H, Cha S, Gloviczki P. Open versus endovascular revascularization for chronic mesenteric ischemia: risk-stratified outcomes. J Vasc Surg. 2009;49(6):1472-9.
- Davies RS, Wall ML, Silverman SH, Simms MH, Vohra RK, Bradbury AW, et al. Surgical versus endovascular reconstruction for chronic mesenteric ischemia: a contemporary UK series. Vasc Endovascular Surg. 2009;43(2):157-64.
- Zerbib P, Lebuffe G, Sergent-Baudson G, Chamatan A, Massouille D, Lions C, et al . Endovascular versus open revascularization for chronic mesenteric ischemia: a comparative study. Langenbecks Arch Surg. 2008;393(6):865-70.
- Atkins MD, Kwolek CJ, LaMuraglia GM, Brewster DC, Chung TK, Cambria RP. Surgical revascularization versus endovascular therapy for chronic mesenteric ischemia: a comparative experience. J Vasc Surg. 2007;45(6):1162-71.
- Biebl M, Oldenburg WA, Paz-Fumagalli R, McKinney JM, Hakaim AG. Surgical and interventional visceral revascularization for the treatment of chronic mesenteric ischemia--when to prefer which? World J Surg. 2007;31(3):562-8.
- Sivamurthy N, Rhodes JM, Lee D, Waldman DL, Green RM, Davies MG. Endovascular versus open mesenteric revascularization: immediate benefits do not equate with short-term functional outcomes. J Am Coll Surg. 2006;202(6):859-67.
- English WP, Pearce JD, Craven TE, Edwards MS, Geary RL, Plonk GW, et al. Chronic visceral ischemia: symptom-free survival after open surgical repair. Vasc Endovascular Surg. 2004;38(6):493-503.
- Jimenez JG, Huber TS, Ozaki CK, Flynn TC, Berceli SA, Lee WA, Seeger JM. Durability of antegrade synthetic aortomesenteric bypass for chronic mesenteric ischemia. J Vasc Surg. 2002;35(6):1078-84.
- Park WM, Cherry KJ Jr, Chua HK, Clark RC, Jenkins G, Harmsen WS, et al. Current results of open revascularization for chronic mesenteric ischemia: a standard for comparison. J Vasc Surg. 2002;35(5):853-9.
- Cho JS, Carr JA, Jacobsen G, Shepard AD, Nypaver TJ, Reddy DJ. Long-term outcome after mesenteric artery reconstruction: a 37-year experience. J Vasc Surg. 2002;35(3):453-60.
- Kasirajan K, O'Hara PJ, Gray BH, Hertzer NR, Clair DG, Greenberg RK, et al. Chronic mesenteric ischemia: open surgery versus percutaneous angioplasty and stenting. J Vasc Surg. 2001;33(1):63-71.