Case Report
Primary Popliteal Vein Aneurysm
Gary K Yang and York N Hsiang*
Department of Surgery, Division of Vascular Surgery, University of British Columbia, Vancouver, Canada
*Corresponding author: York N Hsiang, Department of Surgery, Division of Vascular Surgery, University of British Columbia, Vancouver, BC, Canada
Published: 16 Aug, 2018
Cite this article as: Yang GK, Hsiang YN. Primary Popliteal
Vein Aneurysm. Clin Surg. 2018; 3:
2076.
Abstract
Primary venous aneurysms in the absence of arteriovenous fistula, venous hypertension or occlusion are rare. The main risks are thromboembolic events. Currently, no consensus exists for the management of primary venous aneurysms. We report one case of venous aneurysm involving the left popliteal vein. Surgical repair with an inter-positional polytetrafluoroethylene graft were performed, respectively. The patient had an uneventful recovery and was clinically well at the time of this report.
Introduction
Venous aneurysms are rare occurrences with potentially significant complications of thromboembolic events. Primary venous aneurysms, defined by the absence of arteriovenous fistula, venous hypertension and venous occlusion [1], are even less commonly reported. Given the rarity of venous aneurysms, consensus on management has not been reached due to the lack of well-designed experimental studies. Risks associated with untreated venous aneurysms include nerve compression, thromboembolism and rupture. However, the significance of these risks is unclear. Current management plans include expectant monitoring, medical management with anticoagulation and surgical repair. In this report, we present a case of primary popliteal venous aneurysm.
Case Presentation
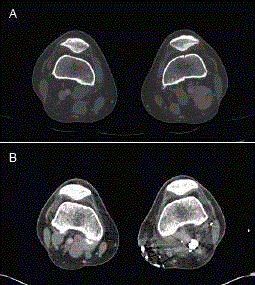
A 47-year-old woman presented for evaluation and management of superficial thrombophlebitis of the left short saphenous vein. The patient’s medical history was unremarkable apart from controlled hypertension. Her only medication was daily ASA. Clinical examination and further evaluation with ultrasound and CT venography, revealed a large fusiform popliteal vein aneurysm (PVA), measuring 3.4 cm x 2.9 cm. It contained intramural thrombus as well as a heterogenous vascular malformation within the distal hamstring muscle (Figure 1A). In consideration of the risk of thromboembolic complications, interim treatment with warfarin was initially recommended. However, following further discussion with the patient regarding definitive management options, the patient agreed to have surgical repair. The patient underwent general anesthesia and the popliteal fossa was accessed through a single longitudinal incision on the medial aspect of the left lower thigh, in the space anterior to the Sartorius muscle. The popliteal artery and venous aneurysm were identified. Proximal and distal control of the aneurysm was achieved by controlling the femoral vein in the mid-thigh level and popliteal vein distal to the aneurysm. For exposure, the medial head of the gastrocnemius muscle was divided and the popliteal artery was separated from the aneurysm by dividing its geniculate branches. The patient was heparinized and the aneurysm incised and noted to be irregular in external morphology and extremely thin-walled. Because of this, the aneurysm was excised and a 10 mm PTFE graft used as a replacement conduit. The decision for graft replacement rather than aneurysmectomy with lateral venorrhaphy was based on the likelihood of future recurrence or thrombosis if the latter was used as the reconstruction method. Thus, both proximal and distal anastomoses were configured in an end-to-end manner. Following clamp release, Doppler examination confirmed venous flow. At six months, the patient was clinically well with no significant swelling in the ipsilateral leg. Her follow up CT scan showed the graft to be patent (Figure 1B).
Discussion
There is no consensus or criteria with regards to size in defining venous aneurysms. Persistent isolated dilatation of one and a half [2], two [3] or three [4] times more than the native vein have all been utilized in previous literatures. Others have suggested that true venous aneurysms should have normal venous segments on both ends and to be distinguished from a large varicose vein; however, in practice this distinction is difficult to achieve. In the case presented here, the aneurysm diameter was more than three times the normal size. Normal venous segments also surround the aneurysm although we do not possess histological confirmation. PVAs are rare. Since its first description in 1968, there have only been around 150 reported cases [5-7]. Venous aneurysms have also been reported in other anatomical locations as summarized by a recent systematic review: 35 head and neck, 42 thoracic, 152 intraabdominal and 279 extremities [8]. PVAs are thought to arise from congenital malformations such as Klippel-Trenaunay syndrome [9]. With local degenerative changes, they pose a risk for thromboembolism [9]. Histologically, evidence of decreased smooth muscle cells in the media with a thickened and fibrous intima may be present [4]. These histological changes were similarly observed in our case where uneven distribution of smooth muscle, fibrous and elastic tissue were seen (Figure 2). The majorities of PVAs are asymptomatic but still pose a life-threatening risk especially when intraluminal thrombus is identified [4]. Clinical presentations of PVAs include symptoms related to chronic venous disease, local mass effect and thromboembolic events [10]. Stroke as a result of paradoxical embolus has also been described [11,12]. The risk of rupture, however, is likely low for PVAs and has never been reported [4]. Management of primary venous aneurysms ranges from monitoring to medical anticoagulation to surgical treatment. Nasr et al. showed a 43% failure rate in preventing thromboembolism in patients with PVAs when treated with anticoagulation alone [10]. However, there is no consensus or sufficient data to support each approach and treatment should depend on patient-, physicianand center-specific factors. Anticoagulation may reduce the risk of thromboembolism but may theoretically worsen the outcome in the event of aneurysmal rupture. Primary venorrhaphy can be done if the aneurysm wall appears to be of good integrity. In our case, intraoperative findings of a severely diseased venous wall dictated the use of an interpositional PTFE graft. The role of post-op anticoagulation following asymptomatic primary venous aneurysm repair is unclear. While some reports suggested oral anticoagulation between 3-12 months, compression stocking use or lifelong ASA [13-16], there is currently no data to support any benefit. Oral anticoagulation was not initiated in our case but the patient remained on 81mg of aspirin daily.
Figure 1
Figure 1
Left popliteal venous aneurysm in a 47-year-old female. Aneurysm was fusiform measuring 10 cm in length with a cross-section shown measuring 3.4 cm x 2.9 cm (A). Six months post-operative scan reveals that the PTFE graft was patent (B). a = popliteal artery; v = popliteal vein; g = PTFE graft.
Figure 2
Figure 2
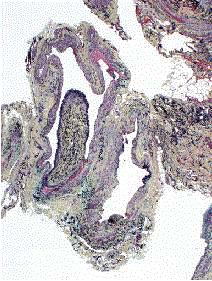
Histological slide of the excised aneurysm demonstrates a
thickened and fibrous intima with an uneven distribution of smooth muscle
cells in the media.
Conclusion
Although rare, primary venous aneurysms are potentially life threatening. Most recently reported cases chose surgical treatment given the potential risk of thromboembolism and rupture. However, the scarcity of these cases poses an ongoing challenge not only in their classification but also in establishing evidence-based guidelines in their management. As imaging modalities become more utilized in the primary care setting, there may be more peripheral venous aneurysms discovered to help build a database and clinical experience around this entity.
Acknowledgement
The authors thank Dr. John English for his assistance in analyzing the histological slides.
References
- Abbott OA, Leigh TF. Aneurysmal Dilatations of the Superior Vena Caval System. Ann Surg. 1964;159(6):858-872.
- Chen SI, Clouse WD, Bowser AN, Rasmussen TE. Superficial venous aneurysms of the small saphenous vein. J Vasc Surg. 2009;50(3):644-647.
- McDevitt DT, Lohr JM, Martin KD, Welling RE, Sampson MG. Bilateral popliteal vein aneurysms. Ann Vasc Surg. 1993;7(3):282-286.
- Sessa C, Nicolini P, Perrin M, Farah I, Magne JL, Guidicelli H. Management of symptomatic and asymptomatic popliteal venous aneurysms: a retrospective analysis of 25 patients and review of the literature. J Vasc Surg. 2000;32(5):902-912.
- Tomko T, Maly R, Jiska S, Chovanec V. Popliteal venous aneurysm as a cause of recurrent pulmonary embolism. Vasc Endovascular Surg. 2013;47(2):155-158.
- Gabrielli R, Vitale S, Costanzo A, Carra A. Our experience of popliteal vein aneurysm. Interact Cardiovasc Thorac Surg. 2010;11(6):835-837.
- Bergqvist D, Bjorck M, Ljungman C. Popliteal venous aneurysm--a systematic review. World J Surg. 2006;30(3):273-279.
- Teter KA, Maldonado TM, Adelman MA. A systematic review of venous aneurysms by anatomic location. J Vasc Surg Venous Lymphat Disord. 2018;6(3):408-413.
- Gillespie DL, Villavicencio JL, Gallagher C, Chang A, Hamelink JK, Fiala LA, et al. Presentation and management of venous aneurysms. J Vasc Surg. 1997;26(5):845-852.
- Nasr W, Babbitt R, Eslami MH. Popliteal vein aneurysm: a case report and review of literature. Vasc Endovascular Surg. 2007;41(6):551-555.
- Willinek WA, Strunk H, Born M, Remig J, Becher H, Schild H. Popliteal venous aneurysm with paradoxical embolization in a patient with patent foramen ovale. Circulation. 2001;104(12):E60-E61.
- Manthey J, Munderloh KH, Mautner JP, Kohl M, Frohlich G. Popliteal venous aneurysm with pulmonary and paradoxical embolization. Vasa. 1994;23(3):264-267.
- Fiori R, Chiappa R, Gaspari E, Simonetti G. A rare case of popliteal venous aneurysm. Case Rep Med. 2010;2010:579256.
- Banno H, Yamanouchi D, Fujita H, Nagata J, Kobayashi M, Matsushita M, et al. External iliac venous aneurysm in a pregnant woman: a case report. J Vasc Surg. 2004;40(1):174-178.
- Forsberg JO, Bark T, Lindholmer C. Non-traumatic rupture of the iliac vein. Eur J Vasc Surg. 1988;2(4):267-268.
- Fourneau I, Reynders-Frederix V, Lacroix H, Nevelsteen A, Suy R. Aneurysm of the iliofemoral vein. Ann Vasc Surg. 1998;12(6):605-608.