Research Article
Can the External Carotid Artery Be Securely Ligated using the BRIG Technique in the Treatment of Carotid Disease?
Philippe De Vleeschauwer1*, Thomas Van den Broeck1,2, Steven Vissers3, Johan Debeuf3, Koen De Feyter2 and Peter Waets2
1Department of Thoracic Vascular Surgery, Heilig Hart Ziekenhuis, Lier, Belgium
2Department of Urology, University Hospitals Leuven, Leuven, Belgium
3Department of Anesthesiology, Heilig Hart Ziekenhuis, Lier, Belgium
*Corresponding author: Philippe De Vleeschauwer, Department of Thoracic Vascular Surgery, Heilig Hart Ziekenhuis, Mechelsestraat, 2500 Lier, Belgium
Published: 16 Aug, 2018
Cite this article as: De Vleeschauwer P, Van den Broeck
T, Vissers S, Debeuf J, De Feyter K,
Waets P. Can the External Carotid
Artery Be Securely Ligated using the
BRIG Technique in the Treatment of
Carotid Disease?. Clin Surg. 2018; 3:
2073.
Abstract
Introduction: Ligating the external carotid artery during carotid artery surgery remains a debatable
act for many surgeons due to the potential impact of facial arterial blood supply. However, in our
previous report on the BRIG technique to treat carotid disease, only one patient developed jaw
claudicating and no other symptoms of facial hypo-perfusion. The goal of this study is to scientifically
substantiate these clinical findings by determining the impact of interruption and restoration of the
carotid blood flow on the External Carotid Artery Stump Pressure (ECASP).
Methods: A prospective proof-of-concept study was performed, including nine consecutive patients
who underwent BRIG surgery for symptomatic ICA stenosis or asymptomatic high grade ICA
stenosis. A Javid shunt was used to measure the ECASP and the CASP during the procedure. An
arterial line was used to measure systemic blood pressure. To compare the ECASP during clamping
and after the restoration of ICA blood flow, multiple Students’ T-testing was performed, correcting
for multiple testing using the Holm-Sidak method.
Results: ECASP and ECASP /BP index did not significantly change during clamping of the
carotid bifurcation and after restoration of cerebral blood. Both CASP and ECASP did not change
significantly during clamping of the common carotid artery.
Conclusion: The internal carotid artery does not influence the ECASP and no high blood pressure
needs to be present in the ECA for it to be functional. Based on these findings, we can conclude that
the ECA can be safely ligated during the BRIG procedure.
Keywords: Carotid artery; Carotid disease; ECASP
Introduction
Currently, the gold standard surgical treatment of carotid artery stenosis is the classical carotid
endarterectomy. Upon restenosis, the resection of the carotid bifurcation and interposition of a
graft is often considered [1].
However, previously we proposed the use of the BRIG surgical technique for carotid artery
disease, in which a PTFE graft is interposed and the external carotid artery is ligated. This technique
in the primary treatment setting of carotid artery disease has shown excellent outcomes with limited
comorbidity and a potential reduction in healthcare costs [2,3]. Nevertheless, the ligation of the
external carotid artery, which is inherent to this procedure, remains a debatable act for many
surgeons due to the potential impact of facial arterial blood supply. However, in our previous series
of 153 patients that underwent BRIG treatment, only one patient had jaw claudication. Not a single
patient had any other signs of facial hypo-perfusion 5 years after treatment. Importantly, none of the
patients undergoing BRIG surgery underwent bilateral ligation of the ECA. If surgery was necessary
bilaterally, on the least affected side a bifurcated graft was interposed, which was performed in 9.4%
of previously described cases [3] (Figure 1A, 1B).
The goal of this study is to scientifically substantiate these clinical findings by determining the
impact of interruption and restoration of the carotid blood flow on the External Carotid Artery
Stump Pressure (ECASP). The measurement of the internal Carotid Artery Stump Pressure (CASP)
is a simple, widely used method to assess cerebral hemispheric collateral blood flow during carotid
surgery and is used to decide whether temporary shunting of the clamped carotid might be required
to prevent hemodynamic stroke. We are the first to investigate the External Carotid Artery Stump
Pressure (ECASP) as a surrogate for facial perfusion.
Figure 1
Figure 1
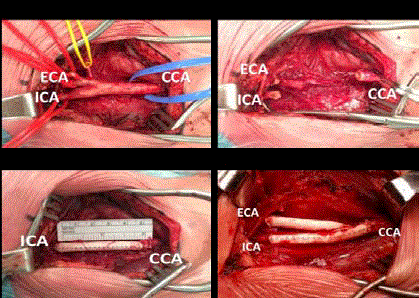
Perioperative images of carotid artery bifurcation (A) before and
(B) after resection of the bifurcation. Surgical repair is shown for (C) classical
BRIG repair with ligation of the ECA and (D) for BRIG using a bifurcated
PTFE graft.
ECA: External Carotid Artery; ICA: Internal Carotid Artery; CCA: Communal
Carotid Artery
Methods
Cohort design and carotid artery stump pressure
measurements
A prospective proof-of-concept study was performed, including
nine consecutive patients who underwent BRIG surgery for
symptomatic ICA stenosis or asymptomatic high grade ICA stenosis.
All patients signed informed consent for the conduction of the
surgical procedure to be performed under general anesthesia.
All the patients had a radial arterial line for monitoring of the
systemic blood pressure. Systemic heparin was given before clamping
the carotid bifurcation. The carotid bifurcation was clamped and the
external carotid artery was ligated at his origin. AJavid shunt was
used to measure the ECASP and the CASP during the procedure.
Simultaneously, the systemic Blood Pressure (BP) and mean
systemic BP were registered. After respecting the carotid bifurcation,
revascularization of the internal carotid artery was obtained by the
interposition of a 6 mm PTFE graft as previously described [3]. A
shunt was never used; even if the CASP was <50 mmHg. At the
time of clamping, the systemic blood pressure was augmented to be
approximately 10% above the patient’s baseline blood pressure. After
restoration of the cerebral circulation, the ECASP, systolic/diastolic/
mean systemic BP was measured again. At the end of the procedure,
heparin was neutralized by administration of protamine and the
patient was transferred to the ICU for a maximum of 24 hr.
Statistical analysis
To compare the ECASP during clamping and after the restoration
of ICA blood flow, the mean values were compared for systolic,
diastolic and mean pressure. To account for inter patient differences
in systemic blood pressure which can influence the (E)CASP, the
ECASP was normalized to systemic pressure (ECASP Index). ECASP
was also compared to the CASP. These multiple comparisons between
two groups were performed using multiple Student’s T-testing,
correcting for multiple testing using the Holm-Sidak method.
Statistical analyses and graph design were performed in Prism v7.0
considering a statistical significance at p<0.05.
Results
In this prospective study 9 patients were included (8 men and 1 woman) with a mean age of 70 years (range 89-62 yrs). Four patients underwent surgery for a symptomatic stenosis and 5 for an asymptomatic high gradestenosis. The preoperative morbidity and mortality was 0%. ECASP measurement during clamping of the carotid bifurcation and after restoration of cerebral blood flow did not show any significant changes in ECASP levels as did the ECASP Index (Figure 2A,2B). Next, the CASP and ECASP were compared during clamping of the common carotid artery, which did not show a significant difference, although two patients did have a lower ECASP compared to their CASP (Figure 2C). Finally, in two patients a Javid shunt was placed between the common and external carotid artery after resection of the carotid bulb. The CASP was measured during clamping of the common carotid artery and after the placement of the Javid shunt, which did not result in an increase of the CASP.
Figure 2
Figure 2
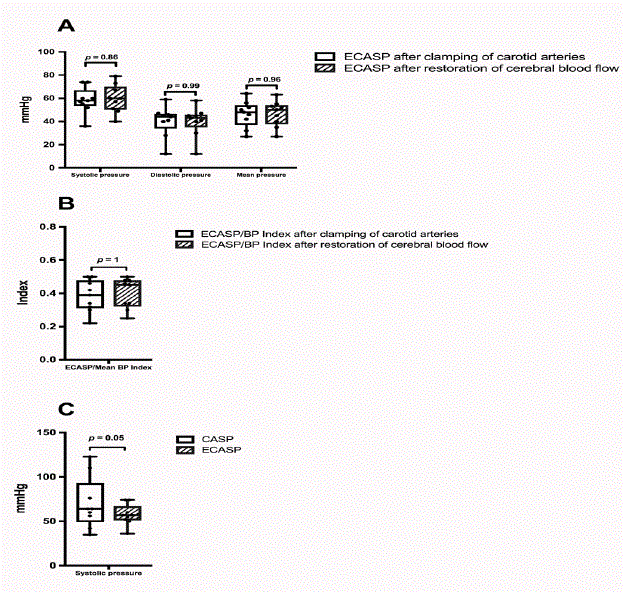
Box and Whiskers plot comparing the ECASP when the carotid
arteries are clamped (white boxes) or when cerebral blood-flow is restored
(filled boxes) for (A) systolic, diastolic and mean ECASP and (B) for the
index (ECASP divided by the mean systemic blood pressure). (C) Systolic
CASP (white boxes) and ECASP (filled boxes) when common carotid artery
is clamped. The individual black dots are the individual measurements; NS:
Not Significant; mmHg: Millimeters of Mercury
Discussion
This small prospective study investigated the impact of the
ligation of the external carotid artery on the ECASP as a surrogate
for facial perfusion. Our previously reported outcome results after
BRIG treatment compared to classical carotid endarterectomy are
encouraging, with lower rates of hospital mortality and morbidity
rates as well as the lower rates of restenosis at long-term follow-up [3].
However, the ligation of the ECA, which is inherent to this procedure,
remains a point of discussion for many surgeons due to the potential
impact that it could influence induce facial hypo-perfusion with
functional impact such as jaw claudication. However, in our previous
study only one of the 153 included patients developed jaw claudication
while eating after more than 5 years of follow-up. Furthermore, the
potential advantages of the BRIG cannot be denied: a) removal of
the sick part of the carotid artery, b) absence of a bifurcation and
consequently turbulences, which can be responsible for restenosis,
c) shorter clamping time of the ICA, d) simplified technique in case
of coiling/kinking of the ICA, e) less surface thrombogenicity of the
PTFE graft compared to the CEA, f) no meticulous endarterectomy
and fixation of the distal intima.
Based on the presented data, it can be hypothesized that when
the external carotid artery is ligated, its effect on facial perfusion is
limited which would explain why only one of our patients undergoing
BRIG surgery develop jaw claudication. Experimental ligation of the
external carotid artery in Chacma baboons did show a decrease in
maxillary blood flow of 40% and 73% when ligated below and above
the origin of the lingulofacial trunk respectively [4]. Furthermore,
some case-reports exist on jaw claudication in the presence of an
occluded or ligated external carotid artery, but data remains limited
and it seems that this only occurs when both sides are affected or
without a functional Circle of Willis [5,6]. This is supported by a case
report of a patient with jaw claudication based on bilateral external
several external carotid artery stenoses, which was resolved by
unilateral endarterectomy [7].
This phenomenon can be explained by multiple hypotheses. First,
it is known that multiple small arteries connect the ICA and ECA,
which mainly goes through the ophthalmic artery [8]. Furthermore,
frequently anastomoses exist between the occipital artery (branch of
the ECA) and the muscular branches of the vertebral artery, of which
its functional role remains limited [9]. However, based on our data
the ECASP does not change when the ICA is clamped or circulation
is restoring again (Figure 1B,2A). This suggests that the role of the
ipsilateral ICA in maintaining ECASP through collaterals remains
limited. In other words, the ECASP seems to be mainly determined
by the contralateral ECA and not by the ipsilateral internal carotid
artery and vertebral artery. This is also confirmed by the fact that
the CASP does not increase after shunt placement between the
common and ECA (see very small observation in our results section).
Second, index data show that ECASP is low compared to systemic
BP (Figure 2B), suggesting that a lower perfusion rate of the facial
arteries does not necessarily result in functional changes. A possible
explanation may be that chewing/eating is not comparable with
walking, since the masticatory muscles are not used continuously
during eating. Furthermore, it cannot be excluded that ECASP stump
pressure(ECASP and index) will increase in the postoperative phase
on the one hand by increasing blood pressure and on the other hand
increase of reasonable collateral circulation.
Although our presented data are unambiguous, sample size
remains small and future studies on a larger scale could validate our
findings and might define a ECASP threshold below which BRIG
should be avoided. However, these data again are encouraging and
support the feasibility of the BRIG technique and ligation of the ECA
as upfront treatment in carotid artery disease.
Conclusion
The internal carotid artery doesn’t have any effect on the external carotid artery stump pressure (ECASP). This study confirms that no high pressure needs to be present in the external carotid artery and that is why the external carotid artery can be safely ligated. We are therefore convinced that the BRIG technique should have a place in the treatment of carotid disease.
References
- Illuminati G, Belmonte R, Schneider F, Pizzardi G, Calió FG, Ricco JB. Prosthetic bypass for restenosis after endarterectomy or stenting of the carotid artery. J Vasc Surg. 2017;65(6):1664-72.
- De Vleeschauwer P, Diebels I, Dubois M. Cost-effectiveness of Carotid Bifurcation Resection and Interposition of a Polytetrafluoroethylene Graft versus Carotid Endarterectomy in Belgium: A Preliminary Study. 2017.
- Mandeville Y, Canovai E, Diebels I, Suy R, De Vleeschauwer P. Carotid Bifurcation Resection and Interposition of a Polytetrafluorethylene Graft (BRIG) for Carotid Disease: A Retrospective Study of 153 Consecutive Procedures. Ann Vasc Surg. 2015;29(8):1589-97.
- Rosenberg I, Austin JC, Wright PG, King RE. The effect of experimental ligation of the external carotid artery and its major branches on haemorrhage from the maxillary artery. Int J Oral Surg 1982;11(4):251-9.
- Venna N, Goldman R, Tilak S, Sabin TD. Temporal arteritis-like presentation of carotid atherosclerosis. Stroke. 1986;17(2):325-7.
- Motamed M, Farrell R, Philpott J, Rea P. Claudication on mastication following bilateral external carotid artery ligation for posterior epistaxis. J Laryngol Otol. 1998;112(1):73-4.
- Janssens MAP, Van Thielen THJ, Van Veer HGL. Jaw claudication as a result of carotid artery disease. Acta Chir Belg. 2008;108(4):438-40.
- Macchi C, Catini C. The anatomy and clinical significance of the collateral circulation between the internal and external carotid arteries through the ophthalmic artery. Ital J Anat Embryol. 1993;98(1):23-9.
- Van Den Bergh R, Van Der Eecken H. Anatomy and Embryology of Cerebral Circulation. Prog Brain. 1968;30:1-25.