Research Article
Some Technical Aspects of Carotid Endarterectomy Performing
Igor M Ignatyev*
Department of Vascular Surgery, Kazan State Medical University, Russia
*Corresponding author: Igor M Ignatyev, Department of Vascular Surgery, Kazan State Medical University, Interregional Clinical and Diagnostic Center, 12 A, Karbyshev st, 420101, Kazan, Russia
Published: 16 Aug, 2018
Cite this article as: Ignatyev IM. Some Technical Aspects
of Carotid Endarterectomy Performing.
Clin Surg. 2018; 3: 2068.
Abstract
Background: The aim of this study is to improve Carotid Endarterectomy (CEA) results by
developing of techniques of carotid bifurcation reconstruction.
Methods: Between January 2012 and December 2017, 1503 patients underwent CEA in the
Department of Vascular Surgery, including 461 (31%) according to conventional technique and
1042 (69%) - to eversion technique. The average age of patients was 61,8 ± 9,5. These operations
were performed in patients with more than 70% stenoses of the Internal Carotid Artery (ICA). 1449
reconstructions were performed under general anaesthesia, 54- under locoregional anaesthesia.
Pre-operative examination included Duplex Ultrasound (DUS), Transcranial Doppler (TCD) and
magnetic resonance angiography. 135 (9%) patients underwent eversion CEA (eCEA) method
with a prolonged incision on ICA and External Carotid Artery (ECA) formation of “extended”
anastomosis between these arteries. CEA with the “Neo Bifurcation” technique by means of Y-shape
arteriotomy of Common Carotid Artery (CCA), IСА and EСА was utilized in 60 (4%) patients. In
order to prevent floatation of the proximal portion of the atherosclerotic plaque cut in the CCA it
was fixed by sutures.
Results: Long-term outcomes (average 25 ± 14 months) of eCEA with the formation of “extended”
anastomosis were seen in 69 (51%) patients. No strokes or deaths occurred. A significant restenosis
(more than 70% IСА lumen) was observed in two patients.
After CEA with the “Neo Bifurcation” there were no damages of cerebral circulation in immediate
postoperative period. In long-term period (average 27 ± 15 months) 29 (48%) patients were
examined. No strokes or deaths occurred. Restenoses of carotid arteries were not revealed in control
DUS.
Conclusion: A preliminary marking of carotid bifurcation by DUS allows optimizing the length of
access in CEA. A routine use of intra-operative DUS provides the opportunity for revealing floating
parts of intima, thrombotic mass and to take actions to eliminate these defects in proper time. The
method of the neo bifurcation formation of carotid arteries can be used in their prolonged stenosis
lesions. It allows avoiding the use of a prosthetic patch with possible unfavorable consequences
(patch infection and aneurysm formation). This method let reduce the time of the main stage of
operation substantially.
Keywords: Carotid Endarterectomy; Eversion Endarterectomy; Carotid Artery Bifurcation; Neo Bifurcation Formation; Extended Anastomosis
Introduction
Carotid Endarterectomy (CEA) is one of the most used vascular reconstructions and is the
‘gold standard’ of surgical treatment of carotid arteries atherosclerotic lesions that is proved by
multi-centre randomized trials NACSET, ECST, ACAS [1-3]. This type of surgery is performed by
three basic methods: conventional CEA with patch, eversion CEA (eCEA) and operation of Internal
Carotid Artery (ICA) prosthetics [4].
Despite the seeming technical simplicity of CEA, this method is still one of the most difficult in
vascular surgery. The assessment of CEA results on the surgical stage is based on the perioperative
stroke frequency and the following mortality. In long-term period, efficacy of operation is
determined by the frequency of restenosis and strokes [5].
Every above-mentioned CEA method has some definite advantages and disadvantages.
Numerous randomized trials demonstrate the advantage of eCEA
because of less frequency of early and late restenosis [6]. However,
the use of this method in extended stenosis is limited. In eCEA there
are great difficulties in inserting of intraluminal shunt in patients
with a low cerebral tolerance to ischemia. In prolonged carotid
arteries lesions the use of prosthetic patch is preferable in comparison
with a primary suture in terms of lower restenosis frequency [7-
9]. However, though it is seldom, a patch using can lead to such
complications as prosthetic patch infection and aneurysm formation
in reconstruction zone [10]. Therefore, the search of new techniques
of carotid bifurcation reconstruction is still of current importance.
The objective of this study is to improve CEA results by developing
of techniques of carotid bifurcation reconstruction.
Figure 1
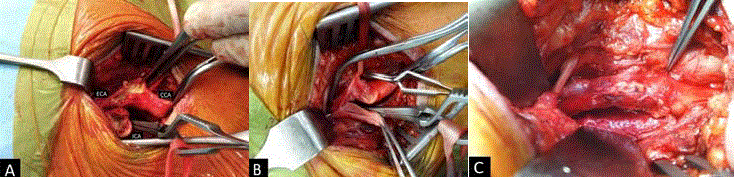
Figure 1
“Extended” anastomosis formation between ICA and ECA in eCEA. A) Incision prolongation on ICA and ECA; B) suturing on posterior wall of anastomosis;
C) anastomosis is completed.
Figure 2
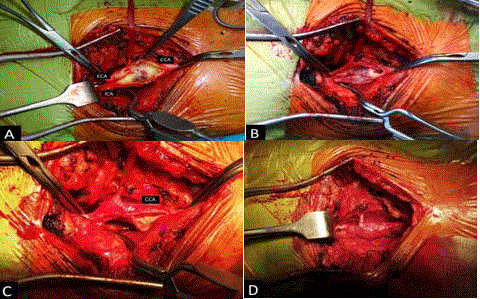
Figure 2
Stages of the “Neo Bifurcation” formation. A) Y-shape incision
of CCA, ICA and ECA; B) suturing of a cut plaque caudal end in CCA; C)
posterior wall suture; D) arteriotomy closure completed.
Materials and Methods
Between January 2012 and December 2017, 1503patients
underwent CEA in the Department of Vascular Surgery, including
461 (31%) according to conventional technique and 1042 (69%) -to
eversion technique. The average age of patients was 61,8 ± 9,5. These
operations were performed in patients with more than 70% stenoses
of the ICA. 1449 reconstructions were performed under general
anaesthesia, 54 - under locoregional anaesthesia.
Pre-operative examination included Duplex Ultrasound (DUS),
Transcranial Doppler (TCD) and magnetic resonance angiography.
Traditionally, with the help of DUS we defined the degree of carotid
artery stenosis and parameters of blood velocity, a characteristic of
the plague and its cap condition. We also marked localization of
ipsilateral carotid artery bifurcation taking into consideration its
location variability. Intra-operative monitoring of cerebral perfusion
during carotid clamping was carried out by TCD (Companion III,
Viasys Healthcare, USA) and electroencephalography (EEG) (Nicolet
OneTM, Viasys Healthcare, USA). The result was assessed by intraoperative
DUS (VIVID i, GE Healthcare, USA).
In standard situation, the Common Carotid Artery (CCA) was
isolated at the place that is more proximal than bifurcation, External
Carotid Artery (ECA) and Internal Carotid Artery (ICA) - more
distal than bifurcation. In case of unstable plague, according to preoperative
DUS and appearance of microembolic signal on TCD,
IСА was primarily dissected in intact part and after intravenous
heparin administration (5000u unfractionated heparin) was clamped
on condition that there is a cerebral tolerance to ischemia. Further
manipulations on carotid arteries were carried out in the conditions
of the clamped IСА.
In cases when cerebral tolerance to ischemia was low according
to TCD and EEG, CEA was performed by conventional method
with inserting of intraluminal balloon shunt Pruitt F3. In the case
of unstable plague and a high possibility of distal embolism we
previously performed endarterectomy (partial or full) in setting of
shunt. In balloon blowing one should follow the instructions strictly.
It is necessary to remember that absolute safe period of time for shunt
setting or removing is two minutes.
Since 2009, in case of an extended plague in ICA, we have been
using eCEA method with a prolonged incision on ICA and ECA
formation of “extended” anastomosis between these arteries (Figure
1A-1C). This type of operation was performed in 135 (9%) patients.
One of the significant technical details of the operation is a
fixation of a distal portion of plague in the case one doesn’t manage
to remove it completely. In CCA the plague is usually cut without
fearing its flotation. Proximal part of a cut plague in CСА we also fix
by two-three 7-0 polypropylene sutures.
Conventional CEA with the “Neo Bifurcation” technique (known
in literature as “carotid bifurcation advancement technique” [11])
was utilized in 60 (4%) patients with extended lesions of IСАиEСА.
The bifurcation advancement consists of a “Y” shape arteriotomy
over CCA, ECA and ICA. Endarterectomy of CCA, ECA and ICA is
then performed in a standard manner at the junction of the intima
and medial layers. Particular attention is paid to the distal fragment of
the plague extending into the ICA and any remnants of the removed
plague which may be adherent to the wall are removed subsequently.
At this stage, copious flushing and suction are recommended
eliminating even the smallest plague remnants to avoid cerebral
embolization. Removal of the atherosclerotic deposits from the ECA
follows a similar course. Endarterectomy of the CCA extends as
far as the proximal end of the Y-shaped incision. The plague being
removed is cut off at this level if it extends into the CCA and, usually,
does not require suturing at the arterial wall as the direction of blood
prevents the creation of a flap. The arteriotomy closure begins at
the bifurcation. A 7-0 polypropylene single running suture is tied
extraluminally and continued intraluminally in the cranial direction
to bring together the “arms” of the Y-arteriotomy consisting of the
ICA and ECA. Upon completing the posterior aspect of the closure
the needle is brought extraluminally and the suture line is continued
caudal on the anterior aspect of the arteriotomy, thus approximating
the ICA and ECA arms of the Y-incision.
The suture line is completed just past the proximal incision, with
care taken to include the proximal edge of the removed plague in the
suturing. Just prior to tying the suture, ECA backflow is restored to
eliminate air from the artery. Following this, CCA clamp is removed
and finally ICA is declamped. The resulting closure runs in a straight
line, with the “neo bifurcation” appearing now more cranial than
prior to closure, everted by intraluminal pressure (Figures 2A,B,C,D).
Intraluminal shunt was used in 8 cases.
Figure 3
Results
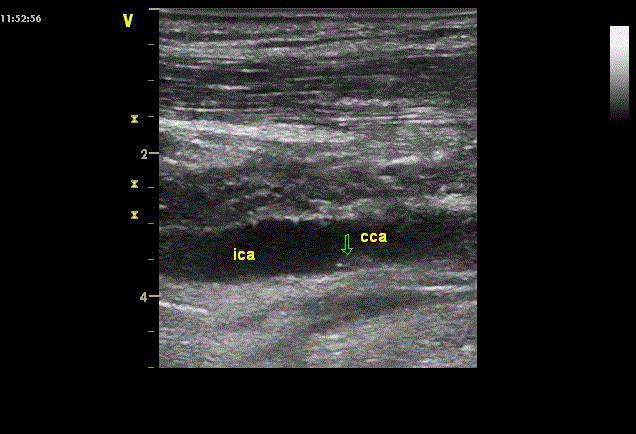
In control DUS after CEA, we paid attention to the fact that a
cut plague in CСА often floats and we consider it is connected with
specific features of hemodynamic in carotid artery bifurcation, that is,
blood flow division into laminar and turbulent, to the zone of which
caudal end of the cut plague can be involved (Figure 3,4). So, it is
necessary to cut plague proximal part as far from the bifurcation as
possible, or to fix it by two-three 7-0 polypropylene as it is shown in
Figure 2B.
Long-term outcomes (average 25 ± 14 months) of eversion CEA
with the formation of “extended” anastomosis were seen in 69 (51%)
patients. No strokes or deaths occurred. A significant restenosis
(more than 70% IСА lumen) was observed in two patients.
After CEA with the “Neo Bifurcation” there were no damages of
cerebral circulation in immediate postoperative period. In long-term
period (average 27 ± 15 months) 29 (48%) patients were examined.
No strokes or deaths occurred. Restenoses of carotid arteries
were not revealed in control DUS. Because of a limited number of
observations, a comparative evaluation of CEA with other techniques
was not carried out.
Conclusion
A preliminary marking of carotid bifurcation by DUS allows
optimizing the length of access in CEA. A routine use of intraoperative
DUS provides the opportunity for revealing floating parts
of intima, thrombotic mass and to take actions to eliminate these
defects in proper time.
The method of the “Neo Bifurcation” formation of carotid arteries
can be used in their prolonged stenosis lesions. It allows to avoid the
use of a prosthetic patch with possible unfavorable consequences
(patch infection and aneurysm formation). This method let reduce
the time of the main stage of operation substantially. This technique
has an advantage over the primary suture that gives a high restenosis
frequency. Despite a small number of observations, this method is a
promising one in carotid arteries reconstruction.
Eversion CEA with formation of “extended” anastomosis
between ICA and ECA increases the possibilities of this technique
and it can be used in ICA prolonged lesion. Taking it into account,
the indications to eCEA should be significantly broadened, as it is
a physiological intervention (it keeps geometry of carotid arteries
bifurcation, foreign tissue is absent).
The above-mentioned techniques in CEA performing allow to
improve short-term and long-term results of this intervention.
Figure 4
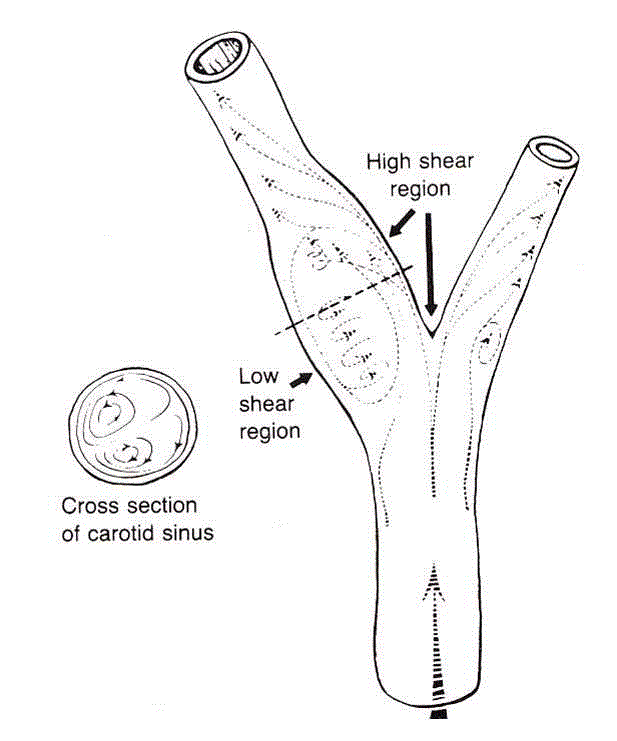
Figure 4
Carotid artery bifurcation showing an area of flow separation
adjacent to the outer wall of the bulb. Rapid flow is associated with high shear
stress, whereas the slower flow of the separation zone produces a region
of low shear. (Zarins CK, Giddens DP, Glagov S. Atherosclerotic plaque
distribution and flow velocity profiles in the carotid bifurcation. In: Bergan
JJ, Yao JST, editors. Cerebrovascular Insufficiency. New York, Grune &
Stratton, 1983).
References
- Ferguson GG, Eliasziw M, Barr HW, Clagett GP, Barnes RW, Wallace MC, et al. The North American Symptomatic Carotid Endarterectomy Trial: Surgical results in 1415 patients. Stroke. 1999;30(9):1751-8.
- European Carotid Surgery Trialists Collaborative Group. Randomised trial of endarterectomy for recently symptomatic carotid stenosis final results of the MRC European Carotid Surgery Trial (ECST). Lancet. 1998;351(9133):1379-87.
- Study design for randomized prospective trial of carotid endarterectomy for asymptomatic atherosclerosis. The Asymptomatic Carotid Atherosclerosis Study Group. Stroke. 1989;20:844-9.
- Pokrovskii AV, Beloyartsev DF, Talybly OL. Eversion CEA outcomes analysis in long-term period. Angiol Vasc Surg. 2014;20:100-7.
- Beloyartsev DF, Adyrkhaev ZA. The protocol of prevention of perioperative strokes in carotid artery bifurcation reconstructions. Angiol Sosud Khir. 2013;19(4):171-5.
- Cao P, De Rango P, Zannetti S. Eversion vs conventional carotid endarterectomy: a systematic review. Eur J Vasc Endovasc Surg. 2002;23(3):195-201.
- Goodney PP, Nolan BW, Eldrup-Jorgensen J, Likosky DS, Cronenwett JL. Restenosis after carotid endarterectomy in multicenter regional registry. J Vasc Surg. 2010;52(4):897-905.
- Markovic DM, Davidovic LB, Cvetkovic DD, Maksimovic ZV, Markovic DZ, Jadranin DB. Single center prospective randomized analysis of conventional and eversion carotid endarterectomy. J Cardiovasc Surg. 2008;49:619-25.
- Curley S, Edwards WS, Jacob TP. Recurrent carotid stenosis after autologous tissue patching. J Vasc Surg. 1987;6(4):350-4.
- Asciutto G, Geier B, Marpe B, Hummel T, Mumme A. Dacron Patch Infection After Carotid Angioplasty. A Report of 6 Cases. Eur J Vasc Endovasc Surg. 2007;33(1):55-7.
- Geremec M, Trochimczuk M, Plonski A, Ostrowsky K, Lewandowsky Z. Technical tips: bifurcation advancement for arteriotomy closure following carotid endarterectomy. Controversies and updates in vascular surgery. Torino: Edizioni Minerva Medica. 2011:302-7.