Research Article
Long-Term Outcome and Quality of Life in Patients after Conversion of the Ileal Conduit to Abdominal Continent Ileal Reservoir
Jian-Wen Huang, Yue-Min Xu*, Xin-Ru Zhang and Ying-Long Sa
Department of Urology, Shanghai Jiao Tong University Affiliated Sixth People’s Hospital, China
*Corresponding author: Yue-Min Xu, Department of Urology, Shanghai Jiao Tong University Affiliated Sixth People’s Hospital and Shanghai Eastern Institute for Urologic Repair and Reconstruction, 600 Yishan Road, Shanghai 200233, China
Published: 10 Aug, 2018
Cite this article as: Huang J-W, Xu Y-M, Zhang X-R, Sa
Y-L. Long-Term Outcome and Quality of
Life in Patients after Conversion of the
Ileal Conduit to Abdominal Continent
Ileal Reservoir. Clin Surg. 2018; 3: 2062.
Abstract
Purpose: To investigate the long-term outcome and Health-Related Quality of Life (HRQoL) in
patients after conversion of the ileal conduit to abdominal continent ileal reservoir.
Methods: From June 2001 to November 2007, 10 patients with Bricker conduit underwent a
procedure to convert their existing ileal conduit to abdominal continent ileal reservoir. The patients’
own opinions about their reservoir function and HRQoL (SF-36) were assessed during follow-up. In
addition, urodynamic study of the efferent tubes and pouch was performed at three and 12 months
post-op.
Results: All patients successfully underwent the operation without perioperative complications and
were followed for 102 to 180 months (mean 142 months). All patients expressed satisfaction with
the reservoir function and preferred the abdominal continent reservoir compared to previous ileal
conduit. Eight patients were continent day and night. All patients had stable renal function and
metabolic balance. There was no significant difference in six of the eight scales of SF-36 between
patients and general population in china (p>0.05). The urodynamic study showed that the maximum
close pressure of the tapered ileum was significantly higher when the pouch was full than when it
was empty at both three and 12 months (p<0.05).
Conclusion: Our study indicated that patients with abdominal continent reservoir had a good
long-term outcome and HRQoL. The abdominal continent reservoir is a therapeutic option when
patients require conversion from an incontinent type of urinary diversion to continent type.
Keywords: Urinary diversion; Quality of life; Continent; Urinary reservoir; Ileal conduit
Introduction
Urinary diversion is one of common surgical approaches in urology. In 1950, Bricker first
described the ileal conduit urinary diversion, which has become the standard for urinary diversion
during the last 30 years [1]. However, patients with ileal conduit have to wear cumbersome
collection devices all of the time and urine leakage often leads to skin erosion around the abdominal
stoma, which not only inconveniences patients, but also influences patients’ body image, sexual
attractiveness and sexual performance. Thus, the ileal conduit was not acceptable for every patient
requiring urinary diversion.
In 1982, Kock et al. initially described the continent ileal reservoir with low pressure as an
approach for urinary diversion [2]. The emergence of the continent ileal reservoir was an important
turning point for the conversion of urinary diversion approaches. Thereafter, several techniques
using a continent reservoir have been described [3-7]. In the present study, we reported a technique
for converting an existing ileal conduit to abdominal continent reservoir and evaluated the longterm
outcome and quality of life in patients with conversion to abdominal continent reservoir.
Materials and Methods
Patients
From June 2001 to November 2007, 10 patients (eight men and two women) with Bricker
conduit after cystectomy due to malignant (N=7) and benign (neurogenic bladder, N=3) underwent
a conversion procedure of their ileal conduit to abdominal continent ileal reservoir. The median
age at operation was 55.7 years (range, 32-68 years). The patients had a two to 18 years (median
six years) history of Bricker conduit. Of the 10 patients, seven had
several complications, including renal insufficiency due to adhesive
obstruction of the intestinal segment in three patients, repeated
retrograde urinary infection and high fever due to obstruction of
the ileal conduit at the abdominal part in three patients and severe
skin erosion due to urine leakage around the abdominal stoma in one
patient (Figure 1a); The remaining three patients hated wearing the
urine collection devices (Figure 1c).
Surgical technique
The ileal conduit of the abdominal wall was resected, and the
remaining conduit, approximately 20 cm in length, was freed from
the abdominal wall and divided into two vascularized segments (14
cm and 6 cm). The distal conduit (14 cm) was detubularized. A new 35
cm long ileal loop with the blood pedicle isolated from the intestinal
tract was divided into two vascularized segments (25 cm and 10 cm),
and the 25 cm segment was detubularized. The detubularized ileal
segment was anastomosed with the detubularized conduit to form a
new U-shape pouch. A 5-6 cm segment of the proximal conduit, which
was approximately 4 cm away from the ureteroileal anastomosis, was
tapered over a 22 Fr catheter and replanted into the U-shape pouch
by an extramural serous lined tunnel (Figure 2a). The short 8 cm to 10
cm ileal segment was tapered over a 16 Fr catheter constructed with
an efferent tube. An end of the tapered ileum was anastomosed to
the pouch by an end-to-side all layer procedure using an interrupted
4-zero polygalactin suture. The other end of the tapered ileum was
then brought out to the umbilical hole to form a stoma (Figure 2a).
The enhanced continent mechanism technique has been described
previously [7]. Briefly, a portion of the tapered ileum approximately
4 cm long was embedded and fixed between the tubular segment of
the pouch and the abdominal wall by a 3-zero nylon sutures passing
through the mesenteric windows of the tapered ileum (Figure 2a).
Follow-up
Ureteral drainage tubes (8 Fr single-J-tubes) were removed 10
days postoperatively and the pouch was maintained on drainage (16 Fr
catheters) for 21 days. All patients regularly took sodium bicarbonate
(1 g each time, twice a day) for one to two years postoperatively,
especially for patients with preoperative renal dis function. All patients
were followed every three months for the first 12 months, and every
one to two years thereafter. Follow-up testing included blood gas
analysis, blood renal function, serum electrolytes, upper urinary tract
ultrasonography, abdominal plain film, and Intravenous Urogram
(IVU). Urodynamic study, retrograde radiography of the efferent
tube and radiography of the pouch were postoperatively performed at
three months. The urodynamic study was postoperatively performed
again at 12 months.
A questionnaire survey was carried out to assess the patients’ own
opinions on their reservoir function and Health-Related Quality of Life
(HRQoL) at an outpatient clinic at least 12 months after conversion
from ileal conduit to continent reservoir. The questionnaire survey
included two questionnaires. One questionnaire included questions
about reservoir function and reservoir-related problems. The other
was the Short Form-36 survey (SF-36) to assess the HRQoL. The SF-
36 contains 36 questions assessing eight aspects of HRQoL, including
Physical Functioning (PF), Role-Physical Functioning (RP), Bodily
Pain (BP), General Health (GH), Vitality (VT), Social Functioning
(SF), Role-Emotional Functioning (RE) and Mental Health (MH).
Each question is given a score of 0-100 and a mean score obtained for
each scale (range 0-100). The higher the score, the better the result [8].
Statistical analysis
The data were presented as the mean ± Standard Deviation (SD).
Data comparisons between the groups were analyzed using the paired
Student two-tailed t-tests. Differences were considered statistically
significant at P values <0.05.
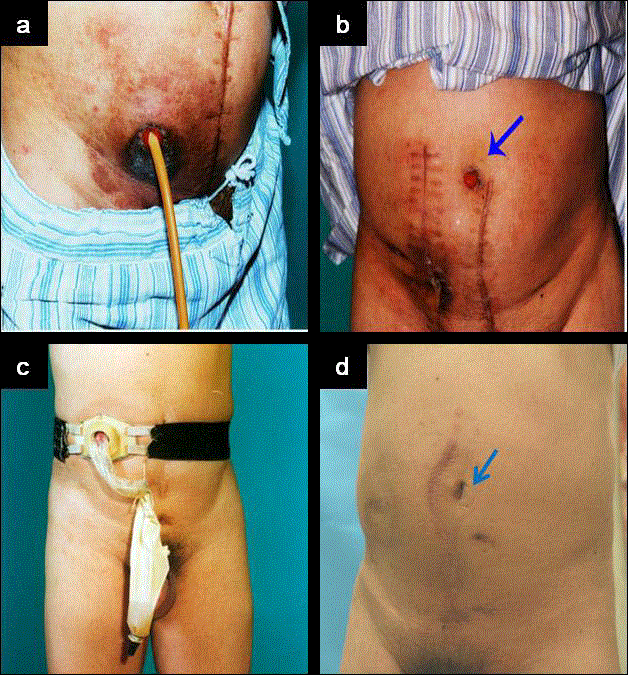
Figure 1
Figure 1
a) Severe skin erosion due to urine leakage around the abdominal
stoma.
b) Skin erosion has been cured at one month postoperatively; A stoma at the
umbilical hole and complete continence has been achieved day and night
(arrow).
c) The abdominal appearance of a patient with severe neurogenic bladder
before the continent ileal reservoir.
d) Good appearance of an abdominal stoma after the conversion of an ileal
conduit to a continent reservoir 12 years postoperatively and with complete
continence day and night (arrow).
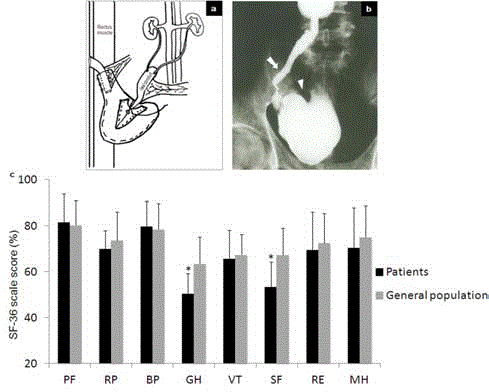
Figure 2
Figure 2
a) The tapered ileal conduit was replanted into the U-shape pouch
by an extramural serous lined tunnel and the tapered ileal segment was fixed
between the back surface of the rectus muscle and the ileal pouch wall.
b) Retrograde radiography of the efferent tube and the pouch demonstrated
that the efferent tube was fixed straight between the abdominal and pouch
wall (white arrow), and there was no contrast medium in the ureters (arrow
head). c) A comparison of the SF-36 scores among patients with continent
reservoir and the general population of the china.
*Significantly lower than the general population (P<0.05).
Results
All patients successfully underwent the operation without
perioperative complications. Two patients died of cancer metastasis
six and seven years postoperatively, and all patients were followed
for 102 to 180 months (mean 142 months). All patients expressed
satisfaction with the reservoir function (Table 1). Eight patients were
completely continent day and night at 4 hr to 5 hr intervals, with urine
production less than 400 ml, while only two patients were partially
incontinent during sleep, with more than 400 ml of urine produced.
However, the two patients who had some leakage problems did not
change the stomal pad between the catheterizations. All patients
reported never or seldom experiencing stomal catheterization
problems (Table 1). Good appearance of abdominal stoma after
conversion of the ileal conduit to a continent reservoir was found in
all patients (Figure 1b and 1d). All patients preferred the abdominal
continent reservoir compared with the previous ileal conduit.
IVU revealed normal upper tracts in all patients. Blood renal
function became totally normal postoperatively in three patients with
preoperative renal insufficiency. The results of the repeated renal
function indicated that serum creatinine increased somewhat with
longer follow-up in seven patients, but it remained within the normal
range at all times. Additionally, after the slight increase at three
months postoperatively in six patients, the chloride levels remained
stable during follow-up. The acid-base balance was assessed by base
excess from blood gas analysis and the values were in the normal
range in all patients during the follow-up. Clinical manifestations
due to serum electrolyte disorder and metabolic acidosis were not
observed in any of the patients, and the serum potassium and sodium
were normal during follow-up.
Mean score obtained for each scale of SF-36 for patients and for
sex-and age-matched general population of china was showed in
(Figure 2c). Mean scores for GH and SF in patients were significantly
low compared to those in the general population (p<0.05). However,
there was no significant difference in other six scales between patients
and general population (p>0.05).
At three months postoperatively, retrograde radiography of the
tapered tube demonstrated that the tube was fixed straight between
the abdominal and pouch walls without stenosis. Radiography of
the pouch at a gravity pressure of 50 cm. water showed no contrast
medium in the ureters (Figure 2b). Urodynamic analysis showed that
the maximum closure pressure (MCP) for the efferent tube was 48
cm to 84 cm water (mean 69.00 ± 10.92) when the pouch was empty.
When the pouch was filled with saline, the MCP was 82 to 114 cm.
water (mean 96.60 ± 9.17) (Table 2). The difference in the mean
MCP between the empty and full pouch was statistically significant
(p<0.05).
At 12 months postoperatively, urodynamic analysis showed that
the reservoir capacity was 360 ml to 550 ml (mean 431 ± 65.90). The
reservoir pressure was 6 cm to 9 cm. water (mean 6.23 ± 1.21) when
the pouch was filled with 50 ml water and 16 cm to 35 cm water
(mean 23 ± 5.77) when it was filled to maximum capacity (Table 2).
There was no contraction wave during filling in any patient. The MCP
in the efferent tube when the pouch was empty was 56 cm to 75 cm
water (mean 67.60 ± 6.29). When the pouch was filled with saline, the
MCP was 77 cm to 101 cm water (mean 94.50 ± 7.3) (Table 2). The
difference in the mean maximum closure pressure between the empty
and full pouch was also statistically significant (p<0.05).
Table 1
Table 2
Discussion
Urinary diversion is a common choice for urologists after total
cystectomy due to bladder carcinoma or benign disease, such as
neurogenic bladder. The orthotopic neobladder is now commonly
used as a type of urinary diversion in both genders and should be
offered to male and female patients who lack any contraindications [9].
However, some patients are not suited for an orthotopic neobladder
after total cystectomy, such as patients with a tumor affecting the
urethra or bladder neck or with severe neurogenic bladder, and need
ileal conduit or other options.
The Bricker Ileal conduit is acknowledged as an alternative choice
for these patients who are not suited for orthotopic neobladders after
total cystectomies. However, persistent complications, including
obstruction leading to renal damage, stomal stenosis and urinary
tract infections, continue to be associated with ileal conduits [10,11].
The patients with ileal conduits have to wear cumbersome collection
devices at all times, which are not only inconvenient but also influence
the patients’ body images. In addition, stomal leakage, odor, and lack
of sexual attractiveness and performance were common complaints
among patients with ileal conduits [12,13]. In response to these
problems with the ileal conduit, the continent reservoir has become
an option when orthotopic bladder is not possible.
In general, we do not recommend conversion for patients with
a diversion system functioning normally because the procedure
requires a major operation. In the present study, however, seven
patients had several complications after their initial Bricker conduit,
including renal insufficiency due to adhesive obstruction of the
intestinal segment in three patients, repeated retrograde urinary
infection and high fever due to obstruction of the ileal conduit at the
abdominal part in three patients and severe skin erosion around the
abdominal stoma due to urine leakage in one patient. In addition,
three younger patients with benign disease strongly wished to have a
later conversion to continent diversion to avoid external appliances
and to improve their quality of life. Thus, we devised conversion
of previous ileal conduit to abdominal continent reservoir. After
resolving the obstruction and constructing the continent reservoir,
blood renal function returned to normal, and the patients did not
need to wear urine collection devices and only needed interval
catheterization because the pouch could store 400 ml to 500 ml urine
without urine leakage, thereby leading to improved patients’ body
images and sexual attractiveness and performance. In addition, the
patient has suffered from severe skin erosion due to urine leakage for
one year in half a year after ileal conduit, which led to not use urine
collection device. After reconstruction of the continent reservoir, the
complication was totally resolved and the skin around the abdominal
stoma had consistent good appearance. Thus, the patients were
satisfied with the reservoir function and preferred the abdominal
continent reservoir compared with the previous ileal conduit.
It is generally accepted that continent urinary diversion
enables the patient greater freedom in bathing, sporting, travelling
and facilitates social activities [14-16]. Whether the continent
reservoir improves quality of life compared with the ileal conduit
is controversial. Some studies have reported no difference in the
quality of life between the continent reservoir and the ileal conduit
[14,17]; while other studies have indicated a better quality of life
with the continent reservoir compared with the ileal conduit [15].
However, the opinions of patients who have experienced both types
of diversions have been published in several previous studies [17,18].
The studies have reported that patients who converted from an
ileal conduit to a continent reservoir were most satisfied with their
diversion status, which were consistent with our results in the present
study. To investigate HRQoL in patients with abdominal continent
reservoir, mean score of each scale of SF-36 for patients was compared
with sex-and age-matched general population. The result showed that
all scores except GH and SF in patients were similar to those in the
general population. Therefore, patients with conversion of previous
ileal conduit to continent reservoir were generally satisfied with their
overall health and quality of life.
Critical points in creating a continent reservoir from an existing
conduit are the continent mechanism, ureteral implantation and
metabolic changes after urinary diversion [19]. In terms of continence
eight of ten patients were completely continent day and night at 4 hr
to 5 hr intervals, when the produced urine was less than 400 ml. In the
present study, we modified the technique through tapering the ileal
as the efferent tube, fixing the partial efferent tube between the back
surface of the rectus muscle and the ileal pouch wall, anastomosing
the internal orifice of the tapered ileum to the ileal pouch and
anastomosing its external orifice to the umbilicus. When supported
by the pouch-abdominal wall, the tapered ileum worked effectively
as a continent valve. The MCP of the tapered ileum was significantly
higher when the pouch was full than when it was empty at both three
and 12 months (p<0.05). This suggests that the continent mechanism
of the efferent tube is greatly enhanced with an increase in the volume
and pressure of the pouch, even when the tapered ileum was not
tunneled submucosally into the pouch, which is based on either the
flap valve principle or Laplace’s law.
To avoid ureteral reflux, we tapered the terminal ileum over a
22 Fr catheter and then replanted it into a U-shaped pouch using an
extramural serous lined tunnel in all patients. A pouch gram with a
gravity pressure of 50 cm water showed no contrast medium in the
ureters, which indicated that the approach can prevent urine from
refluxing.
The results of repeated renal function testing indicated that the
serum creatinine increased somewhat over longer term of follow-up
in seven patients, but it remained within the normal range at all times.
This increase with time in the conversion patients may be explained
by the increase in renal function with increasing age, especially in
older patients [20]. Thus, the continent reservoir does not appear to
impair renal function. Metabolic disturbances are s consequence of
incorporating any segment of the bowel into the urinary tract. Thus,
we regularly monitor the acid-base balance and gave early medical
intervention (sodium bicarbonate) for balancing a base deficit
prevents metabolic acidosis. Clinical manifestations due to serum
electrolytes disorder and metabolic acidosis were not observed in any
patients, and the serum potassium and sodium were in the normal
range during follow-up.
Our study has some limitations. Firstly, this is a retrospective,
non-randomized study in a small number of patients. It caused
a lack of information about pre-conversion HRQoL evaluation.
Therefore, the study did not compare difference of HRQoL between
pre-conversion and post-conversion, even if patients preferred the
abdominal continent reservoir. Secondly, the study investigated the
renal function by monitoring serum creatinine level during follow-up.
However, serum creatinine alone may not be enough to evaluate true
renal function in urinary diversion, because serum creatinine usually
underestimates the decrease in Glomerular Filtration Rate (GFR) in
the elderly [21]. Therefore, we should choose to use more valuable and
sensitive method to evaluate the renal function in further study, such
as 99mtechnetium diethylenetetraminepentaacetic acid (99mTc-DTPA)
renal scintigraphy. Moreover, further randomized and prospective
large study will be needed to investigate long-term outcome and
HRQoL in patients with conversion of previous incontinent diversion
to continent type.
Conclusion
Our study indicated that the conversion of an existing ileal conduit to an abdominal continent ileal reservoir has a good longterm outcome and HRQoL. The abdominal continent reservoir is a therapeutic option when patients require conversion from an incontinent type of urinary diversion to continent type.
References
- Bricker EM. Bladder substitution after pelvic evisceration. Surg Clin North Am. 1950;30(5):1511-21.
- Kock NG, Nilson AE, Nilsson LO, Norlén LJ, Philipson BM. Urinary diversion via a continent ileal reservoir: Clinical results in 12 patients. J Urol. 1982;128(3):469-75.
- Pahernik S, Stein R, Hohenfellner M, Thüroff JW. Conversion from colonic or ileal conduit to continent cutaneous urinary diversion. J Urol. 2004;171(6):2293-7.
- Pahernik S, Wiesner C, Gillitzer R, Stein R, Thüroff JW. Conversion from colonic conduit into recto-sigmoid pouch (Mainz pouch II). BJU Int. 2006;97(1):157-60.
- Rowland RG, Mitchell ME, Bihrle R, Kahnoski RJ, Piser JE. Indiana continent urinary reservoir. J Urol. 1987;137(6):1136-9.
- Thüroff JW, Alken P, Riedmiller H, Engelmann U, Jacobi GH, Hohenfellner R. The Mainz pouch (mixed augmentation ileum and cecum) for bladder augmentation and continent diversion. J Urol. 1986;136(1):17-26.
- Xu YM, Xu YZ, Qiao Y, Sa YL, Zhang XR, Zhang J, et al. Enhanced continent mechanism of tapered ileum by extramural support from the pouch and abdominal walls: a preliminary report of a clinical study. J Urol. 2001;165(3):794-7.
- Stansfeld SA, Roberts R, Foot SP. Assessing the validity of the SF-36 general health survey. Qual Life Res. 1997;6(3):217-24.
- Witjes JA, Compérat E, Cowan NC, De Santis M, Gakis G, Lebret T, et al. EAU guidelines on muscle-invasive and metastatic bladder cancer: summary of the 2013 guidelines. Eur Urol. 2014;65(4):778-92.
- Hovey RM, Carroll PR. Non-continent urinary diversion. In: Urologic Oncology. Edited by JE Oesterling and JP Richie. Philadelphia: WB. Saunders Co., chapt. 22. 1997;323-35.
- Pitts RW Jr, Muecke EC. 20-year experience with ileal conduits: the fate of the kidneys. J Urol. 1979;122(2):154-7.
- Jones MA, Breckman B, Hendry WF. Life with an ileal conduit: results of questionnaire surveys of patients andurological surgeons. Br J Urol. 1980;52(1):21-5.
- McLeod RS, Fazio VW. Quality of life with the continent ileostomy. World J Surg. 1984;8(1):90-5.
- Kitamura H, Miyao N, Yanase M, Masumori N, Matsukawa M, Takahashi A, et al. Quality of life in patients having an ileal conduit, continent reservoir or orthotopic neobladder after cystectomy for bladder carcinoma. Int J Urol. 1999;6(8):393-9.
- Månsson Å, Johnson G, Månsson W. Quality of life after cystectomy. Comparison between patients with conduit and those with continent caecal reservoir urinary diversion. Br J Urol. 1988;62(3):240-5.
- Okada Y, Oishi K, Shichiri Y, Kakehi Y, Hamaguchi A, Tomoyoshi T, et al. Quality of life survey of urinary diversion patients: Comparison of continent urinary diversion versus ileal conduit. Int J Urol. 1997;4(1):26-31.
- Boyd SD, Feinberg SM, Skinner DG, Lieskovsky G, Baron D, Richardson J. Quality of life survey of urinary diversion patients: Comparison of ileal conduits versus continent Kock ileal reservoirs. J Urol. 1987;138(6):1386-9.
- Jonsson O, Olofsson G, Lindholm E, Törnqvist H. Long-time experience with the Kock ileal reservoir for continent urinary diversion. Eur Urol. 2001;40(6):632-40.
- Pahernik S, Stein R, Hohenfellner M, Thüroff JW. Conversion from colonic or ileal conduit to continent cutaneous urinary diversion. J Urol. 2004;171(6 Pt 1):2293-7.
- Granerus G, Aurell M. Reference values for 51Cr-EDTA-clearance as a measure of glomerular filtration rate. Scand J Clin Lab Invest. 1981;41(6):611-6.
- Palmer BF, Levi M. Effect of aging on renal function and disease. In: The Kidney. 5th ed. Brenner MB, editor. Philadelphia: W. B. Saunders Co., vol. IV, chapt. 52. 1996;2274.