Case Report
Emergency Progressive Tracheal Dilation with Conventional Tubes before Stenting in Thyroid Mass: A Case Report
Alessandro Crepaldi1*, Enrico Giustiniano2, Alberto Testori1, Nadia Fusilli2, Marco Alloisio1, Ugo Cioffi3 and Giorgio Maria Ferraroli1
1Department of Thoracic and General Surgery, Istituto Clinico Humanitas, Rozzano (Milano), Italy
2Department of Anesthesia and Intensive Care Unit, Istituto Clinico Humanitas, Rozzano (Milano), Italy
3Department of Surgery, University of Milan, Milano, Italy
*Corresponding author: Alessandro Crepaldi, Department of Thoracic and General Surgery, Istituto Clinico Humanitas, Rozzano (Milano), Italy
Published: 31 Jul, 2018
Cite this article as: Crepaldi A, Giustiniano E, Testori A,
Fusilli N, Alloisio M, Cioffi U, et al.
Emergency Progressive Tracheal
Dilation with Conventional Tubes before
Stenting in Thyroid Mass: A Case
Report. Clin Surg. 2018; 3: 2057.
Abstract
An 80-year-old female patient presented to the emergency room for dyspnea and “tirage” caused
by massive thyroid cancer. In these cases tracheal dilation by rigid bronchoscopy is the treatment of
choice. Before the procedure we performed progressive dilatation with repeated intubations using
conventional tube with increased diameters. No adverse events occurred. She was discharged from
ICU to the ward on the day after the operation. This procedure allows being more confident in
terms of patient ventilation, less trauma to the stenotic tracheal mucosa, less ICU stay, easy material
availability and less cost for public health.
Keywords: Tracheal stenosis; Thyroid tumors; Rigid bronchoscopy; Emergency intubation
Introduction
Tracheal stenosis due to invasion or compression by thyroid tumor is usually treated by dilation
and stenting using rigid bronchoscope, when surgical procedures are not indicated. In very rare
cases (emergency setting with respiratory failure, severe distortion of the trachea), rigid endoscopic
intubation could be at high risk or even not feasible. We describe a technique to progressively dilate
in emergency setting a severe tracheal stenosis using conventional tubes.
This procedure allows sufficient dilation of the stenotic trachea, while maintaining adequate
ventilation of the patient. It then allows a safe insertion of a stent via rigid bronchoscopy.
Case Presentation
80 year-old woman was admitted to the Emergency-Room of our Hospital for dyspnea and
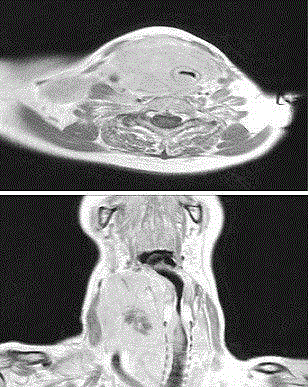
“tirage” due to a bulky cervical mass. Few days before she underwent a neck and chest MRI that
showed a neoplastic thyroid mass deforming and invading the upper trachea for a 3 cm length,
associated with pulmonary lesions, suspected for metastasis (Figure 1). The patient was dyspneic
with peripheral desaturation, blood hypertension and tachycardia. She was immediately transferred
to the operatory theatre to dilate the tracheal stenosis and insert a stent in Rigid Bronchoscopy
(RB). Tracheostomy was not feasible for the presence of the cervical tumor. In our Institution, rigid
endoscopy is performed assuring a spontaneous breathing during total intra-venous anesthesia. In
this case, we expected a complex performance of RB and a coexisting difficult airways management.
Hence we adopted a type of sedation with a more limited risk of respiratory function worsening:
pre-medication with atropine (0.5 mg i.m.) and administration of midazolam (2 mg i.v.) and
ketamine (50 mg i.v). When the patient reached a sufficient level of sedation, we tried to introduce
the rigid bronchoscope through the vocal cords, but the maneuver resulted particularly difficult.
In the meanwhile the patient became quickly hypoxic (SatO2 35%) and cyanotic. After increasing
bradycardia, asystole occurred despite the administration of atropine (0.5 mg i.v). Cardiopulmonary
resuscitation started and the patient was intubated with an orotracheal tube (#5.5 Hi-
Contours, Mallinkrodt™). She was ventilated with FiO2 100% until saturation and cardiac function
were restored. External thoracic compression and epinephrine (1 mg i.v.) was needed. Effective
circulation was restored in 2 min, with normal and light-reactive pupils. After resuscitation, sedation
was maintained with ketamine and propofol. After that, we decided to try to dilate the trachea
with repeated intubation using progressive bigger conventional
tubes (Hi-Contour, Mallinkrodt™), reaching an adequate caliber to
allow intubation with rigid bronchoscope. Therefore we substituted
the small orotracheal tube repeatedly with other larger tubes sliding
them on a Frova catheter. After insertion of #8.0 orotracheal
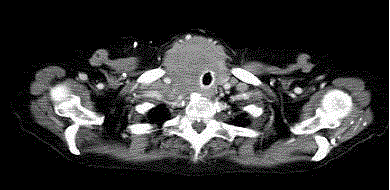
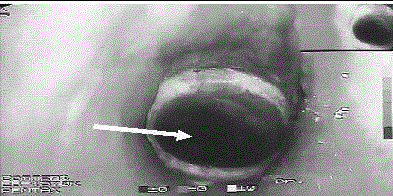
tubes, the patient was extubated. The surgeon introduced the rigid
bronchoscope and bypassed the tracheal stenosis with a silicone stent
(Novatech, 14 × 40, La Chiotat, Marseille, France) (Figure 2, 3).
During the procedure (lasted 20 min) the patient did not
experienced any adverse event. Despite patient’s spontaneous
breathing, she was manually assisted during the operation through
the rigid bronchoscope when needed. Hemodynamics always stayed
in a normal setting. At the end of the procedure, blood gas-analysis
showed pH 7.36, pCO2 47 mmHg and pO2 133 mmHg, SatO2 98%,
normal serum lactate and base excess. At the completion of the
procedure, the patient was re-intubated with an orotracheal tube #8.
Sedation was gradually stopped. When vital signs allowed, she was
extubated and admitted to our ICU for over-night surveillance. No
adverse events occurred. She was discharged from ICU to the ward
on the day after the operation. She was dismissed from the Hospital
after 5 days. The histological examination showed a great cells non-
Hodgkin B-lymphoma of the thyroid gland. The patient started a
chemotherapic treatment and she is still alive after 2 years from the
operation.
Figure 1
Figure 2
Figure 3
Discussion
In emergency event, the anesthesiologists should take valuable treatment to ensure ventilation. In this case we performed a procedure before the rigid bronchoscopy to enable us to take prompt action in case of sudden and critical changes. We consider this technique may be safe, easy to perform with low cost. It could be useful in treating tracheal stenosis in emergency setting, particularly when there is a severe distortion that could make any endoscopic treatment particularly challenging.
References
- Nishijima Y, Takahashi H, Taguchi N, Naito H. A newly devised endotracheal tube for patients with narrowed trachea. Masui. 1993;42:455-7.
- Lacoste L, Gineste D, Karayan J, Montaz N, Lehuede MS, Girault M, et al. Airway complications in thyroid surgery. Ann Otol Rhinol Laryngol. 1993;102(6):441-6.
- Loftus PA, Ow TJ, Siegel B, Tassler AB, Smith RV, Schiff BA. Risk Factors for Perioperative Airway Difficulty and Evaluation of Intubation Approaches among Patients With Benign Goiter. Ann Otol Rhinol Laryngol. 2014;123(4):279-85.
- Yamaguchi K, Fujimoto K, Koide Y, Kurahashi K. Safe induction of anesthesia in 3 patients with severe tracheal stenosis caused by thyroid cancer. Masui. 2013;62(1):78-82.
- Tsutsui H, Kubota M, Yamada M, Suzuki A, Usuda J, Shibuya H, et al. Airway stenting for the treatment of laryngotracheal stenosis secondary to thyroid cancer. Respirology. 2008;13(5):632-8.
- Han YH, Jung BH, Kwon JS, Lim J. Successful Treatment of Tracheal Invasion Caused by Thyroid Cancer using Endotracheal Tube Balloon Inflation under Flexible Bronchoscopic Guidance. Tuberc Respir Dis. 2014;77:215-8.
- Lee J, Won JH, Kim HC, Soh EY. Emergency dilation by self-expandable tracheal stent for upper airway obstruction in a patient with a giant primary thyroid lymphoma. Thyroid. 2009;19(2):193-5.