Case Report
Dislocated Corneal Lamellar Flap Following Blunt Ocular Injury: A Case Report
Lung-Kun Yeh* and Linda Yi - Hsing Chen
Department of Ophthalmology, Chang - Gung University College of Medicine, Taiwan
*Corresponding author: Lung-Kun Yeh, Department of Ophthalmology, Chang - Gung Memorial Hospital at Linko, Chang - Gung University College of Medicine, No: 5, Fusing St, Gueishan Township, Taoyuan county 333, Taiwan
Published: 27 Jul, 2018
Cite this article as: Yeh L-K, Yi - Hsing Chen L. Dislocated
Corneal Lamellar Flap Following Blunt
Ocular Injury: A Case Report. Clin Surg.
2018; 3: 2053.
Abstract
Purpose: We report a case of post-traumatic dislocated corneal lamellar flap with diffuse lamellar
keratitis following ocular blunt injury without receiving previous refractive surgery procedure before.
Methods: Retrospective case report.
Results: The dislocated lamellar flap was surgically repositioned. DLK was treated with intensive
steroid regimen. The best corrected visual acuity of the injured eye was 20/30 after treatment.
Conclusion: DLK may be caused by blunt ocular injury even without previous refractive surgery.
The proper reposition of traumatic lamellar flap could reach good outcomes.
Keywords: Corneal lamellar flap; Refractive surgery; Blunt ocular injury
Introduction
Diffuse Lamellar Keratitis (DLK), first discovered in 1988, is a noninfectious interface keratitis, usually occurred between corneal flap and stromal bed after laser in situ keratomileusis (LASIK) [1,2]. It can vary from a mild self -limiting condition that responds quickly to topical corticosteroid treatment to a severe condition associated with stromal melting, scarring, and a hyperopic shift3. We report a patient who never received refractive surgery presented diffuse lamellar keratitis and limited epithelial ingrowth following blunt ocular injury by a sharp steel bar.
Case Presentation
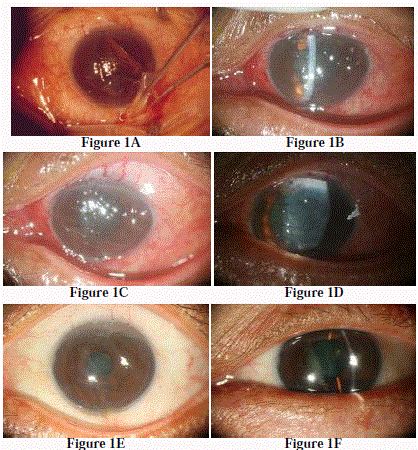
The 48 year - old healthy male came to our emergency room described his left eye being injured by a steel bar two hours ago. His Uncorrected Visual Acuity (UCVA) was 20/800 in the left eye and 20/40 in the right eye. Slip - lamp microscopy revealed one 7 mm x 10 mm in size deep lacerated triangular - shaped lamellar corneal flap with depth to deep stroma in his left eye with moderate conjunctival hyperemia. The deep penetrating wound extended to conjunctiva and sclera with an iron foreign body embedded in deep sclera tissue (Figure 1A). Severe cornea edema and anterior chamber reaction with degree 2 flare reaction were discovered. No aqueous leakage was noted from the wound by Seidel test. The lens was clear and relative afferent papillary response was negative. The fundus exam disclosed attached retina. The patient denied of previous ocular trauma or surgery history. After iron fragment removal, the lamellar corneal flap and lacerated conjunctiva were irrigated with balanced salt solution cannula and repositioned carefully with interrupted suture. The presence of white granular cells was found in the center and periphery of the lamellar interface and Diffuse Lamellar Keratitis (DLK) was impressed on the first day after surgery (Figure 1B). The cellular reaction was much decreased after applying topical tobramycin and 0.1% fluorometholone for 1 week (Figure 1C, 1D). One month later, there was fibrotic scarring formation between corneal lamellar interface spaces (Figure 1E). The best corrected visual acuity of left eye was 20/30 (-1.50/- 3.00*85) with limited marginal epithelial ingrowth during the one year follow-up period (Figure 1F).
Discussion
DLK is usually seen early or late onset after LASIK procedure [1-4]. Povidone - iodine solution, meibomian gland secretions, microkeratome blade debris, carboxymethylcellulose drops, interface hemoglobin, bacterial endotoxins, and epithelial defects at the time of LASIK were possible etiologic factors for the development of DLK. Both sporadic and epidemic cases of DLK have been reported [5]. In this case, ocular blunt injury created one lacerated corneal lamellar flap by sharp steel bar in a similar way to LASIK flap by microkeratone. However, the instrument that produced the flap was not sterile; the stromal bed was only partially exposed and the flap was pushed aside into a pleated configuration. The accumulated inflammatory cells between the lamellar interfaces subsequently developed DLK in this patient. Prompt topical steroid treatment and early treatment are required for a fair outcome.
Figure 1
Figure 1
A) Blunt ocular injury by sharp steel bar caused lacerated lamellar
corneal flap. Arrow indicated iron fragment embedded under lacerated
scleral tissue.
B) Diffuse white granular inflammatory cells were found in the center and
periphery of the lamellar interface on the first day after surgery.
C) Corneal edema was still noticed at one week after primary repair.
D) Significantly decreased in inflammatory cells was noted after one week.
E) The lacerated lamellar corneal flap was stable one month after corneal
stitches removal. Limited epithelial ingrowth with scarring formation was
noted along the flap margin after one year follow - up period.
F) The central corena was clear after one year follow - up period.
References
- Smith RJ, Maloney RK. Diffuse lamellar keratitis; a new syndrome in lamellar refractive surgery. Ophthalmology. 1998;105(9):1721-6.
- Johnson JD, Harissi-Dagher M, Pineda R, Yoo S, Azar DT. Diffuse lamellar keratitis: incidence, associations, outcomes, and a new classification system. J Cataract Refract Surg. 2001;27(10):1560-6.
- Steven EW, Renato AS. Sporadic diffuse lamellar keratitis (DLK) after LASIK. Cornea. 2002;21(6):560-3.
- Chang - Godinich A, Steinert RF, Wu HK. Late occurrence of diffuse lamellar keratitis after laser in situ keratomileusis. Arch Ophthalmol. 2001;119(7):1074-6.
- Stulting RD, Randleman JB, Couser JM, Thompson KP. The epidemiology of Diffuse Lamellar Keratitis. Cornea 2004;23(7):680-8.