Research Article
Walk in Walk Out Hernia Service - A New Era for Hernia Repair
Niroshini Rajaretnam1* and Raj Bhutiani2
1Department of Surgery, Derriford Hospital, UK
2Department of Surgery, Northwick Park Hospital, UK
*Corresponding author: Niroshini Rajaretnam, Department of Surgery, Derriford Hospital, Derriford Road, Crownhill, Plymouth, UK
Published: 18 Jul, 2018
Cite this article as: Rajaretnam N, Bhutiani R. Walk in Walk
Out Hernia Service - A New Era for
Hernia Repair. Clin Surg. 2018; 3: 2044.
Abstract
Background: Herniae cause significant morbidity which results in a reduced quality of life.
Approximately 78% of surgical repairs are performed under General Anaesthesia (GA). Repair
under Local Anaesthesia (LA) is more cost-effective and life-changing for an increasing number
of patients who are refused surgery due to their co-morbidities. This approach is likely to become
increasingly necessary as our population ages and co-morbidities rise.
Methods: Retrospective analysis of a prospective database of hernia repairs performed under LA of
696 operations between May 2006 and December 2013 under supervision of a single consultant in
the Walk-In-Walk-Out (WIWO) hernia service in one NHS Trust. Data collected included patient
demographics, co-morbidities, operation details and complications. Cost-effectiveness analysis
performed using hospital payment tariffs.
Results: Of the total 696 repairs, there was zero mortality and five recorded complications. Costeffectiveness
analysis showed that with open hernia repair under LA, our institution saved £411.00
per patient; £561.00 if overnight stay; and £861.00 when compared to overnight stay under GA.
Conclusion: As our aging population develops co-morbidities which are high risk of morbidity/
mortality from surgery under GA, open hernia repair under LA is not only cost-effective and safe
but is considered the only option. Due to present demands of offering laparoscopic surgery (only
possible under GA) in training future surgeons, we feel trainees are inexperienced to manage the
needs of the comorbid population unless surgical training is modified to offer operations under LA.
Combining priorities of training and cost-effectiveness makes the WIWO hernia service desirable
for any healthcare institution.
Introduction
Hernia repair is the one of the commonest general surgical operations performed word wide [1].
It is estimated that over 120,000 new inguinal herniae [2] are diagnosed in England annually, with
inguinal hernia being the most common, having an annual rate of 70,000 - 74,000 surgical operations
[3,4]. Inguinal herniae have a prevalence of 1.7% and a lifetime risk in men of 27% and in women of
3% [5]. The other abdominal wall herniae including epigastric, umbilical / para-umbilical, spigelian,
ventral, femoral, incisional and parastomal also need surgical repair. Besides being symptomatic,
they carry a risk of incarceration and strangulation. The risk of incarceration is approximately 4
per 1000 patients with a groin hernia per year [6]. Risk of strangulation has been reported to < 1%
per year in patients with inguinal hernias at least in the first few years of onset of the hernia [7].
The mortality associated with elective hernia repair has been reported as 0.07-1.3% under General
Anaesthetic (GA) [8,9] but it increases with emergency repair to 3.4-19% [8-14] and 20-fold if bowel
resection is required [15]. The reported morbidity is 0.45-22% [10] for elective and 31-58% [10-12]
for emergency hernia procedures. Nearly 40,000 patients annually are advised against surgery due
to significant co-morbidities [2]. Factors associated with poor outcome following emergency repair
include increasing age [6,12,13], increasing co-morbidities/ASA grade [6,8,12,16] femoral hernias
[6,11,15,17], bowel resection [6,12,15-17] and prolonged time to diagnosis and surgery [6,14,16].
Surgical repair is the mainstay of treatment for abdominal wall herniae. Patients try TRUSS, tight
underclothes and corsets to keep the symptoms under control when repair is not offered because
of the level of comorbidity and the risk of surgery. Local Anaesthetic (LA) repair would be ideal
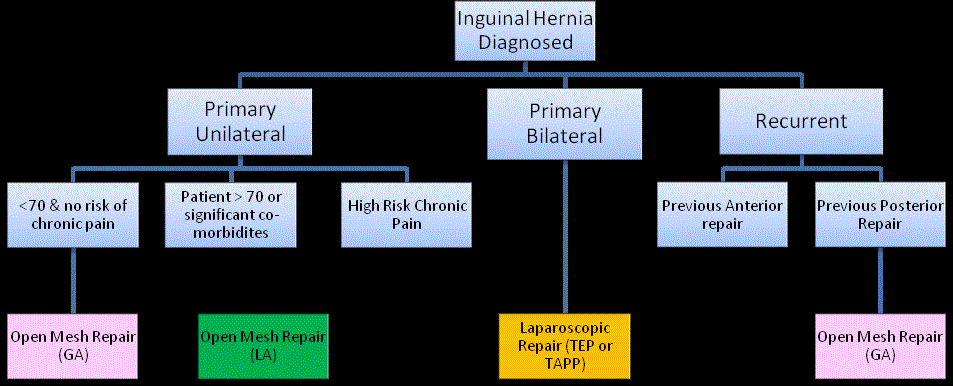
for this cohort of patients. The current ASGBI guidelines [18] for inguinal herniae are summarised
in (Figure 1). The latest figures [4] demonstrate that approximately 78% of surgical hernia repairs
are open and under GA, 17% laparoscopic and only 5% are open
under LA. With the advancement of technology, laparoscopic repair
is being utilised more favourably over the traditional open repair.
However it can only be done under GA which in elderly patients with
comorbidities carries a high risk.
The Walk-In-Walk-Out (WIWO) clinic based at the ACAD
unit of North West London Hospitals (NWLH) NHS Trust gives
patients the choice of having both their initial consultation and
hernia operation under LA on the same day. This is beneficial to the
increasing number of elderly patients with significant comorbidities
as well as being associated with significant cost savings and reduction
in acquired nosocomial infections.
Efficacy& Safety
A significant amount of literature evidence comparing open (LA
and GA) and laparoscopic techniques for hernia repair is reported.
Whilst laparoscopic intervention offers slightly better outcomes
in terms of chronic pain, haematoma formation, wound infection
and faster return to normal activities, it is associated with increased
seroma formation and an increase in serious complications such as
visceral and vascular injuries [2,18,19]. However a significant majority
of elderly patients with severe and significant comorbidities are not
suitable or are at a significantly higher risk of morbidity/mortality if
subjected to GA; besides needing a prolonged hospital stay with the
risk of nosocomial infections which can safely be reduced or avoided
if the surgery is performed in clinics like WIWO.
A recent large meta-analysis has shown that open hernia repair is
associated with a significantly lower recurrence rate (2.49% vs. 4.46%)
When compared to laparoscopic repair [19]. In a randomised control
trial (RCT), Nordin et al [20] randomised 616 Swedish patients
into LA, GA or regional anaesthesia (RA). LA was administered
by the surgeons, according to the method described by Amid et
al [21], whilst RA and GA were administered by an anaesthetist.
They reported that LA was associated with significantly less earlypostoperative
complications (P <0.0001) as compared to the other
groups, no micturition difficulties (0% LA vs. 29% RA vs. 8% GA, P
<0.0001), reduced unplanned overnight admission (3% vs. 14% vs.
22% P <0.0001) and shorter hospital stay (3.1 days vs. 6.2 days for
RA and GA, p =< 0.0001). No statistically significant difference was
reported amongst the groups with regards to returning to normal
activities (9 days), work (14 days) or leisure activities (15 days).
O’Dwyer et al [22] in a similar randomised study of 279 patients
in Scotland did not find any significant difference amongst the three
groups with respect to complication rate, recovery times or 1 year
outcomes. The LA group however did have significantly less pain
post-operatively, even though this effect was transient and pain
scores between the groups were the same after 24 hours. Interestingly,
patient satisfaction was reduced with LA in that only 84% of patients
saying they would recommend their procedure compared to 95% of
GA patients (P =0.011).
Sanjay & Woodward [23] in a retrospective analysis of 577 hernia
operations performed by one surgeon over 9 years reported that LA
repair had a significantly higher day case rate as compared to the
GA cases ( P <0.05), lower urinary retention rate (P =0.05), lower
analgesia requirements (P <0.05) and much higher satisfaction scores
(P <0.05). This study however lacked randomisation and had large
discrepancy between the group sizes.
Financial Aspects
In the current economic climate when many trusts are struggling
to balance the books, financial considerations are gaining importance
so long as patient care is not affected. McIntosh et al [24] in a cost
utility study reported that open surgery was found to be £320 cheaper
than laparoscopic surgery. Similar results were also reported by
McCormack et al [2] showing a cost difference of £300-350 between
open and laparoscopic procedures. Although these studies did not
compare LA and GA costs between the groups, they do unequivocally
highlight that as a class procedure, open repair is significantly
cheaper than laparoscopic repair. LA repair by virtue of requiring less
medication and monitoring or no pre-assessment, as in the Walk-
In-Walk-Out Clinic by Bhutiani [25] would always be cheaper than
a GA repair (open or laparoscopic). Indeed Khan et al [25] reported
that LA costs on average £441 less than a GA day case per patient
when they were operated on according to WIWO clinic protocol for
an open inguinal herniorraphy and £861 as an inpatient. He recorded
the savings for his 122 patients to be £50, 142 and £105, 042 over the
year for both the WIWO clinic and as an inpatient stay respectively.
This is a substantial saving that no hospital manager should argue
with. Kreckler et al [26] provided an in-depth direct cost comparison
between the various methods of inguinal hernia repair within the UK,
of which their results are summarised in Table 1.
Open LA repair is by far the most cost effective method of
inguinal hernia repair besides providing the same quality of care for
the patients. Kreckler et al [26] state evidence shows that LA repair
in not inferior to other modes of repair and advise that there should
be significant scope to increase the proportion of procedures taking
place under LA. The most important aspect of this analysis is that
a significant number of elderly patients with comorbidities needing
hernia repair are not only at a high risk with GA but also need
extensive investigations before surgery is offered. This significantly
adds to the cost, waiting time and risk of incarceration/strangulation
which can all be avoided by doing their procedure under LA.
As demonstrated, LA does carry many benefits and can be offered
to a patient demographic who once may not be deemed appropriate
to have surgery due to high anaesthetic risks. Another benefit of
the above WIWO service includes relieving the pressure off waiting
lists and hospital services, thus resulting in a higher turn-over of
operations performed and better patient-centred care. This also
allows General Practitioners (GPs) to have more input and control of
who they refer for hernia repairs and the associated funding behind it.
Once given the eligibility criterion, the GPs are able to book directly
onto the WIWO service and give a date of operation to the patient
from their consulting room.
With such benefits of performing procedures under LA,
it is imperative that the basic surgical skills acquired when
performing these operations are continued to be practiced and
taught in the surgical curriculum. The technique of conversion
to the open approach should always be learnt as a bail out option
if the laparoscopic approach is no longer considered a safe option,
however, these techniques should not be learned as a back-up plan
but instead should be utilised with the best operative conditions to
ensure a successful outcome. Thus surgical trainees should be taught
and required to learn open surgical techniques and reach proficiency
in these prior to advancing to laparoscopic surgery, so as to be able to
serve the aging population of the future.
Aim
We present a group of patients undergoing elective hernia repair
under LA who in many departments including ours would have and
have been refused surgery because of their comorbidities and their
resultant ASA grades. We report the cost-effectiveness of performing
the elective hernia repairs under LA as compared to the same
procedure done under GA. We also recommend that in a specific
cohort of patients, it is necessary to repair herniae under LA, due to
the high risk of GA. Such open surgical skills must not be allowed
to fade away due to the pressure of laparoscopic surgery by patients,
trainees and surgeons alike.
Figure 1
Table 1
Table 2
Figure 2
Methods
Patients undergoing hernia repair under local anaesthetic in the WIWO hernia clinic, under the care of a single consultant surgeon (RB) were recorded prospectively since 2006. Data including demographic details, medical co-morbidities and operation comments were recorded. These were respectively analysed and review of the notes was undertaken to establish complications. All patients were placed on the WIWO hernia list by the GPs in the covering area and assessed by a single surgeon before being offered a repair under LA during the consent process if deemed appropriate. The American Society of Anaesthesiologists (ASA) grade was used to classify co-morbidities and the group was divided into groups with ASA grade 1 and 2 and grades 3 and 4. Patients are administered 0.5mg - 1.5g of Midazolam IV at the time of operation pre-operatively. Each patient received a single dose of 1.5g Cefuroxime unless allergic to Penicillin, in which case the Trust’s antibiotic guidelines would stipulate an appropriate alternative. The surgeon then administers a 60ml mixture of 0.25% lignocaine with adrenaline (1:200,000) (maximum permitted is 7 mg/ kg body weight) and 0.25% bupivacaine with adrenaline (maximum permitted is 4 mg/kg body weight) to induce a nerve and infiltration block [27]. All procedures were performed with the same technique and the use of a mesh (tension-free Lichtenstein technique for inguinal hernias). Operations were performed both by consultant and trainee with the consultant scrubbed as the assistant. The total cost of performing each hernia repair under LA is then compared to the total cost of the repair under GA and then also including costs of an inpatient stay. This included the costs of medication, pre-operative outpatient consultations, investigations, pre-assessment clinics, anaesthetic reviews, consumables, post-operative stay and follow consultations. The cost of pre-assessment was deduced based on the investigations performed, the resources used and also the time of the nursing staff and junior doctor.
Results
696 operations were recorded between May 2006 and December
2013. 102 (14.7%) patients were female and 488 (85.3%) were male.
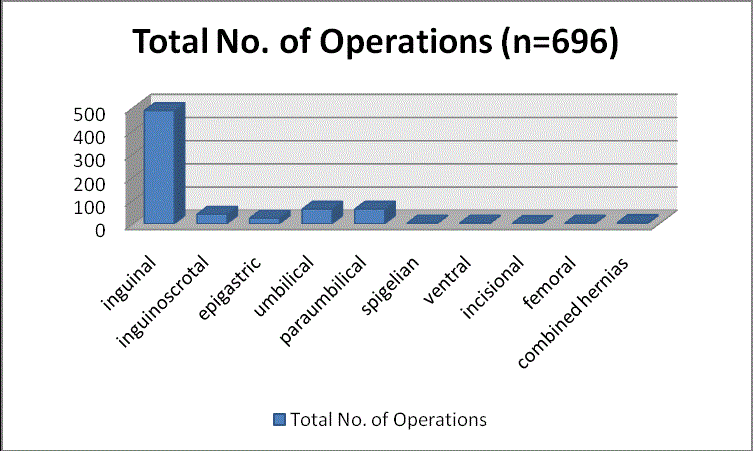
Of the total, 527 were inguinal, 63 umbilical, 63 paraumbilical, 24
epigastric, 3 femoral, 3spigelian, 41inguino-scrotal, 3 ventral, 2
incisional and 6 combined repairs (where 2 hernias were repaired at
the same time). 22 operations were for recurrence. 4 contained bowel
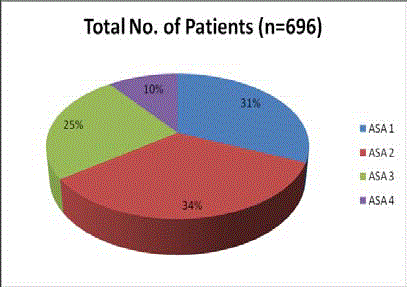
& omentum and 2 required omental resection. 31.5% of patients were
ASA- 1, 33.5% ASA- 2, 24.7% ASA- 3 and 10.3% ASA- 4. The age range
varied from 23 years to 95 years, with a mean age of 61.0 years. Of
those patients who were ASA 3 or 4, the mean age was 71.9 years. The
patients’ co-morbidities are summarised in Table 2. The distribution
of patients across the various ASA grades is shown in (Figure 2). Five
patients had documented refusal of general anaesthetic due to high
risk when assessed by anaesthetists. 145 patients (20.8%) were taking
anti-coagulation (warfarin/aspirin/clopidogrel).
Over the study period there was no mortality. There were
only five recorded complications - 6 (0.9%) patients developed
haematomas (five of which were taking anti-coagulation), 2 (0.3%)
post-op retention and were discharged home with a catheter, 2
(0.3%) developed seromas (one of which needed aspiration), 3 (0.4%)
developed chronic pain which all resolved by six months, and 1
(0.1%) developed a stitch granuloma.
Discussion
The WIWO database analysed data collected over a nine year
period but it still continues to accumulate to this day. The WIWO
hernia service was the first of its kind to be implemented in the NHS
and continues to provide successful surgical care to hundreds of
patients in the North West London area each year and helps to tackle
the waiting time of 18 weeks (as per the Government’s recommended
target time) for a hernia repair. According to Leff et al [2] in 2006, a
hernia repair in a private clinic would cost approx. £1300. This has
increased substantially to £2250. Likewise, to perform an open hernia
repair under a GA on the NHS today would cost £1440and as an
inpatient under GA is £1890. This is a large price for taxpayers to pay
compared to the significantly lesser amount of £1029 (in the NWLH
NHS Trust)of having the same hernia repair under LA as per the
WIWO hernia service which means they can go home the same day.
If the patient did need an overnight stay (mainly for social reasons)
then this would cost an added £300. This means that by performing
open hernia repairs under LA allows the patient to avoid the high
risk of GA, extensive investigations and nosocomial infections. In
addition, our Trust could potentially save £411.00 per patient when
compared to a day case hernia repair under GA; £861.00 compared to
an overnight stay under GA; and £561.00 if our LA repair needed an
overnight inpatient stay post-operatively for any reason.
So for the 696 operations performed in our WIWO hernia clinic,
over the 9 year period, the NHS would have only paid £716,184.00
(not taking into account for inflation) compared to an approx. sum of
£1,002,240.00 if those very same cases were performed under a GA.
This equates to a saving of £286,056.00 that can be better allocated
to other services. Studies designed to analyse the cost-effectiveness
have reported significant savings by performing hernia repairs
under LA when compared with open under GA [29] or laparoscopic
procedures [30]. From the data shown, we have found that 85% of
patients undergoing hernia repair were male and of these 70.7% had
an inguinal hernia repaired which is by far the most common type of
hernia repair in the UK. Unfortunately, the database did not record
whether the herniae were direct or indirect in nature. However the
repair procedure is the same for both and this should not make any
difference to the reported and recorded benefits of this approach and
such clinics.
Besides the financial benefit, the most important outcome to
note is that patients with ASA 3 & 4 (59% of our cohort) are able to
undergo the operation as a day case (without being exposed to the
risk of GA and nosocomial infections) and live a better quality of life
independently. A significant proportion of these patients would have
either been refused surgery due to their significant comorbidities and
resultant high anaesthetic risk, or forced to live with the discomfort/
pain of the hernia. These patients would have also undergone a
number of expensive tests and specialist opinion before the final
decision to operate or not to operate would be taken. In contrast a
significant majority could be offered the hernia repair under LA
without the need for expensive tests or specialist opinion with the
added waiting time making patients continued suffering.
Sanjay et al [23] looked at ASA grades 3 and 4 as being suitable for
day case hernia repair and found that 23% of their patients were ASA 3
and 5% ASA 4. They concluded that patients with ASA grades 3 and 4
can undergo day case inguinal hernia repair with similar complication
rates to patients with ASA grades 1 and 2, when surgery is performed
under local anaesthetic. As a result, it is understandable that patient
satisfaction would also increase as many patients would appreciate
the opportunity to alleviate their hernia symptoms. Gunnarsson et al
[28] in 1999 reported the outcome of patient satisfaction with elderly
patients and concluded that elective hernia repair in the elderly
population is highly appreciated by the patients and is worthwhile.
With an aging population who have increasing number and severity
of co-morbidities and advancing medical treatments, hernia repair
under LA can be offered routinely and we feel that age and comorbidities
are not a reason to refuse patients surgery. Hernia repair
under LA as a WIWO procedure offers cost reductions and provides
a quality of life without the risks associated with GA.
Figure 3
Conclusion
Despite being economically favourable and equivalent to other
surgical techniques in terms of recurrence and post-operative pain,
open repair under LA is still a vastly under-used method of treating
inguinal and abdominal wall herniae. With the ever increasing age
of the population, there will inevitably be many more patients who
cannot safely have general anaesthetic due to their co-morbidities
and thus require an intervention which excludes such a risk. The
current pressure for training surgeons to become proficient in
laparoscopic techniques risks the loss of the skill and competency
in undertaking this kind of repair and thus in future many of these
patients may not be able to have definitive repair, thus exposing them
to the risks that lie therein. With increasing emphasis of teaching/
learning laparoscopic skills due to advances of the last decade or so,
the art of basic surgical skills is becoming clouded by the era of socalled
‘keyhole surgery’, the Minimally invasive surgery, and robotic
surgery due to increasing patient demand and surgeon’s preference
because of the added excitement of the surgical skills. Unfortunately,
with the aging population and the increasing number and severity
of co-morbidities, a significantly high proportion of these patients
are likely to be refused surgery due to the risks associated with the
GA needed to undertake these new advances in keyhole surgery.
We have shown that LA hernia repair is superior to GA in terms of
cost-effectiveness, patient complications and satisfaction and thus
by extension preferable to laparoscopic repair in certain situations
i.e. in those patients who are unable to tolerate a GA due to age and
significant co-morbidities.
To be well equipped to serve the ageing population of tomorrow,
we propose that training surgeons of today and future should be
expected to do a mandatory number of hernia repairs under local
anaesthesia, in addition to being exposed to laparoscopic skills. We
also consider initiatives such as WIWO hernia services to show many
benefits for both healthcare organisations and the patients and should
be implemented in other hospital Trusts to allow for a more costeffective
NHS.
References
- http://www.hernia.org/
- Leff D, Bhutiani R. Give the patients the choice- the Walk in Walk out (WIWO) hernia clinic. J Ambulatory Surgery. 2006;12(3):125-9.
- NICE NIfCE-. Laparoscopic Surgery for Inguinal Hernia Repair. Technology Appraisal. 2004;83.
- NICE NIfCE. NICE implementation uptake report: Laparoscopic surgery for inguinal hernia repair; 2010.
- Jenkins JT, O’Dwyer PJ. Inguinal hernias. BMJ. 2008;336(7638):269-72.
- Van Den Heuvel B, Dwars BJ, Klassen DR, Bonier HJ. Is surgical repair of an asymptomatic groin hernia appropriate? A review. Hernia. 2011;15(3):251-9.
- Leubner KD, Ewigman B, Loven B, William M. Chop. What is the risk of bowel strangulation in an adult with an untreated inguinal hernia? Journal of Family Practice. 2007;56(12):1039-41.
- Nehme AE. Groin hernias in elderly patients. Management and prognosis. Am J Surg. 1983;146(2):257-60.
- Nilsson E, Kald A, Anderberg B, Bragmark M, Fordell R, Haapaniemi S, et al. Hernia surgery in a defined population: a prospective three year audit. Eur J Surg. 1997;163(11):823-9.
- Lewis DC, Moran CG, Vellacott KD. Inguinal hernia repair in the elderly. J R Coll Surg Edinb. 1989;34(2):101-3.
- Malek S, Torella F, Edwards PR. Emergency repair of groin herniae: outcome and implications for elective surgery waiting times. Int J Clin Pract. 2004;58(2):207-9.
- Martínez-Serrano MA, Pereira JA, Sancho JJ, López-Cano M, Bombuy E, Hidalgo J. Study Group of Abdominal Hernia Surgery of the Catalan Society of Surgery. Risk of death after emergency repair of abdominal wall hernias. Still waiting for improvement. Langenbecks Arch Surg. 2010;395(5):551-6.
- Malik AM, Khan A, Talpur KA, Laghari AA. Factors influencing morbidity and mortality in elderly population undergoing inguinal hernia surgery. J Pak Med Assoc. 2010;60(1):45-7.
- Kjaergaard J, Bay-Nielsen M, Kehlet H. Mortality following emergency groin hernia surgery in Denmark. Hernia. 2010;14(4):351-5.
- Nilsson H, Stylianidis G, Haapamäki M, Nilsson E, Nordin P. Mortality after groin hernia surgery. Ann Surg. 2007;245(4):656-60.
- Davies M, Davies C, Morris-Stiff G, Shute K. Emergency presentation of abdominal hernias: outcome and reasons for delay in treatment - a prospective study. Ann R Coll Surg Engl. 2007;89(1):47-50.
- Dahlstrand U, Wollert S, Nordin P, Sandblom G, Gunnarsson U. Emergency femoral hernia repair: a study based on a national register. Ann Surg. 2009;249(4):672-6.
- ASGBI. Groin Hernia Guidelines; 2013.
- Treadwell J, Tipton K, Oyesanmi O, Sun F, Schoelles K. Surgical Options for Inguinal Hernia: Comparative Effectiveness Review. Comparative Effectiveness Review 2012.
- Nordin P, Zetterström H, Gunnarsson U, Nilsson E. Local, regional, or general anaesthesia in groin hernia repair: multicentre randomised trial. Lancet. 2003;362(9387):853-8.
- Amid PK, Shulman AG, I L Lichtenstein. Local anesthesia for inguinal hernia repair step-by-step procedure. Ann Surg. 1994;220(6):735-7.
- O'Dwyer PJ, Serpell MG, Millar K, Paterson C, Young D, Hair A, et al. Local or General Anesthesia for Open Hernia Repair: A Randomized Trial. Ann Surg. 2003;237(4):574-9.
- Sanjay P, Woodward A. Inguinal Hernia Repair: Local or General Anaesthesia? Annals of The Royal College of Surgeons of England. 2007;89(5):497-503.
- Medical Research Council Laparoscopic Groin Hernia Trial Group. Cost–utility analysis of open versus laparoscopic groin hernia repair: results from a multicentre randomized clinical trial. Br J surg. 2001;88(5):653-61.
- Khan RA, Bhutiani RP. The Walk In Walk Out Hernia Clinic: A study of its cost effectiveness. Ambulatory Surgery. 2008;14(14).
- Kreckler S, McWhinnie D, Khaira H, Jackson I. The financial considerations of inguinal hernia surgery: does the surgical approach matter? Ambulatory Surgery. 2012;18:10-3.
- Leff DR, Nortley M, Dang V, Bhutiani RP. The effect of local cooling on pain perception during infiltration of local anaesthetic agents, a prospective randomised controlled trial. Anaesthesia. 2007;62(7):677-82.
- IbañezRde M, A Saied SA, Vallejo JA, Canales JM, Prieto CB, Sotos FE. Cost-effectiveness of primary abdominal wall hernia repair in a 364-bed provincial hospital of Spain. Hernia. 2011;15(4):377-85.
- Eklund A, Carlsson P, Rosenblad A, Montgomery A, Bergkvist L, Rudberg C; Swedish Multicentre Trial of Inguinal Hernia Repair by Laparoscopy (SMIL) study group. Long-term cost-minimization analysis comparing laparoscopic with open (Lichtenstein) inguinal hernia repair. Br J Surg. 2010;97(5):765-71.
- Gunnarsson U, Degerman M, Davidsson A, Heuman R. Is elective hernia repair worthwhile in old patients? Eur J Surg. 1999;165(4):326-32.