Research Article
Clinical and Radiological Midterm Results of the MAYO® Short Stem Total Hip Arthroplasty
Dietz J, Radetzki F, Zeh A, Delank KS and Wohlrab D*
Department of Orthopaedic Surgery and Traumatology, Martin-Luther- University of Halle-Wittenberg, Halle/Saale, Germany
*Corresponding author: David Wohlrab, Department of Orthopaedic Surgery and Traumatology, Martin-Luther- University of Halle- Wittenberg, Halle/Saale, Germany
Published: 16 Jul, 2018
Cite this article as: Dietz J, Radetzki F, Zeh A, Delank KS,
Wohlrab D. Clinical and Radiological
Midterm Results of the MAYO® Short
Stem Total Hip Arthroplasty. Clin Surg.
2018; 3: 2033
Abstract
Short stem arthroplasty of the hip is still controversial discussed. There are currently only a few
mid and long-term results for short stem hip arthroplasties published. The goal of this retrospective
single center study was to analyze the clinical and radiological midterm results of the Mayo® short
stem prosthesis in terms of subjective patient’s satisfaction, implant positioning and long term
stability. There were 51 patients with 61 Mayo® hip replacements included which were performed
from 2000 to 2003 based on osteoarthrosis. The Harris Hip Score (HHS) and Forgotten Joint Score
(FJS) were used to measure the patient’s satisfaction, hip function and awareness of the hip joint
in every day’s life. Based on radiographs leg length, stem positioning, femoral offset and Center of
Rotation (COR) were proved. The occurrence of radiolucent lines and heterotypic ossifications were
noted.
The mean follow up was 164 months. For the HHS, an average of 84 points and for the FJS an
average of 68% was measured. There was no leg length discrepancy and a mean stem position was
1,6° valgus. The femoral offset increased by an average of 6 mm. The COR was medialized by an
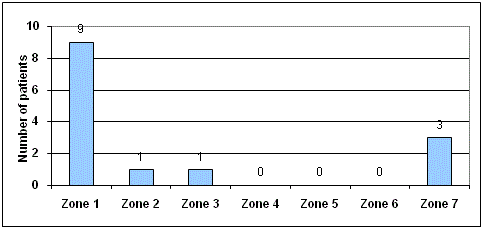
average of 6 mm. In 14 hips, radiolucent lines appeared in Gruen-Zones 1, 2, 3 and/or 7. Heterotypic
ossifications were detected in 27 Mayo® stems at stage 1 to 3 using Brooker classification. The Mayo®
prosthesis is a reliable stem with comparable midterm results compared to conventional stems.
That’s why it should be used for the treatment of younger patients.
Introduction
The total hip arthroplasty is one of the most successful surgical procedures in medicine
worldwide. The number of treatments is increasing because of good long-term stability and high
patient’s satisfaction. In Germany, this operation is one of the 20th most common interventions with
about 230.000 procedures per year and the number of surgeries increases every year. The number of
revision procedures is increasing as well to 9,5% in 2011 [1,2].
Studies with a mean follow up of 15 years shows a survival rate of metaphyseal and metadiaphyseal
anchored stem systems about 95% to 98% [3]. For that reason the use of short stems in younger and
active patients gets more and more frequent increasing quality of life [4]. The portion of patients with
an age under 60 years undergoing a THR is nearly 20% [5]. The decreasing mean age of the patients
will lead to an increasing number of revision procedures. Therefore, it is essential to use implants
with a proximal/metaphyseal load transfer to preserve the bone of the proximal femur during the
primary implantation. For these younger patients, the short stem hip arthroplasty was developed. It
should reduce stress shielding of the proximal femur and leads to bone stock preservation. In case of
revision surgery received bone stock permits the use of anatomical or distal fixed primary implants.
Furthermore, short stem prosthesis appropriate for minimally invasive procedures. On the other
hand, a shorter fixation could due to lower primary implant stability. To receive a long-term and of
bone-preserving stem fixation with shorter anchorage make high demands on the stem design [4].
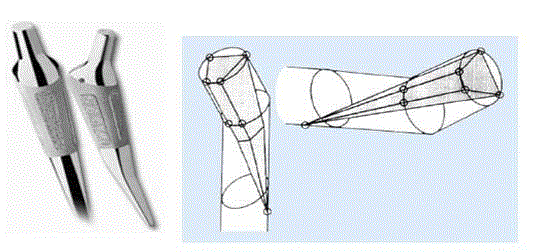
The Mayo® short stem (Zimmer Inc., Warsaw, USA) was developed in 1985 at the Mayo-Clinic
(Rochester, USA) and performed at the Martin Luther University of Halle-Wittenberg (Germany)
since 2000. It is cement less short stem hip prosthesis with a double conical design in A/P and
M/L plane ensuring immediate primary fixation of the prosthesis with a proximal/metaphyseal
load transfer [5]. It is made of a Titanium-Aluminium-Vanadium alloy and has a fibre-meshstructure
proximally [6]. The simple stem preparation leads to a shorter surgical time. The intraand
postoperative blood loss is reduced significantly. The reduction of the soft tissue damage
improves postoperative mobilization and rehabilitation as well as reduces postoperative pain [4].
In osteodensitometry an increasing bone density of the calcar femoris
could be demonstrated. This leads to reduced stress shielding and
bone atrophy. The principles of the metaphyseal load transfer were
confirmed using the Mayo® stem [7].
Short stem arthroplasty of the hip is still controversial discussed.
There are follow ups of five and seven years from Cruz-Vazquez et
al. and Tadeusz et al. [8,9] with a good mid-term stability. But up to
now long term results for short stem hip arthroplasty-especially of the
Mayo® short stem - are not available.
Figure 1
Material and Methods
The goal of this retrospective single center study was to analyze
midterm term results of the MAYO® short stem prosthesis (Zimmer
Inc., Warsaw, USA). We included 51 patients with 61 Mayo® hip
replacements, performed at the Martin Luther University Halle-
Wittenberg (Germany) from January 2000 to April 2003. We
measured subjective patient’s satisfaction, implant positioning and
long term stability.
We recorded date of surgery, gender, age, height and body weight,
calculated Body Mass Index (BMI).
The subjective patient’s satisfaction related to pain and hip
function was measured (1=very satisfied up to 5=very dissatisfied).
The patients were asked if they would agree to the hip replacement
again from today’s perspective. The answer options were ‘yes’,
‘maybe’ and ‘no’. The Harris Hip Score (HHS) measured the objective
patient’s satisfaction and hip function. The Forgotten Joint Score
(FJS) recorded the awareness of the hip joint in every day’s life.100
% in the FJS indicates the highest degree of ‘forgetting’. A low score
reflects the awareness of the presence of an artificial joint. Based on a
x-rays (pelvis AP view in standing position and the hip in Lauenstein
position)using a 25 mm reference metal ball at joint level we
measured the reconstruction of leg length, stem positioning, femoral
offset and Center of Rotation (COR). To compare the pre- and postoperative
situation we used preoperative X-rays or the opposite site.
The occurrence of radiolucent lines and heterotopic ossifications was
noted as well and were classified according to the Gruen Zones or
Brooker classification.
Results
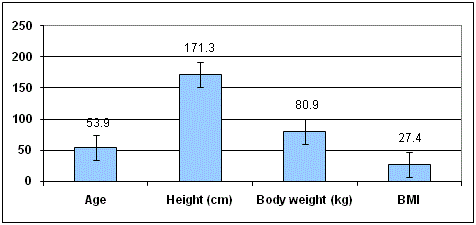
There were 31 out of 51 patients male (61%) and 20 female (39%).
In 32 cases the Mayo stem was implanted on the left side (52%) and
in 29 cases on the right (48%) side. The median age was 53.9 years (27
to 71 years), height 171.3 cm (157 cm to 185 cm), body weight 80.9 kg
(49 kg to 115 kg) and the calculated body mass index was 27.4 kg/m2
(19.1 kg/m2 to 39.8 kg/m2). The mean follow up was 164 months (13.7
years). The requested patient’s satisfaction related to pain amounted
1.4 (1 to 3) and related of function amounted 1.5 (1 to 4). All patients
would agree to the performed hip replacement again from today’s
perspective. The analysis of HHS data showed an average of 84 points
(34 to 96 points). The average for subscore "pain" constituted 39 (10
to 44 points) of 44 points and for subscore "function" 39.6 (19 to 47
points) of 47 points. Concerning the Forgotten Joint Score (FJS), in
which a maximum of 100% can be achieved, averaged 68% (0% to
100%). This means, that 68% of the patients don’t aware their hip
joint in every day’s life. In 32 hips, the FJS measured 80% to 100%.
The length discrepancy was measured with an average of -0.1 mm
(-18mm to + 14 mm). In 28 hips a leg extension (1 mm to 14 mm), in
25 hips a leg shortening (1 mm to 18 mm) and only in 8 hips were no
leg length discrepancy detected.
The stem alignments of all 61 hips were calculated mean 1.6°
valgus. 35 stems were implanted in a valgus position (0.9° to 11.6°)
and 17 stems in a varus position (0.4° to 7.6°). In only 9 hips there
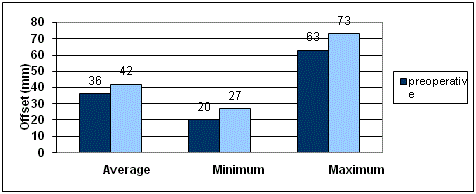
were a neutral alignment measured. The femoral offset was reduced
in 15 hips (1 mm to 26 mm) and increased in 46 hips (1 mm to 17
mm). In comparison to preoperative offset (an average of 36 mm)
and postoperative offset (an average of 42 mm) the femoral offset
increased averaged 6 mm.
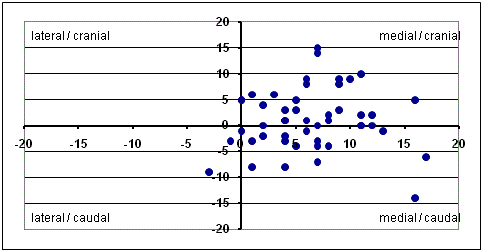
The COR was medialized in 52 cases and lateralized in 31 cases.
The horizontal COR was reduced from 36 mm to 30 mm and the
vertical COR was increased from 16 mm to 17 mm. The location of
the horizontal COR was medialized averaged 6 mm. The location of
the vertical COR wasn’t change (an average of 1 mm).
In 14 cases (23%), radiolucent lines appeared in GruenZones 1, 2,
3 and/or 7. There were no radiolucent lines in 47 cases (77 %). They
mostly occurred in GruenZones 1 and 7. In one case, radiolucent
lines were seen simultaneously in the Gruen-Zones 1 and 2 and in
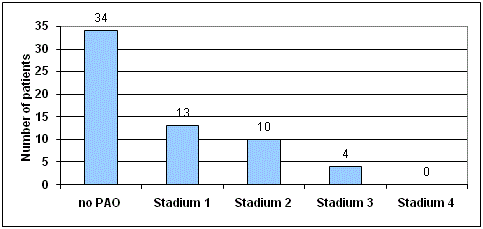
another case in the GruenZones 1 and 7. Heterotopic ossifications
were detected in 27 Mayo® stems (44 %) at stage 1 to 3 using
Brooker classification. In 34 cases (56 %), there were no heterotopic
ossifications. There was a cumulated occurrence of heterotopic
ossifications at stage 1 and 2.
We found are correlations between some of the single parameters
which are shown below.
There is a dependency between pain and function satisfaction
and the body mass index. An increasing BMI is related to lower
satisfaction in pain and function. A correlation between a decreasing
Harris Hip and Forgotten Joint Score is associated with increasing
BMI. Obese patients are more aware of their artificial hip joint in
everyday life than regular-weight patients.
An increasing leg shortening as well as a lengthening led to
a lower Harris Hip Score. Leg shortening is also combined with
lower Forgotten Joint Score. Patients with a postoperative leg length
shortening have a higher awareness of the presence of their artificial
hip joint.
Both, an increasing varus or valgus stem positioning was
accompanied by a decrease of the Harris Hip Score. In patients with
valgus stem position we measured a higher Harris Hip Score compared
to patients with a varus stem position. Moreover, the Forgotten Joint
Score was higher in patients with a neutral or valgus stem positioning
than in patients with varus stem positioning. An increasingly varus
stem position increases the awareness of the existing hip replacement.
Furthermore, no correlation between HHS and surgery-related
offset change could be determined. Patients with a postoperative
offset reduction achieved only a slightly higher Harris Hip Score
than patients with an offset magnification. But there is a dependency
between an offset change and a decrease in the total value of the
Forgotten Joint Score. The decrease of the FJS was significantly more
pronounced in an offset reduction than in an offset magnification.
Patients with postoperative offset magnification are less aware of their
articular joints than patients with an offset reduction.
There is an increase of the Harris Hip Score with increasing
medialization and/or cranialization, as well as a decrease in the
HHS with increasing lateralization and/or caudalization of the
COR. A higher percentage of the Forgotten Joint Score could also
be determined with increasing medialization and/or cranialization,
as well as a low percentage with increasing lateralization and/or
caudalization of the COR.
Furthermore, there is a correlation between a varus stem
positioning and leg length extension as well as a valgus stem
positioning and leg length shortening. There is also a strong correlation
between a valgus stem positioning and offset reduction, as well as a
varus stems positioning and offset increase. Neither a postoperative
medialization nor a postoperative lateralization of the COR led to a
significant change of the stem alignment. But a correlation between
the postoperative vertical COR and the stem alignment could be
determined. An increasing postoperative cranialization of the vertical
center of rotation was associated with an increased valgus stem
positioning.
Moreover, there is a dependency for a surgery-related change
of the horizontal center of rotation and an offset change. An
increasing medialization of the horizontal center of rotation due to
an enlargement of the femoral offset. There could be no correlation
established between a surgery-related change of the vertical center of
rotation and an offset change.
There is no significant gender-specific accumulation of
radiolucent lines and no correlation between BMI and radiolucent
lines. But radiolucent lines were observed frequently at neutral and
valgus stem alignment.
There is a correlation between the male sex and a reduced
patient’s functional satisfaction and the occurrence of periarticular
ossifications. However, no correlation between the BMI and the
occurrence of periarticular ossifications could be determined.
Figure 2
Figure 3
Figure 4
Figure 5
Figure 6
Discussion
The high patient’s satisfaction rate after short stem total hip
arthroplasty is described by different authors. Wittenberg et al.
documented in 85% very satisfied patients out of 85 Metha® stems.
Tadeusz et al. described for the Mayo® stem very good results after 7
years as well [10,7].
The midterm results of different short stems as well as conventional
stems are also comparable with the good results in Harris Hip and
Forgotten Joint Score presented in our study. A certain bias of the
findings resulted from the fact that the results of the scores in the
patients with double-sided hip prosthesis implantation were also
considered twice in the evaluation. There was also a reduction in the
objectively measured overall percentage of the FJS due to subjective
complaints of other diseases of the musculoskeletal system, for
example by a degenerative spinal column or a gonarthrosis.
With the implantation of a Mayo® short stem the leg length could
be reconstructed well. The leg length extension after the implantation
of a hip end prosthesis, which has been described and discussed
frequently in the literature, could not be confirmed.
In this study, there is a variation of shortening up to 18 mm and
lengthening up to 14 mm. In the case of shortening of the leg length
preoperatively there was fulminant femoral head destruction due to
a femur head necrosis with a clearly cranialized center of rotation. In
the case of the leg length extension only the X-ray image of the nonreplaced
contra lateral hip joint was available for the evaluation of the
preoperative situation. A possible cause for the leg length difference
could not be determined here.
Leg length modification can also be influenced by other factors
such as the implant design factors (length of the head implant,
CCD angle, stem offset) as well as axis of the implanted stem and
the position of the vertical center of rotation (cup implantation).
A postoperative leg length discrepancy depends decisively on the
preoperative planning, implant selection and position.
The average valgus stem position in this study was only partly
comparable with the current literature. In a study of 32 implanted
Mayo® stems from Kamada et al. [11] a valgus stem position was
described in comparison to the none treated opposite side. Wittenberg
et al. [10] described in the five-year follow up of 250 Metha® stems a
neutral shaft position (130° to 140°) in 74, 6%. In the follow up of 202
Nanos® stems Ettinger et al. [12] reported a change in the CCD angle
from 133,8° preoperatively to 134,6° postoperatively.
There seems to be a different implantation behavior of single short
stem systems. Furthermore, there is a greater variance between a varus
and valgus stem positioning, especially in short stems. Further studies
with a focus on the anatomical hip remain to be seen. There was a good
reconstruction of the femoral offset (average offset magnification
of 6 mm) after the implantation of a Mayo® stem. Investigations by
John Charnley have shown that an offset magnification extends the
lever arm of the abductor muscles and reduces the required muscle
strength, which due to a decrease in joint loading. By an offset
magnification, the dislocation rate and the impingement risk are also
reduced by an increased soft tissue tensioning. Moreover, the ROM
is increased. A reduced offset caused a limping gait (Trendelenburg
limping) due to the abductor weakness as well as lateral hip pain and
leads to instability and subluxation [13,14]. Little et al. [15] described
in a 49 months f/u of 43 uncemented total hips a decreasing wear rate
in case of offset magnification less than 5 mm. In a follow-up of 17
patients with a bilateral THR (same implant designs with different
offsets), an increased PE wear rate in the group with larger offsets
was shown by Sakalkale et al. [16] after 5,7 years f/u. Kleemann et al.
[17] described an increasing risk of implant failure with increasing
femoral offset (max. +5 %). Thien et al. [18] also documented an
increased risk of revision with increasing offset magnification. Due
to the above-mentioned advantages of an offset magnification, the
recommendation for a postoperative offset magnification of up to 5
mm can be given. This recommendation could be met in this study.
The current literature provides considerably different results for
the postoperative femoral offset after the implantation of a total hip
replacement, so that there appears to be a correlation between offset
and stem design. However, a reduction of the femoral offset can also
be caused by a medialization of the cup position. The femoral offset
is also influenced by a lateralization of the trochanter major and an
extension of the prosthesis neck with an accompanying extension of
the leg length.
In 2011 Dastane et al. [19] described a cranialization of the
center of rotation up to 6 mm and a medialization of the center of
rotation up to 5 mm as an acceptable reconstruction. We showed
with the presented results a COR medialization on average 6 mm and
canalization on average 1 mm using a Mayo® short stem. Based on
findings of Dastane et al. with the Mayo® short stem the COR can
be optimally reconstructed. The influence of the cup position on the
horizontal and vertical center of rotation must to be considered again.
To prove the long-term stability of the Mayo® short stem
prosthesis, the appearance of radiolucent lines was examined. In
the current literature, the frequent occurrence of radiolucent lines,
especially in the GruenZones 1 and 7, is described in short stems and
in conventional stem prostheses as well [20,21].
The reason for this accumulated occurrence seems to be micro
motions caused by the proximal load transfer. In the absence of
progression of the existing radiolucent lines an impact of long term
stability is not expected.
In this study the occurrence of PAO was observed in stage 1 and 2
using Brooker classification. In the current literature, the occurrence
of a periarticular ossification is also described in stage 1 and 2 both in
short stems and in conventional stem prostheses [10,21,22].
The cause for a PAO still does not seem to be clarified yet. The
occurrence of a PAO was observed above all in the first postoperative
year. It seems that stem design is not a predicting factor for
appearance of PAO but there are correlations between PAO and intra
operative soft tissue damage caused by lateral or anterolateral surgical
approaches [23-25].
These results of this retrospective mono center study could show
that the midterm results of the Mayo® short prosthesis are comparable
with results of conventional stems.
References
- Statistisches Bundesamt.
- Falez F, Casella F, Panegrossi G, Favetti F, Barresi C. Perspectives on metaphyseal conservative stems. J Orthop Traumatol. 2008;9(1):49-54.
- Effenberger H, Imhof M, Witzel U, Rehart S. Cement less stems of the hip. Current status. Orthopade. 2005;34(5):477-500.
- Hube R, Zaage M, Hein W, Reichel H. Early functional results of a short stem prosthesis of the hip joint with metaphyseal-intertrochanteric anchoring. Orthopedist. 2004;33(11):1249-58.
- Jerosch J. Is shorter really better? Philosophy of short stem prosthesis designs. Orthopade. 2011;40(12):1075-83.
- Meldrum RD, Willie BM, Bloebaum RD. An assessment of the biological fixation of a retrieved Mayo femoral component. Iowa Orthop J. 2003;23:103-7.
- Hagel A, Hein W, Wohlrab D. Experience with the Mayo conservative hip system. Acta Chir Orthop Traumatol Cech. 2008;75:288-92.
- Cruz-Vazquez FJ, De la Rosa-Aguilar M, Gomez-Lopez CA. Evaluation of the uncemented Mayo femoral stem. The first 10 years. Acta Ortop Mex. 2011;25(2):108-13.
- Tadeusz N, Adam N, Lukasz N. Total hip replacement in young patients with use of MAYO prosthesis-early result of treatment. Chir Narzadow Ruchu Ortop Pol. 2007;72(5):319-21.
- Wittenberg RH, Steffen R, Windhagen H, Bucking P, Wilcke A. Five-year results of a cementless short-hip-stem prosthesis. Orthop Rev (Pavia). 2013;5(1):e4.
- Kamada S, Naito M, Nakamura Y, Kiyama T. Hip abductor muscle strength after total hip arthroplasty with short stems. Arch Orthop Trauma Surg. 2011;131(12):1723-9.
- Ettinger M, Ettinger P, Ezechieli M, Buermann S, Budde S, Calliess T, et al. CCD and offset after Nanos short stem in total hip arthroplasty. Technol Health Care. 2013;21(2):149-55.
- Charnley J. Low friction arthroplasty of the hip. Springer Verlag. 1979;336.
- Jerosch J. Soft tissue balancing in the context of hip arthroplasty. OUP. 2013;360366.
- Little NJ, Busch CA, Gallagher JA, Rorabeck CH, Bourne RB. Acetabular polyethylene wear and acetabular inclination and femoral offset. Clin Orthop Relat Res. 2009;467(11):2895-900.
- Sakalkale DP, Sharkey PF, Eng K, Hozack WJ, Rothman RH. Effect of femoral component offset on polyethylene wear in total hip arthroplasty. Clin Orthop Relat Res. 2001;388:125-34.
- Kleemann RU, Heller MO, Stoeckle U, Taylor WR, Duda GN. THA loading arising from increased femoral ante version and offset may lead to critical cement stresses. J Orthop Res. 2003;21(5):767-74.
- Thien TM, Karrholm J. Design-related risk factors for revision of primary cemented stems. Acta Orthop 2010;81:407-12.
- Dastane M, Dorr LD, Tarwala R, Wan Z. Hip offset in total hip arthroplasty: quantitative measurement with navigation. Clin Orthop Relat Res. 2011;469(2):429-36.
- Zweymuller KA, Schwarzinger UM, Steindl MS. Radiolucent lines and osteolysis along tapered straight cementless titanium hip stems: a comparison of 6-year and 10-year follow-up results in 95 patients. Acta Orthop. 2006;77(6):871-6.
- Brinkmann V, Radetzki F, Delank KS, Wohlrab D, Zeh A. A prospective randomized study comparing the clinical, radiological and osteodensitometric results after implantation of the Metha® and Nanos® short stem prosthesis. J Orthop Traumatol. 2015;16:237-43.
- Gierse H, Scherberich M, Fuchs S. Does the shape of the prosthesis have an influence on the development of periarticular ossification? Z Orthop your Grenzgeb. 1994;132:516-20.
- Regis D, Sandri A, Sambugaro E. Incidence of heterotopic ossification after surface and conventional total hip arthroplasty: a comparative study using anterolateral approach and indomethacin prophylaxis. Biomed Res Int. 2013;2013:293528.
- Bischoff R, Dunlap J, Carpenter L, DeMouy E, Barrack R. Heterotopic ossification following uncemented total hip arthroplasty. Effect of the operative approach. J Arthroplasty. 1994;9:641-4.
- Eggli S, Woo A. Risk factors for heterotopic ossification in total hip arthroplasty. Arch Orthop Trauma Surg. 2001;121:531-5.