Case Report
Intrahepatic Bile Duct Cyst Calculus and Gallbladder Stones Treated With Surgery: A Case Report
Koichi Kimura1,2*, Yasuhiro Doi1, Yasushi Takii1, Ryosuke Tsutsumi1, Kensuke Kudou2, Norifumi Tsutsumi1, Tetsuo Ikeda2 and Soichiro Maekawa1
1Department of Internal Medicine, Munakata Medical Association Hospital, Japan
2Depatment of Endoscopy and Endoscopic Surgery, Fukuoka Dental College, Japan
*Corresponding author: Koichi Kimura, Department of Endoscopy and Endoscopic Surgery, Fukuoka Dental College Fukuokashi, Japan
Published: 16 Jul, 2018
Cite this article as: Kimura K, Doi Y, Takii Y, Tsutsumi R,
Kudou K, Tsutsumi N, et al. Intrahepatic
Bile Duct Cyst Calculus and Gallbladder
Stones Treated With Surgery: A Case
Report. Clin Surg. 2018; 3: 2028.
Abstract
Background: Intrahepatic bile duct cyst calculus is an extremely rare case. We report a case of
intrahepatic bile duct cyst calculus and gallbladder stones treated with surgery.
Case Presentation: A 76-year-oldwoman consulted our institution because of epigastric pain.
Her blood chemistry results showed elevation of hepatic-cystic system enzymes. Computed
tomography revealed cholecystitis with gallbladder stones and stones with in an intrahepatic bile
duct cyst at the root of the right hepatic duct, which was suspected as a sub-gallbladder. Endoscopic
retrograde cholangiopancreatography and other examinations were performed. Finally, the patient
was diagnosed with double gallbladder stones and cholecystitis, and she underwent surgery.
Intrahepatic bile duct cyst (considered as accessory gallbladder) and gallbladder resections and
hepaticojejunostomy were performed with laparotomy. She progressed well post operatively
and was discharged from the hospital on postoperative day 19. Postoperative histopathological
examinations showed a definite diagnosis of intrahepatic bile duct cyst calculus and gallbladder
stones with cholecystitis.
Conclusion: We report a case of intrahepatic bile duct cyst calculus and gallbladder stones treated
with surgery. Decision of surgical procedure by the location of intrahepatic bile duct cyst is essential
for the treatment.
Keywords: Intrahepatic bile duct cyst calculus; Type V bile duct cyst; Gallbladder stone
Background
Acute cholecystitis is the most frequent complication of cholelithiasis, accounting for up to 20%
of patients with symptomatic gallstones [1]. Acute cholecystitis is one of the most frequent causes
of urgent admission at surgical departments due to the high prevalence of cholelithiasis [2]. The
Todani classifications chemeis typically used to classify bile duct cysts based on their location and
morphology [3]. Todani type V cysts are described as single or multiple intrahepatic cystic dilations
with no extra hepatic involvement. Type V cysts are a rare form of bile duct cyst, and solitary type
V cysts are even less common, with an estimated incidence of 1:1,000,000 [4]. Solitary diverticular
type V cysts are exceedingly rare.
Complications associated with bile duct cysts include bile duct stricture, cholangitis, bile duct
stones, pancreatitis and biliary malignant changes. The risk of biliary malignancies increases with
age [5]. Subsequently, bile duct cysts are surgically managed with complete cyst excision and
hepaticojejunostomy reconstruction or hepatectomy [6].
Here, we present a patient with so litary type V intrahepatic bile duct cyst with calculus and
gallbladder stones treated with surgery.
Case Presentation
The patient was a 76-year-old female with epigastric pain. Her blood chemistry study
results showed elevation of hepatic-cystic system enzymes (as part at aminotransferase: 193U/L,
alanineamino transferase: 238U/L, alkaline phosphatase: 826U/L, gamma-glutamyl transpeptidase:
559U/L, total bilirubin: 4.0mg/dL, C-reactive protein: 3.93 mg/dL). Computed tomography
revealed gallbladder enlargement, gallbladder wall thickening with gallbladder stones, common
bile duct expansion (8 mm), common bile duct stones and stones with in an intrahepatic cyst at
the root of right hepatic duct, suspected as an accessory gallbladder
(Figure 1A and 1B). Magnetic resonance cholangiopancreatography
showed the same findings as computed tomography (Figure 2A
and 2B). Subsequently, she was diagnosed with common bile
duct stones, double gallbladder stones, and cholecystitis, and
endoscopic retrograde cholangiopancreatography was performed.
Cholangiopancreatography showed filling defects in the gallbladder,
common bile duct, and intrahepatic cyst at the root of the right
hepatic duct, which was suspected as an accessory gallbladder (Figure
3). Endoscopic sphincterotomy was performed for the common
bile duct stones. No malfusion of the pancreaticobiliary ducts was
observed. Two black stones were discharged from the common bile
duct. One biliary stent was placed into the common bile duct.
Finally, surgical procedure was performed for double gallbladder
stones and cholecystitis. First, laparoscopic surgery has been
planned; however, almost all the intrahepatic bile duct (considered
as accessory gallbladder) existed in the liver parenchyma (Figure
4A). Subsequently, intrahepatic bile duct (considered as accessory
gallbladder) and gallbladder resections and hepaticojejunostomy
were performed with laparotomy. She progressed well postoperatively
and was discharged from the hospital on postoperative day 19.
Postoperative histopathological examinations revealed no muscular
layer in the wall of the intrahepatic cyst (considered as accessory
gallbladder) (Figure 4B), and the definite diagnosis was intrahepatic
bile duct cyst calculus and gallbladder stones with cholecystitis.
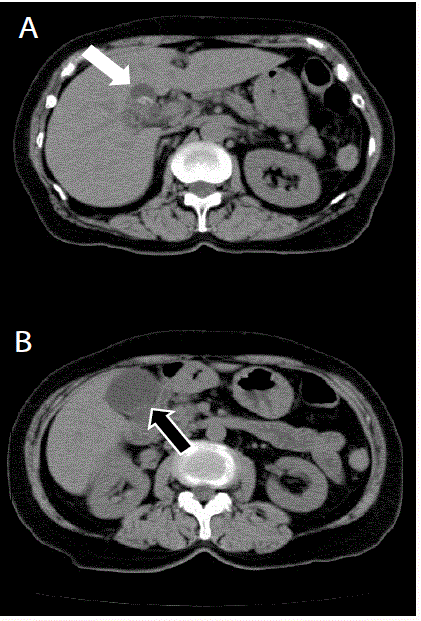
Figure 1
Figure 1
Cystic structure (white arrow) (A) and normal gallbladder (black
arrow) (B) are confirmed by computed tomography.
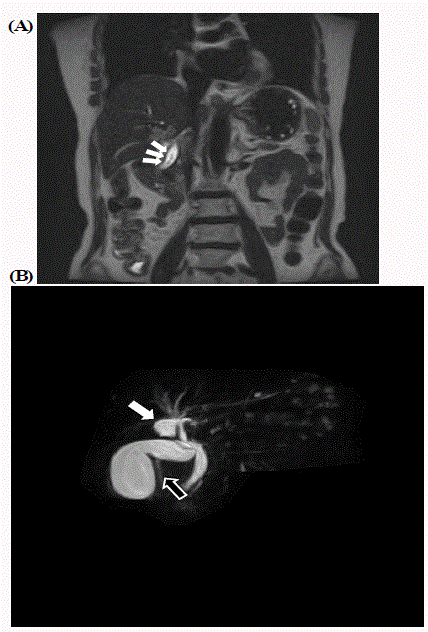
Figure 2
Figure 2
A: Common bileduct stones (white arrows) are confirmed by
magnetic resonance cholangiopancreatography. B: Cystic structure (white
arrow) and normal gallbladder (black arrow) are also confirmed by magnetic
resonance cholangiopancreatography.
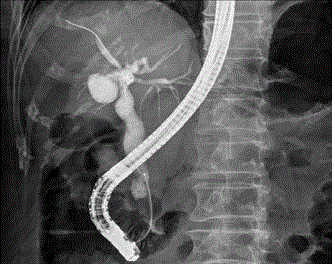
Figure 3
Figure 3
Cystic structure (white arrow) is confirmed by endoscopic
retrograde cholangiopancreatography.
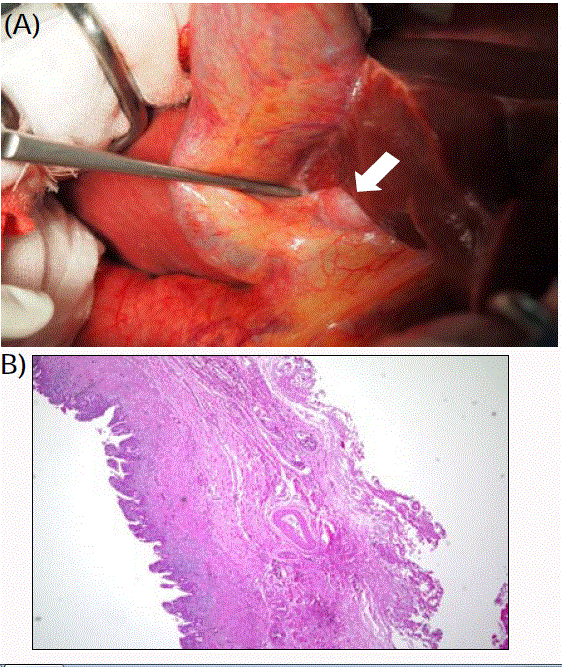
Figure 4
Figure 4
A: Intraoperative image of the duct cyst during laparotomy (white
arrow). Almost all intrahepatic bileducts are in the liver parenchyma. B:
Microscopic image of the intrahepatic bileduct cyst. The muscular layer
structure of the gallbladder could not be seen in the intrahepatic bileduct cyst.
Discussion
Bile duct cysts are rare worldwide, with an estimated incidence
of 1:100,000-1:150,000 [7,8]. Early identification and treatment of
bile duct cysts is recommended due to the potential for liver injury
and malignant degeneration, presumably due to chronic cholestasis
and cholangitis [9]. The risk of degeneration to cholangio carcinoma
is the highest for intrahepatic cysts [10]. The case reported here is
exceptional because the intra hepatic cyst appears to be a single,
diverticular lesion with no other apparent malformations of the
biliary tree. To the best of our knowledge, only two previous cases of
a solitary diverticular type V cyst have been reported in the literature
[11,12].
In contrast, the preoperative diagnosis of this case was double
gallbladder stones. Double gallbladder is a rare congenital anomaly,
reported in 2 (0.02%) of 9921 autopsy cases and 3 (0.03%) of 9970
cases in a radiographic survey [13]. Gorecki et al. [14] reported a case
of double gallbladder in a 69-year-old female with stones in both
gallbladders with the accessory gallbladder originating from the left
hepatic duct. In 2009, Kim et al. [15] have reported a 78-year-old male
with duplicate gallbladder with stones arising from the left hepatic
duct 10 years after an open cholecystectomy. However, postoperative
histopathological examinations revealed no muscular layer in the wall
of the intrahepatic cyst (considered as accessory gallbladder) in this
case.
Complications associated with adult choledochal cysts include
bile duct stricture, cholangitis, bile duct stones, pancreatitis, and
biliary malignant changes. Biliary malignancy is the most important
among these complications. The incidence of biliary malignancy in
adult choledochal cysts is 9.8% to 30%. The risk of biliary malignancies
increases with age. Among 204 cases of adult choledochal cysts, Cho
et al. [16] found that the incidence of biliary malignancies was 3.9%
for the 18-30 years age group, 6.9% for the 31-40 years age group, 10%
for the 41-50 years age group, 10.7% for the 51-60 years age group,
and 37.5% for the 61-67 years age group. Possible carcinogenic factors
included chronic inflammation, cholestasis, and sparse distribution
of the protective mucin-secreting glands of the bile duct. Under the
influence of these factors, chronic irritation, ulceration, regeneration
and metaplasia of the epithelium of the cystic wall may develop,
and invasive carcinoma may eventually occur. The most common
type of biliary cancer is adenocarcinoma; only few cases have been
reported for undifferentiated carcinoma, squamous cell carcinoma,
and adenosquamous carcinoma [5].
Aggressive treatment (total resection or transplantation) has been
proposed to lower the risk of subsequent cholangio carcinoma [4].
In the current case, considering the presence of the stones and the
relative respectability of the cyst, the benefits of surgical resection have
been decided to outweigh the potential risks. However, this case is
solitary intrahepatic bile duct, and the cyst is partially outside the liver
parenchyma. Subsequently, surgical procedures, such as hepatectomy
or transplantation, are excessive invasive surgery. Intrahepatic bile
duct cyst and gallbladder resection and hepaticojejunostomy seem to
be reasonable procedure for this case.
Conclusion
In conclusion, we report a case of solitary type V intrahepatic bile
duct cyst with calculus and gallbladder stones treated with surgery.
Decision of surgical procedure by the location of intrahepatic bile
duct cyst is essential for the treatment.
References
- Strasberg SM. Clinical practice. Acute calculous cholecystitis. N Engl J Med. 2008;358(26):2804-11.
- Al Jundi W, Cannon T, Antakia R, Anoop U, Balamurugan R, Everitt N, et al. Percutaneous cholecystostomy as an alternative to cholecystectomy in high risk patients with biliary sepsis: a district general hospital experience. Ann R Coll Surg Engl. 2012;94(2):99-101.
- Todani T, Watanabe Y, Narusue M, Tabuchi K, Okajima K. Congenital bile duct cysts:classification, operativeprocedures ,and review of thirtyseven cases including cancer arising from choledochalcyst. Am J Surg. 1977;134(2):263-9.
- Mabrut JY, Partensky C, Jaeck D, Oussoultzoglou E, Baulieux J, Boillot O, et al. Congenital intrahepatic bile duct dilatation is a potentially curable disease: long-term results of a multi-institutional study. Ann Surg. 2007;246(2):236-45.
- Liu QY, Lai DM, Gao M, Wan YL, Lin XF, Li HG, et al. MRI manifestations of adult choledochal cysts associated with biliary malignancy: a report of ten cases. Abdom Imaging. 2013;38(5):1061-70.
- Mabrut JY, Bozio G, Hubert C, Gigot JF. Management of congenital bile duct cysts. Dig Surg. 2010;27(1):12-8.
- Singham J, Schaeffer D, Yoshida E, Scudamore C. Choledochalcysts: analysis of disease pattern and optimal treatment in adult and paediatric patients. HPB (Oxford). 2007;9(5):383-7.
- Jablonska B. Biliary cysts: etiology, diagnosis and management. World J Gastroenterol. 2012;18(35):4801-10.
- Diao M, Li L, Cheng W. Timing of surgery for prenatally diagnosed a symptomatic choledochal cysts: a prospective randomized study. J Pediatr Surg. 2012;47(3):506-12.
- Edil BH, Cameron JL, Reddy S, Lum Y, Lipsett PA, Nathan H, et al. Choledochal cyst disease in children and adults: a 30-year single institution experience. J Am Coll Surg. 2008;206(5):1000-5.
- Brown DK, Kimura K, Sato Y, Pringle KC, Abu-Yousef MM, Soper RT. Solitary intrahepatic biliary cyst: diagnostic and therapeutic strategy. J Pediatr Surg. 1990;25(12):1248-9.
- Burke ZD, Boechat I, Tabsh K, Deugarte DA. Solitary diverticular type V bile duct cyst. Pediatr Surg Int. 2014;30(2):245-7.
- Boyden EA. The accessory gall-bladder: an embryological and comparative study of aberrant biliary vesicles occurring in man and the domestic mammals. A J A. 1926;38(2):177-231.
- Gorecki PJ, Andrei VE, Musacchio T, Schein M. Double gall bladder originating from left hepatic duct: a case. Report and review of literature. JSLS. 1998;2(4):337-9.
- Kim RD, Zendejas I, Velopulos C, Fujita S, Magliocca JF, Kayler LK, et al. Duplicate gall bladder arising from the left hepatic duct: report of a case. Surg Today. 2009;39(6):536-9.
- Cho MJ, Hwang S, Lee YJ, Kim KH, Ahn CS, Moon DB, et al. Surgical experience of 204 cases of adult choledochal cyst disease over 14 years. World J Surg. 2011;35(5):1094-102.