Surgical Technique
Monovision Strategies: Our Experience and Approach on Pseudophakic Monovision
Misae Ito CO* and Kimiya Shimizu
Department of Ophthalmology, Sanno Hospital, Japan
*Corresponding author: Misae Ito, Department of Opthalmology, Eye Center, Sanno Hospital, 8-10-16 Akasaka, Minato-ku, Tokyo, 107-0052, Japan
Published: 16 Jul, 2018
Cite this article as: Misae Ito CO, Shimizu K. Monovision
Strategies: Our Experience and
Approach on Pseudophakic
Monovision. Clin Surg. 2018; 3: 2027.
Surgical Technique
While advancing surgical techniques continually improve modern cataract surgery, the rise of refractive surgery also plays a part in elevating patients’ expectations for presbyopia correction today. Current lens-based options to combat the onset of presbyopia include premium IOLs (ig. multifocal and accommodating) and monovision. But regardless of the technique we use, today’s patients expect an improvement in their quality of vision and a rejuvenation of their accommodation. Depending on the selected strategy, however, this may be challenging. Monovision strategy is based on the assumption that it will be easier to suppress blur in the non dominant eyes than in the dominant eyes, with the dominant eyes usually being corrected for distance and the non dominant eyes for near vision. Anisometropia, a relative difference in the refractive state of the two eyes, is not uncommon in myopic and hyperopic patients [1]. This article reviews the monovision methods available to us today.
Pseudophakic Monovision Strategies
When differences in bilateral visual acuity are identified before surgery, however, the visual
performance of the eyes must be balanced to allow adjustment tests to ensure maintaining the
patient’s visual performance after surgery.
Conventional monovision
The use of standard monofocal IOLs for monovision in the pseudophakic eye is limited
because these IOLs do not preserve natural accommodation. In our practice, the target refraction is
emmetropia (0 to −0.5 D) in the dominant eye and myopia (−1.5 to −2.5 D) in the non dominant.
A large degree of anisometropia is needed to obtain excellent near visual acuity, and a resulting
relative decrease of near stereopsis occurs. We have, however, performed pseudophakic monovision
with good results. A key point for success of monovision is patient selection [2,3]. For successful
monovision outcomes, the following conditions should be met: Patients should have excellent
distance UCVA in the dominant eye, near exophoria angle of less than 12 prism diopters, and
age greater than 60 years. At our center, we choose monovision carefully in patients with large
exophorias, vertical deviation or strabismus. If the patient has more than 1.0 D of astigmatism but
desires pseudophakic monovision, we choose from one of the following strategies: cataract surgery
with a limbal relaxing incision, photo astigmatic keratectomy, or implantation of a toric IOL. In
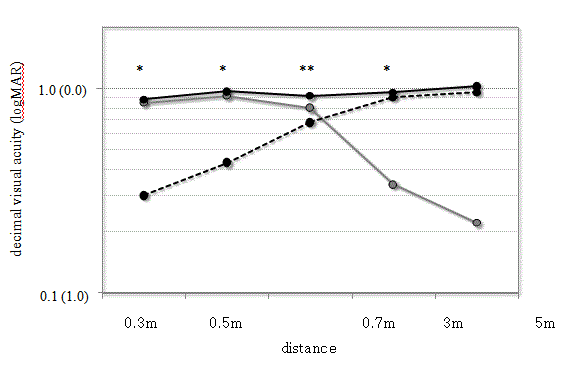
our experience (Figure 1 and Table 1), Log MAR of the binocular
UDVA was at least 0.10 in 100% of patients, with 83% achieving J2
or better binocular UNVA. From middle distance to near distances,
more favorable results were obtained relative to monocular visual
acuity (0.3, 0.5, 3m; p<0.05, 0.7m; p<0.01). Near stereopsis in patients
who shifted from exophoria to intermittent exotropia decreased,
but no serious problems have been observed. The percentage of
spectacle dependence was 93% preoperatively, 54% (1 year), 27% (5
years), and 10% (10 years). The proportion of patients responding as
“acceptable,” “satisfied,” and “very satisfied” categories was 90.0%,
96.7%, and 100% at 1, 5, and 10 years post-surgery, respectively.
Mild monovision
We currently use monovision with pseudo accommodation in
patients with pupil diameters of less than 2.5 mm [4]. In our practice,
the target refraction is emmetropia (0 to −0.5 D) in the dominant
eye and slight myopia (−1.0 to −1.5 D) in the non dominant eye if
the pupil diameter is 2.5 mm or less. This method achieves the same
positive effects, maintains contrast sensitivity and stereopsis, and
causes less anisometropia. In our experience, at least 90% of patients
are satisfied with mild monovision. Pupil diameter decreases with
age, and therefore this approach to monovision is more beneficial for
elderly patients. But regardless of the pupil diameter patients have, if
the patient has more than 12 prism diopters of near-exophoria angle
but desires pseudophakic monovision, we also choose this target
refraction. In our results, near visual acuity decreased, but no patients
shifted from intermittent exotropia to exotropia, near stereopsis was
maintained.
Hybrid monovision
In this strategy, we implant a monofocal IOL in the dominant
eye and a diffractive multifocal IOL in the non dominant eye. With
this type of binocular vision, patients do not complain of discomfort,
and more than 85% are satisfied with their results. We have noticed
a relative decrease in stereopsis; however, the normal range was
maintained in 63% of patients. No serious complaints have been
reported after hybrid monovision [5].
Figure 1
Figure 1
Uncorrected visual acuity after pseudophakic monovision.
(Solid black line: Binocular visual acuity; Dotted black line: Dominant eye visual acuity; Solid gray line: Nondominant
eye visual acuity).
Table 1
Conclusion
Monovision can effectively compensate for accommodative loss after cataract surgery when a careful patient selection process is followed. In our clinical results, pseudophakic monovision was an effective approach for correcting presbyopia throughout the 10- year observation period when a careful patient selection process is followed. Currently, the market is shifting from multifocal IOLs to EDOF IOLs, however, these are low add power lens and near vision may not be sufficient. In a study using high speed OCT that we developed; we confirmed that what could add some physical force to IOLs is the iris and ciliary muscle. This means that the most ideal lens to correct presbyopia is accommodative IOLs that utilize actions of iris and ciliary muscles and their fluid changing shape. In addition, fixation of IOL needs to be changed from in the bag fixation, which is currently a main stream, to out of the bag fixation. In our opinion, out of the bag fixation is not very bad, and on the contrary, it may even solve various issues of IOLs, such as posterior capsular opacification and dysphotopsia.
References
- Ito M, Shimizu K, Kawamorita T, Ishikawa H, Sunaga K, Komatsu M. Association between ocular dominance and refractive asymmetry. J Refract Surg. 2013;29(10):716-20.
- Ito M, Shimizu K. Pseudophakic monovision. CRST Europe. 2009;4:64-6.
- Ito M, Shimizu K, Iida Y, Amano R. Five-year clinical study of patients with pseudophakic monovision. J Cataract Refract Surg. 2012;38(8):1440-5.
- Kawamorita T, Uozato H, Handa T, Ito M, Shimizu K. Effect of pupil size on visual acuity in a laboratory model of pseudophakic monovision. J Refract Surg. 2010;26(5):378-80.
- Iida Y, Shimizu K, Ito M. Pseudophakic monovision using monofocal and multifocal intraocular lenses: hybrid monovision. J Cataract Refract Surg. 2011;37(11):2001-5.