Research Article
Is Peroral Endoscopic Myotomy for Achalasia Safe in a Small-Volume Center?
Rushfeldt C1*, Nordbø M1 and Goll R2
1Deptartment of Gastrointestinal Surgery, University Hospital of North Norway, Norway
2Deptartment of Gastrointestinal Medicine, University Hospital of North Norway, Norway
*Corresponding author: Christian Rushfeldt, Department of Gastrointestinal Surgery, Division of Surgery, Oncology and Women’s Health, University Hospital of North Norway, 9038 Tromsø, Norway
Published: 20 Jun, 2018
Cite this article as: Rushfeldt C, Nordbø M, Goll R. Is
Peroral Endoscopic Myotomy for
Achalasia Safe in a Small-Volume
Center?. Clin Surg. 2018; 3: 1993.
Abstract
Background and Aims: Peroral endoscopic myotomy (POEM) is a minimally invasive procedure
for the surgical treatment of achalasia and an endoscopic alternative to open or laparoscopic Heller
myotomy (HM). POEM was initially developed in Japan, was first published in 2010, and has since
been increasingly adopted in Western countries. The aim of this study is to present preliminary data
from the introductory phase of POEM in a small-volume center.
Material and Methods: The first 14 patients operated with POEM for achalasia at the University
Hospital of North Norway were registered in a prospective database and retrospectively evaluated,
as a quality assurance study. Indications for the procedures were manometric diagnosis of achalasia
and a significant Eckardt symptom score (≥ 7 points).
Results: A total of fourteen patients, 6 female, median age 47 years (19-77 years), were operated in a
day care unit and observed in the hospital ward for a median of 1 day (1-17 days). The preoperative
and three month postoperative follow-up median Eckardt symptom scores were 8 (7-12) and 0 (0-
9), respectively. One complication was encountered, which resulted in an intraoperative mucosal
perforation, and was subsequently treated with an endoscopically implanted stent. Four patients
reported acquiring occasional gastro esophageal reflux disease (GERD), which did not necessitate
regular antacid medication.
Conclusion: Preliminary results from the introductory phase of POEM for achalasia in a small
volume center demonstrate that the procedure was performed safely and with satisfactory short
term results.
Keywords: Per oral endoscopic myotomy; POEM; Achalasia
Introduction
Achalasia is a severe neuro-inflammatory disease of the esophagus causing dysfunction of
the esophagus that, if not treated, results in weight loss and malnutrition [1]. A disturbance or
weakening of the esophageal peristalsis combined with a lack of relaxation of the Lower Esophageal
Sphincter (LES) when swallowing causes dysphagia with chest pain and regurgitation as concurrent
symptoms. The condition is commonly misdiagnosed as GERD [2].
Traditional treatments of achalasia include botulinum toxin injection to relax the LES, PBD
(pneumatic balloon dilation) to stretch the circular muscle fibers and finally surgical division
(myotomy) of the LES in order to assist the passage of food and liquid into the stomach. Botulinum
toxin injection and PBD are considered to give only temporary symptomatic relief, whereas
myotomy results in a permanent solution for most patients [3].
Until quite recently an open or laparoscopic HM was the only surgical procedure in the
treatment of achalasia. Fundoplication most often accompanies HM in order to prevent GERD
after opening of the gastroesophageal junction (GE-junction) [4]. In 2010, the Japanese doctor
Inoue H et al. published a new and revolutionary method for dividing the LES by an endoscopic
technique based on a series of 17 patients [5]. This procedure quickly grew in popularity and became
widespread in the course of few years because of its minimally invasive nature [6,7]. Inoue’s novel
endoscopic procedure spares patients open or laparoscopic surgery and has minimal impact on
the patient, entailing only a small incision in the mucosa and myotomy of the circular muscle layer
including the LES. It is debated whether there is more reflux following POEM than HM combined
with fundoplication but this question is not yet fully answered.
The relatively small population of 0.5 million people in the region
served by the University Hospital of North Norway, combined with
a low incidence of achalasia ranging from 1-2/100.000 implies few
cases per year [8]. In a small volume center it is crucial to demonstrate
a sufficient level of quality and safety in order to provide a given
surgical procedure.
Table 1
Figure 1
Figure 1
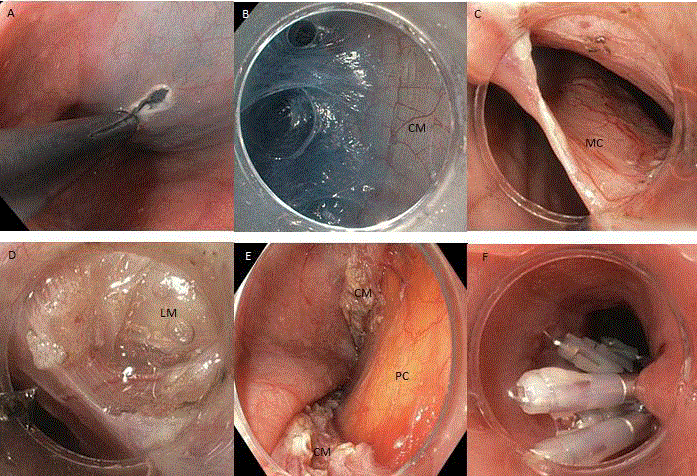
A) Primary mucosal incision, B) developing the submucosal tunnell
with inner circular muscle (CM) to the right, C) tunnellentrance with mucosa
(MC) flap, D) outer longitudinal muscle (LM) exposed after myotomy of the
circular muscle, E) pericard (PC) is visible after spontaneous cleavage of
longitudinal muscle layer, F) clip-suturing of primary mucosa inscision.
Methods
From June 2016 to February 2018, 14 patients with achalasia were
operated with POEM at the University Hospital of North-Norway
and prospectively registered in a database, which was analyzed
retrospectively. The selection of patients suitable for POEM was
based on a clinical scoring system for achalasia (Eckardt score) [9],
esophageal High Resolution Manometry (HRM) according to the
Chicago classification [10], gastroscopy-findings and an esophageal
X-ray after oral ingestion of barium contrast. Patients with an Eckardt
score of ≥ 7 out of a maximum of 12 points and manometric findings
consistent with achalasia were selected for POEM if gastroscopy
and barium esophagography excluded other esophageal diseases.
Patients received written and oral information regarding the
procedure with an emphasis on potential complications and the
risk of GERD following the division of the LES. The evaluation of
the implementation of POEM, as a procedure already in use in many
other countries, is categorized as a quality assurance project with
no requirement for disclosure or consent according to the rules of
the Norwegian ethical committee. Due to its recent introduction as
a surgical operative technique, POEM is registered in the National
Norwegian database for evaluation of new methods in hospitals at
The Norwegian Institute of Public Health.
All patients were operated in a day care unit under general
anesthesia. Patients received prophylactic antibiotics intravenously as
well as Proton Pump Inhibitor (PPI) intraoperative. The esophagus
was washed with an antiseptic chlorhexidine solution 1 mg/ml
(Fresenius Kabi, Halden, Norway). The operations were conducted
with a gastro scope (Olympus GIF-HQ190, Olympus, Hamburg,
Germany) with an oval, transparent cap on the tip (Fujifilm DH-
29CR, Tokyo, Japan) and with CO2 gas for insufflation. An Erbe VIO
300 (ErbeElectromedicin GmbH, Tübingen, Germany) was used for
diathermy. The POEM procedure used, as initially described by Inoue
[5], is outlined below.
A submucosal bubble was first created by injecting a solution of
saline with 2% Indigo Carmine (Amino AG, Gebenstorf, Switzerland)
approximately 14 cm cranial to the GE-junction between the 1 and
3 o’clock position using an endoscopic needle (Needle master NM-
610U-0426, Olympus). A 2 cm longitudinal incision was made in
the lifted mucosa (Figure 1A) with a Triangle Tip knife (KD645-L,
Olympus). This mucosal incision was used to create a 15 cm sub
mucosal tunnel, which exposed the circular muscle layer. The sub
mucosal tunnel was extended caudally and ended 3 cm caudal to
the GE-junction (Figure 1B and 1C). The tunnel was washed with a
gentamicin solution 80 mg/20 ml NaCl (Sanofi-Aventis, Paris, France).
A 13 cm myotomy of the circular muscle was then performed. This
myotomy, which included the LES, was made in a caudal direction
from 2 cm below the lower edge of the mucosal incision to 3 cm below
the GE-junction (Figure 1D and 1E). Finally the mucosal incision was
closed with small clips (N1085930, Olympus) (Figure 1F). Free gas
in the abdomen was drained intra operatively with a left sub costal
venflon if needed.
Patients were allowed to drink water immediately following
the operation and received analgesics as required. Patients stayed
overnight in the ward and were discharged on the first postoperative
day if the clinical condition was satisfactory. No routine X-ray was
performed before discharge. They were allowed liquid nutrition
from day one with a gradual transition to solid food during the first
week. Patients were given an extended antibiotic prophylaxis for five
days (doxycycline 100 mg ×1, metronidazole 400 mg × 3) and PPI
(pantoprazole 40 mg × 1) for one month.
A follow-up telephone interview was performed after three
months with an Eckardt symptom score. In addition, patients were
asked if they experienced symptoms of GERD and if they still required
the use of PPI medication.
Results
In all, 14 patients, 6 female and 8 male, were included in the study.
All patients with achalasia referred to The University Hospital of
North-Norway during the study period fulfilled the criteria for POEM
operation with a significant Eckardt score (≥ 7) and a diagnostic
manometry. Patient and procedural data are listed in Table 1. Median
age 47 years (19-77 years). Type II achalasia was most frequent with
11 patients, followed by type I and type III with two and one patients,
respectively. Median integrated relaxation LES pressure (IRP4s) was
38 38 mmHg (26-68 mmHg). Five patients had previously been treated
with 1 to 3 PBDs and one patient with botulinum toxin injection in
the LES. A barium esophagography was diagnostic for achalasia in 12
of the 14 patients. Median procedure time in the operating theatre
was 167 mins (110-219 mins) with the shortest procedure being the
last. Four of the first seven patients required intra operative drainage
of free gas from the abdomen. The median number of nights in the
ward after POEM was 1 day (1-17 days).
One patient presented with severe submucosal fibrosis around the
LES (Figure 2), did not profit from the POEM, and was admitted for a
total of 17 days. This patient had suffered weight loss due to achalasia
and was therefore admitted to receive intravenous nutrition therapy
after the failed POEM procedure. This fibrotic LES was later treated
with several PBDs and stented with no permanent symptomatic relief.
After a second POEM, still without effect, an intraluminal endoscopic
incision through the hard fibrotic stricture was undertaken, and the
patient was finally able to eat slowly.
The blood test C-reactive protein (CRP) was slightly elevated to a
median value of 37 mg/l when measured the day after the operation,
but with a great variation (5-73 mg/L). One complication occurred,
which was treated endoscopically. A 2 mm hole in the mucosa resulted
from application of diathermia to cauterize a bleeding artery in the
mucosa at the GE-junction (Figure 3A). Ligation with intraluminal
clips proved to be insufficient, due to the defect’s difficult position,
and therefore a covered stent was inserted when free intra-abdominal
gas under the right hemi diaphragm presented on x-ray the day after
the procedure (Figure 3B and 3C). The stent proved patent upon
barium X-ray (Figure 3C).
Patients were scored for achalasia symptoms with the Eckardt
score before and three months after the operation with the exception
of the last patient operated, who was scored just under two months
postoperatively. Median preoperative Eckardt score was 8 (7-12)
while median postoperative score was 0 (0-9). Four patients reported
mild and occasional GERD symptoms and two of these used PPI
medication occasionally.
Figure 2
Figure 2
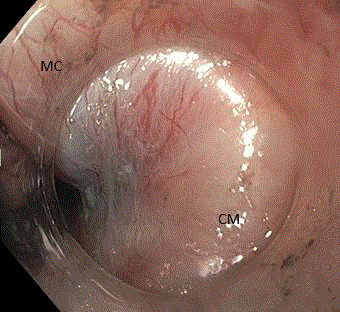
Severe submucosal fibrosis in the LES with no visible or dissectible
layer between the mucosa (MC) and the circular muscle (CM).
Figure 3A
Figure 3B
Figure 3C
Figure 3C
X-ray of the esophagus with barium contrast showed noleak after
stenting. The stent is fixed with two clips to prevent migration.
Discussion
This study reports a satisfactory level of treatment effect and
safety following the introduction of a new endoscopic technique for
the treatment of achalasia, which will replace the laparoscopic HM
in our department. A meta-analysis of four nonrandomized studies
comparing laparoscopic HM with POEM demonstrated lower
Eckardt symptom score after surgery in the POEM group and no
difference in the rate of complication or length of hospital admission
[11]. Thus far there is no meta-analysis reporting an inferior outcome
of POEM compared to HM [6,7,11-13].
Studies comparing post-procedural GERD in POEM vs.
laparoscopic HM show that patients undergoing POEM were more
likely to develop GERD symptoms in some meta-analysis [6,12,13]
while in another meta-analysis no difference in symptomatic GERD
was found [7]. In this study four patients (27%) reported occasional
and mild GERD with no need for regular PPI-medication. Due to
great variability regarding post-POEM GERD in different studies
[7], a 2-year follow-up study of patients operated with POEM at the
University Hospital of North-Norway is planned in order to elucidate
the risk of developing GERD following POEM with greater certainty.
HRM is the gold standard for providing the diagnosis of achalasia.
Elevated resting pressure in the LES is found in all three subtypes of
achalasia. Specific deviations from normal peristalsis determines
subtypes I - III. In subtype III, characterized by spastic esophageal
contractions, the myotomy may be extended in the oral direction if
needed to include proximal spastic parts of the esophagus [14]. Types
I and II are treated with the standard length myotomy. In this study
the only patient diagnosed with type III achalasia did not need an
extended myotomy to be cured. In addition to patients with achalasia,
POEM was applied to treat a patient with a related diagnosis of severe
esophageal gastric junction outlet obstruction, but was not included
in this study. Barium contrast X-ray of the esophagus is not a sensitive
test for achalasia and is reported to be diagnostic in about two thirds
of achalasia patients [15]. In this study 86% obtained a positive
esophagram.
The operative technique used was essentially in accordance
with the original method described [5], except that the length of the
myotomy above the GE-juction was somewhat longer in this study.
The longitudinal muscle layer was found to divide itself after making
a thorough myotomy of the circular muscle layer. Intraoperative
hemorrhages occurred mainly in the muscle layer of the cardia and
was avoided by coagulation prior to incision. Free CO2 gas in the
abdomen was detected and intraoperatively drained with a venflon
inserted below the left costal arch in four of the first seven patients.
Also, subcutaneous emphysema of the upper chest and throat was
detected in the first half of the patients, suggesting a decreased use of
insufflation gas with increasing experience.
Five of the study patients were previously treated with PBD and
one with botulinum toxin injection in the LES. These procedures
resulted in temporary symptom relief as shown in other studies
[16,17]. In this study, the POEM procedure was the primary treatment
if Eckardt score was significantly elevated and manometric findings
were diagnostic for achalasia. It is debated whether botulinum
toxin injections and/or PBD lead to submucosal fibrosis in the LES,
reducing or preventing the circumferential relaxation of the LES after
myotomy. One patient presented with severe sub mucosal fibrosis
with no prior achalasia treatment (Figure 2). This patient did not
receive symptomatic relief following POEM. In a review of 1693
patients operated with POEM, 0.77% procedures were aborted and of
these 92.3% were due to severe sub mucosal fibrosis [18].
In an international multicenter case control study the prevalence
of adverse events with POEM was 7.5% of which 0.5% was severe
[19]. Mucosal perforations occurred at a rate of 2.8%. In this sample
one inadvertent mucosal perforation occurred. This perforation was
first repaired with intraoperative endoscopic clipping, which proved
insufficient, and thereafter definitively with a covered stent for two
weeks (Figure 3). Despite the POEM procedure’s proximity to vital
structures in the mediastinum, such as the heart (Figure 1), severe
complications are rare [19-21].
The POEM procedure’s efficacy at reducing achalasia symptoms
was striking, with a median Eckardt symptom score of 0 (0-9), three
months postoperatively. This means a majority of the patients (9 out
of 14) had no dysphagia, chest pain, regurgitation or further weight
loss at follow-up. The observation period of three months in this
study is short and recurrences may occur in the long term. However,
the largest long term study after POEM for a series of 500 Japanese
patients shows a median Eckardt score of 1.0 (± 2.0) after two months,
which persisted at the three year follow-up [20]. In a long term study
from the USA including 115 patients a 92% success rate was observed
after 2.4 years [21].
One gastrointestinal surgeon (C.R.) performed all the POEM
procedures after participating in several at Haukeland University
Hospital, Bergen, Norway. The first two procedures at the University
Hospital of Northern Norway were performed under the supervision
of an experienced POEM surgeon - Dr. Bengt Håkansson, Ersta
hospital, Sweden. Some authors suggest that preclinical POEM
procedures should be performed in animal models in order to learn the
procedure [22], however this option was not available. Moreover, the
surgeon C.R has extensive experience from more than 400 endoscopic
mucosal resections and sub mucosal dissections before starting with
POEM [23]. Whereas some endoscopic resections are performed with
the endoscope in difficult angulations, or even inverted, the POEM
procedure is performed with the gastroscope straight forward and
is therefore technically not very difficult. However, even if reported
serious complications are few, the potential for serious complications
is significant and requires that the operator possesses endoscopic
skills from other advanced endoscopic procedures before learning
POEM.
In conclusion POEM in the treatment of achalasia can be
performed safely and with good short term results in a small-volume
center based on a thorough preoperative investigation including
HRM, and performed by an operator experienced in endoscopic
resections and interventions. In this study mild symptomatic post-
POEM GERD was reported in a quarter of the patients. More studies
of long term efficacy and post-POEM GERD are needed.
References
- Goldblum JR, Rice TW, Richter JE. Histopathologic features in esophagomyotomy specimens from patients with achalasia. Gastroenterology. 1996;111(3):648-54.
- Ates F, Vaezi MF. The pathogenesis and management of achalasia: current status and future directions. Gut Liver. 2015;9(4):449-63.
- Pandolfino JE, Gawron AJ. Achalasia: a systematic review. JAMA. 2015;313(18):1841-52.
- Lyass S, Thoman D, Steiner JP, Phillips E. Current status of an antireflux procedure in laparoscopic Heller myotomy. Surg Endosc. 2003;17(4):554-8.
- Inoue H, Minami H, Kobayashi Y, Sato Y, Kaga M, Suzuki M, et al. Peroral endoscopic myotomy (POEM) for esophageal achalasia. Endoscopy. 2010;42(4):265-71.
- Schlottmann F, Luckett DJ, Fine J, Shaheen NJ, Patti MG. Laparoscopic Heller Myotomy Versus Peroral Endoscopic Myotomy (POEM) for Achalasia: A Systematic Review and Meta-analysis. Ann Surg. 2018;267(3):451-60.
- Talukdar R, Inoue H, Reddy DN. Efficacy of peroral endoscopic myotomy (POEM) in the treatment of achalasia: a systematic review and meta-analysis. Surg Endosc. 2015;29(11):3030-46.
- Sadowski DC, Ackah F, Jiang B, Svenson LW. Achalasia: incidence, prevalence and survival. A population-based study. Neurogastroenterol Motil. 2010;22(9):e256-61.
- Eckardt VF. Clinical presentations and complications of achalasia. Gastrointest Endosc Clin N Am. 2001;11(2):281-92.
- Kahrilas PJ, Bredenoord AJ, Fox M, Gyawali CP, Roman S, Smout AJ, et al. The Chicago Classification of esophageal motility disorders, v3.0. Neurogastroenterol Motil. 2015;27(2):160-74.
- zhang y, wang h, Chen X, Liu L, Wang H, Liu B, et al. per-oral endoscopic myotomy versus laparoscopic heller myotomy for achalasia: A meta-analysis of nonrandomized comparative studies. Medicine (Baltimore). 2016;95(6):e2736.
- Marano L, Pallabazzer G, Solito B, Santi S, Pigazzi A, De Luca R, et al. Surgery or peroral esophageal myotomy for achalasia: A systematic review and meta-analysis. Medicine (Baltimore). 2016;95(10):e3001.
- Repici A, Fuccio L, Maselli R, Mazza F, Correale L, Mandolesi D, et al. Gastroesophageal reflux disease after per-oral endoscopic myotomy as compared with Heller's myotomy with fundoplication: a systematic review with meta-analysis. Gastrointest Endosc. Gastrointest Endosc. 2018;87(4):934-943.
- Kumbhari V, Tieu AH, Onimaru M, El Zein MH, Teitelbaum EN, Ujiki MB, et al. Peroral endoscopic myotomy (POEM) vs laparoscopic Heller myotomy (LHM) for the treatment of Type III achalasia in 75 patients: a multicenter comparative study. Endosc Int Open. 2015;3(3):E195-E201.
- Howard PJ, Maher L, Pryde A, Cameron EW, Heading RC. Five year prospective study of the incidence, clinical features, and diagnosis of achalasia in Edinburgh. Gut. 1992;33(8):1011-5.
- Schoenberg MB, Marx S, Kersten JF, Rosch T, Belle S, Kahler G, et al. Laparoscopic Heller myotomy versus endoscopic balloon dilatation for the treatment of achalasia: a network meta-analysis. Ann Surg. 2013;258(6):943-52.
- Leyden JE, Moss AC, MacMathuna P. Endoscopic pneumatic dilation versus botulinum toxin injection in the management of primary achalasia. Cochrane Database Syst Rev. 2014;(12):CD005046.
- Wu QN, Xu XY, Zhang XC, Xu MD, Zhang YQ, Chen WF, et al. Submucosal fibrosis in achalasia patients is a rare cause of aborted peroral endoscopic myotomy procedures. Endoscopy. 2017;49(8):736-44.
- Haito-Chavez Y, Inoue H, Beard KW, Draganov PV, Ujiki M, Rahden BHA, et al. Comprehensive analysis of adverse events associated with per oral endoscopic myotomy in 1826 patients: An International multicenter study. Am J Gastroenterol. 2017;112(8):1267-76.
- Inoue H, Sato H, Ikeda H, Onimaru M, Sato C, Minami H, et al. Per-oral endoscopic myotomy: A series of 500 patients. J Am Coll Surg. 2015;221(2):256-64.
- Hungness ES, Sternbach JM, Teitelbaum EN, Kahrilas PJ, Pandolfino JE, Soper NJ. Per-oral endoscopic myotomy (poem) after the learning curve: durable long-term results with a low complication rate. Ann Surg. 2016;264(3):508-17.
- Hernandez Mondragon OV, Rascon Martinez DM, Munoz Bautista A, Altamirano Castaneda ML, Blanco-Velasco G, Blancas Valencia JM. The Per Oral Endoscopic Myotomy (POEM) technique: how many preclinical procedures are needed to master it? Endosc Int Open. 2015;3(6):E559-E65.
- Rushfeldt C, Aabakken L. Implementation of endoscopic submucosal dissection for gastric lesions in Norway. Scand J Surg. Scand J Surg. 2016;105(2):90-6.