Case Report
Hidden in Plain Sight
Tiffany Jian Ying Lye1, Ye Xin Koh2* and Chung Yip Chan2
1Department of General Surgery, Singapore General Hospital, Singapore
2Department of Hepatopancreatobiliary and Transplant Surgery, Singapore General Hospital, Singapore
*Corresponding author: Koh Ye Xin, Department of Hepatopancreatobiliary and Transplant Surgery, Singapore General Hospital, 169608 Singapore
Published: 20 Jun, 2018
Cite this article as: Lye TJY, Koh YX, Chan CY. Hidden in
Plain Sight. Clin Surg. 2018; 3: 1985.
Abstract
We report a case of Mirrizi’s syndrome with a rare complication of a hepatico-cholecysto fistula, and share our experience and recommendation in its surgical approach in order to achieve safe and successful outcomes.
Introduction
Chronic complications of symptomatic gallstone disease, such as Mirizzi’s Syndrome are rare, with an incidence of less than 1% per year. The implications of this condition are related to its potentially serious surgical complications such as bile duct injury. Patients with Mirizzi’s syndrome constitute a formidable challenge and their surgical treatment is a test to any surgeon’s ability and dexterity. We share our experience of a rare complication of Mirrizi’s syndrome.
Case Presentation
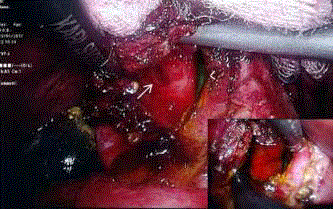
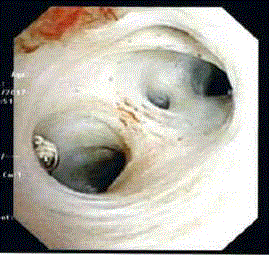
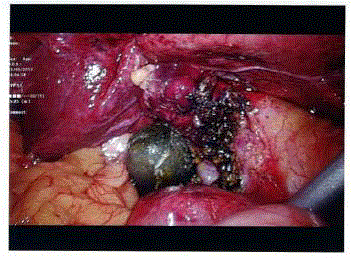
A 62 year old woman was admitted for acute cholangitis and presented with the classic triad of fever, right hypochondrial pain and jaundice. Her liver function tests demonstrated obstructive jaundice with raised serum bilirubin of 132U/L and ALP 545U/L. A Computed Tomography (CT) scan was then requested, which revealed a large 2.5 cm calculus impacted at the Hartmann’s pouch of the gallbladder, resulting in significant upstream biliary dilatation. The gallbladder was contracted with a thickened wall. The patient subsequently underwent an Endoscopic Retrograde Cholangio Pancreato Graphraphy (ERCP). Cholangiogram demonstrated dilated common bile duct and intrahepatic ducts, with narrowing at the common hepatic duct secondary compression from the large impacted gallstone. Endoscopic sphincterotomy and stenting was performed to decompress the biliary system. She was treated and planned for an interval cholecystectomy. At surgery, diagnostic laparoscopy revealed a severely contracted gallbladder with a large gallstone filling the entire gallbladder, and dense adhesions between the gallbladder and duodenum. The gallbladder was incised and the stone extracted. An opening at the gallbladder bed was revealed upon extraction of the large occluding gallstone and the common bile duct stent could also be visualized from within the gallbladder (Figure 1). A choledocho scope was introduced into this opening (Figure 1; bottom right image) and intra-operative choledochoscopy was performed, which confirmed the presence of a fistula between the gallbladder and the intrahepatic bile ducts. Advancement of the choledochoscope demonstrated that the fistula opens into the right posterior hepatic duct (Figure 2). No intra-hepatic ductal calculi were seen. Cholecystoplasty was then performed with interrupted intra-corporeal sutures (Figure 3). Re-apposition of the edges of the incised gallbladder wall was just sufficient to close the biliary tract, leaving little residual space for lithogenesis. The CBD stent was left in situ and there was no evidence of bile leak at the end of the surgery. There were no peri-operative complications and her recovery was uneventful. She was ultimately discharged well from the hospital on the second postoperative day. She was last reviewed 6 months post operation with no recurrent choledocholithiasis or cholangitis.
Figure 1
Figure 2
Figure 3
Discussion
Mirizzi’s syndrome is a rare complication of chronic cholelithiasis occurring in 0.7% to 1.4% of patients with gallstones, and is characterized by impaction of stones in the cystic duct or gallbladder neck. Majority of the cases in the literature describe fistulation between the gallbladder and the extrahepatic bile ducts, and classifications of the disease have been based on the presence of such fistulae and the severity of destruction of the extrahepatic bile duct [1]. However, this is the first reported case of gallbladder stones eroding into an intra-hepatic duct, resulting in a hepatico-cholecysto fistula. In this patient, a large calculus had eroded through the posterior wall of the gallbladder into an aberrant right posterior hepatic duct. The preoperative cholangiogram demonstrated the aberrant duct adjacent to the large gallbladder calculus. The fistula, however, was not apparent as its opening was obstructed by the calculus. In addition, this is an unusual case whereby the patient also has a second fistula (cholecystocholedochal). Mirrizi’s syndrome poses an operative challenge to the surgeon. With a judicious approach during dissection and early recognition of critical anatomy, bile duct injury can be avoided. Good outcomes can be achieved with an appropriate surgical procedure [2]. In patients with severe fibrosis preventing proper visualization of the Calot’s, retrograde subtotal cholecystectomy is the recommended approach and has been shown to be safe with excellent outcomes [3]. However, this case demonstrates the possibility of a hitherto unrecognized complex biliary fistulation. Early cholecystostomy when dealing with large impacted Hartmann’s pouch calculi in this case improved visualization of the gallbladder bed and enabled recognition of this complex fistulation. In this case, this approach enabled appropriate reconstruction of the biliary tract by preserving the gallbladder wall and prevented a potential complication of bile leakage of an unrecognized hepato-cholecysto fistula.
References
- Beltrán MA. Mirizzi syndrome: History, current knowledge and proposal of a simplified classification. World J Gastroenterol. 2012;18(34):4639-50.
- Chan CY, Liau KH, Ho CK, Chew SP. Mirizzi syndrome: a diagnostic and operative challenge. Surgeon. 2003;1(5):273-8.
- Shah OJ, Dar MA, Wani MA, Wani NA. Management of Mirizzi syndrome: a new surgical approach. ANZ J Surg. 2001;71(7):423-7.