Case Report
Didelphys Uterus and Cervical Cancer: A Case Report and Review of Literature
Victor E Valdespino1*, Hilda Mendoza Ramon2, German Maytorena Cordova1, Victor Valdespino Gomez3, Paola Ferrer Torres4 and Pedro Blas Hernandez4
1Department of Oncology Gynecology Service, Gynecology- Obstetrician Hospital 4 "Luis Castelazo Ayala", Mexican Institute Social Service, Mexico
2Department of Pathology, Gynecology- obstetrician Hospital 4 "Luis Castelazo Ayala", Mexican Institute Social Service, Mexico
3Oncology Surgen, Gynecology- Obstetrician Hospital 4 "Luis Castelazo Ayala", Mexican Institute Social Service, Mexico
4Oncology Gynecology, Gynecology- Obstetrician Hospital 4 "Luis Castelazo Ayala", Mexican Institute Social Service, Mexico
*Corresponding author: Victor E Valdespino, Department of Oncology Gynecology Service, Gynecology- Obstetrician Hospital 4 "Luis Castelazo Ayala", Mexican Institute Social Service, Mexico
Published: 30 Apr, 2018
Cite this article as: Valdespino VE, Ramon HM, Cordova
GM, Gomez VV, Torres PF, Hernandez
PB. Didelphys Uterus and Cervical
Cancer: A Case Report and Review of
Literature. Clin Surg. 2018; 3: 1964.
Abstract
Congenital malformations of the female genital tract are defined as deviations from normal anatomy
resulting from embryological maldevelopment of the Müllerian system or paramesonephric ducts.
This condition represents a rather common benign condition with a prevalence of 4% to 7%.
Cervical cancer and didelphys uterus is an infrequent condition in clinical practice. Association
between cervical cancer and Müllerian malformation is limited to medical references. We present
a surgical treatment with a result IB1, with systematic pelvic and paraaortic nodal dissection, with
poor prognostic factors, she is chemoradiotherapy treatment. She is a patient 55 years old, with no
symptoms in young adulthood or teenager in relation to didelphys uterus.
Always it is possible we encourage the primary surgical treatment, we can get prognostic factors
and is possible scan other congenital malformation, also the point A is not constant for planned a
radiotherapy treatment finally lymphatic channels in anatomical distortion could be evaluated and
measure the nodal affection, and improve and personalize radiotherapy treatment. This case is an
absolutely infrequent in the clinical practice.
Introduction
Cervical cancer is typically preventable if pre-cancerous lesions are detected and treated early.
Cervical cancer screening by means of cytology, or the Papanicolaou smear, seeks to detect
precancerous or cancerous cervical lesions prior to symptom onset. Research has consistently
observed that cervical cytology screening is highly efficacious against invasive cervical cancer
incidence and death among women of reproductive age [1]. Therefore, regular cervical cancer
screening and follow-up are critical. Cytological screening will most likely decline in favor of HPVbased
screening because of its superiority over cytology in the 2 characteristics that influence test
efficacy ; HPV DNA testing can detect invasive cervical cancer risk for a longer period than cytology
[2,3], and its sensitivity is an absolute 40% higher than that of cytology [4,5]. Thus, the relationship
between these screening modalities’ efficacies is knowable-the efficacy of HPV-based screening
is expected to exceed that of cytology, all things being equal. Analysis of extant data on cytology
screening, therefore, may offer a minimum estimate of HPV-based screening efficacy among older
women. However, screening by cytology alone remains acceptable under all current guidelines,
and Papanicolaou smears continue to be widely used. Further, a study to evaluate the efficacy of
HPV DNA testing among women will not be possible for years after an HPV DNA–based screening
program is implemented until a sufficient number of deaths have occurred to make meaningful
comparisons on the basis of prior HPV DNA screening history [6,7]. Mullerian duct anomalies are
congenital defects of the female genital system that arise from abnormal embryological development
of the Mullerian ducts. These abnormalities can include failure of development, fusion, canalization,
or reabsorption, which normally occurs between 6 and 22 weeks in utero. Most sources estimate an
incidence of these abnormalities to be from 0.5% to 5.0% in the general population [8,9]. Septate
uterus is the commonest uterine anomaly with a mean incidence of ~35% followed by bicornuate
uterus (25%) and arcuate uterus (20%) [9].
Unicornuate and didelphys uterus have term delivery rates
of ~45%, and the pregnancy outcome of patients with untreated
bicornuate and septate uterus is also poor with term delivery rates of
only ~40% [9].
Most women with a didelphys uterus are asymptomatic, but
some present with dyspareunia or dysmenorrhea in the presence
of a varying degree of longitudinal vaginal septum. Rarely, genital
neoplasm's, hematocolpos hematometrocolpos, and renal anomalies
are reported in association with didelphys uterus. Despite some of
these complications, there are many cases of women with a didelphys
uterus that did not exhibit any reproductive or gestational challenges.
The VCUAM classification (Vagina, Cervix, Uterus Adnex
Associated Malformation) is anatomical. Organs are classified as
separated similar to TNM classification, (Tumor, Nodal, Metastases).
This manner allows a categorization, is precise, detail, and very
representative. Different anatomical anomalies could be described
and the practitioner has a good idea of each organ is affected in a
single manner [10].
Lee reports a case of a congenital abnormality of uterus didelphys
in a patient who developed invasive carcinoma of the cervix. The
patient received radical radiotherapy by a combination of external
beam pelvic radiotherapy and high dose rate brachytherapy by
insertion of afterloading catheters into both uterine canals. A newly
defined prescription point was used midway between the two
catheters and 2 cm above the mean cervical os position. The classical
point A was regarded as inappropriate in this patient with a rare
condition. Acute toxicity was minor and the patient is tumor free
with no significant normal tissue late effects after follow-up of nearly
3 years.
Depends on main cervical tumor is localized, the classical point A,
could change, in position, in consequence, the radiotherapy treatment
should be personalized and very precise for a better response on the
tumor [11].
In addition, we can consider cervical cancer in a patient with
Mullerian anomalies, we must offer the best treatment option, it
is possible to get the nodal status, by lymphadenectomy or radical
surgery by laparoscopic surgery or traditional surgery, when the stage
allow it, or chemoradiotherapy.
When the cervical cancer is treated with surgery, we choose
a specific surgery with a Quelow - Morrow hysterectomy, the
patient does not need more morbidity with a greatest surgery, in
our clinical practice when we performed a cervical surgery control,
we always practice standing nodal affection pelvic and paraaortic
lymphadenectomy, and we can get specific information about the
nodal tumoral invasion, it is necessary specific adjuvant treatment.
Figure 1
Figure 2
Case Presentation
The present case is a women 55 years old, with hypertension 12
years of history, cholecystectomy on 32 years old, no more familiar
background, gynecological antecedent menarche 12 years old, 28 ×
5 days, 5 pregnancies, 1 abortion, 1 labour, 3 caesarean, menopause
50 year old. In a yearly control cervicovaginal cytology reported an
epithelial neoplasia grade II, in the medical first level unit, the patient
was sent to Colposcopy in a third level medical unit, in this evaluation
(colposcopy) they notice two cervices, one of them with cervical
cancer (right) and left cervix without tumoral damage. A curettage
endocervical was performed in both cervix, epidermoid (squamous)
invasive cancer was reported on the right cervix, endocervical glands
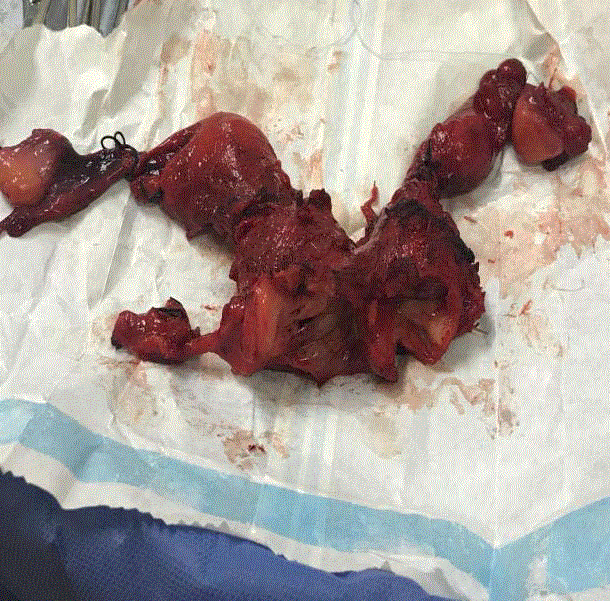
without alterations on the left cervix (Figure 1). Colposcopy service,
operate a conization on right cervix with definitive report squamous
cell carcinoma measure 0.8 cm × 0.5 cm margin was positive an
invasive tumor. An ultrasound was made, cervix reported 32 mm
× 26 mm × 30 mm no tumor was obvious, uterine corpus 46 mm
× 48 mm × 20 mm and we performed a hysterectomy Querlow -
Morrow B2 on right side and Querlow - Morrow A on left side, we
carry on a systematic lymphadenectomy pelvic and paraaortic with
17 nodes without tumor in pelvis and 24 nodes without metastases
in retroperitoneal area [12]. The final tumoral measure was 27
mm, tumoral get involvement all right cervix, with lymph-vascular
infiltration, and tumor comprises lower uterine segment. Surgical
stage final was IB1 epidermoid cervical right cancer. The left cervix
does not expose a tumoral injury, including no cervical dysplasia. At
the moment of transoperative, we found a double uterine body, in a
relationship with double cervix we achievement, a didelphys uterus
and cervical cancer (Figure 2). The patient suffers a ureteral leak,
it was resolved with a catheter JJ, she was sent to radiotherapy and
chemotherapy, she is on concomitant treatment right now with good
tolerance.
In the current clinical practice, this association between uterus
didelphys and cancer are very rare, we performed a surgery a
Querlow-Morrow B2 in right side and a Querlow - Morrow A in
the left side also pelvic and paraaortic lymphadenectomy [12]. As
Chiappa and coworkers, we improve our clinical point of view with
a cervical ultrasound this value measure, is extraordinarily helpful
because improve our clinical diagnosis, and we performed this as
a routine in our service when a patient will be programmed for a
surgery or chemoradiotherapy by cervical cancer [13].
In addition cervical cancer in a didelphys uterus is absolutely
infrequent even in historical technical literature do not is mentioned
change performing a hysterectomy, just is refer briefly to get free
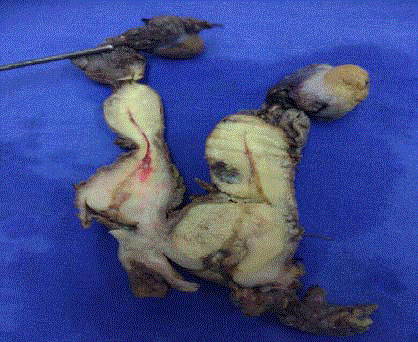
neoplastic margin [14]. Cervical uterine cancer in the right cervix,
with the scar of the cone, and parametrial resection. Atrophied
uterine corpus left, cervix and vagina without tumor. This photo is
sagittal cut-off, we can notice an atrophic uterus and cervix on the left
and cervical cancer in almost all cervix (right image) and parametrial
resection.
Discussion
Rarely, cervical cancer and endometrial carcinoma are reported
in association with cases of didelphys uterus [15,16]. Most women
with a didelphys uterus are asymptomatic but may present with
dyspareunia or dysmenorrhea in the presence of a thick, sometimes
obstructing vaginal septum. This obstructing vaginal septum can lead
to hematocolpos/hematometrocolpos and thus present as chronic
abdominal pain as well or some problems if the patient desire a
pregnant. In the present report, the patient has no acknowledgment
about didelphys uterus because she has no problems at reproductive
age and develops 4 pregnancies with successful evolution. Previously
at his childhood and teenager, she does not refer chronic pelvic pain
or sexual discomfort in early adulthood. This does not agree with
medical reports.
It is generally accepted that having a uterine anomaly is associated
with poorer pregnancy outcomes such as increased chances of
spontaneous abortion, premature labor, cesarean delivery due to
breech presentation, and decreased live births, compared to a normal
uterus. However in the present report could get 4 pregnant, with 1
labours delivery and 3 cesarean [8].
The modalities for correct diagnosis frequently used include highly
invasive methods such as hysteroscopy, hysterosalpingography, and
laparoscopy/laparotomy, also ultrasound. 3D ultrasound is becoming
more commonly used for diagnosis as it is not only noninvasive,
this analytic tool gives all the information needed for morphological
classification [10,17]. Magnetic resonance imaging is also just as
accurate and valuable in diagnosing müllerian abnormalities, as
hysterosalpingograms, hysteroscopy, and laparoscopy are, even more
so as it is noninvasive and can diagnose associated urinary tract
abnormalities at the same time [13]. Nonetheless, it is still difficult to
distinguish between these different anomalies on imaging modalities
due to subjectivity; differences in morphology are often subtle and
changing classification systems [17].
In opposition to the medical reports, this patient was diagnosed
until medical assistance on cancer standing; colposcopy and
ultrasonography evaluation [18].
Other malignant tumors have been reported in Mullerian
anomalies, as Iavazzo, reported a case on didelphys uterus an uterine
carcinosarcoma [19].
Present case report presents an IB1 cervical cancer with nodal
evaluation pelvic and retroperitoneal negative, why a cervix
develops cervical cancer and others do not develop any malignant
or premalignant injury we cannot answer this question, maybe by
epigenetic changes because the viral exposition was positive on both
cervix.
Sugimori, reported two cases of cervical cancer in uterus
didelphys. One was extensive adenocarcinoma and one was squamous
cell carcinoma in situ [20-22].
Conclusion
If a patient has a Müllerian duct anomalies and cervical cancer, clinical staging can be ambiguous, the natural history may be altered, also common association with renal agenesis, or other anatomical variation. Some treatments which could influence the use of potentially nephrotoxic agents, like cisplatin, then are a part of standard chemoradiotherapy, must be considered at moment on select a therapy. Treatment decision making needs to be precise and personalized, in view of the minimal amount of prior literature on the topic. Applicator placement for intracavitary brachytherapy may be fraught with this patients. Because inability to define a point A in patients with anomalies featuring double cervix and uterus is a challenge. Is very useful the surgical approach because we can get prognostic factors, and real pathology stage and another abnormal anatomical variation could be evident and to be evaluated. That's why always it is possible the patients must be treated with surgery the local (pelvic) disease and lymphatic nodes and retroperitoneal, because no available literature to describe the lymphatics of the various Müllerian ducts anomalies. In fact, we recommend performing a lymphatic node dissection pelvic and retroperitoneal in stage IIB or advanced, and know the specific node pathological of the disease and improve radiotherapy field treatment. Among patient with cervical cancer who have Mullerian anomalies, radical surgery should be selected over radiotherapy in the early operable stages. Surgery provides a real stage for nodal metastases pelvic and retroperitoneal, and personalities treatment could be given with more success and less morbidity. When the surgery is not indicated concurrent chemoradiotherapy with image guidance must be used.
References
- Rustagi AS, Kamineni A, Sheila Weinmann S, Reed SD, Newcomb P, Weiss SD. Cervical screening and cervical cancer death among older women: a population-based, case-control study. Am J Epidemiol. 2014;179(9):1107-14.
- Schiffman M, Wheeler CM, Castle PE; Atypical Squamous Cells of Undetermined Significance/Low-Grade Squamous Intraepithelial Lesion Triage Study Group. Human papillomavirus DNA remains detectable longer than related cervical cytologic abnormalities. J Infect Dis. 2002;186(8):1169-72.
- Khan MJ, Castle PE, Lorincz AT,Wacholder S, Sherman M, Scott DR, et al. The elevated 10-year risk of cervical precancer and cancer in women with Human Papilloma Virus (HPV) type 16 or 18 and the possible utility of type-specific HPV testing in clinical practice. J Natl Cancer Inst. 2005 ;97(14):1072-9.
- Mayrand MH, Duarte-Franco E, Rodrigues I, Walter SD, Hanley J, Ferenczy A, et al. Human papillomavirus DNA versus papanicolaou screening tests for cervical cancer. N Engl J Med. 2007;357:1579-88.
- Ronco G, Giorgi-Rossi P, Carozzi F, Confortini , Dalla Palma P, Del Mistro A, et al. Efficacy of human papillomavirus testing for the detection of invasive cervical cancers and cervical intraepithelial neoplasia: a randomised controlled trial. Lancet Oncol. 2010;11(3):249-57.
- Moyer VA. Screening for cervical cancer: U.S. Preventive services task force recommendation statement. Ann Intern Med. 2012;156(12):880-91.
- Saint M, Gildengorin G, Sawaya GF. Current cervical neoplasia screening practices of obstetrician/gynecologists in the US. Am J Obstet Gynecol. 2005;192(2):414-21.
- Heinonen PK. Clinical implications of the didelphic uterus: long-term follow-up of 49 cases. Eur J Obstet Gynecol Reprod Biol. 2000;91(2):183-90.
- Wu TH, Wu TT, Ng YY, Ng SC, Su PH, Chen J, et al. Herlyn-WernerWunderlich syndrome consisting of uterine didelphys, obstructed hemivagina and ipsilateral renal agenesis in a newborn. Pediatr Neonatol. 2012;53(1):68-71.
- Oppelt P, Renner SP, Brucker S, Strissel PL, Strick R, Oppelt PG, et al. The VCUAM (Vagina Cervix Uterus Adnex-associated Malformation) Classification: a new classification for genital malformations. Fertil Steril. 2005;84(5):1493-7.
- Lee CD, Churn M, Haddad N, Davies-Humphries J, Kingston RK, Jones B. Bilateral radical radiotherapy in a patient with uterus didelphys. Br J Radiol. 2000;73(869):553-6.
- Querleu D, Morrow CP. Classification of radical hysterectomy. Lancet Oncol. 2008;9(3):297-303.
- Chiappa V, Di Legge A, Valentini AL, Gui B, Miccò M, Ludovisi M, et al. Agreement of two-dimensional and three-dimensional transvaginal ultrasound with magnetic resonance imaging in assessment of parametrial infiltration in cervical cancer. Ultrasound Obstet Gynecol. 2015;45(4):459- 69.
- Swailes AL, Gockley A, Phaëton R, Kesterson JP. The Wertheim hysterectomy: Development, modifications, and impact in the present day. Gynecol Oncol. 2017;145(1):3-8.
- Heinonen PK. Uterus didelphys: a report of 26 cases. Eur J Obstet Gynecol Reprod Biol. 1984;17(5):345-50.
- Gao J, Zhang J, Tian W, Teng F, Zhang H, Zhang X, et al. Endometrial cancer with congenital uterine anomalies: 3 case reports and a literature review. Cancer Biol Ther. 2017;18(3):123-31.
- Grimbizis GF, Gordts S, Di Spiezio Sardo A, Brucker S, De Angelis C, Gergolet M, et al. The ESHRE/ESGE consensus on the classification of female genital tract congenital anomalies. Hum Reprod. 2013;28(8):2032-44
- Rezai S, Bisram P, Lora Alcantara I, Upadhyay R, Lara C, Elmadjian M. Case Report. Didelphys Uterus: A Case Report and Review of the Literature. Case Rep Obstet Gynecol. 2015;2015:5.
- Iavazzo C, Kokka F, Sahdev A, Singh N, Reynolds K. Uterine carcinosarcoma in a patient with didelphys uterus. Case Rep Obstet Gynecol. 2013;2013:401962.
- Sugimori H, Hachisuga T, Nakamura S, Matsuo N, Nakamura G. Cervical cancers in uterus didelphys. Gynecol Oncol. 1990;36(3):439-43.
- Rastogi M, Revannasiddaiah S, Thakur P, Thakur P, Gupta M, Gupta MK, et al. Müllerian duct anomalies and their effect on the radiotherapeutic management of cervical cancer. Chin J Cancer. 2013;32(8):434-40.
- NCCN Clinical Practice Guidelines in Oncology Cervical Cancer Version 1. 2018 --- October 25, 2017.