Research Article
Exploring the Role of Sildenafil in Acute Pulmonary Embolism
Hall H*, Orton C, Mirza R, Shaw E, Ryan K and Madden BP
*Corresponding author: Helen Hall, Department of Cardiothoracic Medicine, St George’s Hospital, Blackshaw Road, Tooting, London SW17 0QT, UK
Published: 30 Apr, 2018
Cite this article as: Hall H, Orton C, Mirza R, Shaw E,
Ryan K, Madden BP. Exploring the
Role of Sildenafil in Acute Pulmonary
Embolism. Clin Surg. 2018; 3: 1963.
Abstract
Acute pulmonary embolism is a cause of significant morbidity and mortality. If thrombus burden is
sufficient as to cause right ventricular strain, even “intermediate-high risk”, normotensive patients
have a 13% risk of death at 3 months. Current trials do not support thrombolysis in this group due
to excess risk of bleeding. Novel strategies to support the haemodynamic response to acute PE may
be advantageous.
We report our experiences of using Sildenafil in high or intermediate-high risk PE. 18 patients took
Sildenafil 25 mg thrice daily for >3 months. A further patient received 12.5 mg thrice daily with
dose reduction due to side effects. Despite markers of poor prognosis at presentation, all patients
survived to 3 months. 7 received systemic thrombolysis, but none required invasive ventilation or
advanced haemodynamic support. Now at median 9 months follow up, 2 cases of CTEPH have been
confirmed. There have been no deaths directly attributable to thromboembolic disease.
Our findings demonstrate Sildenafil to be a safe, generally well-tolerated adjunct to standard
treatment in this group. Larger controlled trials are now required to better ascertain the role of
Sildenafil in this context.
Introduction
Acute Pulmonary Embolism (PE) is well recognized as a cause of significant morbidity and
mortality. Features including Pulmonary Embolism Severity Index (PESI) score, markers of right
ventricular strain and systemic hypotension are relied upon to identify patients at highest risk of
adverse outcomes [1,2]. Systemic anticoagulation is the mainstay of treatment, with thrombolysis
reserved for those with haemodynamic compromise (“high risk” PE) [1]. However even in the
absence of systemic hypotension, the presence of Right Heart Strain (RHS) doubles the risk of
mortality at 30 days (13% to 17%) and confers a higher risk of Chronic Thromboembolic Pulmonary
Hypertension (CTEPH) [3-5].
Existing trials find that the benefits of thrombolysis in this “intermediate-high risk” group are
offset by the increased risk of haemorrhage [6,7]. Catheter-directed thrombolysis strategies are
under ongoing evaluation, but require access to specialist interventional facilities. Novel, readily
available treatments that aim to alleviate RHS without increasing bleeding risk may therefore be
advantageous.
Sildenafil is a widely available and well-tolerated pulmonary vasodilator, with an established
role in primary Pulmonary Arterial Hypertension (PAH) and evidence of benefit in CTEPH [8-11].
Experimental models of acute PE have demonstrated Sildenafil to be effective in reducing both PVR
and mean Pulmonary Artery Pressure (mPAP) [12-14]. This is further supported by case reports of
Sildenafil administration improving haemodynamics in severely compromised patients with acute
PE [15-17].
We report our experiences of using Sildenafil as an adjunct to standard therapy in 20 patients
with either high or intermediate-high risk acute PE, the majority receiving 25 mg thrice daily for
a minimum of three months. We review clinical features, evidence of RHS and outcomes both at
presentation and at 3 months follow up.
Methods
Patients with high or intermediate-high risk PE were referred to the pulmonary hypertension
team from our emergency department or admitting specialty team. Emergency care had typically
been provided at the time of referral, including diagnostic imaging and initiation of anticoagulation
therapy.
All patients were assessed for clinical and radiological evidence of
RHS. Salient features on 2D Transthoracic Echocardiography (TTE)
or CT Pulmonary Angiogram (CTPA) are listed in Table 1. Cardiac
biomarkers were measured, with Troponin T (TnT) >14 pg/ml and
N Terminal pro-B type natriuretic protein (NT Pro-BNP) >600 pg/
ml deemed significant in the absence of an alternative explanation.
Patients with evidence of RHS on TTE, CTPA or biochemistry,
with or without systemic hypotension, were verbally consented to
receive Sildenafil 25 mg tds in addition to usual care. Patients were
monitored to discharge, and followed up with repeat TTE, CTPA and
clinical evaluation at 3 months.
Table 1
Results
Demographics
Between January 2015 and June 2017, 20 patients received at
least one dose of Sildenafil. 45% (9/20) were male. Mean (± SD)
age at presentation was 54 ± 16 years (range 19-78). Five had active
malignancy, one had COPD, and two had known congestive cardiac
failure. Initial investigations and follow-up TTE results for all patients
are summarized in Table 2.
Initial presentation and management
All patients had clinically significant acute bilateral PE with
a combination of clinical, radiological or biochemical markers of
RHS. All had CTPA performed prior to referral. Bedside TTE was
performed for 4 patients at presentation and performed in a further
15 patients at median day 1 of admission (range 0 - 6).
RHS was evident on TTE in 95% (19/20), on CTPA in 80%
(16/20), with elevated cardiac biomarkers present in 94.7% (18/19).
TnT and NT pro-BNP were measured in 95% (19/20) and 65%
(13/20) respectively. TnT was raised in 94.7% (18/19), median 63 pg/
ml (range 7-800). NT pro-BNP was raised in 76/9% (10/13), median
1505 pg/ml (84-10165).
Five patients had an estimated PASP >60 mmHg, suggestive
of pre-existing Pulmonary Hypertension (PH); however all five
had clinical and radiological features suggestive of large volume
acute PE contributing significantly to this result. One patient (no.
13) self-discharged prior to undergoing TTE or TnT/NT Pro-BNP
measurement, but re-presented and was started on Sildenafil after
TTE and biomarker measurement during her second admission.
A further patient (no. 10) deteriorated 48 hours post CTPA with
presumed clot propagation and RHS on echo, but did not undergo
repeat CT.
Seven patients received systemic thrombolysis with Alteplase;
six were hypotensive at presentation and one deteriorated despite
therapeutic heparinization. Two patients required oxygen delivery
via high flow nasal cannulae. No patients experienced cardiac arrest
and none required invasive ventilation or advanced haemodynamic
support.
All patients were discharged on systemic anticoagulation:
low molecular weight heparin (Dalteparin, n=6), oral coumarins
(Warfarin, n=5) or direct Xa inhibitors (Rivaroxaban, n=9). Choice
was guided by concurrent comorbidities including malignancy,
prior anticoagulation therapy and clinical response to initial agent.
All patients were commenced on Sildenafil 25 mg thrice daily.
One discontinued treatment after one dose due to side effects. The
remaining 19 patients took Sildenafil for a minimum of three months.
Clinical follow up and outcomes
All initial 20 patients were alive at 3 months. After median 9 months
(range 4-28) follow up, two deaths have occurred due to progressive
malignancy, occurring after 10 and 18 months respectively. There
have been no deaths directly attributable to thromboembolic disease.
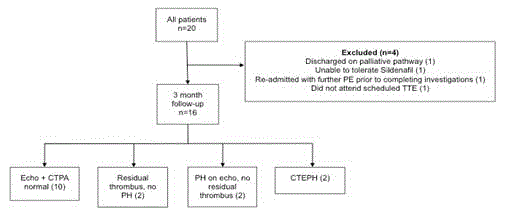
Formal follow-up including CTPA, TTE and clinical assessment
were completed for 16 patients. Two patients were omitted from
ongoing follow up: one had significant neuro disability from
underlying intracranial malignancy and was discharged under a
palliative care pathway, and a second patient had discontinued
Sildenafil after a single dose. Two additional patients failed to
complete all intended investigations. Outcomes are summarized in
Figure 1 and Table 2.
TTE was performed after 96 days (3-483), and CTPA after median
101 days (65-610). 62.5% (10/16) had no evidence of persistent RHS
or residual thrombus. Of the remaining six patients, two have been
diagnosed with CTEPH, two have PH evident on TTE but no residual
thrombus burden, and two have persistent thrombi but without
evidence of ongoing RHS. There was a trend towards higher rates of
recovery in patients who underwent thrombolysis (80%, 4/5 vs. 54.5%,
6/11) but this was not statistically significant. 75% (3/4) of those with
persistent PH, including both those diagnosed with CTEPH, had
initial PASP >60 mmHg suggesting a degree of chronic PH existing
prior to the acute presentation, for which additional investigations
have been performed as indicated.
Adverse events
Two patients developed headaches with Sildenafil; one tolerated
a reduced dose of 12.5 mg tds, the other discontinued treatment after
the first dose. One stopped Sildenafil after 12 months treatment due
to possible ocular complications, but subsequent ophthalmological
review revealed no association. One patient stopped DOAC therapy
prematurely post discharge and was re-admitted with new PE prior to
completing routine follow-up.
Figure 1
Table 2
Discussion
Sildenafil in acute PE
In acute severe PE, occlusion of the pulmonary vascular bed and
release of vasoactive mediators (Thromboxane A2 and serotonin)
contribute to a precipitous rise in pulmonary vascular resistance [12].
The healthy, thin-walled right ventricle is unable to overcome the
sudden increase in after load. Acute RV dilation causes compression
and impaired contractility of the Left Ventricle (LV) and this in
addition to reduced LV filling causes a fall in cardiac output and
haemodynamic decompensation [1]. There is therefore a rationale
for treatments aiming to control the rise in PVR to support the
deleterious effects on the right ventricle, in addition to standard
anticoagulation or fibrinolysis.
Sildenafil is a widely used, orally available pulmonary vasodilator.
It is a selective Phosphodiesterase-5 (PDE-5) inhibitor which
potentiates the effects of cyclic Guanosine Monophosphate (cGMP),
leading to rapid onset of pulmonary vasodilation within 15 min of
administration. It is well established as a first line therapy for Class 1
pulmonary hypertension [8].
Sildenafil appears to be beneficial in established CTEPH, with
small trials demonstrating improvement in PVR, WHO class and 6
min walk test distances [9-11].
In animal models of pulmonary hypertension provoked by acute
PE, intravenous Sildenafil has been found to significantly improve
PVR and mPAP without causing a fall in systemic Mean Arterial
Pressure (MAP) [12-14].
Existing case reports have found administration of Sildenafil to
substantially improve haemodynamics in patients in whom acute PE
has caused severe compromise despite systemic or catheter-directed
thrombolysis [15-17].
Significance and measurement of right ventricular strain
Even in “intermediate-high risk” patients, the presence of RHS is
an independent risk factor for adverse outcomes. A 2014 met analysis
by Cho et al. (n=3283) found a 37.3% prevalence of RV strain in
hemodynamically stable patients with acute PE [4]. Those with RV
strain had an increased short-term mortality rate of 13.7% vs. 6.5%
(OR 2.29; 95% CI 1.61 to 3.26) [5].
Previous studies note the lack of consensus as regards reliable
markers of RHS. The 2014 ESC guidelines find that commonly used
parameters including TTE markers, CTPA and cardiac biomarkers
have reasonably high sensitivity for RHS at 74% to 87% but lack
specificity (35% to 54%) and the positive predictive value for any
one measurement for mortality risk is low at 7% to 9% only. Some
markers also need to be taken in context of the wider clinical picture.
For example, a normal healthy right ventricle is unable to compensate
against very severely elevated PA pressures. An estimated PASP >60
mmHg in the context of a normotensive patient with PE is therefore
highly likely to suggest pre-existing pulmonary hypertension, and
should not be interpreted in isolation as indicative of acute RHS.
Strengths and limitations of our data
We present a case series of patients with acute pulmonary embolus
associated with RHS, in whom the addition of Sildenafil to standard
treatments was well tolerated with few side effects. Outcomes were
generally good with no thrombus-associated deaths seen after median
9 months. Use of Sildenafil in this setting has previously only been
explored in animal studies and isolated case reports. Our findings
should prompt larger, randomised trials to better establish the role of
Sildenafil in this setting.
As with any uncontrolled case series, there are inherent
limitations to the generalisability of these results. Reported cases are
heterogeneous both in terms of pre-existing comorbidities, clinical
severity and use of standard treatments including thrombolysis.
Patients continued under care of the admitting team, and there is
variation in the timing of conversion from parenteral to oral therapy,
initial Sildenafil administration and choice of anticoagulant on
discharge. Five patients had initial results suggesting a degree of preexisting
pulmonary hypertension, which may skew the interpretation
of recovery rates seen at 3 months onwards. Similarly a significant
number of patients received systemic thrombolysis which by design
aims to rapidly improve the haemodynamic response to PE, though
this cohort was too small to comment as to a difference in outcomes
between the two groups.
Right ventricular strain was measured through indirect markers
which, whilst widely relied upon in routine clinical practice, may
lack the sensitivity and accuracy of data obtained invasively via right
heart catheter. CTPA and TTE investigations were interpreted by oncall
radiologists and echocardiogram technicians, and there may be
differences in the interpretation of some of the more subtle markers
of RHS. We recognise that the parameters used may lack specificity,
and accordingly a proportion of patients may have rapidly recovered
with anticoagulation alone. However the markers of RHS used are
widely available to clinicians managing similar patients, and are
reflective of current clinical practice and guidelines.
Conclusion
Sildenafil is a widely used pulmonary vasodilator. It is generally
safe, widely available and well-tolerated. In this group of 20 patients
with acute PE associated with RV strain, Sildenafil was used as
an adjunct to standard anticoagulant therapy. Only one patient
discontinued treatment due to side effects.
Although these patients had features at presentation that
conferred increased risk of death, none required invasive ventilation
or advanced haemodynamic support, and all survived to 3 months.
Follow-up mortality rates remain low, with no deaths attributable
directly to pulmonary embolism. Full recovery was observed in 62.5%
at 3 months. CTEPH has been diagnosed in 2 patients (12.1%) after
median 9 months follow up, though it is likely that both patients had
some degree of pre-existing pulmonary hypertension.
Our experiences support the notion that Sildenafil can be used
safely in this setting. Larger, randomised trials are now required in
order to further elucidate the role of Sildenafil in acute pulmonary
embolism.
References
- Konstantinides SV, Torbicki A, Agnelli G, Danchin N, Fitzmaurice D, Galie N, et al. 2014 ESC Guidelines on the diagnosis and management of acute pulmonary embolism: the task force for the diagnosis and management of acute pulmonary embolism of the European Society of Cardiology (ESC). Eur Heart J. 2014;35(43):3033-73.
- Donze J, Le Gal G, Mine MJ, Roy PM, Sanchez O, Verschuren F, et al. Prospective validation of the Pulmonary Embolism Severity Index: a clinical prognostic model for pulmonary embolism. Thromb Haemost. 2008;100(5):943-8.
- Hoeper MM, Madani MM, Nakanishi N, Meyer B, Cebotari S, Rubin LJ. Chronic thromboembolic pulmonary hypertension. Lancet Resp Med. 2014;2:573.
- Cho JH, Sridharan GK, Kim SH, Kaw R, Abburi T, Irfan A, et al. Right ventricular dysfunction as an echocardiographic prognostic factor in haemodynamically stable patient with acute pulmonary embolism: a metaanalysis. BMC Cardiovasc Disord. 2014;14:64.
- Kucher N, Rossi E, De Rosa M. Prognostic role of echocardiography among patients with acute pulmonary embolism and a systolic arterial pressure of 90 mmHg or higher. Arch Intern Med. 2005;165(15):1777-81.
- Meyer G, Vicaut E, Danays T, Agnelli G, Becattini C, Beyer-Westerndorf J, et al. PIETHO: Fibrinolysis for patients with intermediate risk pulmonary embolism. New Engl J Med. 2014:370:1402-11.
- Sharifi M, Bay C, Skrocki L, Rahimi F, Mehdipour M. Moderate pulmonary embolism treated with thrombolysis. Am J Cardiol. 2013;111(2):273-7.
- Galiè N, Humbert M, Vachiery J, Gibbs S, Lang I, Torbicki A, et al. 2015 ESC/ERS Guidelines for the diagnosis and treatment of pulmonary hypertension: The Joint Task Force for the Diagnosis and Treatment of Pulmonary Hypertension of the European 2016. Eur Heart J. 2016;37(1):67- 119.
- Suntharalingam J, Treacy CM, Doughty NJ, Goldsmith K, Soon E, Toshner MR, et al. Long-term use of sildenafil in inoperable chronic thromboembolic pulmonary hypertension. Chest. 2008;134(2):229-236.
- Reichenberger F, Voswinckel R, Enke B, Rutsch M, El Fechtali E, Schmehl T, et al. Long-term treatment with Sildenafil in chronic thromboembolic pulmonary hypertension. Eur Respir J. 2007;30(5):922-7.
- Dias-Junior CA, Vieira TF, Moreno H, Evora PR, Tanus-Santos JE. Sildenafil selectively inhibits acute pulmonary embolism-induced pulmonary hypertension. Pulm Pharmacol Ther. 2005;18(3):181-6.
- Dias-Junior CA, Souza-Costa DC, Zerbini T, Rocha JBT, Gerlach RF, Tanus-Santos JE. Effect of sildenafil on pulmonary embolisminduced oxidative stress and pulmonary hypertension. Anesth Analg. 2005;101(1):115-20.
- Dias-Junior CA. The use of sildenafil in the therapy of massive pulmonary embolism. Intensive Care Med. 2006;32(8):1284.
- Bonatti HJR, Harris T, Bauer T, Enfield K, Sabri S, Sawyer RG, et al. Transfemoral catheter thrombolysis and use of Sildenafil in acute massive pulmonary embolism. J Cardiothorac Vasc Anesth. 2010;24(6):980-4.
- Ganiere V, Felhi F, Tagan D. Dramatic beneficial effects of sildenafil in recurrent massive pulmonary embolism. Intensive Care Med. 2006;32(3):452-4.
- Lewis GD, Bloch KD, Semigran MJ. Pulmonary thromboembolism superimposed on a congenital ventricular septal defect in a 50-yearold man inhaled nitric oxide and sildenafil to the rescue. Cardiol Rev. 2004;12(4):188-90.
- Galea M, Quiney N. Sildenafil in acute pulmonary embolism: case report and review of the literature. JICS. 2009;10(1):44-5.