Case Report
Rectal Perforation by High Pressure Compressed Air. A Case Report
Amer Hashim Al Ani1*, Aaya Al Jundi3, Safaa Kasim Mohammed2, Zahir Al Jowher1, Sabah Al Kaisy1, Hesham Abdulmoneim1, Hassan Abdulhakim1 and Eltegani Eltayieb Ahmed1
1Department of General Surgery, Sheikh Khalifa General Hospital, United Arab Emirates
2Department of Diagnostic Radiology, Sheikh Khalifa General Hospital, UnitedArab Emirates
3Department of General Surgery, Al Sharjah University, United Arab Emirates
*Corresponding author: Amer Hashim Al Ani, Department of General Surgery, Sheikh Khalifa General Hospital, United Arab Emirates
Published: 30 Apr, 2018
Cite this article as: Al Ani AH, Al Jundi A, Mohammed SK,
Al Jowher Z, Al Kaisy S, Abdulmoneim
H, et al. Rectal Perforation by High
Pressure Compressed Air. A Case
Report. Clin Surg. 2018; 3: 1959.
Abstract
Background: Rectal trauma is rare. Mostly affecting males (>85%).Its location (intra vs extraperitoneal)
determines its management. Rectal injuries cause peritonitis, sepsis and even death if
not detected early. Associated mortality is 3% whereas morbidity is 25%.
Case Study: We report a 47 year old male presented with generalized abdominal pain after
inserting a high pressure compressor in his anus. His past medical history wasn't significant. On
physical examination, his abdomen was tender and distended. Laboratory findings revealed mild
leukocytosis. Chest X-ray showed air under the diaphragm bilaterally. Explorative laparotomy was
done. Posterior wall of upper rectum perforation was discovered. Primary repair was performed. No
complications after one month follow-up.
Discussion: Colo-rectal barotraumas by compressed air may cause rectal perforation. Mostly
at the anti-mesenteric surface of the sigmoid colon. Plain radiographs aid diagnosis. Computed
tomography (CT) is sensitive and specific for rectal injury. The gold standard treatment of intraperitoneal
perforations is primary repair.
Conclusion: Rectal perforation by compressed air is uncommon. Primary repair is appropriate in
early presentations, minimal tissue damage and no peritoneal contamination.
Keywords: Rectum; Barotraumas; Colon; Perforation; Compressed air
Introduction
Rectal trauma is rare [1,2]. According to large trauma databases, rectal injury, either alone or combined with colonic injury, is uncommon with a 1.1% incidence of colorectal injury in 16,814 blunt trauma patients [1]. Published reports of military rectal injury are less common than civilian, but the incidence of rectal injury is often higher in military trauma due to the higher energy transfer wounding mechanisms. Military colorectal injury in general usually results from higher energy transfer than civilian injury, leading to more widespread organ and tissue damage. Colorectal trauma is generally classified as either being blunt or penetrating in nature [3]. A smaller number is caused by other means including surgical or endoscopic mishap, obstetric trauma or misadventure such as autoerotism and sexual assault. Reporting is variable and it is likely that many rectal injuries from iatrogenic trauma, foreign body or sexual assault remain under-reported1. The majority of patients are males1 (>85%), with an average age of 29 year reflecting the higher incidence of vehicular and violence-associated injuries in young men whereas older age groups are more likely to suffer iatrogenic injury from endoscopy. The diagnosis of trans-anal rectal injuries is usually delayed because of patient’s denial and late presentation [4]. High index of suspicion leading to early diagnosis and active management thereafter, are essential for favorable outcomes [4-6]. At present, mortality from colorectal trauma is approximately 3%, most commonly from hemorrhage (40%), associated injuries (19%) and sepsis (14%), but associated morbidity remains high with a rate of 25% due to development of intra-abdominal sepsis. Isolated trauma, typified by rectal foreign body insertion, also carries an associated, but lesser, mortality rate with sporadic reports of fatal perforations. With the increased use of compressed air in industrial work, the risk of associated pneumatic injury from its improper use has also increased. However, colonic damage caused by compressed air is uncommon. Trans-anal barotraumas due to compressed air leading to colonic injury has been reported from time to time. It was first reported in the literature in 1904 [7-9]. Case analysis of pressurized air injuries often reveals an erroneous behavior of the workplace colleagues but air in sufflation during colonoscopy procedure was found to be the most common cause of colon barotraumas [8-10] with a reported incidence of 0.1 to 0.5% and 0.12% in another study [11]. The resulting trauma to the colon may range from a mild ‘‘cat scratch” colon to complete perforation. The overall mortality of pneumatic rupture of the bowel was assessed to be at 65%. If the acute shock was not immediately fatal, the survival was depending on further treatment. Surgery reduced mortality to 42%. The prognosis has generally been favorable in recent years [7- 12], although early collective reviews reported grave results.
Case Presentation
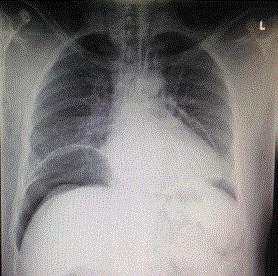
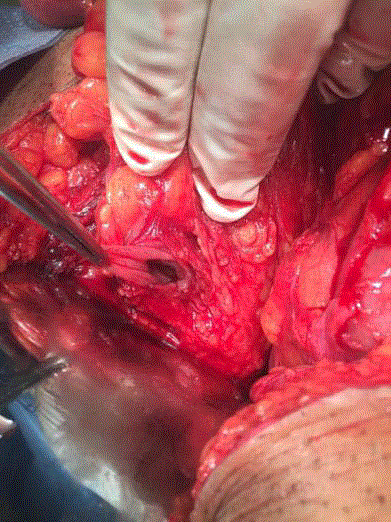
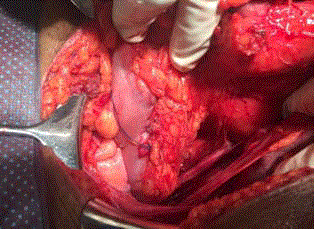
A 47 year old male presented to the ER complaining of severe generalized abdominal pain for 3 hours following applying a high pressure compressor into his anus. His past medical, psychiatric and family history showed nothing of significance. He was not on regular medication.On physical examination he was alert, oriented and febrile (38.2°C). Otherwise all other vital signs were within normal. Abdomen was distended with generalized tenderness. Bowel sounds were positive. Digital rectal examination revealed external hemorrhoids, empty rectum and there was no blood or discharge. Laboratory workup revealed slightly elevated WBC count. (11.07 × 109/ L). Other laboratory findings were within normal. Erect chest radiograph revealed air under both sides of the diaphragm that suggests a perforated intra abdominal viscous (Figure 1). Patient was admitted. Pain killer and prophylactic dose of antibiotic were given. The possibility of bowel perforation was discussed with the patient and consent was taken for explorative laparotomy to deal with the perforation. Explorative laparotomy revealed a clean abdominal cavity, with no spillage or contamination. Preliminary bowel examination showed no clear perforation. Mobilization of the rectum was done yet no clear perforation was found (the bowel was collapsed). A rectal tube was inserted; air was given through anal canal after covering the abdominal content with normal saline to detect any perforation. Air bubbles were revealed pointing to a 4 cm perforation at the posterior wall of recto sigmoid junction (Figure 2). The perforation was sutured in 2 layers with vicryl 2-0 (Figure 3). Leak test was negative. Wash of the peritoneal cavity was done with normal saline. A drain was left in the pelvis. Post-operative period was smooth. Patient was discharged home in good general condition at 5th post-operative day. One month follow-up was an eventful.
Discussion
Merlino and Reynolds (2004) review of 39 studies showed that penetrating trauma accounted for at least 80% of rectal injuries while 6.2% only were due to blunt mechanisms, one third of which were from Motor Vehicle Collisions (MCVs). A systematic (2017) review of available literature from 1999 to 2016, reporting on 1255 an rectal injury patients, showed that gunshot was the most common mechanism of injury (46.9%). Less common mechanisms of injury included explosive or blast injuries sustained in military combat (24.6%), knife stab wounds (0.49%) and foreign body injuries (2.47%). Although retained rectal foreign bodies have been reported in patients of all ages, and ethnicities, more than two-thirds of patients with rectal bodies are men in their thirties and forties, and patients as old as ninety years were also reported. However, there is a bimodal age distribution, observed in the twenties for anal autoeroticism or forced introduction through anus, and in the sixties mainly for prostatic massage and breaking fecal impactions [13]. The commonest cause of rectal foreign body insertion is sexual gratification, other causes include: personal hygiene, relief of pruritus any or constipation, psychosis, drink related betting, accidents and sexual assaults. Patients with psychiatric disorders should be referred to psychiatric assessment to prevent recurrence. There is a wide variety of reported foreign bodies that can cause colorectal injuries, examples include: Billy clubs, various fruits and vegetables, vibrators, nails, light bulbs, bottles, impulse body sprays and cans. Most objects are introduced through anus, however, sometimes; a foreign body is swallowed, passed through the gastrointestinal tract and trapped in the rectum. One of the most common types of rectal foreign body is best known as body packing and is commonly used by drug traffickers. Involuntary sexual foreign bodies are almost exclusively in the domain of rape and sexual assault. Involuntary nonsexual foreign bodies are generally found in the elderly, children, or the mentally ill. The objects are usually retained thermometers and enema tips, aluminum foil wrapping from pill containers and orally ingested objects, such as tooth picks, chicken bones, plastic objects such as erasers or pill bottle caps and even coins or small plastic toys. Cases of full thickness perforation with or without peritonitis do occur occasionally with a fatal outcome, but the majority of rectal foreign body insertions cause mucosal injury only. Anal fisting injuries represent a specific subgroup of rectal insertion injury and are more likely to cause full thickness injury. Rectal foreign bodies can be also introduced for diagnostic and therapeutic purposes. Iatrogenic rectal injury is rare, accounting for about 2.5% of cases (2004), but can range from minor mucosal tears to full thickness injury. Although colonic perforation from procedures is well reported and the risk well quantified there is little data for rectal injury. Quallick and Brown (2009) reported four rectal perforations in nearly 40,000 colonoscopies, attributed to retro flexion in the rectum. There also other sporadic case reports1.The incidence of rectal perforation following barium enema studies ranges from 0.002 to 0.23% and carries a mortality of up to 50% because of the toxic effect of the extra vasated barium1. Rectal injury sustained during pelvic surgery is rare. Rectal injury is always a potential complication during laparoscopic radical prostatectomy, the rate is approximately 1–2%, with the majority recognized and managed intra-operatively. The risk of sustaining a rectal injury is significantly increased in patients with pubic symphysis diastasis or sacroiliac joint fractures. Rectal injury caused by pelvic fracture is associated with high mortality and morbidity levels. The rate of perineal sepsis is up to 77%. Other rare iatrogenic causes of rectal perforation include: a case of necrosis of the rectal wall developed after performing sclera therapy for treating internal hemorrhoids and a case of rectal injury that occurred during cyst copy that was performed because of benign prostatic hypertrophy. Perforations due to cancer (advanced colorectal carcinoma contributes to 1.2 to 9% of rectal perforations [6,14] and infection have higher mortality rates than iatrogenic perforation during colonoscopy [15]. One other worth mentioning entity is spontaneous rupture of the rectum, it is a rare [16,17] occurrence with less than seventy cases being reported in literature. Studies have shown rectal prolapse to be associated in 60–76% of cases. Compressed air is widely used for both industrial and domestic purposes. Compressed air is air kept under a pressure that is greater than atmospheric pressure. With the advent of high-pressure compressed air in industrial work, the risk of associated pneumatic injuries from its improper use is becoming evident. Since it stores large amounts of energy at high pressure, unwise use may lead to grave incidents at the workplace. A misdirected jet of compressed air to the head can cause serious eye injuries or rupture of the eardrum. Aiming the compressed air into the mouth can damage the lungs and esophagus. Careless use of compressed air to blow away dirt or dust from the body, even with a protective layer of clothes, could allow the air to enter the body, which can damage the internal organs7,8. Among pneumatic injuries, colon injury by accidental in sufflation is one of the most serious because an enormous amount of air can be delivered into the rectum in a very short time. It is not well recognized by the public that the pressure of compressed air can penetrate barriers such as clothes and the anal sphincter thereby causing severe colon injury. This injury can occur without directly inserting the air hose into the anus, even when clothes are worn. The worn clothing and the anal sphincters might become weakened due to the pressure and volume of the jet of air, and this can also cause perforation, tension pneumo peritoneum or gangrene of the bowel within a short period of time. The gangrene occurs due to over distension of the bowel, which compromises the blood supply. It was suggested that it takes only 1 or 2 seconds to deliver enough compressed air to cause major damage. Andrews, using compressed air to distend the intestine of a dog, found that normal intestine required a pressure of 0.49–0.88 kg/cm2 to get ruptured. Burt showed that the average pressure needed to cause a full thickness tear in human gastrointestinal tracts is 0.29 kg/cm2. In industrial fields, highly compressed air, exerting higher than 10 kg/ cm2, is widely used. It is far greater than the pressure needed for intestinal perforation. Highly compressed air is known to form a column that acts like a solid body forcing open the anal sphincter. The funnel shaped anatomy of the buttock facilitates the air to concentrate around the anus and allows the easy delivery of air through the anus. As the anal canal and distal rectum are well supported by external structures, the recto sigmoid region, with the firm lateral support of the rectum, is the first part of the colon to be struck by a column of air. Therefore, most of the injuries occur around the junction of the rectum and sigmoid colon. The most common location of injury is the anti-mesenteric surface of the sigmoid colon [7-10]. The sudden high velocity in sufflation of air induces extreme shear force at the point of maximal fixation. The recto-sigmoid junction has bilateral fixation, which limits its mobility, thus, compressed air in sufflation with high velocity can cause recto-sigmoid colon barotraumas. However, colon perforation can occur as single or multiple lesions at any site of the colon. The pathologic lesions following pneumatic in sufflation depend on the resultant in traluminal pressure, the airflow velocity, the anal resting pressure and the distance between the source and anus. The resultant injury usually occurs in a longitudinal direction along the muscle fibers with either serosal hemorrhage, lacerations of the serosa and muscular coat with bulging of the mucous membrane, or full-thickness rupture of the bowel through the serosa, muscular coat and mucous membrane. In the majority of cases, the injuries are only sero muscular lacerations. A case was reported, in 2013, had multiple serosal injuries in all segments of the colon, especially the sigmoid colon and the caecum, although there was no perforation. The diagnosis of rectal barotraumas is not difficult if the patient has a history of abdominal pain and distension after exposure to compressed air. However, a history in these cases may be obscure. Because of the fact that these injuries, even when accidental, are embarrassing and unacceptable from a social perspective, admissions to hospital are usually delayed. Patients may withhold information and attempt to conceal the facts, trying to protect the guilty party or due to hesitancy. Reluctance to seek medical care may lead to delayed presentation. Delayed presentation is a major contributing factor for morbidity. This remains one of the most common challenges in the management of trans-anal rectal injuries. Most patients present to the emergency room after efforts to remove the inserted object at home. Moreover, in the emergency room, patients may often be less than truthful regarding the reason for their visit, leading to extensive workups and further delays. However, patients with acute abdominal pain of unknown origin should be checked for trauma history and occupational history, such as construction, industrial worker and cleaner’s staff, who commonly use compressed air. The assessment of rectal injury is by a combination of clinical, endo luminal and radiographic means. Victims of trauma (other than iatro genesis) should be assessed using a recognized trauma system with the history focusing on the mechanism of injury and the type of weapon or implement used. The secondary survey should assess pelvic fracture, perineal or trans-pelvic penetration and rectal or urethral bleeding. Injury due to foreign body insertion rarely causes widespread trauma, but one should recognize the risk of other physical and psychological injuries, especially in cases of assault1. Examination of the abdomen is essential in order to locate potential sites of penetration or bleeding. The presence of signs of peritonitis such as local or generalized guarding and rigidity will give an indication as to the severity of internal bowel and/or organ damage 3.Digital Rectal Examination (DRE) is part of the routine secondary survey but is insensitive for detecting ano rectal injury with reported sensitivities of 37%, 33% and 5% for detection of decreased anal tone, rectal wall injury and fresh rectal bleeding, respectively, in 2007. Rectal examination is essential in the diagnosis, but it should be performed after abdominal X-ray to prevent accidental injury to the surgeon from sharp objects. Careful attention should also be paid to the status of the sphincter, especially in patients who have no prior history of foreign body placement and those with involuntary insertions. The sphincter tone might be increased secondary to muscular spasm as a result of the foreign object insertion. Laboratory evaluation is not very helpful in patients with trans-anal rectal injuries. If the patient has a suspected perforation, the white blood cell count may be elevated and acidosis may be present on chemistry. These laboratory tests are not very helpful, as the physical examination. If a rectal injury is suspected, a rigid proctoscopy or sigmoidoscopy is mandatory, as it can reveal blood in the lumen or a rectal wall injury, as well as ascertaining the anatomy. It has a higher sensitivity than DRE for detecting any rectal injury (78% vs. 51%), which increases to 88% in the detection of extra-peritoneal injuries. The combination of blood on DRE and positive findings on rigid sigmoidoscopy accurately predicts rectal injury in 95% and is considered the gold standard for investigating rectal trauma1. Another study stated that proctoscopy is the gold standard in the detection of rectal injuries with reported sensitivities near 100%. However, in the case we report; sigmoidoscopy was not done to avoid contamination. Abdominal radiographs are neither sensitive nor specific for colorectal injury but can reveal useful diagnostic information such as free sub-diaphragmatic air and are a rapid method for confirming a retained rectal foreign body. As for the role of ultra sonography, free intra peritoneal air detection using ultrasound is operator dependent and can be difficult even for an experienced ultrasound operator. The ultrasound findings should be correlated with the clinical picture as a whole and used within defined diagnostic algorithms. Point-of-care ultrasound is an extension of the clinical examination. It is a goal-directed study that can be used for rapid diagnosis. It is accurate, non-invasive, cost effective and repeatable. It has no risk of radiation, and can be done in unstable patients parallel to physical examination and resuscitation. Furthermore, ultrasound can be done while the patient is in the supine position, and may detect small amount of free intra peritoneal air compared with an erect chest X-ray which may be negative in up to 10% of patients with perforated bowel. Small amount of free intra peritoneal air can be detected under the anterior abdominal wall and in Morison’s pouch. This would be useful even in early bowel perforation without peritonitis. Also, ultrasound is useful in disaster and austere situations when formal X-rays cannot be performed. Trapped free intra peritoneal air bubbles in a localized fluid collection will give rise to echo genic foci. The associated findings of thickened momentum and bowel, and free pelvic fluid points towards peritonitis. It is important to stress that ultrasound usually rules in and does not rule out a bowel perforation which indicates that a negative study does not exclude a bowel perforation. If needed, and if the patient is hemo dynamically stable, then an abdominal CT scan may give more information than ultrasound. CT scanning has high sensitivity and specificity for diagnosing colorectal injury and is usually advocated in trauma patients as long as it does not delay treatment. In major intraabdominal trauma, its sensitivity and specificity is approximately 100% and 96% respectively, with a negative predictive value of 100%. It can also accurately image the retroperitoneal space. The wellrecognized limitation of CT scanning is the need to remove the patient from the relative safety of the emergency department to radiology department in many hospitals. Common CT findings in rectal trauma are air in the Para-rectal spaces, metallic fragments in close proximity to the rectum, rectal wall thickening and free fluid. In the military setting, CT scanning is a useful tool for rapid evaluation of the poly-trauma patient allowing prioritization of operative resources. No rectal injuries were missed but there were 2/10 false positive scans reported. Diagnostic yield may be increased by adding water soluble oral and rectal contrast to standard intravenous contrast (‘‘triple contrast CT’’) in penetrating trauma. CT scanning has further advantages as it is the gold standard for identification of other organ injuries and diagnose vascular injury in proximity to rectal trauma, it also allows wound track evaluation which may be sufficient evidence to allow a non-operative management strategy and avoid unnecessary laparotomy. Intraperitoneal free air on a simple abdominal or abdominopelvic CT scan confirms the colon perforation. For our case, contrast CT scan would cause more contamination and plain CT scan will not add much to the diagnosis because chest X-ray had already confirmed the presence of air under the diaphragm, and the history along with the overall clinical picture were sufficient for the diagnosis of colonic perforation caused by compressed air. Colorectal trauma is generally classified as either being blunt or penetrating in nature. The simplest classification divides rectal trauma into intraand extra-peritoneal injury, which determines the management. Extra-peritoneal injury occurs by shearing at the ano rectal junction where the bowel is relatively fixed. Management strategies have evolved considerably over the last five decades, largely due to developments in military medicine practices. Battlefield colorectal injury has provided the principles of management that have subsequently been adopted, and then adapted, into the care of civilian injuries. As a result, there has been a significant reduction in associated morbidity and mortality over the years. To date, there are significant international discrepancy and sparse evidence regarding the management of penetrating trauma to the rectum. No definitive guidelines or clear consensus on best strategies of anorectic trauma management are available. However, the severity of the injury to the rectum should be individually assessed and managed on a patient by patient basis. Given the strong association with other serious injuries, management should include appropriate resuscitation and prioritizing life-saving procedures first1.Basic management principals include early hemorrhage control while reducing contamination of the intra-abdominal cavity. Early detection and treatment of visceral injuries is essential. Early emergency laparotomy, after controlling shock, is recommended as soon as the diagnosis of full-thickness perforation is made. Primary repair or resection and anastomosis with or without diversion should be performed. Thorough drainage and irrigation of the contaminated abdominopelvic cavity is advisable. Careful observation following surgery is important since rupture of the colon may have delayed presentation. Intraperitoneal rectal injuries involve the proximal two thirds of the rectum and are sufficiently accessible to be managed as colonic injuries with direct repair or resection with primary anastomosis. The gold standard is primary repair, as demonstrated by a Cochrane review in 2003 which observed better outcomes in terms of total complications, total infectious complications, and abdominal infections and wound complications in those having primary repair versus fecal diversion. However, primary repair or anastomosis after resection is not appropriate if the fecal contamination is severe and the bowel is edematous. Similar to the case we are reporting, patients who present early after the insult, with minimal tissue damage and with little to no contamination can be managed with primary repair and washout. The distal third of the rectum is difficult to access and management of extra- peritoneal rectal injuries is challenging. Direct repair is usually impossible; the mainstay of treatment in most instances remains fecal diversion. To prevent further pelvic contamination. Fecal diversion can be achieved by either a proximal loop colostomy or Hartmann’s procedure, depending on the severity of the injury and the condition of the patient. There is no difference in the efficacy of the two types of proximal diversion but reversal of a loop stoma is easier. In civilian rectal trauma, pre-sacral drainage and distal rectal washout are probably not required but may still play a part in the management of military rectal trauma where an aggressive multi-faceted approach to this injury is warranted to minimize septic complications within the closed confines of the pelvis and maximize functional outcome. Laparoscopic approach to repair of rectal perforation is feasible, especially in cases which present early. One of the first reports of this approach was by Najah and Pocard in 2015. The challenge in these cases would be to suture the rent which is just at the peritoneal reflection, deep in the pelvis and in a limited space. The port placement would be the same as those in rectal prolapse surgery. The site of perforation is identified and the extent of contamination assessed. The prolapsed bowel or omentum, depending on its viability, is either thoroughly cleansed or resected. The rectal tear is repaired and a biopsy of the edges is warranted if an underlying pathology is suspected [14-17]. Laparoscopic approach has been successfully applied in the treatment of colonic perforations, where equivalent operative outcomes as open procedures can be accomplished in selected patients. Conservative management is suitable if no perforation is identified radio logically, and the patient has no signs of peritonitis. If perforation has occurred and is evident radio logically, but signs of general peritonismare absent and the patient’s condition is good, the perforation might have been sealed. In such a case, expectant management should be adopted. Those with partial thickness injuries to the extra-peritoneal rectum could be managed conservatively with observation, antibiotics and avoidance of oral feeding. Merlino and Reynolds’ (2004) analysis of over 1100 rectal injuries from 39 studies revealed an overall complication rate of 24%, the single most common complication being abdominal or pelvic abscess formation (5.3%); fistula formation and generalized sepsis occurred in 2.8% and 2.3%, respectively. Pelvic abscesses may be amenable to percutaneous drainage. Traumatic disruption of the anal sphincter can result in mild to severe fecal incontinence, depending on the degree of the injury. When compared with partial thickness injuries, full thickness injuries had a three times higher rate of complications, including septic complications. They also have longer duration of colostomy and a lower rate of colostomy reversal. When a large amount of gas is introduced into the peritoneal cavity, the intra abdominal pressure increases. High intra peritoneal air pressure can compress the inferior vena cava and cause obstructive shock. Other potential complications may include: pneumothorax, rhabdomyolysis and respiratory distress.The elimination of air using a large bore needle is a simple and effective method for relieving pneumoperitoneum tension and respiratory distress7. Intraperitoneal rectal injuries will cause peritonitis, sepsis and even death if not detected early. The path physiology of death can be acute air embolism, acute fat embolism, acute respiratory insufficiency due to enhanced intra abdominal pressure and chest compression, acute heart failure due to insufficient preload and peritoneal shock. The majority of serious complications and deaths are associated with delayed presentation, more severe injury pattern (as witnessed by other organ injuries) and shock on presentation. Recovery is usual if the injury is only seromuscular. Patients with premorbid disease and elderly are more likely to suffer from complications as they have lower physiological reserve than their healthier counterparts.
Figure 1
Figure 2
Figure 3
Conclusion
Civilian rectal trauma is often associated with life-threatening injury and commonly affects young males. Colonic barotraumas by compressed air could result from the unwise use of air compresses. High index of suspicion leading to early diagnosis and active management thereafter, are essential for favorable outcomes. The majority of cases need surgical intervention. Initially, all patients with traumatic injuries should be managed according to the Advanced Trauma Life Support (ATLS) principles defined by the American College of Surgeons. Assessment of trans-anal rectal injury should include a sexual history, as the patient could be at risk of sexually transmitted diseases or be a victim of sexual abuse. Plain radiographs may aid diagnosis. CT scanning is sensitive and specific for rectal injury and should be performed if the patient’s condition allows. The ‘key’ factor in successful management is the early detection of any visceral injury. The surgical management of the rectal injury depends on its anatomical location in relation to the peritoneum as intra peritoneal injuries may be treated as a colonic lesion. The evidence for extra-peritoneal injury is conflicting. The role of pre-sacral drainage and distal washout remains contentious in the realms of civilian rectal injury but retains a place in battlefield or other high-energy transfer rectal injuries where aggressive early management reduces septic complications. Rectal washout, pre-sacral drainage and proximal diversion are three ongoing controversies in the management of anorectal trauma.
References
- Barkley S, Khan M, Garner J. Rectal trauma in adults. Trauma. 2012;15(1):3-15.
- Gümüş M, Böyük A, Kapan M, Onder A, Taskesen Fetal. Unusual extraperitoneal rectal injuries: a retrospective study. European Journal of Trauma & Emergency Surgery. 2012;38(3);295-9.
- Ahern DP, Kelly EM, Courtney D, Rausa E, Winter DC. The management of penetrating rectal and anal trauma:A systematic review. Injury. 2017;48(6):1133-8.
- Abu-Zidan FM, Abusharia MI, Kessler K. Surgeon-performed sonographic findings in a traumatic trans-anal rectal perforation. World Journal of Emergency Surgery. 2011;6:26.
- El-Ashaal YI, Al-Olama AK, Abu-Zidan FM. Trans-anal rectal injuries. Singapore Medical Journal. 2008;49(1):54-6.
- Fu WP, Quah HM, Eu KW. Traumatic rectal perforation presenting as necrotizing fasciitis of the lower limb. Singapore Medical Journal. 2009;50(8):270-3.
- Park YJ. Rectal perforation by compressed air. Annals of Surgical Treatment and Research. 2017;93(1):61-3.
- Pai V, Shetty S. Fatal recto-sigmoid rupture by compressed air. Egyptian Journal of Forensic Sciences.2016;6(4):542-5.
- Al-Ozaibi, L., Al-Jarrah, Z. (2016). Colorectal injury by compressed air: the rule of conservative therapy. Journal of Coloproctology. 2017;37(1):47-9.
- Choi JY, Park KS, Park TW, Koh WJ, Kim HM. Colon Barotrauma Caused by Compressed Air. Intestinal Research. 2013;11(3):213-6.
- De Bakker J, Bruin S. Successful laparoscopic repair of a large traumatic sigmoid perforation. Journal of Surgical Case Reports. 2012(2):3.
- Yin WB, Hu JL, Gao Y, Zhang XX, Zhang MS, Liu GW, et al. Rupture of sigmoid colon caused by compressed air. World Journal of Gastroenterology. 2016;22(10):3062-5.
- Coskun A, Erkan N, Yakan S, Yildirim M, Cengiz F. Management of rectal foreign bodies. World Journal of Emergency Surgery. 2013;8(1):11-15.
- Bielecki K, Kamiński P, Klukowski M. Large bowel perforation: morbidity and mortality. Tech Coloproctol. 2002;6(3):177-82.
- Shin R, Lee SM, Sohn B, Lee DW, Song I, Chai YJ, Heo SC. Predictors of Morbidity and Mortality After Surgery for Intestinal Perforation. Annals of Coloproctology. 2016;32(6):221-7.
- Kumar A, Jakhmola CK, Kukreja Y, Kumar SS, Sandhu AS. An adolescent with prolapsed omentum per rectum: Spontaneous rectal perforation managed laparoscopically. Journal of Minimal Access Surgery. 2017;13(2):151-3.
- Gupta M, Goyal S, Goyal R, Sharma S. Spontaneous Rectal Perforation: A Rare Occurrence. Journal of Pioneering Medical Sciences. 2014;4(1):49-51.