Case Report
Metastasis of Breast Cancer to Renal Cell Carcinoma: A Rare Case of Tumor-to-Tumor Metastasis (TTM)
Eymen Gazel1|*, Serdar Yalcın2, Engin Kaya2, Aytug Uner3, Yesim Saglıcan4 and Lutfi Tunc5
1Department of Urolog, Acıbadem University, Turkey
2Department of Urology, Gulhane Education and Research Hospital, Turkey
3Department of Oncology, Gazi University School of Medicine,Turkey
4Department of Pathology, Acıbadem University, Turkey
5Department of Urology, Gazi University School of Medicine, Turkey
*Corresponding author: Eymen Gazel, Department of Urology, Acıbadem University, Ankara, Turkey
Published: 09 Mar, 2018
Cite this article as: Gazel E, Yalcın S, Kaya E, Uner A,
Saglıcan Y, Tunc L. Metastasis of
Breast Cancer to Renal Cell Carcinoma:
A Rare Case of Tumor-to-Tumor
Metastasis (TTM). Clin Surg. 2018; 3:
1935.
Abstract
Objectives: The aim of this case presentation was to show a case of primary breast cancer with
metastasis to renal cell cancer.
Methods: A 42-year old female patient presented with a palpable mass in both breasts and tru-cut
biopsy was applied. The result of the biopsy showed in the right breast: invasive ductal carcinoma
and in the left breast: mixed invasive ductal and invasive micropapillary carcinoma. In the upper
pole of the left kidney, a mass of approximately 3cm was determined. With these findings, the patient
was diagnosed as Grade 4 breast cancer with multiple distant metastases and chemotherapy was
planned. At the end of a 10-month follow-up period, the metastases had recovered and the response
of the patient to chemotherapy was reported to be good. However on the follow-up abdominal CT,
there was observed to still be a mass in the mid-section of the left kidney, 2.7 cm × 2.8 cm × 3.3
cm in size, showing contrast involvement and consistent with malignancy. Laparoscopic radical
nephrectomy was applied to the patient. Unclassified type RCC was determined. The general status
of the patient is currently good with no recurrence and follow-up is continuing.
Results and Conclusions: To date, metastasis of breast cancer has been determined in only 3 cases
of resected RCC. This case is of value as the fourth case in literature of RCC metastasis from breast
cancer. In conclusion, metastasis from breast cancer to RCC is not often encountered in patients.
The case presented here is the 4th case of nephrectomy applied and proven breast cancer metastasis
to RCC. Therefore, there is extremely limited information about the follow-up of these patients.
There is a need for long-term follow-up to share the problems and treatment of these patients.
Keywords: Breast cancer; RCC; Metastasis; Oncology; Nephrectomy
Introduction
When two different tumors are determined at the same time in one patient, they are known
as “synchronised tumors”. Although synchronised tumors are often encountered, metastasis to a
tumor from a tumor of different primary origin is a rarely seen occurrence. This is known as Tumorto-
Tumor Metastasis (TTM) phenomenon [1]. TTM was first defined by Berent in 1902, as the
visualisation in the same localisation of two tumors originating from different organs which are
histologically, morphologically and immunophenotypically independent of each other [2-4].
It is known that Renal Cell Cancer (RCC) is often seen together with other organ tumors and
metastases from other organ tumors to RCC are also seen [5]. However, it can be understood
from literature that metastasis of breast cancer to RCC has been observed very rarely [1]. To date,
metastasis of breast cancer has been determined in only 3 cases of resected RCC. Nevertheless,
there have also been 2 cases reported where metastasis of breast cancer to RCC was determined
incidentally during autopsy [6,7].
The aim of this case presentation was to show a case of primary breast cancer with metastasis to
renal cell cancer. This case is therefore the fourth case in literature of RCC metastasis from breast
cancer.
Case Presentation
A 42-year old female patient presented with a palpable mass in
both breasts and tru-cut biopsy was applied. The result of the biopsy
showed in the right breast, invasive ductal carcinoma Grd1, Ki-67
proliferation index: 20%, Estrogen Receptor (ER): 95%, progesterone
receptor (PR): 80% (+), C-ERB-B2 (-); and in the left breast: mixed
invasive ductal and invasive micropapillary carcinoma, Grd2, Ki-67
proliferation index: 30% to 40%, ER:90%, PR:60% (+), C-ERB-B2
(-). In the Computed Tomography (CT) scanning applied to the
patient, multiple primary cancer foci were determined bilaterally in
the breasts and multiple metastases were determined in the bones and
lungs. In the upper pole of the left kidney, a mass of approximately 3
cm was determined.
With these findings, the patient was diagnosed as Grade 4 breast
cancer with multiple distant metastases and chemotherapy was
planned with the Oncology Department. In the chemotherapy, 7 cycles
of FEC (5-FU: 900 mg+ Epirubicin: 170 mg+ Cyclophosphamide:
900 mg) were applied and 5 cycles of TC (Docetaxel 140 mg+
Cyclophosphamide: 800 mg) and bone support treatment of
Zoledronic acid 4 mg once every 21 days.
At the end of a 10-month follow-up period, the metastases
had recovered and the response of the patient to chemotherapy
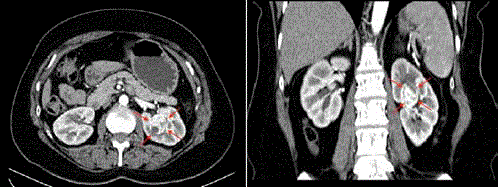
was reported to be good. However on the follow-up abdominal
CT, there was observed to still be a mass in the mid-section
of the left kidney, 2.7 cm × 2.8 cm × 3.3 cm in size, showing
contrast involvement and consistent with malignancy (Figure 1).
Laparoscopic radical nephrectomy was applied to the patient. In the
pathological examination, a tumor 3 cm in diameter was determined
macroscopically in the mid-section of the left kidney (Figure 2) and in
the histological examination, unclassified type RCC was determined
containing micropapillary breast cancer metastasis in the form of
small foci. There was reported to be no invasion to perirenal fat tissue,
the renal vein or lymph nodes and no microvascular invasion. The
pathology was reported as grade T1aN0M0.
In the histochemical examination applied with the Ventana
benchmark xt method, the results were reported as CK7
[Biocare Med(OV-TL 12/30)]: positive; WT1 [CELL MARQUE
(6F-H2)]:negative; ER [LEICA (6F11)]: positive in areas of breast
carcinoma, negative in RCC areas; HER-2/neu 4B5 [VENTANA]:
negative; GCDFP15 [Biocare Medical (D6)]:)]: positive in areas of
breast carcinoma, negative in RCC areas; GATA3 [CELL MARQUE
(L50-823)]:)]: positive in areas of breast carcinoma, negative in RCC
areas; PAX8 [CELL MARQUE (MRQ-50)]:)]: negative in areas of
breast carcinoma, positive in RCC areas; CD10 [SCYTEK (56C6)]:
negative; P504S [Biocare Medical (N/A)]: negative; Ki-67 [DAKO
(MIB-1)]: 5% in breast carcinoma areas, 1% in RCC areas.
Following the nephrectomy, hormonal treatment was started
of tamoxifen 2 × 10 mg/day. In respect of ease of use, bone support
treatment was added of Clodronate disodium 2 × 800 mg/day. The
general status of the patient is currently good with no recurrrence and
follow-up is continuing.
Discussion
Following the definition of Tumor-to-Tumor Metastasis (TTM)
phenomenon by Berent, Campbell stated the conditions required
for a case to be said to be TTM. According to this, the patient has
more than one tumor, the tumor receiving the metastasis is an actual
neoplasm, the tumor making the metastasis develops within the
receiving tumor, it does not develop through adjacent pathways or
by embolisation from vessels and the metastatic tumor is a tumor
which does not metastise to the lymphatic system on the basis of a
lymphovascular malignancy (lymphoma/leukemia) that is already
present [3,4]. The case presented here fulfilled these conditions and
can therefore be accepted as a case of TTM.
Two different theories have emerged to explain the
pathophysiology of the concept of TTM. One of these is the “seed
and soil” theory. According to this, the metastatic cell (seed) shows
easier development within tumor tissue of low metabolism and
containing high collagen and fat (soil). In an animal experiment
with results that supported this theory, it was shown that cancer cells
transferred within sarcoma tissue grew more rapidly than normal
tissue. The other theory is “mechanical”. According to this, there
is an increase in the vascular structure in the tumor tissue which is
present and associated with this an increase develops in the blood
supply. This causes circulation of more malignant cells in the tumoral
region, thereby creating an environment which increases the risk of
metastases [8].
RCC is the tumor that most often accompanies other malignancies
[6]. Furthermore, when all the TTM cases were examined, the most
common receiving tumor was seen to be RCC, followed by sarcoma,
meningioma, and thyroid cancer and hypophysis adenoma. The
cancer type which most often metastasis to other tumors is lung
cancer, followed by breast cancer and prostate cancer [9]. The reason
that RCC receives the most metastases is that the kidneys receive a
large part of cardiac output and are more exposed to metastatic cells.
This hypothesis can be seen to be consistent with the “mechanical”
theory.
The cancer metastising most often to kidney tumors is lung
adenocarcinoma. Although breast cancer is one of the cancers most rare. Metastasis from breast cancer to kidney angiomyolipoma has
been reported in a total of 3 cases [10]. Similarly, metastasis to RCC
is seen very rarely. To date, a total of 5 cases have been reported, 2 of
which were determined during autopsy. Thus, a total of 3 RCC cases
are known where they have been admitted for surgery and breast
cancer metastasis has been seen.
In those cases, it is noticeable that all the metastatic breast cancers
were invasive ductal cancer. In the current case, the breast cancer was
determined as micropapillary subgroup of invasive ductal type. In
literature, metastases have been examined immunohistochemically
with Estrogen Receptor (ER) staining. Two (2/5) cases were reported
as ER: positive, 2/5 as ER: negative, 1/5 as HER-2/neu positive and 3/5
as HER-2/neu negative. The results of 1 case were not available. In the
current case the breast carcinoma areas were stained ER positive and
HER-2/neu negative.
The age of patients with TTM ranges from 43 to 75 years. The
case presented here was 42 years old and is therefore the youngest
case in literature of metastasis from breast cancer to RCC. The time to
TTM after diagnosis of breast cancer has been reported to range from
1 year to a maximum of 30 years and in one case TTM was found
to be present during the breast cancer diagnosis [1]. In that case, no
response was seen to chemotherapy and as it was suspected that the
mass in the kidney could be a different malignancy from the breast
cancer, it was decided to perform a nephrectomy. In the current
case, the mass in the kidney was determined during the breast cancer
diagnosis. There is no definitive way of differentiating whether this
simultaneous lesion in the kidney is a metastasis from the primary
cancer, or a different malignancy of the kidney. In such cases it can be
considered more appropriate to start chemotherapy taking metasatic
breast cancer into account and then acting according to the response
to this treatment. When TTM was determined in all the other cases,
there were seen to be multiple metastases already in other locations
apart from RCC. In the current case, bone and lung metastasis was
also found when TTM was determined.
In other TTM cases, survey of the patients has been seen to
be short. One patient was lost at 10 months affter nephrectomy.
Another patient refused treatment and withdrew from follow-up
with recurrence and progression of metastases outside the kidney
in the postoperative 4th month. In the other case, follow-up could
not be made. Since the diagnosis of breast cancer in the current case,
14 months have passed and 4 months since the nephrectomy due
to the diagnosis of RCC. The general performance of this patient is
extremely good, with no recurrence, no progression and ongoing
follow-up.
In conclusion, metastasis from breast cancer to RCC is not often
encountered in patients. The case presented here is the 4th case of
nephrectomy applied and proven breast cancer metastasis to RCC.
Therefore, there is extremely limited information about the follow-up
of these patients. There is a need for long-term follow-up to share the
problems and treatment of these patients. In addition it must not be
forgotten that RCC is the most common tumor accompanying other
tumors and is even the most common metastasis receiving tumor.
If there is kidney involvement in patients with a metastatic tumor,
it should always be considered that there is the possibility that this
could be metastasis to the kidney from the primary tumor or a direct
RCC case.
Figure 1
Figure 2
Figure 2
A tumor 3 cm in diameter was determined macroscopically in the
mid-section of the left kidney.
References
- Huo Z, Gao Y, Yu Z, Zuo W, Zhang Y. Metastasis of breast cancer to renal cancer: report of a rare case. Int J Clin Exp Pathol. 2015;8(11):15417-21.
- Berent W, Seltene metastsenbildung, Zentralbl. Allg. Pathol. 1902;13:406.
- Campbell LV, Gilbert E. Chamberlain CR, Wtne AL. Metastases of cancer to cancer. Cancer. 1968;22(3):635-43.
- Amin M, Radkay L, Pantanowitz L, Fine J, Parwani A. Tumor-to-tumor metastasis (TTM) of breast carcinoma within a solitary renal angiomyolipoma: A case report. Pathol Res Pract. 2013;209(9):605-8.
- Richardson J, Katamaya I. Neoplasma to neoplasm metastasis. Arch Path. 1971;91:135-9.
- Sella A, Ro JY. Renal cell cancer: best recipient of tumor-to-tumor metastasis. Urology 1987;30(1):35-8.
- Val-Bernal JF, Villoria F, Pérez-Expósito MA. Concurrent angiomyolipomas and renal cell carcinoma harboring metastatic foci of mammary carcinoma in the same kidney: an incidental autopsy finding in a patient with a follow-up of thirty years. Ann Diagn Pathol . 2001;5(5):293-9.
- Hart IR. “Seed and soil” revisited: mechanisms of site-specific metastasis. Cancer Metastasis Rev. 1982;1(1):5-16.
- Petraki C, Vaslamatzis M, Argyrakos T, Petraki K, Strataki M, Alexopoulos C, et al. Tumor to tumor metastasis: Report of two cases and review of the literature. Int J Surg Pathol. 2003;11(2):127-35.
- Williams TR, Oakes MF. Metastatic breast carcinoma to renal angiomyolipomas in tuberous sclerosis. Urology. 2008;71(2):e57.