Review Article
Zone 1 Vascular Abdominal Trauma. Damage Control and Staged Management
Ioannis Stamatatos1*, Marigo Theodorou2, Efstathios Metaxas3, Dimitrios Klapsakis4, Konstantinos Bouboulis2,3, Nikolaos Tzatzadakis3 and Athanasios Rogdakis2
1Department of Vascular and Endovascular Surgery, General Hospital Nikaia, Greece
2Department of General Surgery, General Hospital Nikaia, Greece
3Department of Cardiothoracic Surgery, General Hospital Nikaia, Greece
4Department of Orthopaedics and Trauma, General Hospital Nikaia, Greece
*Corresponding author: Ioannis Stamatatos, Department of Vascular and Endovascular Surgery, General Hospital Nikaia, Greece
Published: 12 Feb, 2018
Cite this article as: Stamatatos I, Theodorou M, Metaxas E,
Klapsakis D, Bouboulis K, Tzatzadakis
N, Rogdakis A. Zone 1 Vascular
Abdominal Trauma. Damage Control
and Staged Management. Clin Surg.
2018; 3: 1905.
Abstract
Vascular abdominal injuries of major vessels in zone 1 abdominal cavity are the most common cause of death after penetrating abdominal trauma. Abdominal arterial and vein injuries occur with the same incidence. Patients with retroperitoneal vascular injury and intact retroperitoneum may present hemodynamically stable due to tamponade. The main goal of staged approach is to control any major haemorrhage into the abdomen until the patient is hemodynamically stabilized in the ICU and reconstruction can be done in final reoperation. Multidisciplinary management is imperative to prevent the “lethal triad” and assures the best optimal outcome for these critically wounded patients.
Introduction
Abdominal vascular injuries are the most common cause of death after penetrating abdominal trauma. Blunt injuries to major abdominal vessels are rare. Major injuries to large vessels in the abdominal zone 1 usually cause significant hemoperitoneum and shock. The type of clinical presentation varies widely and depends on the presence of retroperitoneal tamponade. Patients with an intact retroperitoneum may be hemodynamically stable on presentation but when the retroperitoneum tamponade is lost, signs of shock and acute hypovolemia are present. Many patients with major abdominal vascular injuries require massive blood transfusions, are hypotensive, and become severely hypothermic, acidotic, and coagulopathic intra operatively. These patients may benefit from early damage control and definitive reconstruction at a later stage when their general condition improves. The patient is returned to the operating room after resuscitation and stabilization for definitive vascular repair and abdominal wall closure.
Epidemiology
The incidence of abdominal major vascular trauma in civilian penetrating injuries is approximately 10% after stab wound to the abdomen and 20% to 30% after a gunshot wound to the abdomen [1]. The incidence of vascular injuries in patients with blunt abdominal trauma undergoing exploratory laparotomy is 3% [2]. Abdominal arterial and venous injuries occur with the same incidence. The most commonly injured abdominal vessel is the inferior vena cava (IVC), accounting for 25% of injuries, followed by the aorta (21%), the iliac arteries (20%), the iliac veins (17%), the superior mesenteric vein (11%), and the superior mesenteric artery (10%). Hospital mortality rates vary from 30% to 80% for abdominal aortic injuries and from 30% to 65% for IVC injuries. Many patients do not reach the hospital alive; dying at the scene or during transport [3]. Death is usually due to exsanguinations, despite aggressive resuscitation and early operation [4].
Surgical Anatomy
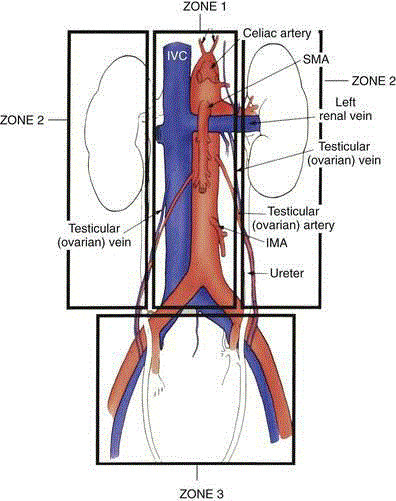
For vascular trauma purposes, the abdomen is conventionally divided into three anatomic areas (Figure 1): Zone 1, which includes the midline retroperitoneum extending from the aortic hiatus to the sacral promontory. The supramesocolic area contains the suprarenal aorta and its major branches (celiac axis, superior mesenteric artery [SMA], and renal arteries), the supramesocolic Inferior Vena Cava (IVC) with its major branches, and the Superior Mesenteric Vein (SMV). The inframesocolic area contains the infrarenal aorta, the Inferior Mesenteric Artery (IMA), the gonadal arteries and IVC. Zone 2 (left and right), which includes the kidneys, paracolic gutter, and renal vessels. Zone 3 which includes the pelvic retroperitoneum and contains the iliac vessels.
Figure 1
Types of Vascular Injuries
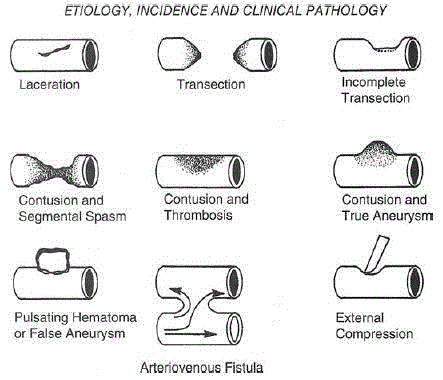
The most common arterial lesions (Figure 2) are partial/ incomplete transection, transection and contusion of the vascular wall. Usually complete transection leads to arterial spasm and thrombosis with subsequent ischemia of the end organ, while partial transection usually causes persistent bleeding or false aneurysm formation. Additionally, partial transection and contusion of the vascular wall may exhibit an intimal flap that may cause vascular thrombosis. Simultaneous arterial and venous lesions can lead to formation of arteriovenous communication.
Clinical Presentation
The clinical presentation depends on the injured vessel, the size and type of the injury, the presence of associated injuries, and time elapsed since the injury. Many patients with major abdominal vascular injuries die at the scene and never reach medical care. Vascular injuries due to blunt trauma are often missed on initial examination or even during the initial hospitalization, unless they are associated with significant bleeding or early ischemic changes. Penetrating injuries to the abdomen associated with hypotension and abdominal distension are highly suggestive of vascular injury [5]. Asymmetric femoral pulses may indicate uni-iliac artery injury. Many patients may be normotensive on admission only to decompensate a few minutes later. Some patients present in a hemodynamically stable condition because of thrombosis of the vessel or tamponade of the bleeding in the retroperitoneum. In most cases the diagnosis is made intra operatively.
Diagnostic Evaluation
The majority of patients presented with penetrating abdominal vascular injury are in critical condition and the need for immediate laparotomy overwhelms further diagnostic investigation. In blunt trauma, radiographic diagnosis of complex pelvic fractures may increase the suspicion of iliac vascular injuries. Computed tomography may play a useful role in blunt trauma by identifying large hematomas, false aneurysms, or vessel occlusions. Digital Subtraction Angiography (DSA) has an important role both in the evaluation of suspected late complications (ex: pseudoaneursym and a-v fistula) and in the evaluation and treatment (embolization) of patients with blunt trauma with pelvic fracture and suspected vascular injury.
Figure 2
Initial Management
In patients with suspected vascular injuries time should not be wasted on fluid resuscitation or diagnostic investigations. Intravenous catheters or central vein catheters should be placed in the upper extremities in case the victim has an injury to the IVC or the iliac veins. The concept of permissive hypotension should be borne in mind, and aggressive fluid resuscitation should not be attempted in the emergency department [6]. Endotracheal intubation should be avoided in the emergency department because rapid-sequence induction is often associated with thrombus dislodgement and increase of the bleeding.
Damage Control Strategy
The surgical team should be ready, and the skin preparation should be performed from the neck to the knees, before induction of anaesthesia because the latter is often associated with rapid hemodynamic decompensation in these patients. The abdomen should be entered through a long midline incision, temporary control of bleeding by direct compression, and aortic cross-clamping, if necessary, at the diaphragm. To facilitate aortic exposure, division of the left crux of the diaphragm may be necessary. With the damage-control approach, all complex venous injuries are ligated, arterial injuries may be shunted, and any diffuse retroperitoneal or parenchymal bleeding is controlled by tight gauze packing [7,8]. The abdomen is closed temporarily with the use of synthetic mesh or vacuum sponge with aspiration and patient is then transferred into the Intensive Care Unit (ICU) for conclusive hemodynamic and coagulation resuscitation, thermal recovery, correction of acidosis and organ malperfusion [9]. Rewarming the patient is a high priority because coagulopathy and acidosis can be corrected and maintained only after the body temperature returns to normal [10,11].
Definitive Surgical Treatment
Twenty four to 72 h may be needed to correct metabolic derangements and after successful stabilization in the ICU the patient is returned to the operating room for definitive surgical treatment. Prior to being taken back to the operating room it is paramount that the resolution of acidosis, hypothermia, and coagulopathy has occurred. Thorough re exploration is made for any additional injuries that may not have been detected in the initial survey and restoration of gastrointestinal continuity and complex vascular repair techniques are done. Not all patients will be able to have their abdomen closed on the first return to the operating room and data suggest that the longer the abdomen is left open from initial laparotomy the higher the rate of complications [12].
Abdominal Compartment Syndrome
Abdominal compartment syndrome is characterized by a tense abdomen, tachycardia, respiratory dysfunction and oliguria. Elevation of the intra-abdominal pressure above 25 cm to 30 cm H2O can cause severe organ dysfunction and result in abdominal compartment syndrome. The intra-abdominal pressure can be measured reliably through the bladder catheter. In general, pressures higher than 30 cm H2O are considered strong indicators for surgical decompression of the abdomen. The abdomen can be opened in the operating room or even in the ICU until the intra-abdominal pressure drops to normal.
Discussion
Damage control strategy represents a surgical emergency approach for the staged management of abdominal vascular trauma in critically wounded patients. The primary goal of this approach is fast control of haemorrhage and prevention of the lethal triad (hypothermia, acidosis and coagulopathy). Damage control is a concept in which the initial surgery becomes part of the resuscitation process rather than part of the curative process. Only when the patient has become physiologically stable is the final therapeutic surgery embarked on and definitive repair with complex vascular anastomosis are undertaken 24hours to 48 hours later. In the last two decades, this approach became part of the gold standard for treatment in critically wounded patients. Multidisciplinary management and perfectly cooperation between doctors of different specialties (ER, Surgeons, Anaesthesiologists and ICU doctors) assures the best optimal outcome.
References
- Asensio JA, Forno W, Petrone P, Rojo E, Tillou A, Murray JA, Feliciano DV, et al. Abdominal vascular injuries: injuries to the aorta. Surg Clin North Am. 2001;81:1395-416.
- Cox EF. Blunt abdominal trauma: A 5-year analysis of 870 patients requiring celiotomy. Ann Surg. 1984;199(4):467-74.
- Coimbra R, Hoyt D, Winchell R, Simons R, Fortlage D, Garcia J. The ongoing challenge of retroperitoneal vascular injuries. Am J Surg. 1996;172(5):541-4.
- Burch JM, Feliciano DV, Mattox KL, Edelman M. Injuries of the inferior vena cava. Am J Surg. 1988;156(6):548-52.
- Gejoe G, Yadev I, Rahul M. Emergency Laparotomies at a Tertiary Care Center-a Hospital-Based Cross-Sectional Study. Indian J Surg. 2017;79(3):206-211.
- Holmes JF, Sakles JC, Lewis G, Wisner DH. Effects of delaying fluid resuscitation on an injury to the systemic arterial vasculature. Acad Emerg Med. 2002;9:267-74.
- Gifford SM, Aidinian G, Clouse WD, Fox CJ, Porras CA, Jones WT, et al. Effect of temporary shunting on extremity vascular injury: an outcome analysis from the Global War on Terror vascular injury initiative. J Vasc Surg. 2009;50(3):549-55.
- Rasmussen TE, Clouse WD, Jenkins DH, Peck MA, Eliason JL, Smith DL. The use of temporary vascular shunts as a damage control adjunct in the management of wartime vascular injury. J Trauma. 2006;61(1):8-12.
- Mohr Alicia M, Asensio Juan A, García-Núñez Luis M, Petrone Patrizio, Sifri Ziad C. Guidelines for the Institution of Damage Control in Trauma Patients, ITACCS. 2005;15(4):185-8.
- Morris JA Jr, Eddy VA, Blinman TA, Rutherford EJ, Sharp KW. The staged celiotomy for trauma. Issues in unpacking and reconstruction. Ann Surg. 1993;217(5):576-84.
- Mikhail J. The trauma triad of death: hypothermia, acidosis, and coagulopathy. AACN Clin Issues. 1999;10(1):85-94.
- Miller RS, Morris JA Jr, Diaz JJ Jr, Herring MB, May AK. Complications after 344 Damage-Control Open Celiotomies. J Trauma. 2005;59(6):1365-71.