Case Report
Disruption of the Staple Line in a Patient wıth Intrathoracic Gastric Conduıt
Mehmet Yildirim*, Savas Yakan, Erkan Oymaci and Hilmi Yazici
Department of General Surgery, University of Health Sciences, Bozyaka Education and Research Hospital, Turkey
*Corresponding author: Mehmet Yildirim, Department of General Surgery, University of Health Sciences, Bozyaka Education and Research Hospital, Izmir, Turkey
Published: 09 Jan, 2018
Cite this article as: Yildirim M, Yakan S, Oymaci E, Yazici
H. Disruption of the Staple Line in
a Patient wıth Intrathoracic Gastric
Conduıt. Clin Surg. 2018; 3: 1851.
Abstract
The treatment of staple line leaks after gastric conduit remains controversial. We present a case of
59-year-old man with distal esophagous cancer. The patient underwent Ivor- Lewis procedure with
gastric conduit. The dehiscence of the staple line occured on the postoperative course. We report
our experience in the management of a patient,and of the various treatment proposals.
Keywords: Esophagogastrectomy; Anastomosis; Gastric conduit
Introduction
Esophagous adenocarcinoma is a highly aggressive nature and has a very poor prognosis [1]. Complete resection of the tumor is the mainstay of treatment. Meanwhile, unlike other gastrointestinal surgical procedures, esophagectomy and reconstruction with gastric conduit is associated with the high morbidity rates. Disruption of the staple line of gastric conduit constitutes one of the most serious condition like mediastinitis. In this study, we present the postoperative course and treatment findings of a case of esophagogastrostomy failure due to staple line dehiscence.
Case Presentation
A 59-year-old man was admitted to the Department of General Surgery with complaints of
dysphagia and retrosternal pain. The patient had no previous history of endoscopic examination of
upper gastrointestinal tract and any other operations. Upper gastrointestinal endoscopy revealed
tumoral mass of the distal thoracic esophagus. Endoscopic biopsy was done. Contrast-enhanced
Computed Tomography (CT) was performed and it revealed a circulated mass with diameter
of 5 cm. Histopathologic examination of biopsy showed adenocarcinoma. Surgery was then
recommended, and the patient underwent subcostal laparotomy and right thoracotomy and partial
esophagogastrectomy with intrathoracic esophagogastric anastomosis (Ivor-Lewis). Reconstruction
was done with the gastric conduit approximately 20 cm in lenght and esophagogastrostomy with 25
mm circular stapler device. The gastric conduit was done based on the great curvature with 7.5 cm
linear cartridges. Microscopically, tumor was the moderately differentiated adenocarcinoma, and
tumor metastasis was found in 13 of the 21 removed lymph nodes.
After an uneventful period of 5 days after surgery metilen blue was administered perorally
to detect any leakage. On the sixth day, peroral feeding was given. On the 10th day, the patient
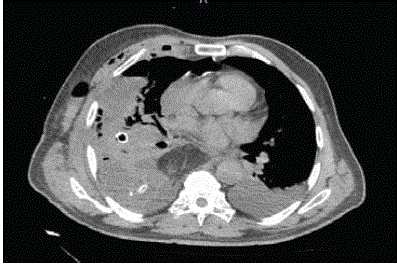
complained of dyspnea and fever, and bilious intestinal fluid was drained through the chest tube. CT
imaging revealed a large pleural fluid collection and pneumonic infiltration of the upper and lower
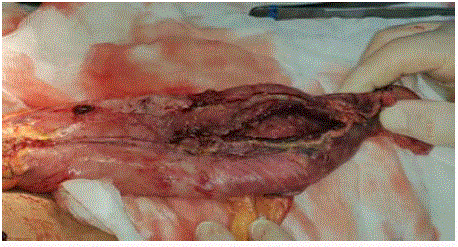
lobe of the right lung (Figure 1). Esophagoscopy was revealed a disruption of the staple line at the gastric conduit nearly 8 cm in lenght. Re-thoracotomy revealed two seperated dehiscence at the gastric staple line 1cm and 8 cm in lenght
(Figure 2). Near total esophagectomy and proximal gastric resection
was done. We performed cervical esophagostomy, tube gastrostomy
to the antrum and chest tube to the right hemithorax. On the second
day of the re-thoracotomy, purulent discharge began from the chest
tube. Three days thereafter, we find dehiscence of thoracotomy
incision. The surgical site was approximated with retention sutures.
Postoperatively, the thorax was continuously flushed with saline via
chest tube. Unfortunately, on the 16th day after the second operation,
the patient died of multiple organ failure.
Figure 1
Figure 2
Discussion
Surgical therapy remains the mainstay for patients with localized adenocarcinomas who are fit for major resection [2]. The surgeon will have to make a choice between performing an intrahoracic versus cervical anastomosis. In general, if the tumor limited to the distal part of esophagus intrathoracic anastomosis is the procedure of choice. There are several reconstructions after distal esophagus resection. Suitability of the stomach as a conduit must be assessed if using the stomach for reconstruction. Currently,anastomotic leak rates continue to be as high as 20%. Especially, intrathoracic anastomoses are a more difficult problem and can lead to mediastinitis and sepsis. Perioperatively, great care is taken to achieve adequate gastric conduit lenght for tension free anastomosis. There is no evidence in either oversewing of the staple line or fibrin application to decrease the disruption. Meanwhile, some surgeons were used omentum flap to reinforcement the anastomosis [3]. A drain placed near the staple line may be useful to detect early leaks. Management depends on clinical presentation and the detection of leakage time. Endoscopic stent placement may be useful in patients with diagnosed early, stable condition without mediastinitis and smaller defects than 2 cm [4]. Surgical approach is indicated in non-stable cases with large defects. Primary repair of the defect is failed because of the friable tissue. Other surgical options are reinforcing flap with adjacent tissues or replacement of gastric conduit to the abdomen and cervical esophagostomy. There is no standardized treatment algorithm for clinicians.
References
- Schaheen L, Blackmon SH, Nason KS. Optimal approach to the management of intra thoracic esophageal leak following esophagectomy: a systemic review. Am J Surg. 2014;208(4):536-43.
- Guo J, Chu X, Liu Y, Zhou N, Ma Y, Liang C. Choice of therapeutic strategies in intra thoracic leak following esophagectomy. World J Surg Oncol. 2014;12:402.
- Zheng QF, Wang JJ, Ying MG, Liu SY. Omentoplasti in preventing anastomotic leakage of oesophagogastrostomy following radical oesophagectomy with three-field lymphadenectomy. Eur J Cardiothorac Surg. 2013;43(2):274-8.
- Dent B, Griffin SM, Jones R, Wahed S, Immanuel A, Hayes N. Management and outcomes of anastomotic leaks after oesophagectomy. Br J Surg. 2016;101(8):1033-8.