Research Article
Cecopexy, a Reemerging Treatment for Cecal Volvulus: Case Report and Systematic Review
Pencle FJR*, Katsichtis T, Schneider J, Strombom PL and Mwesezi SK
Department of Surgery, Lincoln Medical and Mental Health Center, USA
*Corresponding author: Fabio JR Pencle, Department of Surgery, Lincoln Medical and Mental Health Center, Bronx, NY 10451, USA
Published: 20 Dec 2017
Cite this article as: Pencle FJR, Katsichtis T, Schneider J,
Strombom PL, Mwesezi SK. Cecopexy,
a Reemerging Treatment for Cecal
Volvulus: Case Report and Systematic
Review. Clin Surg. 2017; 2: 1838.
Abstract
Background: Cecal volvulus accounts for 25% to 40% of volvulus of the large bowel causing
obstruction with varying degrees of presentation from obstructive symptoms to bowel necrosis
and perforation. In the presence of viable bowel, cecopexy has previously been demonstrated as a
treatment method of surgery. The authors aim to demonstrate the feasibility and reemergence of
cecopexy as a laparoscopic and open technique.
Study Design: We present a case of open cecopexy in a patient with severe hyponatremia with cecal
volvulus and systematic review. A systematic search (January 2017) of PubMed, Scopus, Cochrane
and EMBASE databases was conducted according to the Preferred Reporting Items for Systematic
Reviews and Meta-Analyses (PRISMA) guidelines for literature regarding cecal Volvulus and
cecopexy. Included studies were peer-reviewed articles or academic society publications. Papers
without cecopexy, non-English language, and non-adult cases were excluded.
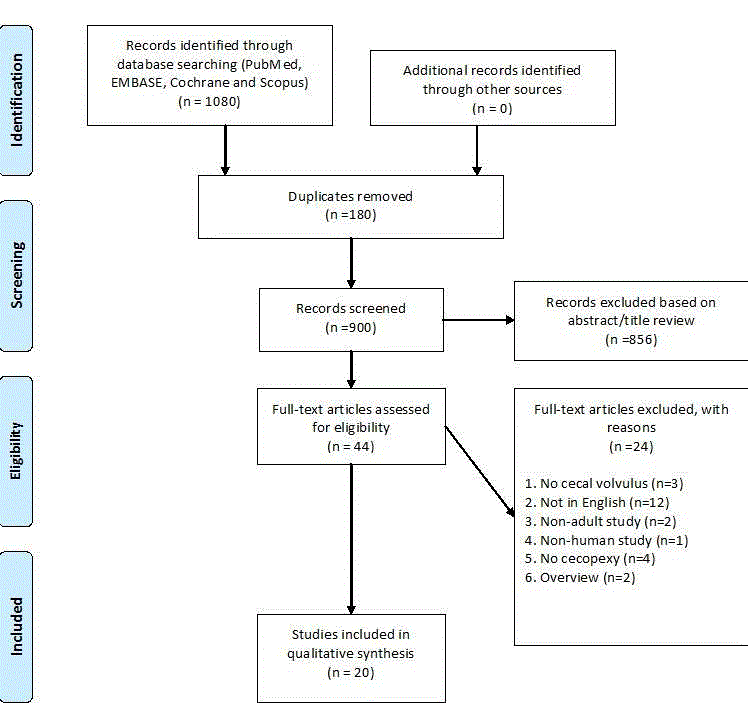
Results: A total of 1080 articles were identified from all four databases through the systematic
search 44 articles were then evaluated for surgical procedure performed; only 20 articles described
Cecopexy. A total of 316 cases were documented for cecal volvulus with a mean age of 51.6 ± 13
years. Further analysis demonstrated 83 cases of resection and 114 cases for cecopexy. Overall
cecopexy recurrence rate was 8.8%.
Conclusion: Operative intervention is the preferred management of cecal volvulus. Cecopexy
can be performed in patients who have viable bowel and require further resuscitation. This can
be performed either via open or laparoscopic approach. Patient with non-viable bowel require
resection with either primary anastomosis or colostomy.
Keywords: Cecopexy; Cecal volvulus; Cecal bascule; Literature review; Beer potomania;
Hyponatremia
Introduction
Cecal volvulus causes approximately 1-3 percent of all large bowel obstructions. It is defined as the rotation or torsion of a flexible cecum and ascending colon around its mesentery [1-3]. Patients most commonly present with acute obstructive symptoms and signs, including nausea, vomiting, and abdominal pain and distension [2,4-6]. It frequently progresses to bowel obstruction, ischemia, necrosis, and perforation [7]. Initial imaging evaluation with plain abdominal X-rays can demonstrate dilated colon usually pointing to the direction of the spleen. CT Abdomen and Pelvis (CTAP) should be performed in patients without signs of perforation or peritonitis. This allows for localization of the level of obstruction. There are three types of cecal volvulus commonly described based on position and rotation around the mesentery [4,8-11]. Type 1 - An axial volvulus develops from clockwise axial torsion or twisting of the cecum along its long axis; the volvulized cecum remains in the right lower quadrant. Type II - A loop cecal volvulus develops from torsion or twisting of the cecum and a portion of the terminal ileum, resulting in the cecum being relocated to an ectopic location (typically left upper quadrant) in an inverted orientation. Most, but not all, type II cecal volvuli have a counterclockwise twist [10]. Type III - Cecal bascule involves the upward folding of the cecum rather than an axial twisting. Torsion-type cecal volvuli (types I and II) are more common, accounting for approximately 80 percent of all cecal volvuli [10]. Cecal bascules (type III) account for the remaining 20 percent. The treatment algorithm of cecal volvulus is based on bowel compromise and hemodynamic stability [12-14]. If gangrenous bowel is present this should not be untwisted to reduce risk of septic shock [14]. The standard of treatment involves surgical resection and primary anastomosis based on decreased complication rates and no recurrence of volvulus [14]. Improved perioperative management may reduce complications in patients presenting with viable bowel and change this notion. The authors aim to perform a review of the literature to evaluate the feasibility, reemergence and rationale for performing cecopexy in patient with viable bowel based on a recent case of cecal volvulus.
Figure 1
Figure 2
Methods
Case report
A 71 year old male with medical history of diabetes, hypertension
and alcohol abuse presented to the ED with a five day history of
increasing abdominal girth, passing flatus intermittently and was
able to tolerate clear liquids prior to presentation. Other symptoms
included cough, and subjective fevers x 4 days, watery emesis for 3
days, and no bowel movement or flatus on the day of presentation.
Patient endorses drinking 6-8 beers per day but denies smoking
or illicit drug use. In the emergency room patient was a febrile (T:
98.5F), with a heart rate of 84bpm and mildly hypertensive to 167/87
mmHg. Physical examination demonstrated a soft, mildly distended
abdomen with mild tenderness, without masses or guarding. Rectal
examination revealed no masses, no blood, and an empty vault.
Blood tests were within normal ranges except for sodium of 114
mEQ/l, lactate 3. 0 mmol/L and serum osmolality of 229 mOsm/
kg. An abdominal plain film was performed, which demonstrated
excessively distended cecum. These findings were confirmed with
CTAP demonstrating cecal volvulus (Figures 1A-1C). Resuscitation
was started preoperatively in the emergency room with bolus normal
saline and patient taken emergently to operating room (OR). On
exploratory laparotomy via a midline incision, all bowels were viable.
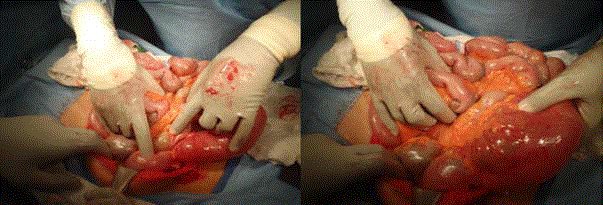
The cecum was identified as a midline structure and was found to
be volvulized, with small intestine in the right lower quadrant
(Figures 2A and 2B). The cecum was untwisted and inspected;
there was a 1.5 cm serosal tear on the anterior mesenteric border,
but no full thickness injuries were identified. The cecum was placed
back in its normal anatomic position in the right lower quadrant. A
cecopexy was performed using 2-0 Vicryl sutures to approximate
epiploic appendages to the lateral abdominal wall to secure the
cecum in place and prevent future volvulus. Postoperatively patient
transferred to Surgical Intensive Care Unit (SICU) intubated and
further resuscitated with repeat sodium of 127 mEQ/L. The patient
was extubated on Post Op Day (POD) 1 and transferred to floor with
NGT. Patient received IVF at 84ml/hr normal saline and clear liquid
diet started on POD 2 with addition of salt tabs. The patient recovered
uneventfully and was discharged POD 9 with resolving hyponatremia
(Na 135 mEQ/L). Patient has had no evidence of recurrence after 6
months and continues to follow up.
Study design and search strategy
An initial search of the international prospective database of
systematic reviews (PROSPERO) revealed no ongoing or published
systematic reviews assessing cecal volvulus or cecopexy protocols.
According to the Preferred Reporting Items for Systematic Reviews
and Meta-Analyses (PRISMA) guidelines, a systematic review of
PubMed, Scopus, Cochrane database and EMBASE was performed on
January 5, 2017. The employed search strategy including all Medical
Subject Heading (MeSH) terms consisted of the following: (“Cecal
volvulus” OR “Cecal bascule”) AND (“cecopexy”). Filters were then
applied to select for English language papers. To identify additional
citations missed by electronic searches, references of included studies
were checked manually.
Inclusion and exclusion criteria
All studies, published up to January 5th, 2017, evaluating cecal
volvulus and cecopexy were included. The add-on requirements had
been: Case studies; Literature review. Studies were then analyzed to
determine if there was cecopexy performed for cecal volvulus.
Study selection
Two authors (FJRP and PS) individually reviewed the papers,
assessed the study quality, with confirmation of cecopexy performed
for cecal volvulus, and cross-checked after initial review. Any
difference of opinion within the two reviewers’ data collection was
reviewed until a general opinion was attained; if agreement could
not be reached a third independent author (SK) was included in the
dialogue as a final referee. The details of the final studies included the
authors, publication year of the research and journal (Table 1).
Statistical analysis
Statistical analysis was performed using SPSS v22 (IBM
corporation, New York, USA). An independent sample student
T-test was used to compare groups for continuous data and chisquared
used for categorical data. Continuous data comparisons
were expressed as means with standard error. Tests were considered
significant if p< 0.05.
Figure 3
Figure 4
Table 1
Results
A total of 1080 articles were identified from all four databases
through the systematic search. After removing the duplicates, the
title and abstract of 900 references were screened for meeting the inclusion criteria. A total of 62 articles were found with a combination
of keywords “Cecal volvulus” or “cecal bascule” and “Cecopexy”.
Using the inclusion criteria of keywords and English full text articles
44 articles remained. No additional studies were obtained following a
manual reference list search of included studies. The 44 articles were
then evaluated for surgical procedure performed; only 20 articles
described Cecopexy depicts the systematic analysis to achieve the final
twenty studies for synthesis in the PRISMA flow diagram (Figure 3).
Analysis of final studies
Further analysis of age, total cases, number of cases with resection
and cecopexy with number of recurrences is tabulated in (Table 2).
Of the 20 articles [6,15-33], a total of 316 cases were documented for
cecal volvulus with a mean age of 51.6 ± 13 years. Further analysis
demonstrated 83 cases of resection and 114 cases for cecopexy.
There were a total of 10 recurrences in cecopexy group with an
overall recurrence rate of 8.8%. Overall mortality range in all studies was 9% to 19%. Table 3 demonstrates mortality by procedure with
higher mortality in cases when appendectomy was performed and
ileocolectomy.
Table 2
Table 3
Discussion
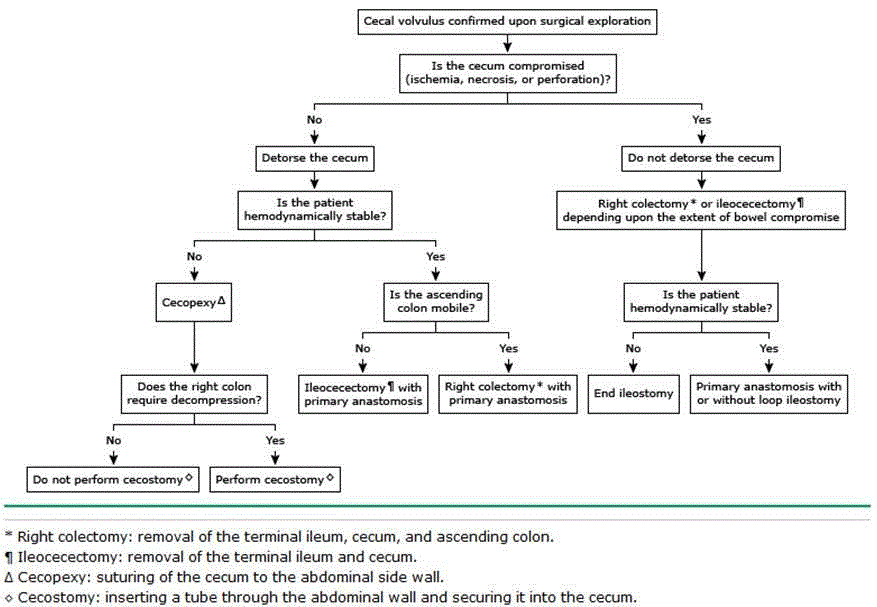
This study aimed to review the available literature to assess the feasibility and reemergence of cecopexy for cecal volvulus base on a recent case at performed. The case demonstrates a patient who presented with severe hyponatremia which can be a combination of malnutrition or intoxication both due to alcoholism. Malnutrition described primarily in beer drinkers (hence called beer potomania or beer drinkers’ potomania), leads to low dietary solute intake. Presentation is usually of hyponatremia and low osmolality with decreased solute excretion and dilute urine [34]. Management goals include increasing serum sodium < 10 mEQ/L in first 24 hr and increasing serum sodium by < 18 mEQ/L in first 48 hr. This should be performed in an intensive care unit with judicial monitoring of fluid intake and serial serum sodium levels [34]. The case was also complicated with the presence of cecal volvulus, management of which is primarily surgical [14,35]. There is an increased risk of complications with non operative management with a less than five percent (< 5%) success rate [12-14,35]. Review of the literature reveal two major options for viable bowel in cecal volvulus. These are cecopexy in cases of hemodynamic instability or resection and primary anastomosis in cases of hemodynamic stability. Treatment algorithm for cecal volvulus is illustrated in (Figure 4) [36]. A review of the major reports relating to choice of operation follows. Looking at early literature, Todd et al. [19] assessed recurrence rate of several prior studies comparing patients who had resection, cecostomy, cecopexy and detorsion [19]. The overall recurrence of cecopexy is noted to be 6.9% (8/116), and there was no noted recurrence in their series of patients. There were no recurrences with resection or tube cecostomy. They concluded no evidence to support resection was associated with lower recurrence than tube cecostomy. A larger study Ballantyne et al. [6] a total of 71 patients was noted to have cecal volvulus [6]. Further subdivisions of two groups were created, patients with cecal fold volvulus or full cecal volvulus. There were no recurrences noted in patients who underwent procedure of cecopexy (N=12) or resection and primary anastomosis (N=35) or resection and stoma (N=4). Mortality was higher in patients with gangrenous bowel 33% vs. 12% in patients with viable bowel. Although no definitive conclusion was stated from this study for cecal volvulus. Cecopexy showed no recurrence and one mortality which were comparable to resection group of a total of 39 patients with no recurrence and 6 cases of mortality [6]. Konvolinka et al. [23] reported on a case with previous left hemicolectomy, complicated with cecal volvulus. Cecopexy was the preferred treatment to preserve colonic function as significant portion of the left colon had previously been resected [23]. More recent literature has shown several laparoscopic case studies demonstrating the use of minimally invasive technique as both diagnostic and therapeutic. The earliest of which was by Shoop et al. [22] which demonstrated the feasibility of the procedure however had no follow up on recurrence. Ortega et al. [29] reported on a 36 year old who presented with cecal volvulus and pneumatosis intestinalis, with no recurrence after one year follow up and resolution of symptoms. The most recent case series noted in this review was conducted by Ishida et al. [33] In 2016. They reported to three cases of cecal bascule after spinal cord injury. The longest follow up was fifteen months with no recurrences. Case 1 and 2 both had cecopexy with case 2 additionally having a cecostomy tube placed. Case 3 had right hemicolectomy and ileocolonic anastomosis. There were no mortalities stated however case 2 was complicated by return to hospital for tube dislodgement requiring replacement. They concluded that right hemicolectomy is the preferred surgical treatment, where as cecopexy is also an acceptable treatment option if hardware is inserted.
Study Limitations
This manuscript is subject to bias in study selection as the included databases, search terms, and inclusion and exclusion criteria may not have retrieved an exhaustive list of existing literature of cecopexy and cecal volvulus or bascule. For example, exclusion of studies in which cecopexy was performed after cases of appendicitis were excluded. However, attempts at maintaining broad search terms and utilizing multiple databases, including EMBASE which contains citations from an extended list of European and Asian journals, were made to facilitate widespread literature study retrieval. Moreover, while the search was systematic, final analysis and summarization of steps for the examination protocol was based on the authors’ experience and clinical expertise. Analysis was also based on available documentation which was limited to several case studies and case series. No level II or higher studies were noted due to the severity of disease process. The authors also aimed to compare cecopexy to cases of resection as demonstrated to be the preferred modes of therapy.
Conclusion
The recommendations based on this study include early resuscitation with appropriate imaging preoperatively. Operative intervention is the preferred management of cecal volvulus. In the setting of bowel compromise resection with either primary anastomosis or end ileostomy should be performed. Cecopexy can be performed in patients who have viable bowel and require further resuscitation due to level of instability. This can be performed either via open or laparoscopic approach. Special considerations should include patients with previous resections as well. The case presented demonstrates a patient who is hemodynamically stable however due to the level of hyponatremia in the setting of chronic alcohol use and malnutrition could be managed with a cecopexy as the procedure is shorter and patient required further resuscitation in the intensive care unit.
References
- Beck DE, Roberts PL, Saclarides TJ, Senagore AJ, Stamos MJ, Nasseri, et al. Colonic volvulus. The ASCRS textbook of colon and rectal surgery. Beck DE RP, Saclarides TJ, editors. New York: Springer. 2011.
- Lee SY, Bhaduri M. Cecal volvulus. CMAJ: Canadian Medical Association journal = journal de l'Association medicale canadienne. 2013;185(8):684.
- Baldarelli M, De Sanctis A, Sarnari J, Nisi M, Rimini M, Guerrieri M. Laparoscopic cecopexy for cecal volvulus after laparoscopy. Case report and a review of the literature. Minerva Chir. 2007;62(3):201-4.
- Katoh T, Shigemori T, Fukaya R, Suzuki H. Cecal volvulus: report of a case and review of Japanese literature. World J Gastroenterol. 2009;15(20):2547-9.
- Swenson BR, Kwaan MR, Burkart NE, Wang Y, Madoff RD, Rothenberger DA, et al. Colonic volvulus: presentation and management in metropolitan Minnesota, United States. Diseases of the colon and rectum. 2012;55(4):444-9.
- Ballantyne GH, Brandner MD, Beart RW Jr, Ilstrup DM. Volvulus of the colon. Incidence and mortality. Ann Surg. 1985;202(1):83-92.
- Habre J, Sautot-Vial N, Marcotte C, Benchimol D. Caecal volvulus. Am J Surg. 2008;196(5):e48-9.
- Pousada L. Cecal bascule: an overlooked diagnosis in the elderly. J Am Geriatr Soc. 1992;40(1):65-7.
- Consorti ET, Liu TH. Diagnosis and treatment of caecal volvulus. Postgraduate medical journal. 2005;81(962):772-6.
- Delabrousse E, Sarliève P, Sailley N, Aubry S, Kastler BA. Cecal volvulus: CT findings and correlation with pathophysiology. Emerg Radiol. 2007;14(6):411-5.
- Perret RS, Kunberger LE. Case 4: Cecal volvulus. AJR American journal of roentgenology. 1998;171(3):855.
- Rabinovici R, Simansky DA, Kaplan O, Mavor E, Manny J. Cecal volvulus. Dis Colon Rectum. 1990;33(9):765-9.
- Madiba TE, Thomson SR. The management of cecal volvulus. Dis Colon Rectum. 2002;45(2):264-7.
- Gingold D, Murrell Z. Management of colonic volvulus. Clin Colon Rectal Surg. 2012;25(4):236-44.
- Meyers JR, Heifetz CJ, Baue AE. Cecal volvulus: a lesion requiring resection. Arch Surg. 1972;104(4):594-9.
- Smith WR, Goodwin JN. Cecal volvulus. Am J Surg. 1973;126(2):215-22.
- Andersson A, Bergdahl L, Linden W. Volvulus of the cecum. Ann Surg. 1975;181(6):876-80.
- O'Mara CS, Wilson TH Jr, Stonesifer GL, Stonesifer GL, Cameron JL. Cecal volvulus: analysis of 50 patients with long-term follow-up. Ann Surg. 1979;189(6):724-31.
- Todd GJ, Forde KA. Volvulus of the cecum: choice of operation. Am J Surg. 1979;138(5):632-4.
- Anderson JR, Welch GH. Acute volvulus of the right colon: an analysis of 69 patients. World J Surg. 1986;10(2):336-42.
- Wright TP, Max MH. Cecal volvulus: review of 12 cases. South Med J. 1988;81(10):1233-5.
- Shoop SA, Sackier JM. Laparoscopic cecopexy for cecal volvulus. Case report and a review of the literature. Surg Endosc. 1993;7(5):450-4.
- Konvolinka CW, Moore RA, Bajwa K. Cecal volvulus causing postoperative intestinal obstruction: report of a case. Diseases of the colon and rectum. 2001;44(6):893-5.
- Tsushimi T, Kurazumi H, Takemoto Y, Oka K, Inokuchi T, Seyama A, et al. Laparoscopic cecopexy for mobile cecum syndrome manifesting as cecal volvulus: report of a case. Surgery Today. 2008;38(4):359-62.
- Makama JG, Ahmed A, Ukwenya Y, Mohammed I. Mobile caecum and ascending colon syndrome in a Nigerian adult. Ann Afr Med. 2009;8(2):133-5.
- Batista TP, Rolim JC, Gomes AA, Carvalho WL, Santos RJ. Cecum volvulus complicated by septic jaundice. Rev Col Bras Cir. 2010;37(6):460-2.
- Arulmolichelvan A, Sivaraman A, Muthukrishnan A. Cecal volvulus associated with intestinal malrotation presenting as postoperative intestinal obstruction. Medical principles and practice : international journal of the Kuwait University, Health Science Centre. 2012;21(4):389-91.
- Jones RG, Wayne EJ, Kehdy FJ. Laparoscopic detorsion and cecopexy for treatment of cecal volvulus. The American surgeon. 2012;78(5):E251-2.
- Ortega PM, Rotellar F, Arredondo J, Baixauli J, Zozaya-Larequi FJ, Betes M, et al. Minimal invasive management of acute cecal volvulus: colonoscopy followed by laparoscopic cecopexy. Revista espanola de enfermedades digestivas : organo oficial de la Sociedad Espanola de Patologia Digestiva. 2014;106(7):497-9.
- Makarawo T, Macedo FI, Jacobs MJ. Cecal bascule herniation into the lesser sac. World J Clin Cases. 2014;2(12):903-6.
- Sujka J, Teixeira AF, Jawad MA. Suspected cecal volvulus as a reason for abdominal pain after gastric bypass: a case series. Surg Obes Relat Dis. 2015;11(4):978-9.
- Chaudry TH, Jamil M, Niaz K, Basher G. Acute caecal volvulus: A diagnostic paradigm. J Pak Med Assoc. 2015;65(12):1357-9.
- Ishida Y, McLean SF, Tyroch AH. Cecal bascule after spinal cord injury: A case series report. Int J Surg Case Rep. 2016;22:94-7.
- Kujubu DA, Khosraviani A. Beer Potomania--An Unusual Cause of Hyponatremia. Perm J. 2015;19(3):74-6.
- Halabi WJ, Jafari MD, Kang CY, Nguyen VQ, Carmichael JC, Mills S, et al. Colonic volvulus in the United States: trends, outcomes, and predictors of mortality. Ann Surg. 2014;259(2):293-301.
- Surgery for cecal volvulus. Up To Date. 2017.