Clinical Image
Pericardial Abscess in a Cardiac Transplant Patient
Thomas Trobiano, Van-Khue Ton and Erika Feller*
Department of Medicine, Division of Cardiology, University of Maryland Medical Center, USA
*Corresponding author: Erika Feller, University of Maryland Medical Center, Baltimore, Maryland, USA
Published: 13 Dec, 2017
Cite this article as: Trobiano T, Ton V-K, Feller E.
Pericardial Abscess in a Cardiac
Transplant Patient. Clin Surg. 2017; 2:
1815.
Clinical Image
Mediastinitis in immunocompromised patients may present with subtle signs and symptoms.
A 49-year-old woman with a history of post-partum dilated cardio myopathy, paroxysmal a trial
fibrillation, and got presented with acute on chronic decompensated heart failure in 7/2016. She
underwent heart transplantation 8/2016. Her post-operative course was complicated by delayed
chest closure, right ventricular dysfunction requiring prolonged inotropic support, and acute
kidney injury necessitating continuous renal replacement therapy (CRRT). Hemodynamics by right
heart catheterization showed restrictive filling patterns.
Approximately 3 months post heart transplantation, the patient complained of right flank pain
without a clear cause by imaging studies. She proceeded to exhibit malodorous, purulent drainage
from an old mediastinal chest tube site, without frank fever, chills or leukocytosis. The fluid culture
grew Morganella morganii. A computed tomography (CT) scan of the chest showed multiple
loculated pericardial fluid collections along the inferior surface of the heart (Figures 1 and 2). The
patient was urgently taken to the operating room for a pericardial window with drainage of copious
amounts of purulent fluid. There was an old fibrinous clot which was shaggily adherent to the heart
and to the diaphragmatic surface. Transthoracic echo showed the supradiaphragmatic space seemed
to be retarding right ventricular filling. In addition to receiving intravenous antibiotics, the patient
endured approximately 20 washout and debridement while the pericardial sac was irrigated with
antibiotic solution.
In conclusion, we would like to alert clinicians to consider Morganella morganii as a potentially
fatal pathogen in those who are immunocompromised [1,2]. To date, there have been four articles
published in reference to pericarditis caused by Morganella morganii. Three of the four cases reported
were found among immunocompromised individuals [1]. Generally not prone to causing harm in the immunocompetent population, Morganella morganii is typically
found within the urinary tract and normal flora of the intestine [2]. It
is important to have a high index of suspicion as immunosuppression
may mask hallmark symptomatology of mediastinitis. Timely CT
imaging is essential when evaluating for mediastinitis. Source control
with antibiotic coverage and recurrent washouts and debridement are
the mainstay interventions in managing this deadly gram-negative
bacterium. Thus far this patient has remained in stable condition
without recurrent evidence of infection.
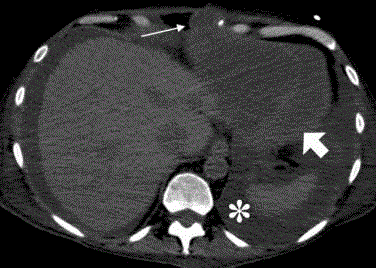
Figure 1
Figure 1
Axial non-contrast CT of the chest demonstrates a loculated pericardial effusion (fat arrow) with
thickening of the pericardium and septations within the pericardial space. Relative increased density of
pericardial fluid compared to pleural effusion (asterisk) suggests the collection is exudative in composition. There
is extension of the collection into the anterior chest wall (thin arrow).
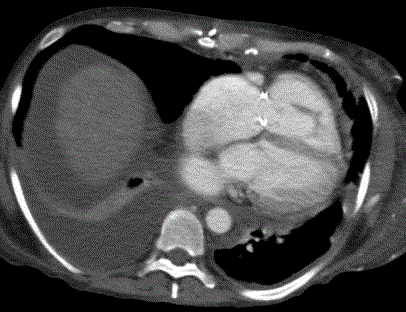
Figure 2
Figure 2
Contrast enhanced CT of the chest 3 months after therapy demonstrates complete resolution of the
pericardial effusion..
References
- Nakao T, Yoshida M, Kanashima H, Yamanae T. Morganella morganii pericarditis in a patient with multiple myeloma. Case Rep Hematol. 2013;1-3.
- Yang ZT, Lecuit M, Suarez F, Carbonelle E, Viard JP, Dupont B, et al. Morganella morganii pericarditis 3 years after allogenic bone marrow transplantation for mantle cell lymphoma. J Infection. 2006;1-3.