Case Report
Pediatric Nodular Fasciitis: Case Series Report
Kondjela Sara Hamunyela1*, Daniel Sidler1, Puleinge Ihuhua2 and Pawel T Schubert3
1Department of Pediatric Surgery, University of Stellenbosch, Tygerberg Children’s Hospital, Cape Town, South
Africa
2Department of Radiology, University of Stellenbosch, Tygerberg Children’s Hospital, Cape Town, South Africa
3Department of Pathology, University of Stellenbosch, Tygerberg Children’s Hospital, Cape Town, South Africa
*Corresponding author: Kondjela Sara Hamunyela, Department of Pediatric Surgery, University of Stellenbosch, Tygerberg Children’s Hospital, Cape Town, South Africa
Published: 20 Nov, 2017
Cite this article as: Hamunyela KS, Sidler D, Ihuhua
P, Schubert PT. Pediatric Nodular
Fasciitis: Case Series Report. Clin
Surg. 2017; 2: 1745.
Abstract
We like to report on two paediatric cases presenting with Nodular Fasciitis. Both were rapid growing soft tissue masses excised between Jan 2016 to Dec 201. After surgical excision they were followed up in outpatient, we would like to describe the histological evaluation and management of these cases. Keywords: Nodular Fasciitis; Inflammation; Sarcoma
Introduction
Nodular Fasciitis (NF) is a rare benign soft tissue tumor more commonly seen in the adult, compared to the pediatric population. It is often mistaken as a malignant soft tissue sarcoma. Benign histology changes the course of management strategy to less aggressive therapy. Our institution reports two pediatric cases of NF, presenting with a soft tissue mass clinically thought to be a soft tissue sarcoma.
Case Series
Case presentation 1
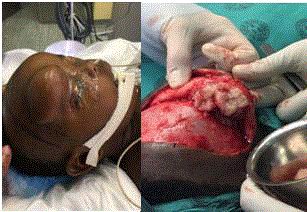
One year old girl presented, with 3 month history of fast growing mass on the forehead. Two days
prior to the onset of growth there was history of blunt trauma to the forehead. The child was born at
term, and past medical history was unremarkable. Clinically the mass had a smooth surface, mobile
and not fixed to the underlying skull. No audible bruit was present. Neurological examination was
normal. The ultrasound showed a complex predominantly solid mass with cystic components and
micro-calcifications. Doppler ultrasound revealed moderate vascularity with arterial waveform in
the solid component. MRI scan showed right lateral supraorbital mass measuring 39 mm x 46 mm
x 23 mm. The mass was superficial to the skull, preseptal and not involving the orbital structures.
Surgical excision was performed. A wide coronal incision was made 2 cm behind the
hairline,dissected to the subgaleal fascia plain avoiding the temporal branch of the facial nerve
(Figure 1), and supraorbital nerve. The lesion was adherent to the frontalis muscle posteriorly and
tempero-pariatal fascia. There was no definitive capsule and therefore the lesion was excised in
pieces rather than intact. The specimen was submitted for urgent histological evaluation.
Case presentation 2
10 year old girl of mixed race, presented with a one month history of a progressive enlarging
non-painful mass on the left anterior chest wall. There was no preceding history of trauma prior to
presentation. Anatomically the mass was located at the fourth intercostal space, mid clavicular line.
It was mobile, not adherent to any surrounding structures, no audible bruit was detected. Chest
x-ray was normal. The mass was surgically excised one week after presentation. No imaging was
done prior because of its small size. The patients were followed up at 2 weeks and 3 months post
operatively (Figure 2), no complications or recurrence occurred.
Histology
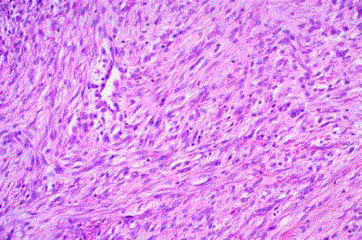
Microscopic sections show a tumor comprising plump myofibroblastic cells growing in a vaguely
storiform pattern. These cells had vesicular nuclei with small nucleoli and basophilic to eosinophilic
cytoplasm. Mitotic activity was present. Randomly arranged within the tumor were collagen fibers
and osteoclast-like giant cells (Figure 3). Myxoid foci were prominent in some areas. The lesion was
seen infiltrating peripheral soft tissues. Immunohistochemical stains showed positive staining for
smooth muscle actin, which appear very different to a malignant lesion (Figure 4). Desmin, CD10,
CD34 and S100 were negative. NF was extending to the excision margin.
Figure 1
Figure 2
Figure 3
Figure 4
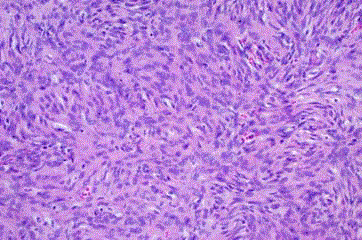
Figure 4
For comparison, a malignant peripheral nerve sheath tumor,
showing a much more cellular neoplasm. H&E stain at 200x.
Discussion
Nodular fasciitis is a rare benign lesion, consisting of proliferating fibroblasts. It is usually in the deep fascia in the head and neck areas, its rapid growth can be deceptively similar to that of soft-tissue sarcomas [1-5]. Approximately 10% of all known cases are found in children. Male to female ratio is equal. The lesion is an idiopathic self-limiting reactive process of unknown etiology. The lesion is described as being a trauma-related phenomenon. Differential diagnosis consists of solid malignancies: rhabdomyosarcoma, neuroblastoma, osteosarcoma, neurofibroma, lymphoma and cysts/abscess. Clinically it presents as a progressively enlarging painless solid mass. The clinical symptoms are non-specific and do not help with the pre-operative diagnosis. Impingement of the surrounding structures can produce pain or other symptoms. Constitutional symptoms such as fever and weight loss are rare. Microscopic evaluation shows discrete and nodular hypercellular growth of fibroblasts and myofibroblasts centered in the tissue. Prominent mitotic activity, areas rich in ground substance with myxoid and microcystic change, and extravasated erythrocytes and inflammatory cells are often present. These characteristics is the classical description of NF. Radiological imaging includes sonar, CT or MRI. Ultrasound helps in differentiating solid tumors from cystic lesions, specifically vascular malformations and post-traumatic false aneurysms. MRI is the imaging modality of choice because it helps to define the lesion in relation to surrounding vital structures, to map surgical approach and detect associated bone remodeling or destruction. The signal characteristics are variable depending on the histological components. Cellular lesions show T1 hyperintensity and T2 hyperintensity due to the myxoid component, whereas more collagenous tumors are hypointense on both sequences. The mass typically enhances diffusely on T1 post-contrast sequences [6-8]. Complete surgical excision is the definitive treatment. The lesion is usually unencapsulated. Observation or partial resection may be considered in special cases. The condition is a self-limiting process with a low recurrence rate. The effectiveness of use of steroids in NF is not known. Cranial fasciitis is a histologically similar condition to nodular fasciitis with involvement of the outer table of the skull bone. One report advocates local intra-lesional injection in this subtype of NF should it recur.
References
- Hseu A, Watters K, Perez-Atayde A, Silvera VM, Rahbar R. Pediatric nodular fasciitis in the head and neck: evaluation and management. JAMA Otolaryngol Head Neck Surg. 2015;141(1):54-9.
- Spunt SL, Skapek SX, Coffin CM. Pediatric nonrhabdomyosarcoma soft tissue sarcomas. Oncologist. 2008;13(6):668-78.
- Boffano P, Campisi P, Forni P, Ramieri G, Berrone S. Nodular fasciitis in the maxillary region. J Craniofac Surg. 2012;23(6):e558-60.
- Pandian TK, Zeidan MM, Ibrahim KA, Moir CR, Ishitani MB, Zarroug AE. Nodular fasciitis in the pediatric population: a single center experience. J Pediatr Surg. 2013;48(7):1486-9.
- Tomita S, Thompson K, Carver T, Vazquez WD. Nodular fasciitis: a sarcomatous impersonator. J Pediatr Surg. 2009;44(5):e17-9.
- Lee JY, Kim YC, Shin JH. Cranial fasciitis treated with intralesional corticosteroids. Int J Dermatol. 2004;43(6):453-5.
- Adam A, Dixon A, Gillard J, Schaefer-Prokop C, Grainger RG. Grainger & Allison's Diagnostic Radiology: A Textbook of Medical Imaging. 6th ed. New York: Churchill Livingstone Elsevier. 2015;Chapter 49:1138-9.
- Kim ST, Kim HJ, Park SW, Baek CH, Byun HS, Kim YM. Nodular fasciitis in the head and neck: CT and MR imaging findings. AJNR Am J Neuroradiol. 2005;26(10):2617-23.