Short Communication
Hybrid Revascularization in the Treatment of Aorto Iliac and Femoral Occlusive Disease
Pulli Raffaele*, Marinazzo Davide, Wiesel Paola, D’Elia Simona and Angiletta Domenico
Department of Vascular and Endovascular Surgery, University of Bari, Italy
*Corresponding author: Pulli Raffaele, Department of Vascular and Endovascular Surgery, University of Bari, Italy
Published: 03 Nov, 2017
Cite this article as: Raffaele P, Davide M, Paola W,
D’Elia Simona, Domenico A. Hybrid
Revascularization in the Treatment
of Aorto Iliac and Femoral Occlusive
Disease. Clin Surg. 2017; 2: 1717.
Short Communication
Endovascular procedures have been widely growing in recent years and, in spite of the actual
indications of the international society guidelines, have become the first choice also for aortoiliac
TASC II C/D lesions because of excellent results in terms of low perioperative mortality and
morbidity rates and of good long-term primary and secondary patency [1,2].
In patients with critical limb ischemia due to severe iliac and femoral occlusive disease hybrid
interventions have emerged as a common method of revascularization. In particular patients with
multilevel occlusive disease and high surgical risk may benefit from a minimally invasive combine
surgical and endovascular approach. In these cases femoral endarterectomy alone would be an
inadequate procedure and would have a high risk of acute thrombosis due to poor inflow. Also,
isolated endovascular aortoiliac revascularization may have a poor outcome in term of patency in
the presence of critical common or bifurcation femoral artery occlusive disease.
On the other hand, a relatively low-risk common femoral endarterectomy followed by aortoiliac
stenting may restore both inflow and outflow at multiple levels, maintaining favorable patency and
limb salvage rates without the need for a complex open surgical procedure (Figure 1-4).
Typically the surgical reconstruction is the first step. The ipsilateral femoral bifurcation is
exposed via a longitudinal incision in the groin. The common femoral artery is opened through
a longitudinal arteriotomy and endarterectomy is performed to remove the occluding plaque.
Reconstruction of the common femoral artery and bifurcation is usually completed using a patch
(autogenous saphenous vein, synthetic or biologic material) or an interposition synthetic graft,
depending on the length of the treated segment.
An appropriate vascular access is imperative to proceed to a successful endovascular aortoiliac
recanalization. Depending on the anatomy and the extent of disease, access options most commonly
include a combination of left brachial and bilateral femoral arterial access. Left brachial access can
be used as a primary access site for treatment or as a supplement to femoral access. The femoral
artery sheath, usually 8 Fr, is positioned in the reconstructed artery through direct puncture of
the patch. Firstly, an aortogram via a contralateral crossover approach is obtained in the distal
aorta. Once the ipsilateral common, external, and internal iliac arteries are assessed, a catheter is
advanced across the aortic carrefour through the contralateral iliac axis in an antegrade fashion and positioned with its tip proximal to the target lesion. Whenever possible, direct retrograde ipsilateral approach was used through the
reconstructed femoral artery. Alternatively, the left brachial approach
with an anterograde recanalization from the above provides a
better pushability in complex lesions involving the distal aorta. The
simplest method of recanalization consists in the use of a hydrophilic
guidewire with a support catheter into intraluminal or subintimal
space. In case of subintimal recanalization the confirmation of reentry
into the true lumen is mandatory before placing a stiff wire in
the iliac axis for subsequent stenting. If the disease extends into the
distal external iliac artery, stents in our opinion should be positioned
up to the proximal portion of the patch, ideally without extension
into the common femoral artery.
As regard the choice of the stent, emerging reports are
demonstrating the non-inferiority and potential advantages of
covered stents compared to bare metal stents in the treatment of
aortoiliac occlusive disease. The COBEST trial [3] outlines the benefits
of stent graft use in the aortoiliac district because these lesions are
sometimes very tough to cross and there is always an imminent
risk of intraprocedural complications like flow limiting dissection,
perforation or embolization. The use of covered stents allows to
prevent these complications. In case of bilateral iliac axis occlusive
disease, covered stent-grafts are usually placed in a “kissing-stent”
configuration and simultaneously inflated.
In the last years different solutions of hybrid revascularization
are emerging. Covered Endovascular Reconstruction of Aortic
Bifurcation (CERAB technique [4]) is a new approach for extensive aortoiliac occlusive disease using three covered balloon expandable
stents to reconstruct the aortic bifurcation. This configuration
simulates a neo-bifurcation avoiding hemodynamic and pathological
changes in combination with the benefits of covered stents. The
aortoiliac bifurcation can also be reconstructed using the AFX
unibody aortoiliac stent-graft [5], originally designed for aneurysm
exclusion, via an open femoral artery approach. This technique has
several potential advantages, preserving the aortic bifurcation and
avoiding limb competition in the distal aorta. It also allows for future
endovascular interventions and protects against potentially fatal
aortoiliac rupture in heavily calcified lesions.
Hybrid interventions have become an effective option for limb
salvage in patients with multilevel arterial occlusive disease and could
be considered as the first choice. Technical success and short- and
long-term limb salvage outcomes have been shown to be as effective
as open surgical reconstruction for severe iliac and femoral occlusive
disease offering the safety and feasibility of a single-stage therapy
without adding surgical risks. Moreover, patients who suffer also from
infrainguinal occlusive disease will have significant improvement of
their symptoms with treatment of their inflow lesions and may no
longer require additional interventions. Anatomical arterial features
remain the main limitation for hybrid revascularization. An accurate
preoperative study with CT scan is mandatory in order to identify
heavy calcified lesions that still need traditional repair.
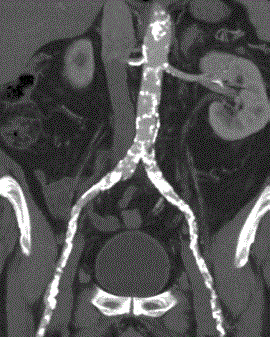
Figure 1
Figure 1
CT scan demonstrates the multiple occlusions and stenosis at left iliac and common femoral arteries.
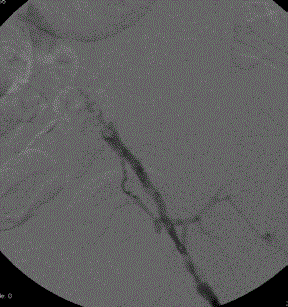
Figure 2
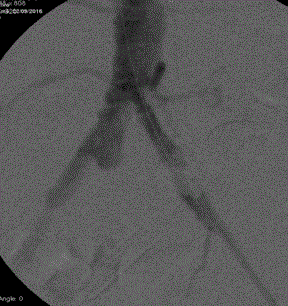
Figure3
Figure 4
References
- Indes JE, Mandawat A, Tuggle CT, Muhsand B, Sosa JA. Endovascular procedures for aorto-iliac occlusive disease are associated with superior short-term clinical and economic outcomes compared with open surgery in the inpatient population. J Vasc Surg. 2010;52:1173-9.
- Vandeweyer D, Verbist J, Bosiers M, Deloose K, Peeters P. Choice of stent in iliac occlusive disease. Interv. Cardiol. 2011;3(3):373-9.
- Mwipatayi BP, Sharma S, Daneshmand A, Thomas SD, Vijayan V, Altaf N, et al. Durability of the balloon-expandable covered versus bare-metal stents in the Covered versusBalloon Expandable Stent Trial (COBEST) for the treatment of aortoiliac occlusive disease. J Vasc Surg. 2016;64:83-94.
- Grimme FA, Goverde PC, Verbruggen PJ, Zeebregts CJ, Reijnen MM. First Results of the Covered Endovascular Reconstruction of the Aortic Bifurcation (CERAB) Technique for Aortoiliac Occlusive Disease. Eur J Vasc EndovascSurg. 2015; 50:638-47.
- Van Haren RM, Goldstein LJ, Velazquez OC, Karmacharya J, Bornak A. Endovascular treatment of TransAtlantic Inter-Society Consensus D aortoiliac occlusive disease using unibody bifurcated endografts. J Vasc Surg. 2017;65:398-405.