Short Communication
Prevention and Management of Inferior Alveolar Nerve Injury Caused by Mandibular Third Molar Removal
Nianhui Cui*, Xiaoqing Pei, Ziyu Yan and Fei Wang
Department of Oral & Maxillofacial Surgery, Peking University School & Hospital of Stomatology, China
*Corresponding author: Nianhui Cui, Department of Oral and Maxillofacial Surgery, Peking University School and Hospital of Stomatology, Beijing 100081, China
Published: 03 Nov, 2017
Cite this article as: Cui N, Pei X, Yan Z, Wang F.
Prevention and Management of Inferior
Alveolar Nerve Injury Caused by
Mandibular Third Molar Removal. Clin
Surg. 2017; 2: 1716.
Short Communication
The constituent ratio of reasons of the tooth extraction
Tooth extraction, as the ultimate dental treatment mostly, is a commonest surgical
procedure carried out by the oral surgeon. Reasons for tooth extraction vary with the
dental treatment and dental habit, education condition, economic level and so on [1,2]. Through the
statistical analysis of the reasons for tooth extraction, it is helpful to know the oral health condition
and the medical condition of oral cavity, and treatment of oral diseases.
From the 1950s till now, investigation of the reasons for tooth extraction have been performed
in many countries or areas [1,3]. But most of these surveys were carried after 1980s. In the 1980 s,
most studies showed that caries is the leading cause of tooth extraction. In France, Cahen et al. [4]
investigated 14,621 cases of tooth extraction. They found that the main reason for the tooth extraction
was caries, and the second was periodontitis. At the same period, Ainamo et al. [5] in Finland, Kay
[6] and Agerholm [7] in the United Kingdom also investigated tooth extraction reasons. The results
showed that the first two reasons were caries and periodontitis. In 1990s, Murray [8] in Canada,
Reich [9] in Germany, Haddad [10] in Jordan investigated the reasons of tooth extraction. They
reported periodontitis had become the first reason instead of caries. In 21st century, some followup
studies had shown that the reason spectrum of tooth extraction had been changed [11]. Trovik
et al. [12] tracked for 30 years in Norway, The result was that ratio of caries had been decreased
significantly. Orthodontic tooth extraction became the main reason for the people under 20 years
old. There were also these kinds of studies in China. In 1956 and 1992, two studies were done by
Liu [13] and Wang [14] in Peking University, Hospital of Stomatology. Caries and periodontitis
alternated leading position. In another famous Chinese dental hospital, West China Stomatological
Hospital, Tian got the same result in 1995 from 23040 cases [15].
From July 2014 to August 2016, we investigated 26760 teeth extracted from 22796 patients in
Peking University, Hospital of Stomatology. 11309 of them were cause by impaction, 6585 were
caries, 4661 were periodontitis and 1576 were orthodontic purpose. In general hospital at the same
time, 589 from 1107 teeth were extracted because of impaction, 290/1107 was caries and 121/1107
was periodontitis. These indicated that impacted teeth might become the first reason in the central
cities of China.
The occurrence and evaluation of the injury of inferior alveolar nerve (IAN)
The treatment of injury of IAN became more and more important with the increase proportion
of the mandibular wisdom tooth extraction. There are many factors that affect nerve injury.
Operation procedure, age, shape and depth of the root might be the main factors [16]|.
Once the nerve injury was happened, the types and degree of nerve injury should be evaluated
firstly. As the IAN injury is a kind of peripheral nerve injury, it could be follow the injury classification
for peripheral nerve. Such as Seddon Classification: neurapraxia, axonotmesis and neurotmesis [17];
Sunderland Classification: Io-Vo [18]; British Medical Research Council neurological dysfunction
criteria: S0-S4 [19].
Common evaluation methods of IAN injury were subjective evaluation method [20,21],
objective examination method and combination of both subjective and objective [20,21]. One of the
especially put forward methods is quantitative sensory testing (QST). It's a quantitative input and
output psychophysiological method to evaluate the reaction of human subject caused by variety of
quantitative stimuli acted on tissues [24]. German Research Network on Neuropathic Pain DFNS)
suggested a standard program of QST depended on related study results [25,26]. After that, Matos
raised a series method of QST for trigeminus.
During 2015, we used QST to evaluate 40 patients who had their
mandibular third molar removed in our department. The QST were
taken in the point of pre-operation, 24 hr, one week and 4 weeks
after operation. The results showed that although all the patients
had not realized the numbness of lower lip, QST could detect the
abnormal of trigeminus. There were significant changes in cold
detection threshold (CDT), warmth detection threshold (WDT),
heat pain threshold (HPT), mechanical pain threshold (MPT),
vibration detection threshold (VDT) and pressure pain threshold
(PPT). Alteration trends were decrease of thermal detection ability,
bluntness of vibration detection ability and sensitive of pressure pain.
The effect of coronectomy in prevention of IAN injury
during the extraction of mandibular third molar
There were some treatment for the IAN injury, such as
neurorrhaphy (epineurial suturing, Beam suture method) [28,29];
autologous nerve transplantation [28,29]; tubulization [30]. And
some non-operative methods: laser treatment [28], taking medicine.
But the therapeutic effect was unpredictable. That mean to prevent is
more important compare with treatment.
Coronectomy is to remove the crown of the wisdom tooth only
instead of extract the whole tooth from the mandible. It was firstly
reported by Ecuyer and Debien in 1984 [31]. In 1989, Knutsson
preceded a prospective experimental study of 33 patients. They
drew a conclusion that coronectomy was a suitable method in the
situation of close contact between root and IAN [32]. After that,
some clinical experiments to study the indication and contradiction
of coronectomy [33,34]. A 10-year follow-up study showed that there
was no untoward effect during the research. A RCT study reported
safety and different kinds of movements of the residual roots without
any pain and infection.
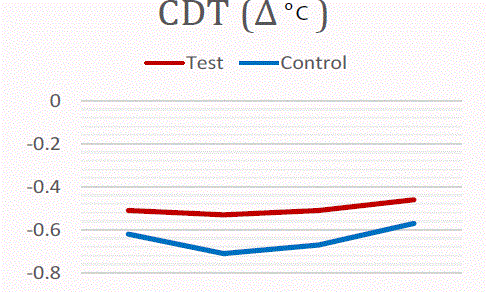
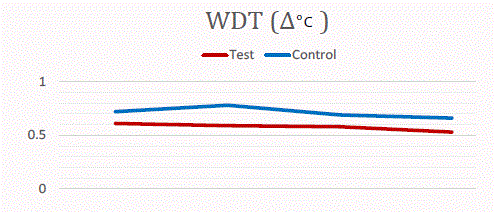
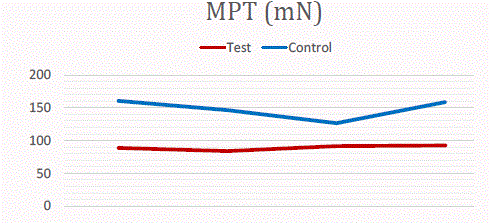
We design a Prospective controlled study of using QST to detect
the neural function of coronectomy compared with total extraction.
Preliminary results showed that less influence was happened in
coronectomy group. CDT, WDT and MPT were more smoothly in
this group in the figure of compare (Figure 1-3). Three move mode
scan be seen in CBCT of residual roots after 6 months follow-up:
stable motionless, straight motion and mesial rotation. Further
follow-up will be taken to find the speed of movement.
Summary, with the development of economy and the change of
population, the constituent ratio of tooth extraction was alternated
in central city in China. The IAN injury was still an intractable
complication. QST is sensitive method to detect the IAN injury after
removal of mandibular third molar. It was also useful in the study of
coronectomy. The result showed that coronectomy can prevent the
injury of IAN, the function of IAN was more stable. The movement of
residual root could be straight or curve. The long-term outcome need
be continuous follow-up.
Figure 1
Figure 2
Figure3
References
- Chestnutt IG, Binnie VI, Taylor MM. Reasons for tooth extraction in Scotland. J Dent. 2000;28(4):295-7.
- Farsi JMA. Common causes of extraction of teeth in Saudi Arabia. Saudi Dental Journal, 1991;4(3).
- Agerholm D. Reasons for extraction by dental practitioners in England and Wales: a comparison with 1986 and variations between regions. J Dent. 2001;29(4):237-41.
- Cahen PM, Frank RM, Turlot JC. A survey of the reasons for dental extractions in France. J Dent Res. 1985;64(8):1087-93.
- Ainamo J, Sarkki L, Kuhalampi ML, Palolampi L, Piirto O. The frequency of periodontal extractions in Finland. Community Dent Health. 1984;1(3):165-72.
- Kay EJ, Blinkhorn AS. The reasons underlying the extraction of teeth in Scotland. Br Dent J. 1986;160(8):287-90.
- Agerholm DM, Sidi AD. Reasons given for extraction of permanent teeth by general dental practitioners in England and Wales. Br Dent J. 1988;164(11):345-8.
- Murray H, Locker D, Kay EJ. Patterns of and reasons for tooth extractions in general dental practice in Ontario, Canada. Community Dent Oral Epidemiol. 1996;24(3):196-200.
- Reich E, Hiller KA. Reasons for tooth extraction in the western states of Germany. Community Dent Oral Epidemiol. 1993;21(6):379-83.
- Lee CY, Chang YY, Shieh TY, Chang CS. Reasons for permanent tooth extractions in Taiwan. Asia Pac J Public Health. 2015;27(2):NP2350-7.
- McCaul LK, Jenkins WM, Kay EJ. The reasons for the extraction of various tooth types in Scotland: a 15-year follow up. J Dent. 2001;29(6):401-7.
- Trovik TA, Klock KS, Haugejorden O. Trends in reasons for tooth extractions in Norway from 1968 to 1998. Acta Odontol Scand. 2000;58(2):89-96.
- Liu FT. Survey of the reason for tooth extration. Chinese Journal of Stomatology. 1956;2(2):108-10.
- Wang DH, Du HT. Analysis of reasons of tooth extraction in 30 years. J Modern Stomatol. 1992;6(3):174-5.
- Tian HJ, Luo KY, Lin JY. Statistical analysis of 23040 cases of tooth extraction. J West China Stomatol. 1995;13(2):139-40.
- Bell GW, Rodgers JM, Grime RJ, Edwards KL, Hahn MR, Dorman ML, et al. The accuracy of dental panoramic tomographs in determining the root morphology of mandibular third molar teeth before surgery. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2003;95(1):119-25.
- Seddon HJ, Medawar PB, Smith H. Rate of regeneration of peripheral nerves in man. J Physiol. 1943;102(2):191-215.
- Sunderland S. A classification of peripheral nerve injuries producing loss of function. Brain. 1951;74(4):491-516.
- Mackinnon SE. Surgical management of the peripheral nerve gap. Clin Plast Surg. 1989;16(3):587-603.
- Poort LJ, van Neck JW, van der Wal KG. Sensory testing of inferior alveolar nerve injuries: a review of methods used in prospective studies. J Oral Maxillofac Surg. 2009;67(2):292-300.
- Clark W C, Kuhl J P, Keohan M L, Helena Knotkova, Rachel T Winer, Germaine A Griswold, et al. Factor analysis validates the cluster structure of the dendrogram underlying the Multidimensional Affect and Pain Survey (MAPS) and challenges the a priori classification of the descriptors in the McGill Pain Questionnaire (MPQ). Pain. 2003;106(3):357-63.
- Teerijoki-Oksa T, Jaaskelainen S K, Forssell K, Forssell H. Recovery of nerve injury after mandibular sagittal split osteotomy. Diagnostic value of clinical and electrophysiologic tests in the follow-up. Int J Oral Maxillofac Surg. 2004;33(2):134-40.
- Jaaskelainen S K, Peltola J K, Lehtinen R. The mental nerve blink reflex in the diagnosis of lesions of the inferior alveolar nerve following orthognathic surgery of the mandible. Br J Oral MaxillofacSurg. 1996;34(1):87-95.
- Yang GJ, Cao Y, Zhang L, Qin XY, Xie QF. Data of the quantitative orofacial somatosensory functions of healthy subjects and its influence factors analysis. Beijing Da Xue Xue Bao. 2015;(03):521-8.
- Rolke R, Magerl W, Campbell KA, Schalber C, Caspari S, Birklein F, et al. Quantitative sensory testing: a comprehensive protocol for clinical trials. Eur J Pain. 2006;10(1):77-88.
- Rolke R, Baron R, Maier C, Tölle TR, Treede RD, Beyer A, et al. Quantitative sensory testing in the German Research Network on Neuropathic Pain (DFNS): standardized protocol and reference values. Pain. 2006;123(3):231-43.
- Matos R, Wang K, Jensen JD, Jensen T, Neuman B, Svensson P, et al. Quantitative sensory testing in the trigeminal region: site and gender differences. J Orofac Pain. 2011;25(2):161-9.
- Eppley BL, Snyders RV Jr. Microanatomic analysis of the trigeminal nerve and potential nerve graft donor sites. J Oral Maxillofac Surg. 1991;49(6):612-8.
- Jones RHB. Microsurgical repair of nerves injured during third molar surgery. Australian Dental Journal 1992;37(4):253–61.
- Tay ABG, Poon CY, Teh LY. Immediate repair of transected inferior alveolar nerves in sagittal split osteotomies. J Oral Maxillofac Surg. 2008;66(12):2476–81.
- Knutsson K, Lysell L, Rohlin M. Postoperative status after partial removal of the mandibular third molar. Swed Dent J. 1989;13(1-2):15-22.
- Hatano Y, Kurita K. Clinical Evaluations of Coronectomy (Intentional Partial Odontectomy) for Mandibular Third Molars Using Dental Computed Tomography: A Case-Control Study. J Oral Maxillofac Surg. 2009;67:1806-14.
- Leung YY, Cheung LK. Safety of coronectomy versus excision of wisdom teeth: a randomized controlled trial. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2009;108(6):821-7.
- Pogrel MA. In Reply to Coronectomy : A Questionable Procedure. J Oral Maxillofac Surg. 2005;63:723-5.