Case Report
Thoracic Spinal Cord Glioblastoma: A Case Report
Emre Unal*
Department of Surgery, Medical Park Fatih Hastanesi, İstanbul, Turkey
*Corresponding author: Emre Unal, Department of Surgery, Medical Park Fatih Hastanesi, İstanbul, Turkey
Published: 25 Oct, 2017
Cite this article as: Unal E. Thoracic Spinal Cord
Glioblastoma: A Case Report. Clin
Surg. 2017; 2: 1694.
Abstract
We report a case of a 62-year-old female patient with paraplegia. Magnetic resonance imaging showed an intramedullary mass lesion of thoracic region. Surgery was performed and histopathological evaluation revealed primary glioblastoma of the spinal cord. Primary spinal glioblastoma is a rare entity unlike cranial counterpart; with high mortality rate. Survival rates are still unsatisfactory even with surgery accompanied by adjuvant chemotherapy and radiotherapy.
Introduction
Glioblastoma is the most common primary cerebral tumor in adults [1] yet Primary Spinal Glioblastoma (PSG) is very rare. Intramedullary spinal tumors constitute 2% to 8.5% of all primary Central Nervous System (CNS) tumors [2]. Primary spinal glioblastomas involve only 4% to 8% of all intramedullary spinal tumors and 1.5% of all spinal tumors [3,4] and they mostly occur in the cervical and cervicothoracic region (60%) [5]. For this reason, we only have few data to interpret on how to manage and treat PSG’s. In this article, we present a rare case of primary glioblastoma of the spinal cord that originated solelyfrom thoracic region.
Patients and Methods
A 62-year-old female patient admitted to hospital with pain and numbness on both legs
(dominantly on the left leg) and on her back for 6 months. She had a history of diabetes mellitus and
mild anemia was spotted on laboratory tests. She complained of shortening her walking distance.
She had no abnormality on physical examination. Neurological examination revealed hypoesthesia
on right leg, hypoactive deep tendon reflexes on both sides and paraplegia. A gadolinium enhanced
thoracic spinal magnetic resonance (MRI) was performed. MRI revealed a hypointense on T1
weighted, and hyperintense on T2 weighted sequences, heterogeneously enhanced lesion between
T7 and T12 vertebral levels that expanded spinal cord (Figure 1).
By a vertical midline incision, laminoplasty was performed to T8, T9, T10 and T11 vertebrae.
After dural opening, intramedullary yellow-grey colored lesion was reached. Due to adhesions to
the rootlets, arachnoid membranes and spinal cord, only a partial removal could be achieved under
neuromonitoring. Closing of laminoplasty was performed using mini titanium screws and plates.
Histopathological examination showed Glioblastoma Grade IV with Ki-67 index of 10% to 15%.
The day after surgery, the patient was mobilized with 4/5 paraparesis. She was sent to radiotherapy
following one month after surgery and she still is under this treatment.
Discussion
Glioblastoma of the spinal cord can develop primarily or due to metastasis of a cerebral lesion.
They tend to occur in the early stages (Mean age: 33.5) of life unlike cerebral glioblastomas6. In our
case, the patient is 62 years old.
Clinical manifestations are not pathognomonic and depend on size and location of the lesion.
Signs and symptoms differ from region to region where the tumor is located and are mostly
generated due to mechanical compression or direct damage to the spinal cord or the rootlets. There
are reported cases of malignant spinal astrocytomas that develop hydrocephalus which is suspected
to be caused by increased protein concentration in the cerebrospinal fluid (CSF) resulting occlusion
of CSF channels [5]. The initial symptoms can be mild and non- specific but in the later stages, the
symptoms worsen including paraplegia, other various motor disorders and urinary incontinence
[6].
The gold standard for imaging is gadolinium enhanced MRI for spinal tumors. Cerebrospinal
fluid cytology and PET scan can also be used especially on glioblastoma drop metastasis but they
are usually inconclusive [7] and PET-CT has a risk of increasing glycolysis in malignant tumors [8].Most of the PSG tumors are seen as infiltrative, expansive lesions that enhance heterogeneously on T1 sequence but using these findings on
MRI scan, differentiation from other spinal pathologies is still difficult
and histopathological evaluation following tissue sampling is needed
[9]. Differential diagnosis for PSG includes other spinal malignancies,
transverse myelitis, abscess and bacterial myelitis [10].
The first line treatment for patients presenting with neurological
impairment is surgery. Total resection is the priority without worsening
neurological condition of the patient. However the infiltrative growth
pattern of these tumors and lack of cleavage plane to the adjacent
tissues allow only subtotal resection or biopsy in most cases [6,11].
Therefore adjuvant chemotherapy and radiotherapy are of the utmost
importance for prolonging survival. Since spinal glioblastoma is
a rare entity, there is no consensus on how to treat it after surgery.
Temozalamide is the most commonly used chemotherapeutic agent
but its effects on long term survival are uncertain [12]. However
including radiotherapy can improve results [13]. Median survival
time for PSG is 8.18 months according to Ozgirayet. Median overall
survival for spinal glioblastoma (including metastases) is calculated
to be 11 months [14]. But glioblastoma metastases significantly lower
this rate because the survival time for patients with glioblastoma
metastases is calculated to be 2-3 months [15]. PSG seem to have
worse outcome than its cranial counterpart but adjuvant therapy
(chemotherapy, radiotherapy or both) significantly improve survival
time.
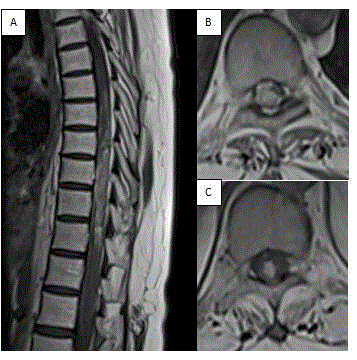
Figure 1
Figure 1
T1-Weighted Contrast Enhanced Preoperative sagittal (A), axial T7
Level (B), and axial T9 Level (C) MRIs.
Conclusion
PSG is a rare condition unlike cranial glioblastoma. Although total resection is unlikely, surgery is essential for patients with neurological deficit and for cytoreduction to prolong survival time. Surgery is the best option for these patients but even with adjuvant therapy, outcome is still poor.
References
- Zhang J, Shrestha R, Li J, Jiang S. Fourth ventricle glioblastoma. Clin Neurol Neurosurg. 2012;114(8):1164-7.
- Samuel N, Tetreault L, Santaguida C, Nater A, Moayeri N, Massicotte EM, et al. Clinical and pathological outcomes after resection of intramedullary spinal cord tumors: a single-institution case series. Neurosurg Focus. 2016;41(2):E8.
- Feryal Karaca, ÇigdemUsul Afsar, Erkut Erkurt, Candas Tunali, HasanSuat Arslantas, Çigdem Kocabas. Primary Spinal Glioblastoma Multiform: A Case Report and Review of the Literature. J Neurological Sci (Turkish). 2014;31(2):366-7.
- Ozgiray E, Akay A, Ertan Y, Cagli S, Oktar N, Ozdamar N. Primary Glioblastoma of The Medulla Spinalis: A Report of Three Cases and Review of the Literature . Turk Neurosurg. 2013;23(6):828-34.
- Morais N, Mascarenhas L, Soares-Fernandes JP, Silva A, Magalhães Z, Costa JA. Primary spinal glioblastoma: A case report and review of the literature. Oncol Lett. 2013;5(3):992-6.
- Behmanesh B, Setzer M, Konczalla J, Harter P, Quick-Weller J, Imoehl L, et al. Management of Patients with Primary Intramedullary Spinal Cord Glioblastoma. World Neurosurg. 2017;98:198-202.
- Tai P, Dubey A, Salim M, Vu K, Koul R. Diagnosis and Management of Spinal Metastasis of Glioblastoma. Can J Neurol Sci. 2015;42(6):410-3.
- Won KS, Kim JS, Ra YS, Sohn CH, Zeon SK. FDG PET of primary spinal glioblastoma initially mimicking a transverse myelitis on MRI. Clin Nucl Med. 2006;31(9):556-7.
- Shen CX, Wu JF, Zhao W, Cai ZW, Cai RZ, Chen CM. Primary spinal glioblastoma multiforme: A case report and review of the literature. Medicine (Baltimore). 2017;96(16):e6634.
- Bourgouin PM, Lesage J, Fontaine S, Konan A, Roy D, Bard C, et al. A pattern approach to the differential diagnosis of intramedullary spinal cord lesions on MR imaging. AJR Am J Roentgenol. 1998;170(6):1645-9.
- Zileli M, Coşkun E, Ozdamar N, Ovül I, Tunçbay E, Oner K, et al. Surgery of intramedullary spinal cord tumors. Eur Spine J. 1996;5(4):243-50.
- Hernández-Durán S, Bregy A, Shah AH, Hanft S, Komotar RJ, Manzano GR. Primary spinal cord glioblastoma multiforme treated with temozolomide. J Clin Neurosci. 2015;22(12):1877-82.
- Mallick S, Madan R, Julka PK. Primary spinal glioblastoma treated with adjuvant radiation and temozolomide: Report of two cases. J Cancer Res Ther. 2015;11(3):654.
- Konar SK, Maiti TK, Bir SC, Kalakoti P, Bollam P, Nanda A. Predictive Factors Determining the Overall Outcome of Primary Spinal Glioblastoma Multiforme: An Integrative Survival Analysis. World Neurosurg. 2016;86:341-8.
- Guzel Aslan, Tatli Mehmet, Dirier Ahmet, Bozbuga Mustafa, Bayindir Çiçek. Spinal Leptomeningeal Metastasis of Cerebral Glioblastoma Multiforme in a Child. Journal of Neurological Sciences (Turkish). 2005;22(2):200-5.