Case Report
Atypical Clinical Presentation of Primary Umbilical Endometriosis
Bachir Elias1, Elias Adam2, Hanane Ziadeh3* and Clemence Matta4
1Department of General Surgery, CHR Metz-Thionville, Bel-Air hospital, Thionville 57126, France
2Department of General Surgery, Centre Hospitalier Universitaire Notre Dame De Secours, Byblos, Lebanon
3Department of Obstetrics and Gynecology, Centre Hospitalier Universitaire Notre Dame De Secours, Byblos,
Lebanon
4Department of Hematology/Oncology, Centre Hospitalier Universitaire Notre Dame De Secours, Byblos, Lebanon
*Corresponding author: Hanane Ziadeh, Department of Obstetrics and Gynecology, Centre Hospitalier Universitaire Notre Dame De Secours, Byblos, Lebanon
Published: 27 Sep, 2017
Cite this article as: Elias B, Adam E, Ziadeh H, Matta C.
Atypical Clinical Presentation of Primary
Umbilical Endometriosis. Clin Surg.
2017; 2: 1635.
Abstract
Primary umbilical endometriosis is a rare condition. Clinical presentation is usually a painful umbilical nodule or bleeding during menstruation. We report a case of this rare condition with atypical clinical presentation. Also is discussed the management of umbilical endometriosis. Keywords: Endometriosis; Umbilicus; Pain; Surgery
Introduction
Umbilical endometriosis is a rare clinical condition, which accounts for 0.5% to 1% of all cases of non-genital endometriosis [1]. When it occurs without any previous surgery is called primary umbilical endometriosis. We report a case of 29 year old female without any surgical history who presented with a painful umbilical mass. Histopathological examination after surgery confirms the endometriosis nature of the lesion. Surgical excision remains the treatment of choice for umbilical endometriosis.
Case Presentation
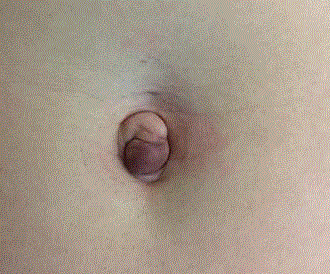
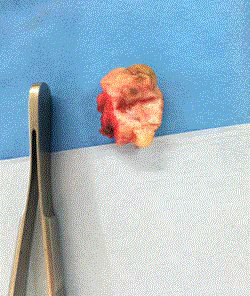
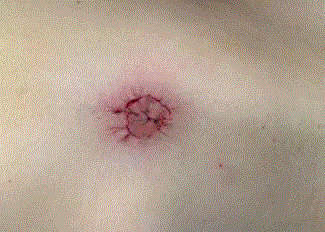
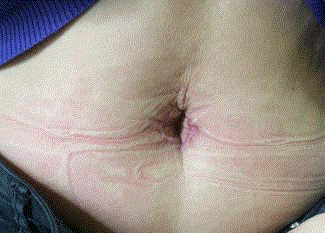
A 29 year old female without any past medical or surgical history, consulted at the emergency department for pain at the umbilicus since three days. She had no gastrointestinal or gynaecological symptoms. She did not notice previous painful episodes even during menstruation. Physical exam showed a 1 cm brownish umbilical mass. The first diagnosis was small incarcerated umbilical hernia with necrotic fat content (Figure1). The patient underwent surgical exploration and excision of the umbilicus and a 2 cm nodule (Figure 2); the nodule was completely extraperitoneal. A reconstruction of a new umbilicus was done (Figure 3), and the patient was discharged at the same day without any complications. The diagnosis of umbilical endometriosis was confirmed by the pathology results. The patient had an asymptomatic follow-up with a good aesthetic result (Figure 4). Because of absence of symptoms related to pelvic endometriosis, laparoscopic exploration for pelvis endometriosis was not done.
Figure 1
Figure 2
Figure 3
Figure 4
Discussion
Cutaneous endometriosis variant is rare: primary umbilical endometriosis called sometimes nodule de Villar in French is a rare clinical condition, which accounts for 0.5% to 1% [1]; less than 150 cases were reported in the literature [2]. There are two type of umbilical endometriosis: primary endometriosis in patients without any past surgical history and the secondary endometriosis occurring after gynaecological operations usually at the trocard site [3]. The pathophysiology is an ectopic migration of endometrial tissue out of the uterus. The exact mechanism of this process is still controversial. Three theories were described: an intraperitoneal migration of endometrial cells during menstruation [4]; or coelomic metaplasia [5] or metastatic dissemination of endometrial by lymphatics or haematogenous spread [2]. Endometriosis was described in many localisations such as ovaries, peritoneum, digestive tract, urinary tract, pleura, lungs, liver, brain, umbilicus and even nasal [6]. Clinical presentation of umbilical endometriosis is usually pain during menstruation and/ or bleeding. Differential diagnoses are umbilical hernia as in our case, malignant tumour, lipoma, or dermoid cyst [7]. Ultrasound, MRI and percutaneous biopsy are used to confirm the diagnosis of umbilical endometriosis before surgery [8-10]. The final diagnosis is obtained by pathology after surgery. Surgical excision of umbilical endometriosis is the treatment of choice. The operative options are a complete umbilical resection, with or without repair of the underlying fascia and peritoneum or local excision of the nodule, sparing the umbilicus. Total removal of the umbilicus is the most frequently performed operation [11]. Some authors have reported some success in relieving symptoms and reducing the size of the endometriosic nodule by using medical hormonal treatment [12]. Once primary umbilicus endometriosis is confirmed, laparoscopic exploration can be recommended to rule out pelvic endometriosis but remains debatable in asymptomatic patients [11,13]. Umbilical endometriosis is a rare condition. It should be considered as a differential diagnosis in any female presenting an umbilical nodule even without previous surgeries. The clinical presentation of painful nodule or bleeding during menstruation is not always typical. Our patient presented atypical clinical symptoms of her primary umbilical endometriosis.
References
- Skidmore RA, Woosley JT, Katz VL. Decidualized umbilical endometriosis. Int J Gynaecol Obstet. 1996;52(3):269-73.
- Zollner U, Girschick G, Steck T, Dietl J. Umbilical endometriosis without previous pelvic surgery: a case report. Arch Gynecol Obstet. 2003;267(4):258-60.
- Rubegni P, Sbano P, Santopietro R, Fimiani M. Case 4. Umbilical endometriosis. Clin Exp Dermatol. 2003;28(5):571-2.
- Sampson JA. The life history of ovarian hematomas (hemorrhagic cysts) of endometrial (mu¨llerian) type. Am J Obstet Gynecol. 1922;4(5):451-512.
- Kruitwagen RF, Poels LG, Willemsen WN, de Ronde IJ, Jap PH, Rolland R. Endometrial epithelial cells in peritoneal fluid during the early follicular phase. Fertil Steril. 1991;55(2):297-303.
- Laghzaoui O, Laghzaoui M. [Nasal endometriosis: apropos of 1 case]. J Gynecol Obstet Biol Reprod (Paris). 2001;30(8):786-8.
- Darouichi M. Endométriose ombilicale primitive et secondaire. Feuillets de Radiologie. 2013;53(1):21-6.
- Ozkol M, Yoleri L, Demir MA, Demireli P, Pabuscu Y. The significance of venous dominance in color Doppler ultrasound for the diagnosis of primary nodular skin lesions: a new perspective in classification. Clin Imaging. 2006;30(1):43-7.
- Yu CY, Perez-Reyes M, Brown JJ, Borrello JA. MR appearance of umbilical endometriosis. J Comput Assist Tomogr. 1994;18(2):269-71.
- Catalina-Ferna´ndez I, Lo´pez-Presa D, Sa´enz-Santamaria J. Fine needle aspiration cytology in cutaneous and subcutaneous endometriosis. Acta Cytol. 2007;51(3):380-4.
- Fancellu A, Pinna A, Manca A, Capobianco G, Porcu A. Primary umbilical endometriosis. Case report and discussion on management options. Int J Surg Case Rep. 2013;4(12):1145-8.
- Bagade PV, Guirguis MM. Menstruating from the umbilicus as a rare case of primary umbilical endometriosis: a case report. J Med Case Rep. 2009;3:9326.
- Mechsner S, Bartley J, Infanger M, Loddenkemper C, Herbel J, Ebert AD. Clinical management and immunohistochemical analysis of umbilical endometriosis. Arch Gynecol Obstet. 2009;280(2):235-42.