Case Report
Is Pancreatic Incidentalomas Biopsy is Necessary during Bariatric Surgery- Three Case Reports
Mohammad Kermansaravi1, Foolad Eghbali1*, Sattar Darabi1 and Abdolreza Pazouki1,2
1Department of Minimally Invasive Surgery, Iran University of Medical Sciences, Iran
2Department of Minimally Invasive Surgery, Center of Excellence of International Federation for Surgery of Obesity,
Iran
*Corresponding author: Foolad Eghbalii, Minimally Invasive Surgery Research Center, Iran University of Medical Sciences, Iran, Hazrat-e-Rasool Hospital, ShahidMansouri Ave., Niyayesh St. Sattarkhan St., Setayesh Street, No. 98, Tehran, Iran
Published: 20 Sep, 2017
Cite this article as: Kermansaravi M, Eghbali F, Darabi S,
Pazouki A. Is Pancreatic Incidentalomas
Biopsy is Necessary during Bariatric
Surgery- Three Case Reports. Clin
Surg. 2017; 2: 1618.
Abstract
Background: Obesity, especially in central form and high body mass index (BMI) ≥ 25 kg/m², lead
to higher incidence of some malignancies such as pancreatic malignant tumors in this population.
In addition, there is a defect on screening test for pancreatic malignancies in morbid obese patients
before bariatric surgery. The approach to incidental solid pancreatic mass (solid incidentaloma)
during bariatric surgery is challenging and has never been described.
Case Summary: We report three morbid obese cases that despite to follow recommended routine
pre-operative evaluation according to bariatric surgery guidelines, it was found prominent mass in
pancreatic head area during bariatric surgery. Laparoscopic biopsy showed focal pancreatitis in the
histopathologic in two cases and showed lipomatosis in one of the cases.
Conclusion: There are no strong evidences that any incidental mass during bariatric surgery must
be biopsied but the patients must be observed via precise follow-ups.
Keywords: Morbid obesity; Bariatric surgery; Pancreatic incidentalomas; Pancreatitis;
Laparoscopic biopsy; Case report
Introduction
Nowadays, the incidence of obesity is increasing and so, bariatric surgeries are being more
common and more popular. Before performing bariatric surgery, medical and psychologic
evaluation must be done by a multidisciplinary team and this evaluation is nearly similar to other
major abdominal surgeries; and malignancy screening is done only based on age and sex according
to international health guidelines
[1,2].
It was reported that obesity, especially central obesity and body mass index (BMI) ≥25 kg/
m², is associated with higher incidence of some malignancies such as pancreatic cancer and some
high volume studies concluded that any 5 units increasing in BMI, lead to 10 percent increasing
pancreatic cancer risk and an increase of 20 to 60% in morbid obesity risk overall
[3-6].
In addition, there is no test for pancreatic cancer screening and even the pancreatic enzymes in
bariatric surgery especially in asymptomatic patients
[1,7].
Due to the lack of screening tests for early detection, it usually presents in advance and
unresectable forms. So, any incidental solid pancreatic mass (solid incidentaloma) needs
histopathological examination to achieve definite diagnosis and differentiate between malignant
lesion from pre-malignant or benign lesions, such as focal pancreatitis, due to difficulty of definite
differentiation with imaging and biochemical tests.
[3,8-10].
Due to the importance of histopathological diagnosis of pancreatic incidentalomas (PIs) and
the increased risk of pancreatic cancer in morbid obese patients, it is reasonable to have a guideline
to approach these lesions which has not been described before., Three hundred and seventy five
patients underwent laparoscopic bariatric surgery in our obesity clinic, Rasool-e-Akram hospital,
Iran University of Medical Sciences, Tehran, Iran, as a Center of Excellence of International
Federation for Surgery of Obesity and Metabolic Disorders (IFSO), from August 2015 to March
2017.
Case Presentation
Case 1
An 18 year old female with BMI of 45 kg/m2 was scheduled for bariatric surgery after psychological and medical evaluations by our multidisciplinary team
according to American Society for Metabolic and Bariatric Surgery
(ASMBS) guideline
[2], Abdominal ultrasonography (US) to evaluate
the liver and gallbladder stones (as a routine in our center) was
normal in this patient. Due to her complain of heartburn, she also
underwent upper gastrointestinal endoscopy (UGIE) and had only
mild gastritis, with negative Helicobacter pylori (HP). All biochemical
analysis such as complete blood count (CBC) and liver function test
(LFT) were normal. She had no familial history of gastrointestinal
malignancies and also no history of alcohol and cigarette usage.
During laparoscopic surgery, we found a prominent lobulated mass
with 3cm diameter in head of pancreas. We did laparoscopic incisional
biopsy of mass and postponed the bariatric operation till getting
the definite histopathological report and send her tumor markers
carcinoembryonic antigen (CEA) and Cancer Antigen 19-9(CA 19-
9). The definite pathologic report was focal chronic pancreatitis with
fibrosis and CEA, CA19-9, amylase and lipase were in normal ranges.
Six days after, the patient underwent laparoscopic sleeve gastrectomy.
Case 2
A 42 year old female with BMI of 52 kg/m2, complete pre-operative
medical evaluation after eradication of HP was scheduled for surgery.
She had normal abdominal US and chronic gastritis in UGIE. She had
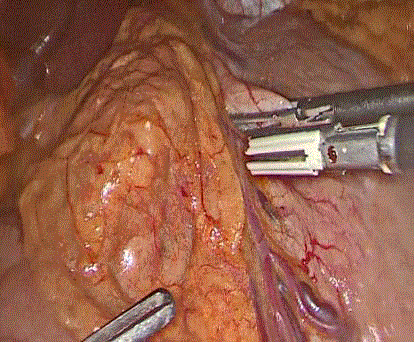
no significant finding in familial history and drug history. During the
surgery, we detected a lobulated prominence pancreatic head zone,
with at least 5 cm diameter and regional enlarged lymph nodes (LNs)
which are shown in
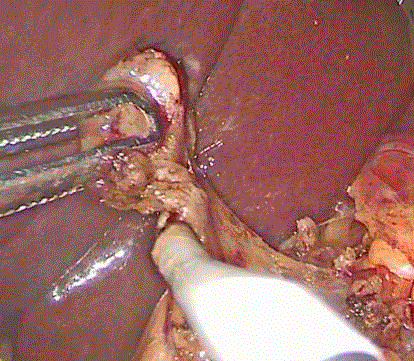
(Figure1). We performed LNs excisional biopsy
(Figure 2), mass incisional biopsy, and laparoscopic mini-gastric
bypass, simultaneously. We also requested pancreatic enzymes test
and tumor markers. All requested biochemical tests were normal and
the pathologic reports were focal pancreatitis with inflammatory LNs,
without any evidences of malignancy.
Case 3
The 29 years old rarely smoker and type-2 diabetic male with
BMI of 56 kg/m2 underwent bariatric surgery after pre-operative
evaluations. He had a 5mm asymptomatic gall stone and other
evaluations had no significant finding. We discovered a 3cm firm
mass in head of pancreas during laparoscopy. We accomplished
laparoscopic core needle biopsy (CNB) with a 16 gauge automatic
reusable biopsy device and performed laparoscopic mini-gastric
bypass at the same time. The pathologic report was focal lipomatosis
without malignancy.
In all above cases, we performed regular follow-ups in addition to
check the CA19-9 and CEA 1,3 and 6 months after surgery. All tumor
markers were free of malignancy evidence and the patients had not
any specific complains.
Figure 1
Figure 2
Discussion
Obesity is an important risk factor for both acute pancreatitis and
pancreatic cancer [4]. Recently, the worldwide incidence of pancreatitis
is increasing in parallel with increased incidence of obesity [11,12].
High inflammatory reactions, obesity or hypertriglyceridemia related
lipotoxicity and high concentrated bilirubin are possible mechanisms
responsible for pancreatitis in obese patients [5,12-14]. Also, obesity
has a significant effect on pancreatic malignancies, with some possible
effects, such as inflammatory and humoral effects of fatty tissue,
hyperinsulinemia and insulin resistance, increased exposure to some
nutritional carcinogens and decreased physical activities [3,4].
Approach to PIs in morbid obese patients should be different
from normal weight patients due to increased risk of malignancy
in obese patients [3] and tissue sampling may be necessary in these
patients.
Biopsy has a critical role in definite diagnosis and determining the
best option for treatment in solid PIs [15]. There are some minimally
invasive methods for tissue sampling including ;endoscopic
ultrasound-guided fine needle aspiration biopsy (EUS-FNA), CT
or US–guided core needle biopsy (CNB), and laparoscopic biopsy.
Some studies demonstrated that EUS-FNA and CT or US-CNB had a
similar accuracy [10,16] and in solid PIs had sensitivity of 75%-99%,
specificity of 82%-100%, and accuracy of 94%-99% [10,15-19].
Küper, et al. [6] reported a diagnosis of pancreatic head cancer,
3 months after laparoscopic sleeve gastrectomy in a morbid obese
patient that despite pylorus-preserving pancreatic head resection and
adjuvant chemotherapy, the patient died due to local recurrence and
liver metastases 9 months post operatively.
We performed laparoscopic incisional biopsy in two patients and
laparoscopic-guided CNB in the other one which resulted in definite
diagnosis and rule out of malignancy in the shortest possible time.
The most common benign solid PIs are focal chronic pancreatitis,
and subsequently lipomatosis, solid pseudo-papillary tumors and
benign neuroendocrine tumors [9]. The bariatric surgery postponed
to receive the histopathologic report in case 1. In this case, the
bariatric surgery was more challenging due to some adhesions of
posterior of stomach to pancreas after incisional biopsy. It seems
that in laparoscopic confronting to PIs during bariatric surgery,
there is no evidence of obvious malignant lesion, laparoscopic biopsy
of lesion with simultaneous bariatric surgery is the best option,
but there is no strong evidence to do biopsy. Although need for a
proprietary algorithmic approach in these patients is very important. Additionally, Regular and more precise follow-ups of these patients,
and serious attention to any new symptoms, particularly abdominal
symptoms are necessary.
In conclusion, it is reasonable to perform tissue biopsy for PIs
during bariatric surgery and to continue the bariatric operation, and
then to have more precise follow-ups post-operatively. It is necessary
to do more studies to assess and provide guidelines for dealing with
an incidental solid pancreatic mass in morbid obese patients during
bariatric or other abdominal surgeries.
Inform Consent
Written informed consent was obtained from all patients to use their document information to write this manuscript.
References
- Committee SG. SAGES guideline for clinical application of laparoscopic bariatric surgery. Surg endosc. 2008;22(10):2281-300.
- Dana Telem ea. American Society for Metabolic and Bariatric Surgery: Care Pathway Development for Laparoscopic Sleeve Gastrectomy. 2016.
- Bracci PM. Obesity and pancreatic cancer: overview of epidemiologic evidence and biologic mechanisms. Mol carcinog. 2012;51(1):53-63.
- Grigor'eva I, Efimova O, Suvorova T, Tov N. Pancreatitis, pancreatic cancer and obesity: hypothesis and facts. Eksp Klin Gastroenterol. 2014;(9):4-10.
- Zyromski NJ. Obesity-Related Effects on Pancreatic Disease. Pancreapedia: The Exocrine Pancreas Knowledge Base. 2015.
- Küper MA, Königsrainer I, Schmidt D, Kramer KM, Granderath FA, Schneider J, et al. Morbid obesity and subsequent pancreatic cancer: pylorus-preserving pancreatoduodenectomy after laparoscopic sleeve gastrectomy. Obes Surg. 2009;19(3):385-8.
- Mechanick JI, Youdim A, Jones DB, Garvey WT, Hurley DL, McMahon MM, et al. Clinical practice guidelines for the perioperative nutritional, metabolic and nonsurgical support of the bariatric surgery patient-2013 update: cosponsored by American Association of Clinical Endocrinologists, the Obesity Society, and American Society for Metabolic & Bariatric Surgery. Endocr Pract. 2013;19(2):337-72.
- Tyng CJ, Almeida MFA, Barbosa PN, Bitencourt AG, Berg JAA, Maciel MS, et al. Computed tomography-guided percutaneous core needle biopsy in pancreatic tumor diagnosis. World J Gastroenterol. 2015;21(12):3579-86.
- Karatzas T, Dimitroulis D, Charalampoudis P, Misiakos E, Vasileiadis I, Kouraklis G. Management of cystic and solid pancreatic incidentalomas: a review analysis. J BUON. 2013;18(1):17-24.
- Yang RY, Ng D, Jaskolka JD, Rogalla P, Sreeharsha B. Evaluation of percutaneous ultrasound-guided biopsies of solid mass lesions of the pancreas: a center’s 10-year experience. Clin Imaging. 2015;39(1):62-5.
- Sawalhi S, Al-Maramhy H, Abdelrahman AI, Allah SEG, Al-Jubori S. Does the presence of obesity and/or metabolic syndrome affect the course of acute pancreatitis?: A prospective study. Pancreas. 2014;43(4):565-70.
- Bonfrate L, Wang DQ, Garruti G, Portincasa P. Obesity and the risk and prognosis of gallstone disease and pancreatitis. Best Pract Res Clin Gastroenterol. 2014;28(4):623-35.
- Nawaz H, Koutroumpakis E, Easler J, Slivka A, Whitcomb DC, Singh VP, et al. Elevated serum triglycerides are independently associated with persistent organ failure in acute pancreatitis. Am J Gastroenterol. 2015;110(10):1497-503.
- Patel K, Trivedi RN, Durgampudi C, Noel P, Cline RA, DeLany JP, et al. Lipolysis of visceral adipocyte triglyceride by pancreatic lipases converts mild acute pancreatitis to severe pancreatitis independent of necrosis and inflammation. Am J Pathol. 2015;185(3):808-19.
- Tarantino I, Di Mitri R, Fabbri C, Pagano N, Barresi L, Granata A, et al. Is diagnostic accuracy of fine needle aspiration on solid pancreatic lesions aspiration-related? A multicentre randomised trial. Dig Liver Dis. 2014;46(6):523-6.
- Sur YK, Kim YC, Kim JK, Lee JH, Yoo BM, Kim YB. Comparison of Ultrasound‐Guided Core Needle Biopsy and Endoscopic Ultrasound‐Guided Fine‐Needle Aspiration for Solid Pancreatic Lesions. J Ultrasound Med. 2015;34(12):2163-9.
- Detlefsen S, Mortensen MB, Pless TK, Cribe A-S, de Muckadell OBS. Laparoscopic and percutaneous core needle biopsy plays a central role for the diagnosis of Autoimmune Pancreatitis in a single-center study from denmark. Pancreas. 2015;44(6):845-58.
- Kahriman G, Ozcan N, Dogan S, Ozmen S, Deniz K. Percutaneous ultrasound‐guided core needle biopsy of solid pancreatic masses: Results in 250 patients. J Clin Ultrasound. 2016;44(8):470-3.
- Xu K, Zhou L, Liang B, Niu L, Zheng X, Xu J, et al. Safety and accuracy of percutaneous core needle biopsy in examining pancreatic neoplasms. Pancreas. 2012;41(4):649-51.