Research Article
Recognition and Management of Traumatic Massive Hemothorax: Evaluation of 67 Cases
Murat Oncel*, Guven Sadi Sunam and Huseyin Yildiran
Department of Thoracic Surgery, Selcuk University, Konya, Turkey
*Corresponding author: Murat Oncel, Department of Thoracic Surgery, Selcuk University, Faculty of Medicine, Konya, Turkey
Published: 13 Jul 2017
Cite this article as:
Abstract
Background: As clinical presentation of massive hemothorax, patients are usually admitted to the
emergency units after thoracic trauma. We evaluated treatment approaches of patients with massive
hemothorax of comparation of 67 cases.
Methods: The 67 patients (53 males and 14 females) who were treated with diagnosis of massive
hemothorax in Konya Numune Hospital and Selcuk University, Hospital of Faculty of Medicine
between 2004 and 2015 years were retrospectively studied. An accumulation of more than 1500 cc
of blood in the pleural cavity, a homogeneous opacity more than half of a hemothorax on the chest
radiograph and computed tomography (CT), or ongoing drainage and hemodynamic instability in
patients were defined as massive hemothorax. Chi-square test was used for comparison of nominal
data.
Results: Hemothorax was associated with blunt thoracic trauma in 39 (59%) patients and with
penetrating trauma in 28 (41%) patients. Extra thoracic accompanying organ injuries were present
in 22 cases and extremity fractures were seen most frequently. Thoracic tube drainage was performed
in 34 blunt trauma and 15 penetrating trauma cases, emergency surgery was performed in 1 blunt
trauma case and 12 penetrating trauma cases.
Conclusion: Tube thoracostomy were found to be significant for massive hemothorax whether due
to blunt or penetrating trauma, and proposed as a first-line therapeutic approach.
Keywords: Hemothorax; Chest tube; Thoracotomy; Thoracic injuries
Introduction
The massive hemothorax developing after the thoracic trauma for which patients are usually admitted to the emergency units are mostly associated with blunt and penetrating trauma [1]. The exact incidence of massive hemothorax is not known. Chest injuries occur in approximately 60% of all polytrauma cases and hemothorax is most frequently caused by chest trauma. Generally, massive hemothorax can be divided into two categories, based on aetiology: penetrating and blunt chest trauma. In this study, we aimed to compare treatment approaches for the hemothorax developed after blunt trauma and developed after penetrating trauma.
Materials and Methods
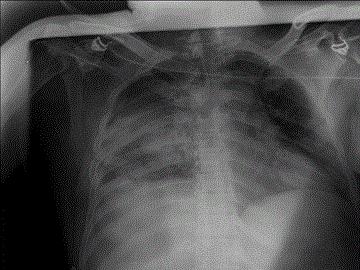
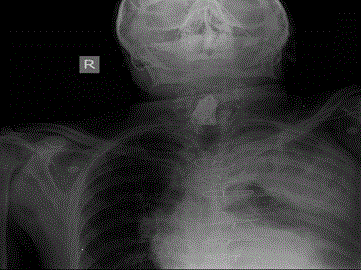
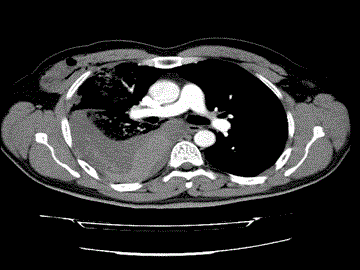
The files of 67 patients including 53 (79%) males and 14 (21%) females who were treated with a diagnosis of massive hemothorax in Konya Numune Hospital, Department of Thoracic Surgery and Selcuk University Faculty of Medicine, Department of Thoracic Surgery between the years of 2004 and 2015 were retrospectively studied. This study, the cases with a) an accumulation of more than 1500 cc of blood in the pleural cavity, b) a homogeneous opacity more than half of a hemothorax on the PA chest radiograph and CT, c) ongoing drainage and hemodynamic instability in patients with a diagnosis of hemothorax were defined as massive hemithorax (Figure 1-3). The diagnosis was confirmed with the presence of unclotted blood from pleural fluid on thoracentesis. The thoracic ultrasounographic (USG) and CT studies were conducted in patients with good general status and stable vital signs. In addition, routine blood tests were performed. The blood for transfusion was prepared until the insertion of the thoracal tube, and adequate blood replacement was then applied in all cases. In addition, as the first therapeutic approach, a 32F chest tube was inserted at the intersection of sixth or seventh intercostal space and mid- or posterior-axillary line of the chest with hemothorax. The presence of and trend of continuing an acute bleeding of 1500 mL from the tube inserted, and bleeding of more than 150 mL to 200 mL per 4 h were considered as an indication for emergency thoracotomy. The tube thoracostomy was terminated upon the end of heamorrhagic drainage or the serious transformation of the drainage that was fall below 50 ml/day. Postoperative and followup complications were recorded. Patients with a stable condition were discharged after 24-48 h of the removal of the tube. Patients were followed-up at outpatient clinic after discharge. The data were summarized as mean ± standard deviation and percentages. Multiple comparisons were performed with Mann-Whitney U test. Kruskal- Wallis analysis of variance was performed for the comparison of more than two groups. Binary comparisons were conducted with Mann-Whitney U test with Bonferroni correction for parameters differed significantly. Chi-square test was used for comparison of nominal data. Significance level was considered as 0.05.
Figure 1
Figure 2
Figure3
Results and Discussion
The youngest case was 19 years old, the oldest patient was 89 years
old, and the mean age was 36, 8 years. Demographics for the study
cohort analysis in Table 1. The mean age was 45.97 ± 13.6 among
patients with blunt trauma and 32.11 ± 7.48 among patients with
penetrating trauma. The mean age of patients with penetrating trauma
were significantly lower (p=0.000). There was no significant difference
between the two groups in terms of gender, and the penetrating
trauma was often occurred at an early age. 39 (58.2%) patients had
right hemothorax, 26 (38,8%) patients had left hemothorax, and 2
(2.9%) patients had bilateral hemothorax. No statistical difference was
found between penetrating hemothorax cases and blunt hemothorax
cases in terms of thoracic side. Hemothorax was associated with blunt
thoracic trauma in 39 (58%) patients and with penetrating trauma
in 28 (42%) patients. While traffic accidents were the most common
cause of blunt trauma, gunshot injuries were the most frequent
cause of penetrating trauma. Extrathoracic accompanying organ
injuries were present in 22 cases. In these cases, extremity fractures
were seen most frequently. Thoracic tube drainage was performed
in 34 blunt trauma cases and 15 penetrating trauma cases, thoracic
tube drainage with emergency surgery was performed in 1 blunt
trauma cases and 12 penetrating trauma cases and elective surgery
was performed in 4 blunt trauma cases and 2 penetrating trauma
cases. The rate of thoracic tube drainage and emergency surgery was
significantly higher in blunt thoracic trauma cases than penetrating
thoracic trauma cases (p. 0.001). A total of 9 patients (including 3
cases of blunt trauma and 6 cases of penetrating trauma) died. 2 of
3 blunt trauma cases died due to pulmonary embolism, whereas 1
patient died due to respiratory failure. In addition, 6 patients with
penetrating trauma died due to cardiac arrest. The mean length of
hospital stay (at department of thoracic surgery) was found as 7 days.
Massive hemothorax often develops after blunt or penetrating
trauma. The most common cause of blunt trauma is traffic accidents.
Fall, compression injury and direct thoracic trauma are the other
causes of blunt trauma. Hemothorax is associated with injuries
of the lung or intercostal vessels caused by the broken rib ends as
a result of rib fractures frequently occurring in blunt trauma. An
isolated chest trauma is not commonly seen [2,3]. The assessments
conducted by several authors have emphasized that the incidence
of extrathoracic organ injuries that accompany thoracic injuries is
not low [4]. Although our results showing that 22 (32,8%) patients
had accompanying injuries are compatible with the literature,
extrathoracic organ injuries were found not to be the determinant
of prognosis, but to have effects only on morbidity. The spectrum of
blunt chest traumas can range from rib fractures to the complicated
tracheobronchial injuries and cardiovascular ruptures [5-7]. Several
studies revealed that more than 25% of deaths resulting from
trauma were due to chest trauma and realized at the scene. The most
important causes are cardiac and great vessel injuries. Patients with
thoracic trauma can be treated with rapid resuscitation, effective
diagnostic tests, and simple applications [8].
The patient with shock caused by massive hemothorax should
first be underwent volume replacement, and adequate ventilation
should be provided for the elimination of hypoxia. A large-scale
cannula is placed in one of the peripheral veins in order to perform
saline and blood infusions. Central venous catheters are inserted for
blood pressure measurements. Because massive hemothorax cases
often require emergency thoracotomy, operating room together
with operating personnel and equipment should be prepared for a
potential thoracotomy [4,9]. For our three hemothorax cases with
penetrating trauma, 112 emergency ambulance team performed
the first intervention at the scene and then warned the hospital, so operating room and equipment have been ready to advance. The
patients were then admitted to the operating room without admitting
to the emergency department and underwent an emergency operation
under the respiratory and circulatory support. Therefore, these three
cases could be rescued. One of the cases was interesting because of 17
stab wounds that penetrated the thorax. In one case of a penetrating
hemithorax, intensive saline supplementation was performed while
being transferred with a peripheral vascular access. The patient was
arrested in the emergency department and emergency thoracotomy
was therefore performed. A clamp was placed on the pulmonary
hilum and the operation was continued in the operating room.
Thoracotomy, sternotomy and major surgical procedures are
required in 10% of blunt trauma cases and 15% to 30% of penetrating
trauma cases, whereas emergency thoracotomy is required in only
1% to 2% of blunt trauma cases [8]. In the present study, emergency
thoracotomy was required in 2 (3%) blunt trauma cases and 11 (16%)
penetrating trauma cases.
The generally accepted mode of treatment in traumatic
hemothorax is thoracic tube implementation [9]. The blood
accumulated in intrapleural space is drained in this way. The risk of
fibrothorax and empyema is minimized. Ventilation improves with
expansion of the lung, and ongoing bleeding decreases and stops
with the convergence of visceral and parietal pleura. If the bleeding
persists, the decision of how the treatment will continue is made by
following hourly and daily amounts of drainage. Thoracotomy should
immediately be implemented in patients with ongoing bleeding and
hemodynamic instability. The rate emergency thoracotomy has a
range as wide as 10% to 71% [10]. In our study, 13 (19%) patients
underwent emergency thoracotomy. Thoracal tube had initially been
inserted in all these cases. The most frequent pathologies associated
with thoracotomy were parenchymal and cardiac injuries that were
seen in 12 cases. In our study, lower rate of emergency thoracotomy
indicates the priority of thoracal tube treatment to emergency
thoracotomy.
Penetrating injuries of the thorax depends on the type of and path
followed by the penetrating object in the thorax. In daily life, lowspeed
bullet and stab injuries are the most common causes leading
to penetrating injuries. The amount of bleeding and severity of the
clinical picture are higher especially in cases of high acceleration
gunshot wounds than swab injury cases. Parenchymal injuries can
often be treated with tube thoracostomy, whereas hemothoraxes
originated from intercostal veins or internal mammary arteries
usually require thoracotomy. Intercostal arteries were most frequently
injured vascular structures in penetrating chest trauma cases [9,10].
The lung parenchyma is also damaged. These injuries also present
with hemothorax. Bleeding in these cases is often self-terminated.
However, thoracotomy may be required in cases of persistent
bleeding. Pulmonary resection may be required; if there is excessive
parenchymal damage and inadequate expansion of relevant lung area
in the exploration after control of bleeding from the lung parenchyma
in thoracotomy [11]. Lower lobe segmental resection was performed
in one gunshot injury case, whereas upper lobe anterior segmental
resection was performed in blunt chest trauma case.
The majority of hemothoraxes that developed after a chest trauma
are injuries that require no major thoracotomy intervention and can
be treated with tube thoracostomy. However, the rate of clot retention
is 2 to 30% in treatments of hemothorax performed only with tube
thoracostomy, inadequate drainage of post-traumatic hemothorax
may lead to complications such as fibrothorax or empyema, which
require thoracotomy [12]. However, the rate of clot retention is
2% to 30% in treatments of hemothorax performed only with tube
thoracostomy, inadequate drainage of post-traumatic hemothorax
may lead to complications such as fibrothorax or empyema, which
require thoracotomy [13,14].
In our study, a total of 67 cases underwent emergency tube
thoracostomy and were then taken under follow-up, and tube
thoracostomy treatment was found to be sufficient in 48 (71,6%)
cases. Only 17 (25,3%) cases underwent additional emergency and
elective surgical treatments, and the rate of clotted hemothorax or
empyema was 5%. It is interesting that this rate can be as high as
30% in the literature. There are some publications indicating that
prophylactic use of antibiotics is effective in reducing the risk of
empyema. Empyema, fibrothorax and chronic atelectasis requires the
thoracotomy for the management of organized hemothorax [1,5,7,9].
VATS drainage is recommended during the post-traumatic first
week to 10 days that corresponds to the period of reduced risk of rebleeding
from the injured lung. In such cases, PA chest radiographs
may not provide sufficient information at any time. Therefore, surgical
intervention (VATS) is recommended following a CT evaluation. Liu
et al. have treated 56 patients with clotted hemothorax occurred after
blunt chest trauma by VATS drainage [15] They have applied VATS
drainage to hemodynamically stable patients without cardiovascular
and major vascular injuries, and reported no morbidity and mortality.
Meyer et al. [16] compared VATS and the second tube
thoracostomy applications in their prospective study on 39 patients
with clotted hemothorax. They have reported that tube thoracostomy
is more practical and inexpensive method, but may not be effective,
so may be require additional surgical procedures, may lead to a longer
hospital stay. They have also drawn attention to that thoracotomy is
an effective but invasive procedure, and to the existence of potential
complications. In addition, they found that VATS is a less invasive
procedure, can treat patients more effectively and more quickly,
and is associated with a shorter hospital stay [17-19]. Organized
hemothorax cases underwent decortication surgery within 3 to 5
weeks regardless of an accompanying infection. This waiting period
has two advantages:
1. The patient will gain time to heal injuries of the other
organs if any, and will have more stable heamodynamic status. The
possibility of surgery will descend to the lowest level.
2. Organized hemothorax can regress spontaneously and may
not need surgical intervention.
Operative mortality rate varies from 0% to 5% in most series
[12,16]. Postoperative complications are bleeding and prolonged
air leakage. After decortication, re-expansion is achieved in patients
with a normal lung parenchyma. Although some cases can have
radiological findings of closed costodiaphragmatic sinus and pleural
thickening in post-operative follow-up period, these findings have no
significance and a full expansion can be achieved with resolution after
several months [1,13,15,17,20].
Table 1
Conclusion
Tube thoracotomy were found to be significant for massive hemothorax whether due to blunt or penetrating trauma, and proposed as a first-line therapeutic approach. Attention has been drawn to the use of VATS drainage in isolated massive hemothorax cases in various publications in recent years. We did not use VATS drainage as can be seen in our clinical study. Because it has been identified that most cases planned for surgery for massive hemothorax had an unstable status and that cardiac and great vessel injuries occurred after thoracotomy. Therefore, the use of VATS would increase the mortality. In addition, it was not possible to perform the decortication surgery with VATS method because of excessive adhesions in patients underwent elective decortication surgery.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
References
- Wilson JM, Boren CH, Peterson SR, ThomasAN. Traumatic hemothorax: Is decortication necessary? J Thorac Cardiovasc Surg.1979;77(4):489-95.
- Tatou E, Steinmetz E, Jazayeri S,Benhamiche B, Brenot R, David M. Surgical outcome of traumatic rupture of thethoracic aorta. Ann Thorac Surg. 2000;69(1):70-3.
- Broos PL, D’Hoore A, Vanderschot P,Rommens PM, Stappaerts KH. Multiple trauma in patients of 65 and over. Injurypatterns. Factors influencing outcome. The importance of an aggressive care.Acta Chir Belg. 1993;93(3):126-30.
- Richardson JD, Miller FB, Carrillo EH,Spain DA. Complex thoracic injuries. Surg Clin North Am. 1996;76(4):725-48.
- BlaisdellFW. Pneumothorax and hemothorax. In: Blaisdell FW, Trunkey DD, eds.Cervicothoracic Trauma. 2nd ed. New York: Thieme Medical Publishers;1994;228-34.
- Karmy-Jones R, Jurkovich GJ,Nathens AB, Shatz DV, Brundage S, Wall Jr MJ, et al. Timing of UrgentThoracotomy for Hemorrhage After Trauma: A Multicenter Study. Arch Surg. 2001;136(5):513-8.
- Boersma WG, Stigt JA, Smit HJ. Treatmentof haemothorax. Respir Med. 2010;104(11):1583-7.
- Cothren CC,Moore EE. Emergency department thoracotomy for the critically injured patient:Objectives, indications and outcomes. World J Emergency Surg. 2006;24:1-4.
- Maloney JV Jr. The conservativemanagement of traumatic hemothorax. Am J Surg. 1957;93(4):533-9.
- Robison PD, Harman PK, Trinkle JK,Grover FL. Management of penetrating lung injuries in civilian practice. JThorac Cardiovasc Surg. 1988;95(2):184-90.
- Kish G, Kozloff L, Joseph WL, Adkins PC.Indications for early thoracotomy in the management of chest trauma. Ann ThoracSurg. 1976;22(1):23-8.
- Menger R, Telford G, Kim P,Bergey MR, Foreman J, Sarani B, et al. Complications following thoracic traumamanaged with tube thoracostomy. Injury. 2012;43(1):45-50.
- Jerjes-Sánchez C, Ramirez-Rivera A,Elizalde JJ, Delgado R, Cicero R, Ibarra-Perez C, et al. Intrapleuralfibrinolysis with streptokinase as an adjunctive treatment in hemothorax and empyema:a multicenter trial. Chest. 1996;109(6):1514-9.
- Coselli JS, Mattox KL, Beall AC Jr.Reevaluation of early evacuation of clotted hemothorax. Am J Surg.1984;148(6):786-90.
- Liu DW, Liu HP, Lin PJ, Chang CH.Video-assisted thoracic surgery in treatment of chest trauma. J Trauma.1997;42(4):670-4.
- Meyer DM, Jessen ME, Wait MA, Estrera AS.Early evacuation of traumatic retained hemothoraces using thoracoscopy: aprospective, randomized trial. Ann Thorac Surg. 1997;64(5):1396-400.
- Fabbrucci P, Nocentini L, SecciS, Manzoli D, Bruscino A, Fedi M, et al. Video-assisted thoracoscopy in theearly diagnosis and management of post-traumatic pneumothorax and hemothorax.Surg Endosc. 2008;22(5):1227-31.
- Çobanoglu U, Sayir F, Mergan D[Should videothorascopic surgery be the first choice in isolated traumatichemothorax? A prospective randomized controlled study]. Ulus Travma AcilCerrahi Derg. 2011;17(2):117-22.
- Smith JW, Franklin GA, Harbrecht BG,Richardson JD. Early VATS for blunt chest trauma: a management techniqueunderutilized by acute care surgeons. J Trauma. 2011;71(1):102-5.
- Wells BJ, Roberts DJ, Grondin S,Navsaria PH, Kirkpatrick AW, Dunham MB, et al. To drain or not to drain?Predictors of tube thoracostomy insertion and outcomes associated with drainageof traumatic hemothoraces. Injury. 2015;46(9):1743-8.