Case Report
Survival Rate Following Trans Metatarsal Amputation: A Five-Year Retrospective Review
Georgeanne Botek1*, Fernando Cruz2, Christopher Tulodzieski2 and Tammy Owings Deng1
1Department of Podiatry, Mercy Regional Medical Center, USA
2Department of Podiatry, Cleveland Clinic Foundation, USA
*Corresponding author: Georgeanne Botek, Department of Podiatry, Mercy Regional Medical Center, Cleveland, OH 44195, USA
Published: 07 Jul 2017
Cite this article as: Botek G, Cruz F, Tulodzieski C, Deng
TO. Survival Rate Following Trans
Metatarsal Amputation: A Five-Year
Retrospective Review. Clin Surg. 2017;
2: 1550.
Abstract
Background: The aim of this study is to examine the five-year mortality rate, after a Tran’s metatarsal
amputation (TMA), in comparison to reported mortality rates of a below-knee amputation (BKA).
This study also analyzes disease(s) that increase mortality.
Methods: The records of patients who underwent TMA at the Cleveland Clinic by podiatric surgery
between 2009 to 2011 were retrospectively reviewed. Records were evaluated for mortality status,
age, and co-morbidities.
Results: A total of 129 post-TMA patients were investigated, 90 males (69.7%) and 39 females
(30.2%) with the mean age of 62 (20-91). Of 129 patients, 54 were deceased (41.8%), with 33% of
the population expiring within the first 12 months of the TMA. Co-morbidities included diabetes
(79%), hypertension (90%), PVD (53%), CAD (36%), previous foot amputation (30%), neuropathy
(68%), and renal disease (45%). Compared to the other diseases, there were more deceased patients
who suffered from renal diseases (57%).
Conclusion: Following TMA procedure, there is a 39%, 5-year mortality rate, compared to 40%
to 82%, after BKA. This demonstrates the differences in mortality of major versus minor limb
amputation, with TMAs increasing patient longevity. Thus, this limb salvage procedure should be
considered when applicable. Also, mortality in patients with renal disease was higher compared to
other diseases.
Keywords: Tran’s metatarsal amputation; Mortality; HTN; PVD
Introduction
According to Effeney et al. [1], Tran’s metatarsal amputation (TMA) was first described in 1855, but did not experience widespread acceptance until the mid 20th century. At that time, the use of the procedure increased for the treatment of distal pedal gangrene. Prior studies have shown that more proximal lower extremity amputations are associated with poorer survival rates, than amputations performed at more distal sites, including TMA. The five-year survival rate for below-knee amputation (BKA) varies among the literature, ranging as low as 28% up to 82% [2]. However, the authors are unaware of any similar study reporting the 5-year survival rate of patients after TMA, although a 79% estimate for survival rate after mid-foot amputation was extrapolated by Izumi et al [3]. Decreased survival rates in cases of both proximal and distal lower extremity amputation are associated with patient co-morbidities. Through retrospective review, we sought to evaluate prognosis for survival, by determining 5-year survival rates among patients who underwent TMA. Additionally, we sought to evaluate the impact of co morbidities.
Methods
With the institutional review board approval, a retrospective review of electronic medical records (EMR) of patients who underwent ‘Trans metatarsal Amputation,’ within the Cleveland Clinic System, between 2009-2011, was performed. The only exclusion criterion was patients who had a TMA, secondary to cancer. The date of death was recorded from the hospital’s EMR and/or through search of the patient’s obituary. The patient’s gender and the date of surgery, in comparison to date of expiration, were investigated. The specific co-morbidities recorded included diabetes (DM), neuropathy, hypertension (HTN), peripheral vascular disease (PVD), coronary artery disease (CAD), cerebro vascular accident (CVA), renal disease, smoking status, previous amputation, and higher amputation (BKA/AKA) after TMA. The hemoglobin A1c (HbA1c) of diabetic patients prior to surgery, the Glomerular Filtration Rate (GFR) for patients with Chronic Kidney Disease (CKD)/Acute Kidney Insufficiency (AKI)/ Renal insufficiency (RI), and the ambulation status after surgery, were inspected.
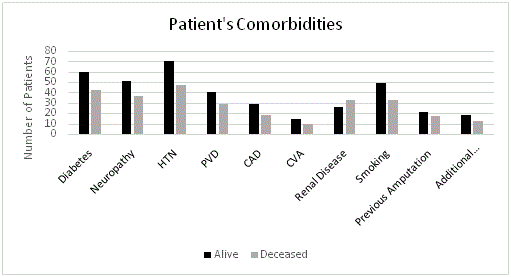
Graph 1
Table 1
Results
There were a total of 129 patients, 90 males (69.7%) and 39 females (30.2%). Patients’ age range from 20-91, with a mean age of 62. In the Cleveland Clinic system, 11 different facilities performed TMA procedures; 30 procedures were performed in 2009 (23.25%), 59 in 2010 (45.7%), and 40 in 2011 (31.0%). None of the patients qualified for the exclusion criterion. The co-morbidities for each patient were examined and the values were compared to those of patients deceased (Table 1 and Graph 1). More than 50% of patients were diabetic (79.1%) and smokers (62.3%). The majority of patients had neuropathy (68.2%), HTN (89.9%) and PVD (52.7%). Only 29.5% of patients had limb amputations, prior to TMA. Of the 58% of patients with renal diseases, there were 32 with End Stage Renal Disease (ESRD) (55.2%), 15 CKD (25.9%), eight AKI/Renal insufficiencies (13.8%), and three kidney transplants (5.2%). Thirty-one patients (24.03%) had higher amputations after TMA with26 BKAs and five AKAs. After TMA, 102 patients ambulated (79.1%). In surveying the deceased population, there were more patients that expired with renal disease (56.89%). Also, the majority of departed patients were deceased within the first year post TMA (33.3%). Only 9.3% of the departed patients lived past 5 years (Table 2). Sixty-five of the 102 DM patients (63.7%) had a documented HbA1c, with an average of 8.2%. Nineteen of the 42 deceased DM patients (45.2%) had a documented HbA1c with an average of 6.8%. The average estimated GFR was 82.2, in patients with CKD/AKI/Renal insufficiency.
Table 2
Discussion
The only article cited that examined mortality with TMAs was Thomas et al. in 2001 [4]. The findings revealed 17%, 30-day mortality after TMA and 10%, 1-year mortality, which is lower compared to our findings of 14%, 1-year mortality. However, their sample size was 41 patients and they only examined diabetics versus non-diabetic patients. Wiessman et al. [5] found 31.7%, 1-year all-cause mortality with minor amputations, which was considered below ankle amputations. Izumi discovered a 10.5%, 10-month mortality with initial mid-foot amputation. Also, in distal amputees, CVD, CAD and ESRD were strongly associated with death. All lower extremity amputation runs the risk of early post-operative mortality, averaging between 4% to 22%, but more proximal the level of amputation, the greater the risk of unfavorable outcomes [6]. Proximal amputation causes immediate loss of preload, which leads to cardiac overwork. Below the knee amputation has a greater negative effect on the survival rate because the preload loss depends on the volume of tissue loss. Many studies surveying morality after BKA were reviewed. Throud had the most updated statistics, demonstrating the range of mortality after BKA was 40% to 82% and after AKA was 40% to 90%. Our study found following TMA, there is 39%, 5-year mortality, which is greatly lower than documented BKA rates. Also, the mortality in renal patients was higher compared to other diseases. In any lower extremity amputation, surgeons consider the decision to undergo the procedure and subsequently the level of surgery. The decrease in life span with a more proximal amputation, in the setting of extensive co-morbidities, should be considered in surgical decision-making process. This study attempts to define the potential value that may improve the process of care for patients and increase longevity in patients with limb-threatening circumstances, in major versus minor limb amputation.
References
- Effeney DJ,Lim RC, Schecter WP. Trans metatarsal amputation. Arch Surg. 1977;112(11):1366-70.
- ThorudJC, Jupiter DC,Lorenzana J, Nguyen TT, Shibuya N.Reoperation and Reamputation after Trans metatarsal Amputation: A SystematicReview and Meta-Analysis. J FootAnkle Surg. 2016;55(5):1007-12.
- Izumi Y, Satterfield K, Lee S, Harkless LB, Lavery LA. Mortality offirst-time amputees in diabetics: a 10-year observation. Diabetes Res Clin Pract.2009; 83(1):126-31.
- Thomas SR, Perkins JM, Magee TR, Galland RB. Transmetatarsal amputuation:an 8-year experience. Ann R Coll Surg Eng. 2011;83(3):164-6.
- WiessmanMP, Liberty IF, Segev RW, Katz T, Tailakh, Novack V. Clinical characteristicsand survival of patients with diabetes mellitus following non-traumatic lowerextremity amputation. IMAJ. 2015;17(3):145-9.
- vanNettenJJ, Fortington LV, Hinchliffe RJ, Hijmans JM. Early Post-operative Mortality afterMajor Lower Limb Amputation: A Systematic Review of Population and Regional Based Studies. Eur J VascEndovasc Surg. 2016;5(2):248-58.