Case Report
Surgical Treatment of Peroneus Brevis Tendon Repair with and without Human Amniotic Allograft: A Comparison Study
J Joseph Anderson1, Adebola T Adeleke1*, Brittany Rice2 and Zflan Swayzee1
1Department of Podiatric Surgery, American Foundation of Lower Extremity Surgery and Research, Alamogordo,
NM, USA
2Department of Podiatric Surgery, Scripps Mercy Hospital, San Diego, CA, USA
*Corresponding author: Adebola T Adeleke, Department of Podiatric Surgery, American Foundation of Lower Extremity Surgery and Research, 2301 Indian Wells Dr. Suite A, Alamogordo, NM, 88310, USA
Published: 15 Jun, 2017
Cite this article as: Anderson JJ, Adeleke AT, Rice B,
Swayzee Z. Surgical Treatment of
Peroneus Brevis Tendon Repair with
and without Human Amniotic Allograft:
A Comparison Study. Clin Surg. 2017;
2: 1515.
Abstract
Surgically repairing peroneus brevis tendon tears include postoperative complications such as
adhesions, which is concerning given the period of postoperative immobilization. The use of human
amniotic allograft (HAA) has been found to have anti-microbial, anti-fibrotic, anti-inflammatory,
and analgesic properties. These benefits may help decrease postoperative adhesions and pain.
All patients included in the study (129) were surgically treated for longitudinal peroneus brevis
tendon tear. The procedure included the Triad procedure (ankle arthroscopy, lateral ankle ligament
reconstruction, and peroneal retinacular tightening), tubularization of the tendon, and debridement
of low lying peroneus muscle belly, if present. Some patients (58) had their repair augmented
with HAA, while others (71) did not. There was no significant between the two groups in terms
of gender, age and modified American College of Foot and Ankle Surgeons hindfoot and ankle
scores preoperatively or pain scores preoperatively. There was significance in postoperative physical
therapy times between the control group (7.01 weeks) to the graft group (5.21 weeks) (p < 0.001).
Mean postoperative visual analog scales between the human amniotic allograft and control group
were 1.24 and 1.62 respectively and also rendered statistically significant (p< 0.001). The authors
found the use of human amniotic allograft to be a viable and effective adjunct in peroneal tendon
repair with reduced postoperative pain, physical therapy time with minimal or no associated
complications.
Keywords: Tendon repair; Triad procedure; Dehydrated placental allograft
Introduction
Peroneus brevis tendon tears often present as lateral ankle pain and instability caused by
mechanical or anatomical factors. Since first reported by Myers in 1924, its prevalence today is not
always considered. Longitudinal peroneus brevis tears have been reported to be between 11% and
37% with significant lateral ankle injuries [1-4]. Tears of the peroneus brevis tendon are frequently
overlooked leading to misdiagnosis and mistreatment. Dombek et al. [5] found that only 60% of
peroneal tendon disorders were accurately diagnosed at first visit. Tears and ruptures are commonly
associated with other disorders including chronic ankle instability, inversion ankle sprains,
tenosynovitis, and ankle fractures [6,7].
Proper treatment of these injuries requires an understanding of potential anatomical
abnormalities that may contribute to this pathology. The anatomical position of the peroneus
brevis tendon predisposes the tendon to shear stress due to its location between the distal fibula
and the peroneus longus tendon [8]. A flat or convex retro-malleolar groove, low lying muscle belly,
peroneus quartus, rearfoot varus, procurvatum ankle, posterior lateral fibular spurring, and superior
peroneal retinaculum incompetence are additional anatomical abnormalities that can contribute to
weakening of the peroneus brevis tendon [2,5,9-12].
Surgical treatment options for peroneus brevis tendon tears may include one or more of the
following: primary repair of the tendon, debridement, excision of tendon with tubularization,
tenodesis, tendon transfer, lateral ankle ligament reconstruction, repair using allograft, peroneal
sulcus deepening, or superior peroneal retinaculum repair [2,6,13-17]. More than one procedure
is often performed to sufficiently address the tear and its concurrent anatomical abnormalities as
mentioned above.
Human amniotic allograft (HAA) is a commercially available
product that is composed of human amniotic membrane. Although
the use of HAA in peroneal tendon repair has been minimally
reported in the literature, it is well documented in its use for many
other clinical procedures. Over the past 100 years, HAA has been
used in chronic wounds, burns, tendon repair, nerve repair, corneal
repair, intra-oral reconstruction, hip arthroplasty, microvascular
grafts, genital reconstruction, peritoneal reconstruction, dural
defects, skin reconstruction, intra-abdominal adhesions, talar dome
lesions, calcaneal osteotomies, and reconstruction of nasal lining
and tympanic membranes [18-24]. Several studies have shown that
HAA contains an array of growth factors, cytokines and proteins that
contribute to its analgesic, anti-microbial, and anti-inflammatory
properties [18-20,25-27]. The primary glycosaminogly can present in
amniotic allograft is high molecular weight hyaluronic acid, which has
been shown to decrease adhesions and fibrosis; therefore, helping with
the reduction of scars [18-20,23,25,28-31]. HAA is immunologically
inert, eliminating the risk for host rejection. Each tissue specimen
undergoes a thorough screening process for relevant communicable
diseases and is sterilized [32]. The pluripotent property of the cells
found in human amniotic allograft allows for potential regeneration
into different tissue types such as cartilage, bone, muscle, or tendon
[19,21,27]. All of these qualities of HAA have made it a suitable
product for a variety of foot and ankle pathologies.
There are currently no outcome studies on surgical treatment
recommendations for peroneus brevis tendon tears. Publications on
the use of allograft in the treatment of peroneal tendon tears are also
sparse and limited to a few published case reports. The purpose of this
study is to report comparative outcomes of peroneus brevis tendon
tear repairs using human amniotic membrane allograft versus a
control group without HAA and to present any significant differences
found. The authors hypothesize that the analgesic, anti-microbial,
anti-inflammatory and adhesion reducing properties of HAA
will result in functional preservation, reduced rehabilitation time,
reduced postoperative pain, minimal complications and increased
patient satisfaction as opposed to control group.
Patients and Methods
A total of 368 ankle arthroscopy cases that underwent the
Triad procedure were reviewed from January 2006 to May 2013.
Each patient was treated operatively by a single surgeon (JJA). All
patients with talar osteochondral defects, peroneus longus pathology,
previous ankle surgery, diabetes, BMI over 30.1, subtalar joint
pathology and inadequate follow-up were excluded. The final patient
cohort consisted of 129 consecutive Triad cases, 58 with HAA used at
the peroneus brevis repair site and 71 without (control). All patients
had history of injury to the ankle with continued pain, instability, and
inability to perform regular activity including exercise and sports.
All patients failed conservative care that included bracing, NSAIDS,
rest, and immobilization a minimum of 4 weeks of physical therapy.
Patients received physical therapy preoperatively and postoperatively.
The operative procedure included a peroneus brevis tendon repair
using tubularization, and excision of low lying muscle belly with the
Triad surgical procedure, which consists of ankle joint arthroscopy,
lateral ankle ligament reconstruction and peroneal retinacular
tightening [33]. The human amniotic allograft was then wrapped
around the peroneus brevis repair site prior to repair of the peroneal
retinaculum in the HAA group. Primary outcomes were patient
satisfaction using a preoperative and postoperative visual analog scale
(VAS), and modified American College of Foot and Ankle Surgeons
(ACFAS) hind foot ankle score system. The ACFAS score was
modified for radiographic findings, which were converted to neutral
points preoperatively and postoperatively. The modified ACFAS
score was measured preoperatively as well as 3, 12 and 24 months
postoperatively. A paired T-test was used to determine statistically
significant findings between the preoperative and postoperative
scores.
Surgical technique
A standard anterior, lateral and medial ankle scope portal
approach was used. Any superficial chondritis, anterior lipping or
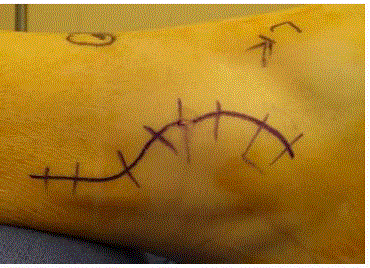
anterior pinch lesions were addressed. An 8 cm curvilinear incision
was made over the lateral portion of the ankle beginning 5cm posterior
to lateral malleolus and curving distally anterolateral to incorporate
the lateral portal and then posteriorly below the tip of the fibula for
the lateral ligament exposure (Figure 1). The incision was deepened
through soft tissue down to the level of the peroneal tendons. The
peroneal retinaculum was entered proximal to allow reattachment
and periosteum on the fibula to sew to. No anchors were used. Any
presence of a low-lying peroneus brevis muscle belly, accessory
tendon, and/or synovitis and redundant retinaculum were excised.
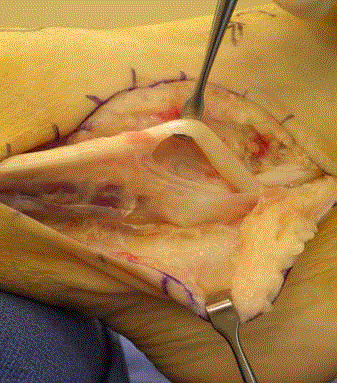
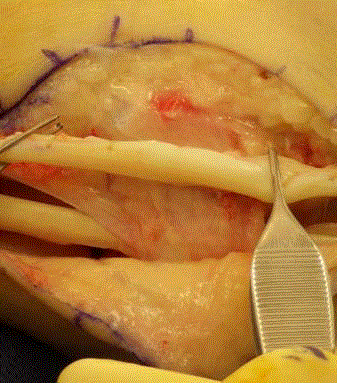
The longitudinal tears were repaired with direct tubularization of the
brevis (Figure 2 and 3).
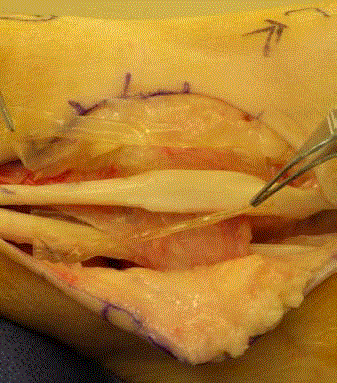
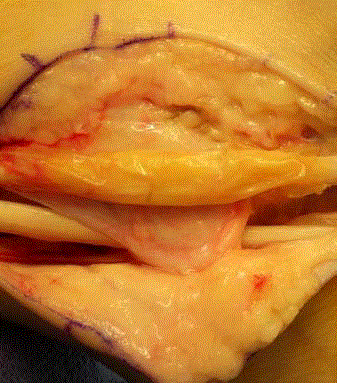
In the HAA group, human amniotic allograft* was wrapped
around the brevis and the peroneal retinaculum was re-approximated
and tightened. The peroneal tendons were then returned to their
retrofibular groove (Figure 4 and 5). Lastly, the anterior talofibular
ligament and calcaneofibular ligament were imbricated, repaired and
reinforced with the lateral slip of the extensor retinaculum. Skin was
closed in standard fashion with vicryl and nylon suture. An identical
procedure was performed in the control group without the use of
HAA.
*NuShield® protective patch, Nutech Medical, Inc., Birmingham,
AL.
Figure 1
Figure 2
Figure3
Figure 4
Figure 5
Results
The average ages of the HAA and control groups were 38.36 and
39.24 years, respectively. The sex of the patients were fairly evenly
split between males and females in the HAA (M=36, F=22) and
control (M=49, F=22) groups. The age ranges for the two groups
were 18-70 for the HAA group and 18-68 for control group. In both
groups, patients had comorbidities of hyperthyroidism, thyroid
disease, hypertension, diabetes and obesity. One additional patient
had coronary heart disease in the control group (Table 1).
Pre and postoperative VAS scores were 6.0 and 1.2 respectively in
the HAA while the control group had scores of 6.0 and 1.6. The preoperative
HAA and control VAS Score were not significantly different
(p=.89) but post-operative VAS scores were (p< 0.001) (Table 2).
The ACFAS scores were measured pre-operatively and postoperatively
at 3 months, 12 months and 24 months for every patient.
The average score for the HAA group was 72.69 pre-operatively, 89.42
at 3 months post-operatively, 91.46 at 12 months post-operative and
91.31 at 24 months post-operatively. The average score for the control
group was 72.08 pre-operatively, 87.50 at 3 months post-operatively,
90.08 at 12 months post-operative and 89.23 at 24 months postoperatively.
There was no significance between the pre-operative
scores of the HAA group and control group, but there was significant
improvement between the 3 month, 12 month and 24 month postoperative
scores, ( p <0.001, p< 0.001, p< 0.001 respectively). When preoperative
to post-operative comparisons were made, the differences
seen between HAA and control group was significant (p=0.012)
(Table 2).
HAA patients had a mean postoperative physical therapy time
of 5.21 weeks while control group subjects exhibited mean physical
therapy of 7.01 weeks, also a significant difference (p<0.001) (Table
2).
Postoperative complications (4.65%) included one patient
who developed complex regional pain syndrome and another who
experienced nerve entrapment in HAA group while two subjects
developed nerve entrapments in the control group and 2 more with
tissue scarring (Table 1).
Discussion
The results of the present study have demonstrated promising
outcomes for the use of HAA in surgical procedures to repair
peroneus brevis tendon tears. With a significant reduction in
postoperative pain and physical therapy time, minimal complications,
and zero postoperative infections, the results are consistent with
prior publications showing that the use of HAA in foot and ankle
procedures is safe. Since its first use in skin transplantation in the
early 1900s, there have been several studies showing its utility and
safety in foot and ankle surgeries [18,19,21-27]. Demill et al. [18]
published a retrospective study reporting the short-term outcomes
of cryopreserved amniotic membrane and umbilical cord tissue in
foot and ankle surgery. The authors reported 20 different surgical procedures that involved the use of amniotic allograft, with the most
common procedure performed being Achilles and peroneal tendon
repair. Of the 129 patients, the overall wound complication rate
was 4.65% with only 2.3% having continued pain at surgical site.
The authors found that the complication rate was much lower than
what was historically noted [18]. Anderson et al. [21] found that
using HAA in addition to micro-fracture for treatment of talar dome
lesions also helped decrease postoperative pain. In a retrospective
study, 37 patients with osteochondral lesions measuring 2 cm2 or
less were treated with micro-fracture and HAA. VAS scores and
modified AFCAS ankle scores were recorded preoperatively and
postoperatively and the authors reported a statistically significant
improvement in these scores with no identified complications.
Another study by Anderson et al. [24] reported the safety of HAA
in calcaneal osteotomies, which included 63 patients undergoing an
Evans calcaneal osteotomy with implantation of tri-cortical iliac crest
bone graft. The authors retrospectively reviewed all 63 patients with
a 2 year follow up and found that the use of HAA did not increase
the time to union or return to normal shoe gear for this procedure.
There were no documented wound dehiscence, nonunion, infection,
or immune reactions reported. Warner et al. [29] examined the safety
and efficacy of cryopreserved amniotic membrane and umbilical cord
in 14 patients undergoing complex reconstructive and/or revision
foot and ankle procedures. While the study sample was small, the
outcomes showed no complications directly related to the use of the
allograft, as well as a statistically significant improvement in pain and
function via the ACFAS score.
The results of this study have also have shown that the use of
HAA significantly improved pain as demonstrated by the decreased
VAS scores and physical therapy time. Within the HAA group,
significant ACFAS scores substantiate the efficacy of human amniotic
allograft in affecting patient outcomes with improved function and
movement at the 3 month, 12 month and 24 month postoperative
intervals. Postoperative adhesions in tendon surgery are of concern
to any foot and ankle surgeon due to range of motion limitations
which may alter the rehabilitation period and lead to continued pain
and immobility. The authors feel that wrapping the tendon in HAA
made a meaningful contribution to decreasing those complications
due to the fact that the subjects in this study who had HAA applied
showed significantly improved VAS scores and physical therapy time
as opposed to control group.
Table 1
Table 2
Conclusion
The clinical use of human amniotic allograft is steadily increasing in foot and ankle surgeries and additional larger, prospective studies will be useful in confirming its niche in the field. In conclusion, the present study has added to the growing body of research demonstrating the utility and safety of human amniotic allograft in foot and ankle surgery, specifically peroneal tendon repair. With its anti-microbial, anti-inflammatory, anti-fibrotic properties, human amniotic allograft affords numerous benefits to peroneal tendon repairs including pain reduction, shorter physical therapy utilization and minimal complications. HAA can prove to be an effective, cost sensitive adjunct in surgical repair of peroneal tendon repairs.
References
- Sobel M, DiCarlo EF, Bohne WH, Collins L. Longitudinal splitting of the peroneus brevis tendon: an anatomic and histologic study of cadaveric material. Foot Ankle. 1991;12(3):165-70.
- Sobel M, Geppert MJ, Warren RF. Chronic ankle instability as a cause of peroneal tendon injury. Clin Orthop Relat Res. 1993;296:187-91.
- Sobel M, Bohne WH, Levy ME. Longitudinal attrition of the peroneus brevis tendon in the fibular groove: an anatomic study. Foot Ankle. 1990;11(3):124-8.
- Freccero DM, Berkowitz MJ. The relationship between tears of the peroneus brevis tendon and the distal extent of its muscle belly: an MRI study. Foot Ankle Int. 2006;27(4):236-9.
- Dombek MF, Lamm BM, Saltrick K, Mendicino RW, Catanzariti AR. Peroneal tendon tears: a retrospective review. J Foot Ankle Surg. 2003;42(5):250-8.
- Heckman DS, Reddy S, Pedowitz D, Wapner K, Parekh SG. Operative Treatment for Peroneal Tendon Disorders. J Bone Joint Surg Am. 2008;90(2):404-18.
- Clarke HD, Kitaoka HB, Ehman RL. Peroneal tendon injuries. Foot Ankle Int. 1998;19(5):280-8.
- Major NM, Helms CA, Fritz RC, Speer KP. The MR imaging appearance of longitudinal split tears of the peroneus brevis tendon. Foot Ankle Int. 2000;21(6):514-9.
- Meyers AW. Further evidence of attrition in the human body. Am J Anat. 1924;34:241-67.
- Krause JO, Brodsky JW. Peroneus brevis tendon tears: pathophysiology, surgical reconstruction and clinical results. Foot Ankle Int. 1998;19(5):271-9.
- Sobel M, Geppert MJ, Olson EJ, Bohne WH, Arnoczky SP. The dynamics of peroneus brevis tendon splits: a proposed mechanism, technique of diagnosis, and classification of injury. Foot Ankle. 1992;13(17):413-22.
- Geller J, Lin S, Cordas D, Vieira P. Relationship of a low-lying muscle belly to tears of the peroneus brevis tendon. Am J Orthop (Belle Mead NJ). 2003;32(11):541-4.
- Raply JH, Crates J, Barber A. Mid-substance peroneal tendon defects augmented with an acellular dermal matrix allograft. Foot Ankle Int. 2010;31(2):136-40.
- Mook WR, Parekh SG, Nunley JA. Allograft reconstruction of peroneal tendons: operative technique and clinical outcomes. Foot Ankle Int. 2013;34(9):1212-20.
- Ozbag D, Gumusalan Y, Uzel M, Cetinus E. Morphometrical features of the human malleolar groove. Foot Ankle Int. 2008;29(1):77-81.
- Steel MW, DeOrio JK. Peroneal tendon tears: return to sports after operative treatment. Foot Ankle Int. 2007;28(1):49-54.
- Demetracopoulos CA, Vineyard JC, Kiesau CD, Nunley JA 2nd. Long-term results of debridement and primary repair of peroneal tendon tears. Foot Ankle Int. 2014;35(3):252-7.
- DeMill SL, Granata JD, McAlister JE, Berlet GC, Hyer CF. Safety Analysis of Cryopreserved Amniotic Membrane/Umbilical Cord Tissue in Foot and Ankle Surgery: A Consecutive Case Series of 124 Patients. Surg Technol Int. 2014;25:257-61.
- Niknejad H, Peirovi H, Jorjani M, Ahmadiani A, Ghanavi J, Seifalian AM. Properties of the amniotic membrane for potential use in tissue engineering. Eur Cell Mater. 2008;15:88-99.
- Fairbairn NG, Randolph MA, Redmond RW. The clinical applications of human amnion in plastic surgery. J Plast Reconstr Aesthet Surg. 2014;67(5):662-75.
- Anderson JJ, Swayzee Z, Hansen MH. Human Amniotic Allograft in Use on Talar Dome Lesions: A Prospective Report of 37 Patients. Stem Cell Disc. 2014;4(3):55-60.
- Gruss JS, Jirsch DW. Human amniotic membrane: a versatile wound dressing. Can Med Assoc J. 1978;118(10):1237-46.
- Jay RM. Initial clinical experience with the use of human amniotic membrane tissue during repair of posterior tibial and achilles tendons. AFCell Medical. 2009.
- Anderson JJ, Gough AF, Hansen MH, Swayzee Z. Initial experience with tricortical iliac crest bone graft and human amniotic allograft in Evans calcaneal osteotomy. Stem Cell Disc. 2015;5:11-7.
- Werber B, Martin E. A prospective study of 20 foot and ankle wounds treated with cryopreserved amniotic membrane and fluid allograft. J Foot Ankle Surg. 2013;52(5):615-21.
- Zelen CM, Poka A, Andrews J. Prospective, randomized, blinded, comparative study of injectable micronized dehydrated amniotic/chorionic membrane allograft for plantar fasciitis--a feasibility study. Foot Ankle Int. 2013;34(10):1332-9.
- Zelen CM, Snyder RJ, Serena TE, Li WW. The use of human amnion/chorion membrane in the clinical setting for lower extremity repair: a review. Clin Podiatr Med Surg. 2015;32(1):135-46.
- Shimberg M. The Use of Amniotic-Fluid Concentrate in Orthopaedic Conditions. J Bone Joint Surg. 1938.
- Warner M, Lasyone L. An Open-label, Single-center, Retrospective Study of Cryopreserved Amniotic Membrane and Umbilical Cord Tissue as an Adjunct for Foot and Ankle Surgery. Surg Technol Int. 2014;25:251-5.
- Ozbölük S, Ozkan Y, Oztürk A, Gül N, Ozdemir RM, Yanik K. The effects of human amniotic membrane and periosteal autograft on tendon healing: experimental study in rabbits. J Hand Surg Eur Vol. 2010;35(4):262-8.
- Koob TJ, Rennert R, Zabek N, Massee M, Lim JJ, Temenoff JS, et al. Biological properties of dehydrated human amnion/chorion composite graft: implications for chronic wound healing. Int Wound J. 2013;10(5):493-500.
- NuTech Medical (2012) NuCel: Product Overview. 1;1-2.
- Spencer LK, Anderson JJ, Fowler Z. Ankle Arthroscopy, Lateral Ligament Repair and Peroneal Tendon Reefing for Chronic Lateral Ankle Instability: The Triad versus Arthroscopy with Ligament Repair. Surg Sci. 2015;6:403-11.