Research Article
Tibiotalocalcaneal Fusion as Treatment of Cerebral Palsy Patient with Failed Total Ankle Replacement
Amber M Shane*, Christopher L Reeves, German Mikheyev and Zachary Cavins
Department of Foot and Ankle Surgery, Orlando Foot and Ankle Clinic, USA
*Corresponding author: Amber M Shane, Department of Foot and Ankle Surgery, Orlando Foot and Ankle Clinic, Orlando, FL, USA
Published: 12 Jun 2017
Cite this article as: Shane AM, Reeves CL, Mikheyev G,
Cavins Z. Tibiotalocalcaneal Fusion as
Treatment of Cerebral Palsy Patient
with Failed Total Ankle Replacement.
Clin Surg. 2017; 2: 1499.
Abstract
Patient selection and a thorough pre-operative musculoskeletal exam arekey in determining longterm success of total ankle replacements. The authors discuss a case of a patient with cerebral palsy with a rigid cavovarus deformity who previously underwent TAR on the affected limb.
Introduction
The evolution in surgical technique and implant design has allowed Total Ankle Replacement
(TAR) surgery to more frequently be used for treating end stage ankle arthritis, a problem that has
historically resulted in ankle arthrodesis. Utilization of TARs has been on the increase recently,
with the number of TARs performed in the US rising by 57% from 2004 to 2009. They are powerful
procedures that maintain motion in a previously painful and arthritic joint. However, the increased
use of TARs has also brought to light its range of complications, highlighting the importance of
patient selection. The most common complications with TARs occur as often as 50% of the time
and include infection, implant subsidence, polyethylene dislocation, wound dehiscence, and periimplant
fracture. While there are several acceptable indications for performing TARs, including
rheumatoid arthritis, posttraumatic arthritis, osteoarthritis, avascular necrosis, clubfoot, and others,
a thorough evaluation of each patient’s medical history and biomechanical landscape must be
completed for successful results. TAR revisions are difficult procedures that often occur secondary
to component loosening, infections, erosion, recurrent pain, or joint instability [1-4].
Patient factors that may lead to failure of TAR have been described in the literature, including
severe osteoporosis, diffuse osteonecrosis, or significant bone defect on the tibial and/or talar site. If
the patient has a heavy physical demand at their job, medium to high level of sports activities, high
body mass index, diabetes, and smoking, risk of failure increases [3].
Absolute contraindications for TAR include: neuroarthropathy, non-manageable hindfoot
malalignment, massive joint laxity, highly compromised periarticular soft tissues, severe sensory
motor dysfunction, and active soft-tissue or bony infection [4].
Case Presentation
Our case is that of a 47-year-old male that presented to our clinic with a painful right ankle.
His pain was getting progressively worse over the last year, to the point where it was limiting daily
activities and restricting normal weight bearing to that extremity. Additionally, he began to notice
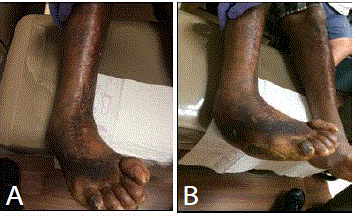
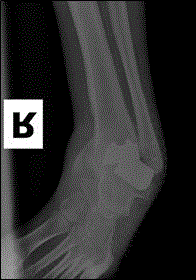
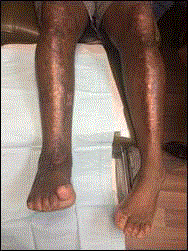
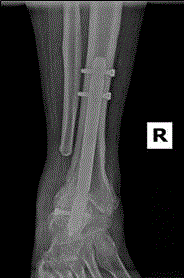
frequent falls. One year prior to presentation, the patient was treated by a different physician for
adductovarus foot deformity (Figure 1A and 1B) with a total ankle replacement (Figure 2 and 3).
The patient went on to a poor outcome, with recurrence of the deformity and pain. Notably, it was
determined that infection was not present as the cause of implant failure.
The primary reason for the patient’s lower extremity deformities was cerebral palsy, which
resulted in spastic contractures of his posterior muscle groups bilaterally, and was not addressed
at the index TAR procedure. He had equinovarus deformities of his feet along with rigid varus
angulation at the ankle joints. The patient’s remaining history was relatively innocuous, with medical
history including only GERD and cerebral palsy. He did not drink alcohol or use tobacco products.
After failing to improve with ankle bracing, the patient elected to undergo surgical correction of his
deformities.
Surgical approach
The senior author’s approach in the operating room was to first perform a percutaneous
tendoachilles lengthening procedure. Next, a curvilinear medial ankle incision was made to release the flexor retinaculum, tarsal tunnel, plantar fascia, and the medial and lateral plantar nerves. Once released, lengthening of the posterior
tibial, flexor hallucislongus and flexor digitorumlongus tendons was
completed to help attenuate the varus deforming forces.
A stab incision was made at the anterior leg for access to the
proximal tibia where 15 cc of bone marrow aspirate was obtained.
Next, attention was directed to the lateral aspect of the distal fibula and
ankle joint where a curvilinear incision was created to gain enough
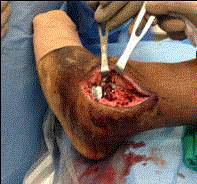
exposure to perform the distal fibula osteotomy and takedown. With
the take down complete the dislocated TAR was visualized with the
poly insert protruding laterally (Figure 3). The poly insert was then
removed followed by the removal of tibial and talar components with
help of osteotome. Further, subtalar joint soft tissues were released to
help relieve the cavus foot.
Still, the cavovarus deformity remained at the ankle joint,
prompting a curvilinear anteriomedial incision that was then made
over the ankle joint. Scar tissue was debrided before realigning
the talus beneath the tibia. Next, a proximal talar osteotomy was
completed to help bony apposition with tibia, as well as to prepare
the joint for fusion.
Once the cavovarus deformity was reduced and confirmed with
fluoroscopy, attention was directed to placing an intermedullary nail to maintain the corrected position. A guide-pin was placed from
calcaneus into tibia via a small plantar incision, again with the aid
of intraoperative fluoroscopy. Great care was taken to ensure proper
alignment at this step as it determines the outcome of the remaining
procedure. The tibia was then reamed and filled with bone allograft
mixed with the patient’s own fibular autograft and BMA from the
tibia to assist in the fusion process. Next, a tibio-talo-calcaneal (TTC)
fusion nail (T2™ Ankle Arthrodesis Nail, Stryker, 325 Corporate Dr.
Mahwah, New Jersey 07430) was placed and screwed into the now
prepared tibia and talus. Intraoperative fluoroscopy revealed no
gapping at the ankle joint with excellent boney apposition and contact.
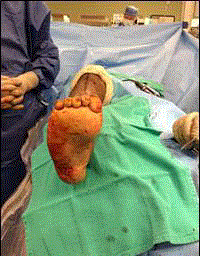
The foot and leg were then evaluated clinically to ensure that the foot
was plantar grade and that lower extremity was in alignment (Figure
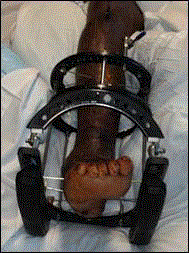
4). Next, an external fixator was applied to help reduce motion across
joints and to help protect the fusion site (Figure 5).
The patient was followed continually on an outpatient and at 3
months the external fixator was removed once there were signs of
fusion noted. The patient had developed a medial ankle wound of
approximate 2 cm which was also debrided at this time and followed
with local wound care. The wound later went on to heal without
incident (Figure 6 and 7). Due to the success and level of patient
satisfaction from this procedure, he elected to undergo a primary
TTC fusion with fibular takedown to the contralateral (left) lower
extremity 5 months later.
Figure 1
Figure 2
Figure 3
Figure 4
Figure 5
Figure 6
Figure 7
Discussion
The number of total ankle replacements (TARs) performed has
been increasing, warranting increase in research regarding their
outcomes [1]. Failed TARs are complicated cases to manage, and
require more robust research, as all available studies looking at TTC
fusions after failed TARs are either case studies or retrospective case
series; no prospective studies are available. The fusion rates for TTC
arthrodesis as salvage procedures for failed TARs range between
60%-100% in the literature [2].
An ideal candidate for TAR has a normal or low body mass
index, middle-to-old age, with no significant co-morbidities. X-ray
exam should reveal adequate bone stock. Their musculoskeletal exam
should reveal a well-aligned and stable hindfoot with good soft tissue
coverage without neurovascular impairment [3]. These qualities are
not always encountered, and the foot and ankle surgeon must be
realistic when identifying a patient capable of supporting an ankle
replacement. In the case of TAR failure, the surgeon must also be
aware of salvage techniques, with TTC fusions being one of the most
reliable options [4].
Our case is a good example of a salvage TTC fusion for a failed
TAR, but more importantly it is a learning point for patient selection.
In hindsight, this patient’s medical history and physical exam should
likely preclude the surgeon from recommending a TAR. Fortunately,
appropriate salvage options are available, and this patient went on
to solid fusion at 1 year follow up. A contralateral TTC fusion was
completed and also healed well, with the patient returning to pain
free ambulation with the ability to perform activities of daily living.
References
- Berkowitz MJ, Sanders RW, Walling AK. Salvage arthrodesis after failed ankle replacement: surgical decision making. Foot Ankle Clin. 2012;17(4):725-40.
- Deleu PA, DevosBevernage B, Maldague P, Gombault V, Leemrijse T. Arthrodesis After Failed Total Ankle Replacement. Foot Ankle Int. 2014;35(6):549-57.
- Gougoulias NE, Khanna A, Maffulli N. History and evolution in total ankle arthroplasty. Br Med Bull. 2009;89:111-51.
- Gross C, Erickson BJ, Adams SB, Parekh SG. Ankle arthrodesis after failed total ankle replacement: a systematic review of the literature. Foot Ankle Spec. 2015;8(2):143-51.