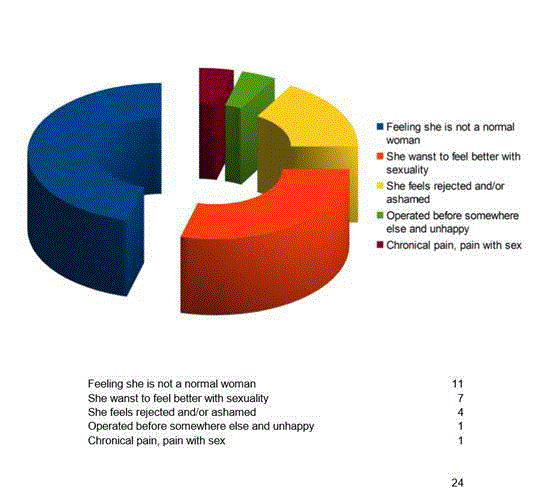Research Article
Outcome of External Genital Reconstruction after Female Genital Mutilation (FGM): A Pilot in Selected Patients in the Netherlands
Karim RB1* and Dekker JJML2
1Department of Plastic Surgery, Kliniek Amstelveen, Amstelveen, Netherlands
2Department of Gynecology and Obstetrics, VU Medical Centre, Amsterdam, Netherlands
*Corresponding author: Karim RB, Department of Plastic Surgery, Kliniek Amstelveen, Groenhof 111-112, NL-1186 EW Amstelveen, the Netherlands
Published: 25 May 2017
Cite this article as: Karim RB, Dekker JJML. Outcome of
External Genital Reconstruction after
Female Genital Mutilation (FGM):
A Pilot in Selected Patients in the
Netherlands. Clin Surg. 2017; 2: 1483.
Abstract
Background: The demand for reconstruction of external genitalia after Female Genital Mutilation
(FGM) is increasing as a result of the empowerment of migrated and naturalized women from Africa
and the Middle East. We present our procedures and the outcome of our selection and surgery.
Patients and Methods: From 2010 to 2015, 41 women presented with FGM. All underwent wellspecified
patient selection before operation. Clitoroplasty according to Foldes was performed in
selected patients. These patients were followed-up for 13.4 months and post-operatively assessed.
Results: Sixteen of the 41 women (39%) were not operated because they had unrealistic expectation
about the outcome of surgery (n=11) or had comorbidities that had to be dealt first (n=5). One
woman chooses to have only her Bartholin cyst corrected after pre-opeartive consultation.
Clitoroplasty was performed in the remaining 24 women. Post-operatively, we observed no major
and only 3 minor post-operative complications. Nineteen of these 24 women were satisfied with the
surgery and had a better self-esteem after surgery. Three of the remaining five women were lost for
follow-up and two were disappointed with the surgical outcome.
Conclusion: External genital reconstruction after well-specified preoperative selection leads too
predictable results with minor surgical complications. A better self-esteem achieved by minor
surgery should not be a contra-indication for reconstructing these women.
Keywords: Reconstruction; Female genital mutilation; Clitoroplasty
Introduction
Female genital mutilation (FGM) is defined by the World Health Organization as ‘all procedures
that involve partial or total removal of the external female genitalia or other injury to the female
genital organs for non-medical reasons’ [1]. FGM has a tribal origin and is based upon gender
inequality. It is widely supported as a cultural ritual mostly in sub-Saharan Africa, and to a lesser
extent in the Far East, the Middle East, and among immigrant communities in Europe. Women are
the gatekeepers and initiators of this rite. FGM is typically carried out domestically and without
anesthesia, by a traditional circumciser using a knife or razor. About 125 million girls in Africa and
the Middle East have undergone FGM [1]. The age of the girls varies from toddler to puberty [1].
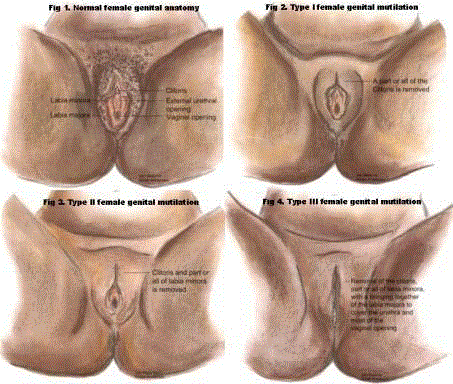
FGM involves one or more procedures which vary according to geographical region and local
cultural practices (Figure 1) and may be categorized as:
Type I in which all, or part of the external clitoris and clitoral hood is removed;
Type II in which Type I is combined with removal of all, or a part of the minor labia;
Type III (infibulation) in which all, or part of the minor and major labia are removed and the
resulting wound is sutured. A small cutaneous fistula is left for the passage of urine and menstrual
blood, and the wound is opened only for intercourse and childbirth.
Type IV are all other harmful procedure to the female genitalia for non-medical purposes.
In Europe, the demand for reconstruction of mutilated female genitalia is increasing due to the
empowerment of immigrant and naturalized women from Africa. Their quest for reconstruction
involves more than just the request for surgical correction of their external genitalia [1-5]. It implies the questioning of the very existence and legitimation of FMG.
Furthermore, having come to live in another society, these women
may start to feel different from the women in their new habitat
and consequently wish to become “complete” again. Although the
detrimental effects on health depend on the type of FGM, [1,4] all
types include removal of all, or part of the clitoris and clitoral hood.
Correction of the mutilated clitoris, therefore, usually comprises the
mainstay of the correction of the state of FGM for these women.
Current recommendations regarding the health care of woman
after FGM differs among the European countries. While clitoris
reconstruction is fully reimbursed in France, other countries such as
England and the Netherlands are still debating about the potential
psychophysical harm of FGM and about the questions whether, or
not, reconstruction after FGM is advisable and should, or should not,
be part of basis health-care [6-8]. Furthermore, surgical correction
of FMG is often seen by more conservative health care professionals
as a way of only supporting gender identity and promoting female
completeness, which can allegedly be achieved also by sexual
counseling and anatomy lessons [6].
The surgical techniques for clitoris reconstruction after FGM is
well established by Pierre Foldes and his surgical results have been
reproduced by other surgeons [9-11]. Still, the surgical and emotional
outcome of external genital reconstructive surgery in this group of
women has not been fully established, to date. Furthermore, little has
been recorded on pre-operative patient selection while we observed
discrepancies between the type of FGM determined at physical
examination and the extent and severity of the patient’s complaints.
Moreover, the expectations on the outcome of surgery may be
unrealistic, which may severely hamper recovery from treatment with
such an emotional weight.
Figure 1
Figure 2
Patients and Methods
Patients
From January 2010 through September 2015, 41 women aged 18
years or older consulted our practice for potential surgical correction
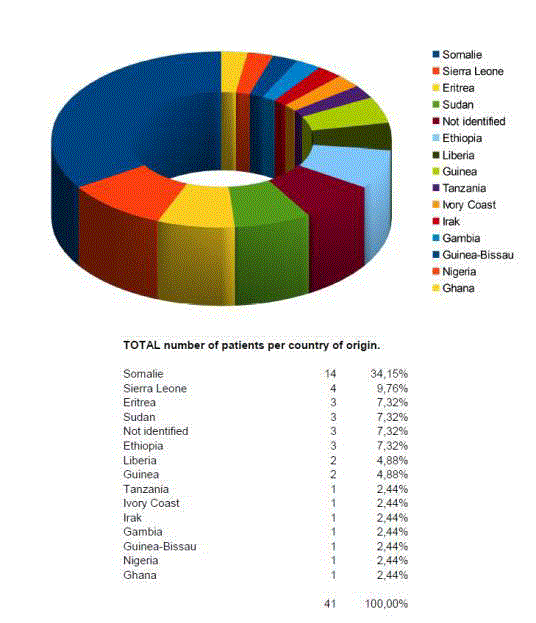
after FGM. All patients came from the sub-Saharan region or the
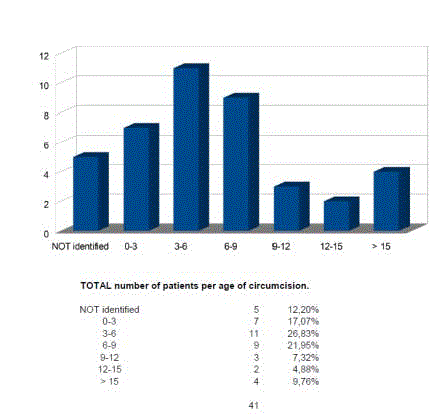
Middle East (Figure 2) and were circumcised at childhood (Figure
3). Most of the patients presented themselves (n=12), whereas the
others were referred to us by their general practitioner (n=20), their
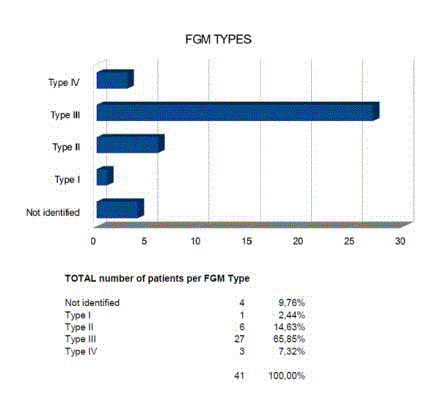
gynecologist (n=8), or their plastic surgeon (n=1). Most women
presented after type III FGM (infibulation) (Figure 4). Still, no
reconstruction of the introitus needed be done as we operated on
women who had their vagina opened for child birth.
Pre-operative work-up
As part of the pre-operative work-up, all women had an extensive
interview with a dedicated case-manager and their surgeon and they
filled out a questionnaire at entry about their characteristics (age,
country of origin, country of circumcision, age at circumcision).
Patients were explicitly asked pre-operatively what their main motive
for seeking surgical correction was. For this, they were asked to
choose one of five options:
1- Not feeling a complete or normal woman;
2- Wanting to feel better with sexuality;
3- Feeling rejected and/or ashamed;
4- Experiencing chronic pain or pain during intercourse;
5- Feeling dissatisfied with outcome of treatment elsewhere.
Even though we noticed high level complains regarding pain and
discomfort with an apparent poor injury in six women in whom there
seems to be no real agreement between the state of the scar and pain
situation, we have tried to very carefully interpret these situations
in a multidisciplinary approach [6,7,9,12]. In woman suffering
spontaneous vulvar pain further investigation of this complaint was
performed by the gynecologist before deciding on the procedure [12].
Patients were informed orally about possibilities, limitations, and
complication of surgical correction and an informed consent was
issued.
Treatment
Surgical correction was carried out under general anesthesia because of the risk of reliving the initial trauma when alert. The
women were operated in the lithotomy position and a single-dose
intravenous antibiotic prophylaxis (1500 mg cefuroxime, Fresensius
Kabi, Bad Homburg, Germany) was provided on induction.
In two women, a pseudo-cyst in the FGM scar was resected before
the clitoral reconstruction could take place and in another, a stenosis
of the urethral meatus was additionally corrected.
The principles described by Foldes were applied [9,10,11],
respecting the dorsal clitoral vascularization of the clitoral remnant
that was found left to the symphysis. After removal of all lateral and
ventral scar tissue and dissection of the suspensory ligament dorsally,
this clitoral remnant was folded ventrally towards the vaginal
introitus.
A layer of sutures is placed around the clitoral stump to prevent
retraction. Above the clitoris the skin is closed with interrupted
stitches passing through the subcutaneous connective tissue.
Surgery was extended to include reconstruction of labia minora
in three women. This was done by raising a medially based random
skin flap from both lateral aspects of the introitus, which was covered
laterally by a full thickness skin graft from the infragluteal fold.
At the conclusion of surgery, a local block with 10 cc of ropivacaine
hydrochlorid 7.5 mg/ml (Fresensius Kabi, Bad Homburg, Germany)
was applied subcutaneously to reduce post-operative pain.
All patients were prescribed amoxicillin/clavulanic acid
500/125 gram orally, three times daily for 5 days. After sole clitoris
reconstruction, the women were discharged on the day of surgery
and advised to keep bed rest for three days (n=22). Following labial
reconstruction, women remained admitted for 24 hours to allow
clinical observation and wound control (n =3). After this, 5 days of
bed rest at home was recommended.
To prevent pain on voiding or walking, women were additionally
prescribed lidocaine 2%-paraffin crème to be applied thinly to the
wound three times daily for the first 3 post-operative days, and estriol
vaginal crème, to be applied thinly on and around the wound once a
day from day 2, for 3 weeks.
Patients were instructed to limit their activities, to cool the affected
area, not to smoke, and not to carry out any heavy physical efforts
during the recovery period in the first 3 weeks after surgery. They
were additionally instructed that it may take 6 to 12 weeks before the
wound had fully healed. Women were routinely reviewed at the outpatient
clinic at 3 weeks, 3 months, 6 months, and 1 year after surgery
and were encouraged to call their case-manager whenever needed in
between scheduled appointments.
Assessment
All post-operative events were noted. As such, we defined a
major complication as any event that needed clinical re-admission
or repeated surgery. Minor complications could be treated
conservatively.
Patient satisfaction with the outcome of surgery was standardly
assessed by their case-manager, 3 months post-operatively (Figure 6).
Again, the women were explicitly asked to choose one of three
options:
1- Satisfied with the outcome of surgery;
2- Not satisfied with the outcome of surgery;
3- Unfavorable sexual experience after surgery.
Furthermore, all women were interviewed by their case-manager
in the autumn of 2015. The operated women’s pre-operative
expectations were compared to this post-operative satisfaction.
Figure 3
Figure 4
Figure 5
Figure 6
Results
Pre-operative work-up
We found the recovery of personal autonomy by rejection of the
physical mutilation imposed on them by their family to be unanimous
present among the 41 potential candidates for FGM correction.
Following our work-up procedure [12], 16 of the 41 women were
not felt eligible for FGM correction. Surgical procedures were not
initiated in 11 of these 16 women because we observed a discrepancy
between the type of FGM determined at physical examination and
the extent, severity, and type of complaints or unrealistic expectations
that could not be corrected by our team. The remaining five women
were not felt eligible because of comorbidities such as post-traumatic
stress syndrome that had to be dealt with prior to surgery.
Of the 25 women felt eligible for surgery, one only allowed removal
of a Bartholin cyst but refused external genital reconstruction of her
type IV FGM. The main reasons for surgery among the remaining 24
women were the lack of female completeness and the wish to improve
sexually (Figure 5) [9-11,13-15].
Patients
The 24 women who underwent genital reconstruction had a
mean age of 35.2 years (range 23-52 yrs; SD 6.21). All but one lived
in the Netherlands and had access to the health-care system. The one
remaining woman came self-referred from Saudi Arabia.
Five of these 24 (21%) women presented with type II mutilation
with clitoral excision, whereas 19 (79%) had a type III mutilation.
Treatment
We observed no major complications in our series and none of
the women needed to be re-admitted. Mild local inflammation (n=2)
or urinary tract infection (n=1) were observed in three women.
ssessment
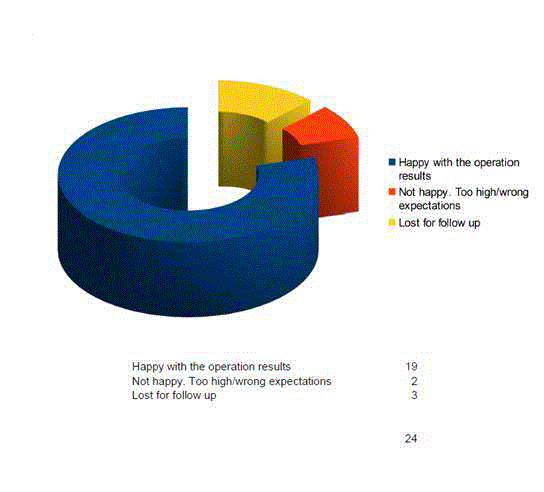
The average follow-up was 13.4 months (range 2–134 weeks; SD
39). Three women were lost for follow-up (12%). Nineteen women
were satisfied with the surgery and claimed better self-esteem after
surgery (79%). The two remaining women were disappointed with
the aesthetic outcome but were still glad to have undergone surgery
(8%). Additional post-operative counseling to further clarify their
expectations regarding the outcome of surgery revealed both women
to have expected a more voluminous clitoris. Still, the surgery and
additional post-operative empowerment of their knowledge of basic
anatomy and the surgical possibilities reportedly improved their selfesteem.
Discussion
The erectile tissue in females consists of parts of the labia minora,
the clitoris consisting of glans, cavernosal body and crura, the
vestibular spongious bulbs, and the urethral corpus spongiosum. Of
these, the glans and part of the clitoral body and the labia minora
may have been excised in infibulated women, while other structures
of orgasm have not [16,17]. Clitoral reconstruction is often feasible
after female genital mutilation and involves a reproducible and
standardized surgical procedure with acceptable complications rates
[5,9-11,13,14]. Consequently, 80% of women who undergo FGM may
function better sexually 12 months after clitoris correction, and that
their self-esteem and self-image is likely to increase [5,9-11,13,14].
Although we have not properly quantified what effect corrective
surgery after FGM in the Netherlands has on quality of life and selfesteem,
our observations in the current series seem to support this.
FGM is recognized internationally as a violation of human
rights. A total ban on all forms of circumcision in young women is
becoming the standard policy in Europe [15]. As we accept this as
a mutilation then we have to equally accept the next step as a basic
human right. That is to try and correct the genital appearance of these
women, if and when there is a demand for such a correction. For this
reason, we feel that genital corrective surgery should be an integral
part of the care provided to these women [5]. Not every genitally
mutilated woman will opt for surgery but if they do patient-selection
is an important tool to optimize quality of care and to prevent
postoperative disappointments.
That the surgery is often rejected by more conservative healthcare
professionals as a way of only supporting gender identity and
promoting female completeness [6], in our opinion, is based on the
failure of these professionals to fully understand the complex sociocultural
context of women’s sexuality among societies which practice
FGM [16]. In any case, human sexuality is a complex matter between
mind and body but also in the light of relationships and self-esteem.
Although difficult for us to understand FGM does not necessarily
have a negative impact on psycho sexual life [16], but it may impair
sexuality. A small group of mutilated woman is seeking surgical
solution. We as health care professionals should be open-minded and
cultural sensitive in our approach to these patients and explore their
need for surgery. A thorough patient selection is important.
Conclusion
External genital reconstruction leads too predictable results with few minor surgical complications after specified selection of FGM patients. Because better self-esteem may be achieved by minor surgery, such surgery ought to be offered to these women.
Acknowledgement
The authors are grateful to Dr Pierre Foldes, urologist at Clinique St. Germain in St. Germain en Laye, France, for his mental inspiration and guidance.
References
- Office of the United Nations High Commissioner for Human Rights (OHCHR), Joint United Nations Programme on AIDS (UNAIDS), United Nations Development Programme (UNDP), United Nations Economic Commission for Africa (UNECA), United Nations Educational, Scientific and Cultural Organization (UNESCO), United Nations Population Fund (UNFPA), United Nations High Commissioner for Refugees (UNHCR), United Nations Children’s Fund (UNICEF), United Nations Development Fund for Women (UNIFEM), World Health Organization (WHO). Eliminating female genital mutilation: an interagency statement. Geneva: World Health Organization. 2008.
- Vloeberghs E, Knipscheer J, van der Kwaak A, Naleie Z, van den Muijsenbergh M. Versluierde pijn, Onderzoek naar psycho-sociale gevolgen van meisjesbesnijdenis. 2010; 978-90-75955-72-9-ISDN.
- EURAPS. Reconstruction after FGM, Kliniek Amstelveen. 2013.
- Vos C, van Roosmalen J. Een klein onderwerp: vrouwelijke genitale verminking. Ned Tschr Obst Gyn. 2013;126:447-450.
- Karim RB, Dekker JJML. From female genital mutilation to female genital reconstruction.
- Abdulcadir J, Rodriguez MI, Say L. Research gaps in the care of women with female genital mutilation: an analysis. BJOG. 2015;122(3):294-303.
- Abdulcadir J, Rodriguez MI, Say L. Systematic review of the evidence on clitoral reconstruction after female genital mutilation/cutting. Int J Gynaecol Obstet. 2015;129(2):93-7.
- Royal College of Obstetricians & Gynaecologists. Female Genital Mutilation and its Management.
- Foldes P, Cuzin B, Andro A. Reconstructive surgery after female genital mutilation: a prospective cohort study. Lancet. 2012;380(9837):134-41.
- Foldes P, Louis-Sylvestre C. Results of surgical clitoral repair after ritual excision: 453 cases. Gynecol Obstet Fertil. 2006;34(12):1137-41.
- Foldes P. Reconstructive plastic surgery of the clitoris after sexual mutilation. Prog Urol. 2004;14:47-50.
- Karim RB, Dekker JJML, Paarlberg KM, Vos MC, IJland MM. Modelprotocol Reconstructieve chirurgie na Vouwelijke Genitale Verminking (Dutch guidelines reconstructive chirurgy after FGM).
- Ouédraogo CM, Madzou S, Touré B, Ouédraogo A, Ouédraogo S, Lankoandé J. Practice of reconstructive plastic surgery of the clitoris after genital mutilation in Burkina Faso, report of 94 cases. Ann Chir Plast Esthet. 2013;58(3):208-15.
- Madzou S, Ouédraogo CM, Gillard P, Lefebvre-Lacoeuille C, Catala L, Sentilhes L, et al. Reconstructive surgery of the clitoris after sexual mutilation. Ann Chir Plast Esthet. 2011;56(1):59-64.
- Leye E. Female genital mutilation: a study of health services and legislation in some countries of the European Union. Ghent, Belgium Ghent University. Faculty of Arts and Philosophy. 2008.
- Catania L, Abdulcadir O, Puppo V, Verde JB, Abdulcadir J, Abdulcadir D. Pleasure and orgasm in women with Female Genital Mutilation/Cutting (FGM/C). J Sex Med. 2007;4(6):1666-78.
- Public Policy Advisory Network on Female Genital Surgeries in Africa. Seven things to know about female genital surgeries in Africa. Hastings Cent Rep. 2012;42(6):19-27.