Case Report
Neuropraxia Following Resection of a Retroperitoneal Liposarcoma
Stevenson Tsiao*, Subhasis Misra and Nail Aydin
Department of Surgery, Texas Tech University Health Sciences Center, USA
*Corresponding author: Stevenson Tsiao, Department of Surgery, Texas Tech University Health Sciences Center, 1400 S. Coulter Street, Amarillo, TX 79106, USA
Published: 19 May, 2017
Cite this article as: Tsiao S, Misra S, Aydin N.
Neuropraxia Following Resection of
a Retroperitoneal Liposarcoma. Clin
Surg. 2017; 2: 1473.
Abstract
This is an 81 year old female who, on CT for evaluation of her atherosclerosis, was found to have an incidental right-sided retroperitoneal mass extending from the right renal capsule inferiorly through the inguinal canal. At this point, the patient reported mild right sided abdominal pain and right lower back pain, but reported no neuromotor deficits of the right lower extremity. Surgical intervention was pursued. On exploration, the lipomatous lesion, suggestive of liposarcoma, was invading the right genitofemoral nerve and ilioinguinal nerve which were sacrificed to ensure a complete oncologic resection. Following complete removal of the mass, she developed right side femoral nerve neuropraxia, suffering complete loss of motor function in the femoral distribution. Pathology revealed the mass to be a low grade liposarcoma. She required only physical therapy and oral prednisone following surgery for treatment of the neuropraxia. She responded well and has regained significant neuromotor function of the affected limb.
Introduction
An estimated 11930 cases of sarcoma were diagnosed in 2015, comprising less than 1% of all cancers diagnosed in the United States [1-3]. Of these, only approximately 10 to 20% are located in the retroperitoneum [2], and an even smaller subset of these will be diagnosed as liposarcomas, as opposed to fibrosarcomas which are more common. Typical complications following such masses include bleeding, infection, and incomplete resection of the mass. To our knowledge, neuropraxia, a transient paralysis due to blockage of nerve conduction, commonly associated with athletes and orthopaedic procedures, has not been previously reported as a complication following resection of such a mass.
Case Presentation
This is an 81 year old female who had an incidental finding of a large retroperitoneal mass on
CT Angiography for evaluation of her atherosclerosis. On imaging, she was found to have a right
sided large retroperitoneal mass measuring 11.3 cm × 7.8 cm × 6.2 cm extending from the renal
capsule down to and through the inguinal canal into the femoral triangle (Figure 1 and 2). The initial
reading was consistent with a lipomatous lesion suggestive of a liposarcoma. At the time, patient
reported only mild back pain with no known triggers and denied any neurological or neuromotor
dysfunction. She also stated she had pain along the right midportion of the thigh, but relates this to
a knee injury from many years ago.
Initial workup included measurements of CEA, CA-125, and HCG for the possibility of an
ovarian origin. Pelvic ultrasonography was also performed, and in addition to the negative results of
the chemical markers for ovarian or adnexal origin, the patient was referred to the surgical oncology
department.
Her past medical history is significant for cardiovascular disease, a descending aortic aneurysm,
previous myocardial infarction, left ventricular hypertrophy, angina, aortic and tricuspid valve
disorders, glaucoma, hypertension, and hypothyroidism. She had significant smoking history
of 58 years pack-years. Surgical history is significant for past tonsillectomy and adenoidectomy,
lipoma removal, haemorrhoidectomy, abdominal aortic aneurysm repair, and cataract surgery.
Family history is significant for breast and cervical cancer. The patient states she has up-to-date
mammograms and colonoscopies, which she reports are both normal.
Her physical exam was unimpressive; abdomen was soft, non-tender, and non-distended.
Surgical resection was recommended.
On the day of the surgery, bilateral urethral stents were placed
under cystoscopy, and an exploratory laparotomy was performed. No
signs of metastatic disease or other organ involvement were noted in
the peritoneum. The right retroperitoneum was accessed by a medial
visceral rotation, including a complete mobilization of the right colon
and duodenum, and the entirety of the mass was then visualized. The
mass, including the caudal extension, was freed with blunt dissection.
The mass was dissected with great care, freed initially from the
superior aspect, moving caudally. The right kidney, ureter, and IVC
were completely skeletonized. Gerota’s fascia, a portion of the inferior
1/3 of the psoas muscle, and portions of the genitofemoral nerve and
ilioinguinal nerve were respected along with the mass and its capsule
in its entirety. Careful blunt dissection was used throughout the case,
especially in the area of the femoral nerve. The mass was removed
en bloc without complication, with good visualization of the femoral
nerve afterwards.
Following surgery, the patient was tolerating PO diet and was
recovering well, other than complaining of difficulty flexing her right
lower extremity at the hip and extending at the knee. She also lacked
a patellar reflex. Motor ability of the ankle and foot were intact. These
signs indicated a femoral nerve paralysis.
Neurology was consulted to evaluate the patient’s loss of
aforementioned motor ability. She was found to have no cerebellar
dysfunction and full motor control of the left lower extremity.
Evaluation of the right lower extremity was significant. She was found
to have 0/5 hip flexion and 0/5 knee extension with an absent knee
jerk reflex. Additionally, all distal lower extremity muscle groups
were intact, with 5/5 dorsiflexion, plantarflexion, inversion, and
eversion of the foot, as well as an intact ankle jerk reflex bilaterally.
All the evidence pointed towards an injury to the femoral nerve, but
specific care was taken during surgery to avoid sharp dissection at the
level of the inguinal canal and the nerve, and therefore transection of
the nerve was highly unlikely.
Diagnostic MRI performed on post-operative day 14 revealed
a fluid collection 7 × 6 × 1 cm with the anterior aspect of the right
illiacus (Figure 3) which under different circumstances could
be worrisome for abscess, but given the patient’s benign clinical
presentation (afebrile, no leukocytosis) this was more consistent with
inflammation and post-operative changes rather than infectious in
origin.
At post-operative day (POD) 4, patient began having some
increased muscle strength in the affected leg. She was referred for
inpatient rehabilitation and aggressive physical therapy for two
weeks, and experienced significant improvement in muscle strength
and mobility. No other squeal from the surgery were noted at that
time.
Prednisone was started POD 21 for inflammation and swelling
in the inguinal canal. She was discharged to a skilled nursing facility
on POD 22.
Electromyogram (EMG) performed 8 weeks after surgery
showed mild slowed conduction velocity and minimal femoral nerve
response, unable to exclude demyelinating neuropathy.
Following discharge, the patient was followed closely in clinic.
She was still actively participating in a rehabilitation program. At
her 6 week post-operative clinic visit, she was ambulating with
minimal aid from a walker. She is continuously being followed for
any metastases as an indicator for prognosis, since her age it is already
a poor prognostic factor [6].
To monitor for any local recurrence, it was recommended that
the patient be seen every 6 months for the first two years, with CT
imaging of the chest, abdomen, and pelvis to check for any metastasis.
After these two years, annual CT exams up to 5 years are appropriate.
She is also following with her neurology team for management of the
neuropraxia, and is scheduled for another EMG 6 months from the
date of operation.
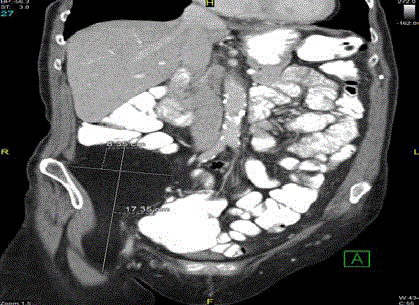
Figure 1
Figure 1
Initial CT imaging of the mass, showing extension of the caudal tail
into and through the inguinal canal.
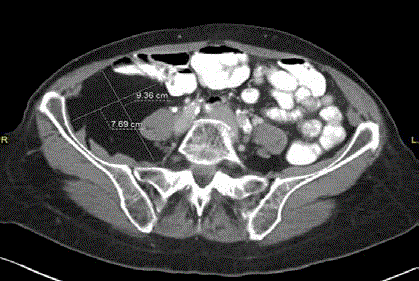
Figure 2
Figure 2
Transverse image of the mass, showing anterior displacement
of the psoas muscle and loops of bowel, consistent with a retroperiotoneal,
rather than intraperitoneal, mass.
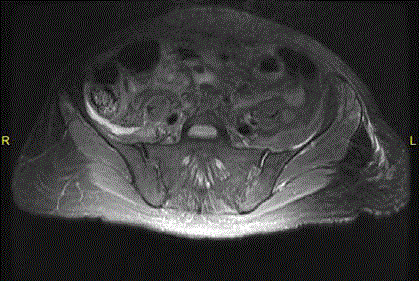
Figure 3
Figure 3
Post-operative MRI, day 14, showing large fluid collection (marked
by two solid arrows) overlying the right illiacus muscle.
Discussion
Extensive discussion was held with the patient to discuss treatment options, and it was eventually agreed that the best course of treatment would be surgical resection, given the potential for malignancy
and recurrence, as well as the tumor’s likely poor response rate to
chemotherapy [4]. Five year survival following an R0 resection of a
large retroperitoneal liposarcoma was found to be 85.7% compared to
R1 resection at 33.3% [5], while recurrence of the tumor for patients
undergoing R1 or R2 resection was as high as 96.7% [6]. No tissue
biopsy before the surgery was indicated to rule out other pathologies
due to the lack of distant metastases, as well as the respectable
appearance of the mass on imaging [7]. Given her social history, the
patient was advised to quit smoking before the operation, and she
also underwent cardiac clearance and pulmonary function testing
to assess her risk. Risks and benefits, as well as alternative treatment
options were discussed, including but not limited to bleeding, surgical
site infection, incomplete resection, recurrence, possible need for
adjuvant therapy, hernias, bowel resections, and bowel resection
related risks such as anastomotic leaks, need for an ostomy, as well
as reoperation. She expressed her understanding at this point and
agreed to proceed with surgical therapy.
CT evaluation of the patient that initially discovered the mass
did not show evidence of distant metastasis. Additionally, the mass
did not appear to arise from any retroperitoneal organ structure
(e.g. pancreas, adrenals, kidney, or duodenum). The patient also
presented without B-symptoms (fever, chills, night sweats), thus
making lymphoma an unlikely diagnosis. A gastrointestinal stromal
tumor (GIST), arising from the interstitial cells of Cajal (ICC) was
also a possibility, given its incidence as the most common soft tissue
sarcoma affecting the GI tract General Surgery [7]. Given the findings that there were
no appreciable metastases, and the respectable appearance of the
tumor, there was no indication for a tissue biopsy before resection,
even for GIST General Surgery [7], and the decision was made to take the patient
to surgery for complete excision, to spare her from undergoing a
separate biopsy procedure before surgery.
Few pathologies present as a large, uniform mass in the
retroperitoneum. Fibroadenoma, fibrosarcoma, lipoma, and
liposarcoma are the major constituents of a large, uniform,
retroperitoneal mass. Consideration was also made for gynaecological
in origin, however pelvic ultrasonography, CA-125, CEA, and HCG
were negative.
To the best of our knowledge, neuropraxia has not previously
been reported as a complication of respecting large retroperitoneal
sarcomas. Great care was taken in the operating room to preserve as
many neural structures as possible. However due to the involvement
of the ilioinguinal and genitofemoral nerves, tributary branches of
these structures were sacrificed out of necessity to achieve a proper
oncologic resection. The ilioinguinal nerve, a branch of L1, serves
primarily a sensory function to the upper medial thigh, mons pubis,
and labia majora in females. The genitofemoral nerve, from the upper
L1 and L2 segments of the lumbar plexus, serves as both the sensory
and motor arms of the cremasteric reflex which is more applicable in
males than females. Sacrificing either of these nerves should not have
any residual motor deficit as seen in this patient.
Flexion of the hip and extension of the knee is controlled by
numerous muscles, primarily the psoas, illiacus, rectus femoris, and
Sartorius. Of these muscles, the latter three have innervations from
the femoral nerve. Given the close proximity of the mass to the nerve
in the inguinal canal, as well as trauma from the blunt dissection and
removal of the mass from the femoral triangle, it is then most likely
that the etiology of this patient’s neuropraxia is from femoral nerve
manipulation. Since neither sharp instruments nor bovie was used in
the dissection of mass from the femoral canal, it is unlikely that the
femoral nerve was permanently damaged.
A conservative course of treatment was taken in response to
the patient’s neuropraxia. Physical therapy was the mainstay of
treatment, and an MRI was performed on post-operative day 14 after
surgical staples were removed. The fluid collection seen on MRI was
initially read as a possible abscess, but the patient’s presentation did
not correlate with this finding. Further discussion between surgeon
and radiologist concluded that the collection was more consistent
with inflammation and post-operative changes, which is important to
note as it saved the patient an additional invasive procedure to drain
the fluid, possibly further endangering the nerves.
With regards to clinical radiology, good clinical judgement must
be employed for the best benefit of the patient. While initial CT
imaging and initial pathology reported the mass as a lipoma, clinical
judgement was more suggestive of a liposarcoma, which necessitates
more aggressive treatment. A second review of the pathology found
the tumor to be a liposarcoma. Additionally, had the team acted on
the MRI report of an abscess, the patient would likely have been
subjected to placement of a drain by interventional radiology, which
exposes the patient to another source of infection, bleeding, and
complications. Good clinical judgement was also exercised in this case,
correlating the patient’s clinical presentation to the imaging report,
and collaboration between two distinct specialties was necessary to
spare the patient an invasive, painful, and costly procedure.
Conclusion
Neuropraxia has not previously been associated with resection of retroperitoneal liposarcomas. Given this mass’s extent through the inguinal canal, great care during resection and preservation of the nervous structure in the area are of upmost importance to reduce the patient’s overall level of post-operative morbidity.
References
- Maksimowicz-McKinnon K, Clark TM, Hoffman GS. Takayasu arteritis and giant cell arteritis: A spectrum within the same disease?. Medicine (Baltimore). 2009;88(4):221-6.
- Rojo-Leyva F, Ratliff NB, Cosgrove DM, Hoffman GS. Study of 52 patients with idiopathic aortitis from a cohort of 1,204 surgical cases. Arthritis Rheum. 2000;43(4):901-7.
- Nuenninghoff D, Hunder G, Christianson T, McClelland RL, Matteson EL. Incidence and predictors of large-artery complication (aortic aneurysm, aortic dissection, and/or large-artery stenosis) in patients with giant cell arteritis: A population-based study over 50 years. Arthritis Rheum. 2003;48(1):3522-31.
- Evans JM, O’Fallon WM, Hunder GG. Increased incidence of aortic aneurysm and dissection in giant cell (temporal) arteritis. A population-based study. Ann Intern Med. 1995;122(7):502-7.
- Svensson LG, Arafat A, Roselli EE, Idrees J, Clifford A, Tan C, et al. Inflammatory disease of the aorta: patterns and classification of giant cell aortitis, Takayasu arteritis, and nonsyndromic aortitis. J Thorac Cardiovasc Surg. 2015;149(2):S170-5.