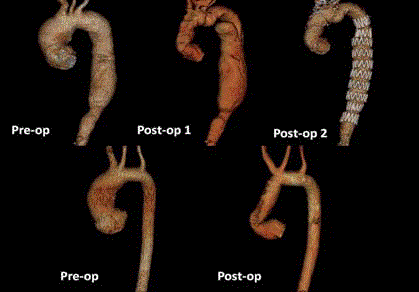Case Report
Aortic Root Aneurysms in Twenty-Year-Olds: Don’t Forget to Check the Histology
Monica A Isabella1, Carol Langford2, Alison Clifford3 and Eric E Roselli4,5*
1Departments of General Surgery, Cleveland Clinic, Cleveland, Ohio 44195, USA
2Department of Rheumatic and Immunologic Diseases, Cleveland Clinic, Cleveland, Ohio 44195, USA
3Department of Biological Sciences, University of Alberta, Edmonton, Alberta T6G 2E9, USA
4Department of Thoracic and Cardiovascular Surgery, Heart and Vascular Institute, Cleveland Clinic Foundation,
Cleveland, Ohio 44195, USA
5Aortic Center, Heart and Vascular Institute, Cleveland Clinic Foundation, Cleveland, Ohio 44195, USA
*Corresponding author: Eric E Roselli, Department of Thoracic and Cardiovascular Surgery, Cleveland Clinic, 9500 Euclid Ave., Desk J4-1, Cleveland, OH 44195, USA
Published: 19 May, 2017
Cite this article as: Isabella MA, Langford C, Clifford A,
Roselli EE. Aortic Root Aneurysms
in Twenty-Year-Olds: Don’t Forget to
Check the Histology. Clin Surg. 2017;
2: 1472.
Abstract
When confronted with an aortic root aneurysm in a young patient, one of the most common
etiologies is a connective tissue disorder (CTD, such as Marfan’s, Loeys Dietz, and Ehlers-Danlos.)
Aortitis is considered rare among young patients and can be easily missed in asymptomatic cases.
Aortitis can be difficult to diagnose but is important to investigate during surgery because missing
the diagnosis may affect late outcomes. Undertreated aortitis may progress beyond the treated
segment. Our understanding of arteritis is improving, and it has been suggested that Giant Cell
Arteritis (GCA) and Takayasu Arteritis (TAK) may represent an overlapping spectrum of disease.
CTD, GCA, and TAK require lifelong surveillance and immunosuppressive treatment for active
disease. However, Autoimmune Aortitis may be cured surgically. We describe two patients in their
twenties with aortic root aneurysms who underwent valve sparing aortic root replacement. Both
were found on histologic examination to have chronic aortitis. The cases presented here demonstrate
the importance for surgeons to send aortic specimens for histologic review when performing aortic
aneurysm repair.
Keywords: Aorta; Aneurysm (Root); Histology (Aortic); Pathology (Aortic); Surgery
Case Presentation
Case 1
A 27-year-old woman with a history of chronic back pain presented with an exacerbation.
Computed tomography (CT) revealed a 4.5 cm ascending aortic aneurysm. Follow-up serial imaging
showed diffuse dilation from the aortic root to the descending aorta with a 5.1 cm maximum diameter
(Figure 1). Echocardiogram confirmed a tricuspid aortic valve with moderate-to-severe regurgitation.
Family history was significant for a cerebral aneurysm in a cousin. There were no clinical signs
suggestive of a CTD or vasculitis; and blood work revealed normal levels of inflammatory markers.
She underwent a valve- sparing aortic root replacement with valve reimplantation (modified David’s
procedure); ascending aorta and aortic arch repair as well as a prophylactic first stage elephant trunk
procedure. Operative findings included a chronic; focal proximal ascending aortic dissection with
interval healing. Aortic tissue histopathologic examination showed chronic aortitis (Figure 2A and
2B). She was discharged home on post-operative day 10. Rheumatologic workup found no evidence
of active arteritis in other vessels that necessitated treatment. Two years later; she underwent
successful elephant trunk completion with a thoracic endovascular aortic repair.
Case 2
A 23-year-old man presented with an incidentally found ascending aortic aneurysm during
workup for a new heart murmur. Echocardiogram revealed a dilated aortic root and ascending aorta;
and tricuspid aortic valve with trivial regurgitation. CT confirmed a proximal aortic aneurysm with
5.1 cm maximum diameter. There was no family history of aneurysms. He underwent a modified
David’s reimplantation procedure with an ascending aorta and hemi-arch repair. Operative findings
were again significant for a healed chronic aortic root dissection. Histopathologic review of the aorta
also noted a chronic aortitis (Figure 2C and 2D). The patient was discharged home on post operative
day seven. Rheumatologic workup found no evidence of other vessel involvement and no indication for immunosuppressive therapy. He was doing well at his one year follow-up. The MRA showed a stable; well-healed aortic repair with
no findings of arthritis; and a well functioning aortic valve with trivial
regurgitation.
Figure 1
Discussion
Patients with asymptomatic aortitis and associated aneurysm
are diagnosed after surgery based on histopathologic review
demonstrating giant cells and other features of vasculitis [1]. These
two cases demonstrate that it is imperative to send aortic tissue for
histologic evaluation after aortic aneurysm repair; particularly for
asymptomatic patients [2,3]. Aortitis may be grossly underestimated
in younger patients because specimens are not routinely reviewed.
In a study involving 513 patients aged 16-85 years undergoing an
ascending aortic aneurysm repair; 57 were diagnosed with aortitis
after histologic review [4].
Common etiologies of aortitis include GCA; TAK; and
Autoimmune Aortitis. However; other important causes include
infection; primary vasculitides such as Cogan’s syndrome and Behcet’s
disease; as well as inflammatory diseases with spondyloarthropathies;
rheumatoid arthritis; and sarcoidosis. Both of these cases show large
vessel arteritis with laminar necrosis surrounded by lymphohistiocytic
infiltrates and multinucleated giant cells in the media. These features
are typically described in GCA which usually affects a much older
population but are occasionally seen in younger patients with isolated
vasculitis. The cases differ in their extent of aortic involvement; and
their operations were tailored to these preoperative imaging findings.
Histopathologic features alone are not specific to predict isolated
versus systemic vasculitis. While it confirms a large vessel vasculitis
diagnosis; further classification requires clinical correlation and
radiologic investigations. A histologic diagnosis of chronic aortitis
with giant cells encompasses GCA; TAK; and Autoimmune Aortitis.
GCA has a propensity to affect external carotid arteries. It can present
early with symptoms; but late and more serious complications;
including aneurysms and dissections; are often detected incidentally
during imaging for other reasons or during autopsy. Aortic
involvement has been found in up to 18% of asymptomatic cases [3].
It is not surprising that both cases described here had evidence of
focal dissection found incidentally during surgery. Patients with GCA
are 17.3 times more likely to develop a thoracic aortic aneurysm and
2.4 times more likely to have an isolated abdominal aortic aneurysm
than normal controls [4].
It has been speculated that TAK and GCA are not two distinct
diseases but represent part of a spectrum within a single entity [1]
Compared to GCA; TAK is known to have a younger age of onset; a
potential predilection for Asian women and aortic involvement. One
study questioned these clinical distinctions and found that patients
with GCA and TAK do have similar signs; symptoms; and imaging
abnormalities suggesting that the difference in diagnosis may be due
to bias [1].
Autoimmune Aortitis; on the other hand; is a disease that is
localized to the thoracic aorta; and may not require medical therapy
after surgery [5]. The mean age of onset in our early series was 63 years
[2]. These patients are unique because their disease can be surgically
cured before the histologic diagnosis is made; as was the case for our
second patient. In an early series; we found that these patients usually
did not require any further intervention; but most patients were older
and late follow-up was limited [2]. In our more recent experience;
we have found that many of these patients do require later thoracic
aortic operations and immunosuppressive therapy does little to slow
this progression [5].
Aortitis was also commonly associated with aortic valve disease
in our recent series; but the etiology of valve dysfunction was due
to mixed morphologic findings. The aortic cusp tissue was healthy
appearing in both of these patients despite root dilatation so the
intraoperative decision in these young patients was to spare the valve
by modified reimplantation. Little is known about how this disease
process affects the aortic valve. Time will tell whether the surgery
proves to be definitive treatment in both of these patients. Given their
young age and the limitation of our knowledge about the etiology of
thoracic aneurysms; surveillance MRA of the thoracic aorta at least
every five years was recommended.
The post-operative Histopathologic diagnosis of aortitis should
be followed by comprehensive rheumatologic evaluation to rule
out other vessel involvement and assess for symptoms or signs
of an underlying vasculitis or CTD. These patients may benefit
from additional medical treatment including corticosteroids or
other immunosuppressive to prevent new aneurysms or further
progression of vasculitis. Our cases demonstrate the vital importance
of histopathologic assessment of surgically respected thoracic aortic
tissue to facilitate comprehensive management of aortitis.
Figure 2
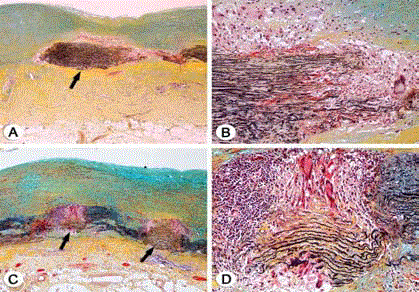
Figure 2
Movat pentachrome stained sections of aortas from patient 1(A&B)
and patient 2 (C&D). Low power magnification shows similar histology in
both cases with marked medial destruction and characteristic foci of laminar
medial necrosis (arrows, A&C). There is reactive intimal thickening and mild
fibrosis of the adventitia, and multinucleated giant cells are common around
segments of necrotic media seen on higher magnification (B&D).
References
- Maksimowicz-McKinnon K, Clark TM, Hoffman GS. Takayasu arteritis and giant cell arteritis: A spectrum within the same disease?. Medicine (Baltimore). 2009;88(4):221-6.
- Rojo-Leyva F, Ratliff NB, Cosgrove DM, Hoffman GS. Study of 52 patients with idiopathic aortitis from a cohort of 1,204 surgical cases. Arthritis Rheum. 2000;43(4):901-7.
- Nuenninghoff D, Hunder G, Christianson T, McClelland RL, Matteson EL. Incidence and predictors of large-artery complication (aortic aneurysm, aortic dissection, and/or large-artery stenosis) in patients with giant cell arteritis: A population-based study over 50 years. Arthritis Rheum. 2003;48(1):3522-31.
- Evans JM, O’Fallon WM, Hunder GG. Increased incidence of aortic aneurysm and dissection in giant cell (temporal) arteritis. A populationbased study. Ann Intern Med. 1995;122(7):502-7.
- Svensson LG, Arafat A, Roselli EE, Idrees J, Clifford A, Tan C, et al. Inflammatory disease of the aorta: patterns and classification of giant cell aortitis, Takayasu arteritis, and nonsyndromic aortitis. J Thorac Cardiovasc Surg. 2015;149(2):S170-5.