Research Article
A Combined Endolaryngeal Approach for Bilateral Vocal Fold Immobility: Microlaryngoscopic Submucosal Cordotomy and Endo-Extralaryngeal Triple-Suture Lateralization
Murat Cem Miman*
Department of Otorhinolaryngology, İzmir University School of Medicine, Turkey
*Corresponding author: Murat Cem Miman, Department of Otorhinolaryngology, İzmir University School of Medicine, Turkey
Published: 19 May 2017
Cite this article as: Miman MC. A Combined Endolaryngeal
Approach for Bilateral Vocal Fold
Immobility: Microlaryngoscopic
Submucosal Cordotomy and
Endo-Extralaryngeal Triple-Suture
Lateralization. Clin Surg. 2017; 2: 1471.
Abstract
Bilateral vocal fold immobility (BVFI) is a challenging clinical entity for laryngologists. The voice
may be nearly normal but mostly there is a severe inspiratory deficiency. The patients may need
surgical interventions primarily for life threatening dyspnea. While treating the dyspnea, dysphonia
appears to be a problem to a certain extent. Providing a serviceable voice and prevention from
further surgery for relapsing dyspnea, a balance is needed. Various techniques have been introduced
for surgical management of BVFI. A modified approach in order to balance between dyspnea and
dysphonia was performed on a BVFI patient and is presented in this report.
Keywords: Bilateral vocal fold immobility; Posterior Cordotomy; Laterofixation; Inspiratory
stridor
Introduction
Because of the complex innervation and re-innervation of the larynx [1] a typical paralytic
condition seen in extremities may not reveal in laryngeal functions after nerve injury. Bilateral
laryngeal nerve injury may be a life threatening clinical entity which can be managed under
emergency conditions. It is important to make a distinction between cricoarytenoid joint fixation
and loss of innervation in order to proceed for treatment bilateral vocal fold immobility (BVFI).
Laryngeal electromyography and palpation of the arytenoid may help for this distinction. Surgical
trauma (i.e. thyroidectomy) is the most common cause of BVFI [2].
Depending on its functional situation, BVFI mostly needs surgical intervention(s) basically
starting with tracheotomy. Voice and breathing are in an inverse relationship in the management of
BVFI. From the aerodynamic-biomechanical standpoint, hoarseness seems to be inevitable to some
extent in procedures which change the endolaryngeal geometry surgically in BVFI patients. Several
methods have been introduced; unilateral total ventriculocordectomy [3], arytenoidectomy [4,5],
posterior cordectomy [6] and laterofixation [7,8].
Surgical management of BVFI should be planned to make a critical balance between dyspnea
and dysphonia. Mostly, the surgical interventions create irreversible structural and functional
alterations to some extent. In case of undesirable results such as overcorrection of airway and
resulting aphonia, it may not be possible to provide a serviceable voice again. In such a situation,
tracheotomy with a fenestrated tracheotomy cannula may even be more favorable. Treatment plan
then may be started from minimally invasive procedures.
Case Presentation
A fifty three years old female was referred to our clinical vocology unit with inspiratory stridor.
She has been operated for nodular thyroid disease 6 years ago. After total thyroidectomy, her
prominent problem has been severe stridor especially at night during sleep. Her breathing deficiency
got worse in the last year and she was not able to manage her daily life which was Grade 4 on MRC
Scale (Medical Research Council’s Breathlessness Scale) [9].
The patient was hospitalized and a combined operation was performed under general anesthesia.
After direct microlaryngoscopy, a mucosal incision was made medially and parallel to the superior
arquate line. Submucosal dissection of Reinke’s space was extended to the subglottic border of the vocal ligament. The vocal ligament and the thyroarytenoid muscle were truncated from its origin from the arytenoid cartilage. Muscle
immediately retracts away to the anterior direction and forms a bulk
for future phonation at the anterior glottis. It is important to truncate
the muscle with its two bellies (i.e. thyrovocalis and thyromuscularis)
with the vocal ligament. Then the mucosal incision was sutured by 8/0
vicryl in order to prevent granuloma formation. The Lichtenberger
suture instrument was then used for suture lateralization of the
posterior glottis. To decrease the risk of long-term soft tissue
loosening, three sutures were placed leaving 2 mm space in-between.
The first suture was placed 2 mm posteriorly to the tip of vocal
process. The second one was placed to the level of the vocal process.
These two sutures were aimed to provide an opposite vector to lateral
cricoarytenoid (LCA) muscle. The last suture was placed to the
posterior membranous glottis for closing the tissue gap which was left
by the truncated TA muscle (Figure 1).
Postoperatively, one year follow-up showed no dyspnea or
inspiratory stridor for daily life conditions. Despite a moderate
hoarseness (i.e. breathy voice) patient’s vocal communication was
not affected except in noisy environment. In the early postoperative
period, there was a moderate to severe anterior glottic edema but
posterior glottis was prominently open; the steroid medication
was given perorally and no tracheostomy was needed. After edema
was resolved, the MRC scale of breathlessness became grade 1 for
the patient. Mucosal defect was completely healed in the first week
and no granuloma formation was determined. Swallowing was not
affected, no aspiration was determined possibly because the arytenoid
bulk was left on site. Patient’s one year follow-up did not show renarrowing
of the posterior glottal gap (Figure 2).
Preoperatively, maximum phonation time was calculated as
3 seconds, it decreased to 2 seconds in postoperative assessment.
Interestingly, functional (F), physical (P), and emotional (E)
parameters in Voice Handicap Index (VHI) showed remarkable
improvement. Preoperative VHI results were F17, P19 and E15.
Postoperative findings were F9, P7 and E5. It was possibly due to
deleterious effects of preoperative dyspnea to communicative skills.
Figure 1
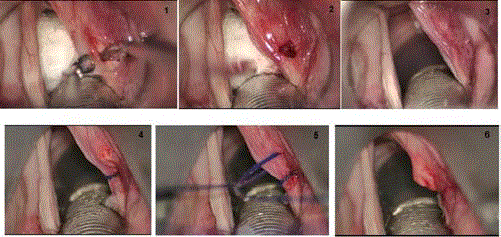
Figure 1
The operation procedure. Upper line from left: 1: Superolateral
incision of vocal folds mucosa and dissection of mucosa to the inferior border
of vocal ligament. 2: Truncation of vocal ligament and TA muscle until the
muscle is drawn away anteriorly. 3: Suturing the mucosa with 8/0 vicryl. 4-6:
Suture laterofixation by Lichtenberger’s needle carrier. The first suture was
placed 2 mm anteriorly to the vocal process. Others were placed posteriorly
to the first suture.
Figure 2
Figure 3
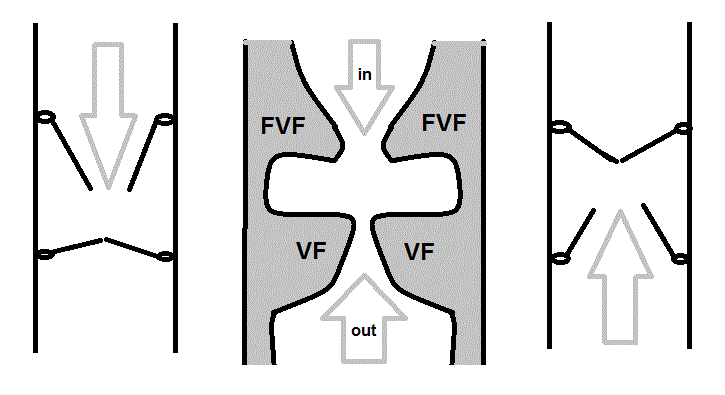
Figure 3
Schematic representation of double-valve function of larynx. FVF:
False Vocal Fold, VF: Vocal Fold, arrows point the direction of airflow.
Discussion
Overall success rate for surgical management of BVFI depends on
voice and breathing outcome. Various techniques have been described
to accomplish a balance between these two important quality of life
factors. Larynx is a complicated valve system and functions of larynx
are basically executed by that active valve mechanism. Vocal folds
function as a unidirectional valve which resists airflow from outsidein.
On the other hand, the ventricular folds (i.e. false vocal folds)
work oppositely as a unidirectional valve resisting airflow inside-out
direction in order to help for thoracic fixation function of larynx
(Figure 3).
Aerodynamic and biomechanical approach tells us that the
true VFs as the inside-out valve, works properly in BVFI but when
it comes to breathing, the valve function leads to an inspiration
deficiency. The possible solution lies behind muscular vectors and the
functional dominancy in glottis. The anterior two-thirds of the glottis
primarily comprise the phonatory function whereas the posterior one
third serves as the dominant component of the respiratory function
of the glottic space. Thus, in order to keep inspiration-phonationaspiration
in balance; three procedural aspects should be taken into
consideration:
1. A lateral movement of vocal process in the opposite direction of
LCA muscle by suture lateralization. This was done with lateralization
sutures which pass around the vocal process of the arytenoid cartilage.
2. Keeping the glottic valve function at the anterior part of
glottis for providing mucosal vibration or at least falsetto effect. The
vocal ligament and thyroarytenoid muscle with its two bellies were
truncated without excision. The body of the muscle was retracted
anteriorly to make a narrower anterior glottic space.
3. Prevention from aspiration by leaving the arytenoid bulk
on site. Vocal fold lateralization is a simple procedure if especially
performed by an endo-extralaryngeal needle carrier. The needle
carrier helps to place the suture to an exact point inside the larynx
with a single attempt which also minimizes edema and hematoma
in laryngeal tissues. Even under the best of circumstances, suture
lateralization may result in a severe edema of the lateralized VF and tracheostomy may be needed in the first week of suture lateralization
surgery. We used Lichtenberger’s needle carrier in our patient, a
meticulous dissection was made to minimize the tissue reaction. No
hematoma was observed in postoperative 3 days. Patient has had a
moderate dyspnea at the postoperative 5th day because of the edema at
the operated side. She was relieved after a short course of intravenous
steroid treatment and no tracheotomy was needed.
Long-term results of suture lateralization alone may not provide
enough airways possibly because the thread is loosened in time by
cutting the soft tissues. Fibrosis in the tissue then may not be enough
for a lateralization effect. In order to enhance this effect, lateralization
of true and false vocal folds by crossing sutures has been introduced
by Katilmis et al. [10]. Because the valve function of the ventricular
folds are against expiration (not inspiration), ventricular folds were
not included to lateralization procedure in our patient.
Arytenoidectomy, posterior cordectomy/cordotomy (even
assisted by laser) on the other hand, may result in granuloma
or hypertrophic scar formation which, in advance, may lead to
inspiratory stridor [11-13]. In order to prevent revision surgeries due
to persistent airway symptoms (re-narrowing scar tissue, granuloma
and tissue loosening after the single suture lateralization), we used
three sutures to minimize the long-term loosening of the tissues and
combined microlaryngeal posterior submucosal cordotomy with
suture lateralization for a greater space posteriorly. One year followup
did not show tissue reactions such as granuloma or hypertrophic
cicatrix and airway obstruction as well. The retracted vocal ligament
with the muscle was still obvious at the anterior vocal fold.
Conclusion
Microlaryngoscopic submucosal cordotomy combined with endolaryngeal triple suture revealed a favorable long-term followup in a BVFI patient. The submucosal cordotomy with minimally invasive dissection prevented further re-narrowing of the posterior glottic region by hypertrophic scar and granuloma formation. Triple suturing (one of which passes around the vocal process) provided effective lateral movement of vocal process. No aspiration was observed and tracheostomy was not needed after the operation. Among various surgical methods for management of BVFI, this new modification seems to provide an effective balance for laryngeal functions. Further studies on large patient groups are needed to confirm the affectivity of the method.
References
- Crumley RL. Laryngeal synkinesis revisited. Ann Otol Rhinol Laryngol. 2000;109(4):365-71.
- Swibel Rosenthal LH, Benninger MS, Deeb RH. A Longitudinal Analysis of Etiology Over 20 Years. Laryngoscope. 2007;117(10):1864-70.
- Jackson C. Ventriculocordectomy. A new operation for the cure of goitrous glottic stenosis. Arch Surg. 1922;4:257-74.
- Woodman D. A modification of the extralaryngeal approach to arytenoidectomy for bilateral abductor paralysis. Arch Otolaryngol. 1946;43:63-5.
- Thornell WC. Intralaryngeal approach for arytenoidectomy in bilateral abductor paralysis of the vocal cords; a preliminary report. Arch Otolaryngol. 1948;47(4):505-8.
- Kirchner FR. Endoscopic lateralization of the vocal cord in abductor paralysis of the larynx. Laryngoscope. 1979;89(11):1779-83.
- Ejnell H, Mansson I, Hallén O, Bake B, Stenborg R, Lindström J. A simple operation for bilateral vocal cord paralysis. Laryngoscope. 1984;94(7):954-8.
- Lichtenberger G. Endo-extralaryngeal needle carrier instrument. Laryngoscope. 1983;93(10):1348-50.
- Fletcher CM. The clinical diagnosis of pulmonary emphysema; an experimental study. Proc R Soc Med. 1952;45(9):577-84.
- Katilmis H, Ozturkcan S, Basoglu S, Aslan H, Ilknur AE, Karaca Erdogan N, et al. New technique for the treatment of bilateral vocal cord paralysis: Vocal and ventricular fold lateralization using crossing sutures with thyroplasty technique. Acta Oto-Laryngologica. 2011;131(3):303-9.
- Özdemir S, Tuncer Ü, Tarkan Ö, Kara K, Sürmelioglu Ö. Carbon dioxide laser endoscopic posterior cordotomy technique for bilateral abductor vocal cord paralysis: a 15-year experience. JAMA Otolaryngol Head Neck Surg. 2013;139(4):401-4.
- Khalil MA, Abdel Tawab HM. Laser Posterior Cordotomy: Is it a Good Choice in Treating Bilateral Vocal Fold Abductor Paralysis? Clin Med Insights Ear Nose Throat. 2014;7:13-17.
- Rinne J. Late results of laterofixation in the treatment of bilateral abductor paralysis of the vocal cords: A clinical study with long-term follow-up. Clin Otolaryngol Allied Sci. 1991;16(5):436-41.