Clinical Image
Protozoan Keratitis: Clinical Image
Maria Alejandra Benavides Cornea1, Maria Belisa Baldo2, Sara Guerrero3, Shachar Tauber4* and
Sandra Fernandez Figueiras5
1Department of Cataract and Refractive Surgery, Centro Medico Docente La Trinidad, Caracas Venezuela, USA
2Department of Retina, Centro Medico Docente La Trinidad, Caracas Venezuela, USA
3Department of Cornea Anterior Segment, Centro Medico Docente La Trinidad, Caracas Venezuela, USA
4Department of Cornea, Cataract and Refractive Surgery, Mercy Clinic, USA
5Department of Bioanalyst Microbiology and Molecular Biology, Centro Medico Docente La Trinidad Caracas,
Venezuela, USA
*Corresponding author: Shachar Tauber, Department of Cornea, Cataract and Refractive Surgery, Mercy Clinic, 1229 East Seminole Suite 430 Springfield, Missouri 65804, USA
Published: 05 May, 2017
Cite this article as: Cornea MAB, Baldo MB, Guerrero S,
Tauber S, Figueiras SF. Protozoan
Keratitis: Clinical Image. Clin Surg.
2017; 2: 1464.
Clinical Image
The patient is a 69-year-old male, dentist, who was referred to theCornea Clinic Ophthalmology
Service of Centro Medico Docente la Trinidad because of pain, photophobia and blurred vision in his
left eye. The patient remembers having a foreign body like traumatic event while polishing a dental
implant one monthbefore we examined him, and just before he left for vacation, travelling from
Venezuela to Texas, USA, where he went swimming in several pools and went fishing and swimming
in Lake Comroe, near Houston.On his third week abroad he began noticing photophobia, blurred
vision, swelling of the eyelid on his left eye. He returned to Venezuela,consulted an ophthalmologist
and was referred to our service on July 27, 2016.
On examination we found:
BCVA: RE: 20/30;LE: 20/60; Biomicroscopy: RE: Revealed moderate nuclear sclerosis of
the lens; LE: revealedan edematous upper eyelid with ptosis with hyperemic conjunctivae. Most
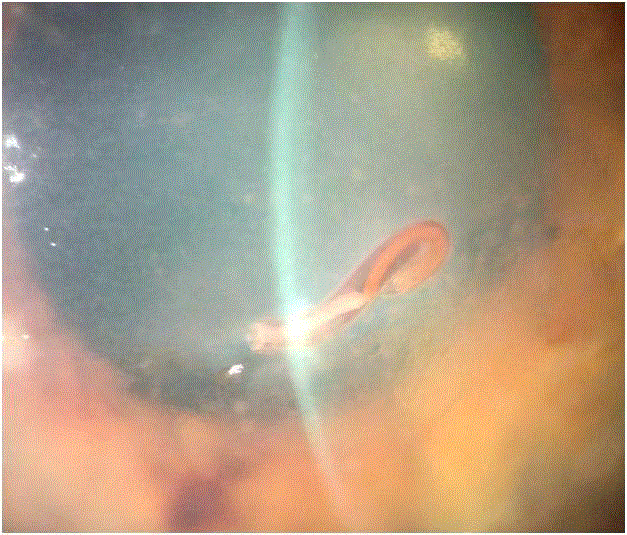
remarkable the anterior stroma of the paracentral cornea revealed the presence of an encapsulated
worm measuring 2 mm × 3 mm diameter. Therewas also coarse pigmented endotelitis and edema of
the stroma (Figure 1); IOP: 18 in each eye; Fundus: within normal limits bilaterally.
General exams for systemic infection or pathology were within normal limits.
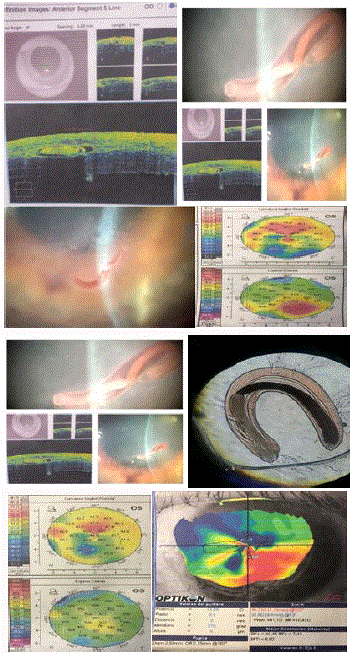
An anterior segment OCT was obtained, Figure 2 revealing the encapsulated organism with
the anterior half of the cornea stroma. The patient underwent urgent partial thickness keratectomy
the next day, under local anesthesia. Theworm was removed in its totality, without rupture of the
surrounding capsule and the material was immediately sent to the microbiology lab where we were
able to obtain live video of the worm moving.
A partial thickness graft was not performed as there was good predicted residual corneal bed
thickness (373 to 420 microns), and concern regarding graft survival due tosevere inflammation of
the borders of the resected tissue.
Moxifloxacin drops every 6 hours, lotesoft every 8 hours,and an oral cycle of albendazol every 12 hours for 10 days were prescribed.
Photographs and videos where studied at our institution at
Microbiology and Molecular biology, Centro Medico Docente La
Trinidad and sent abroad to Kittisak Sawanyawisuth, Associate
Professor Department de Medicine Faculty of Medicine KhonKaen
University, Thailand. We concluded the specimen to be a Gnathostoma
binucleatum.
Despite no clinical findings of skin granulomas or other
neurological or ophthalmic clinical findings a treatment cycle with
albendazol 400 mgq 12 for 10 days was prescribed for systemic
prophylaxis given thehistory of swimming and fishing in river water
and the possibility of swallowing amounts oflarvaeinfested water.
The patientwas seen in later visits with a good visual recovery (20/40)
despite a residual astigmatism of 5 diopters and a low maintained
steroid dose(Loteprednoletabonato).
On September 2016, a phacoemulsification of the cataract in his
right eye was scheduled, but was lost to follow up. The patient did not
come back until February 2017. He had stopped the steroid drops
and was found to have20/80 vision with a central haze, endothelitis
and cataract in the left eye. The patient had also been noted to
have suffered a strokeresulting in left hemiparesia and hypoalgesia.
Blood analysis revealedelevated white cell count of 28,000 cell/ml
andelevated eosinophilsof 45%. Lumbar puncture opening pressure
and LCR fluid analysis were normal. Further workup showed an
abdominal aneurism with mural thrombosis and an upper left renal
tumor were discovered on abdominal ultrasound.
Because the Gantostoma is not a common parasite in Venezuela,
we present our case to stress the importance of carefully obtaining a
good history.
Initially when infectious disease consultants examined the patient
they first considered Onchocerca volvulus, a parasite that causes larva
migrans and is more frequent in Venezuela. Even though the etiology
of the hypereosinophilicsyndrome and the stroke has to be studied,the
recent contact with the Gnathostoma opens a differential diagnosis
probability that has to be considered. Therefore, the importance of
documenting and having prompt access to the information for all the
clinics treating the patient over time.