Research Article
Right Sided Reconstruction of the Heart for Invasive Angiosarcoma of the Right Atrium
Elien Brouwers1, Marie-Christine Herregods1, Eric Verbeken2, Paul Herijgers3 and Wouter
Oosterlinck3*
1Department of Cardiovascular Diseases, Cardiology, University Hospitals Leuven, Belgium
2Department of Imaging and Pathology, University Hospitals Leuven, Belgium
3Department of Cardiovascular Diseases, research unit of Cardiac Surgery, University Hospitals Leuven, Belgium
*Corresponding author: Wouter Oosterlinck, Department of Cardiac Surgery, University Hospitals Leuven Herestraat 493000 Leuven Belgium
Published: 04 May, 2017
Cite this article as: Brouwers E, Herregods M-C, Verbeken
E, Herijgers P, Oosterlinck W. Right
Sided Reconstruction of the Heart for
Invasive Angiosarcoma of the Right
Atrium. Clin Surg. 2017; 2: 1460.
Abstract
A 35-year old male presented with new diagnosis of cardiac angiosarcoma. We describe the case,
diagnosis, treatment modalities and first observations concerning survival.
Overall, cardiac sarcomas are a rare entity. There are several subtypes of sarcomas and the
angiosarcoma is the most common type of heart sarcomas in adults, especially in male population.
The symptoms of cardiac sarcomas are non-specific and depend on the size of the tumor, the
anatomical localization, the myocardial involvement and the presence of metastatic disease.
Dyspnea is the most common symptom by diagnosis.
The number of angiosarcomas diagnosed, has increased since non-invasive imaging
(echocardiography, MRI, CT) has improved in quality.Final diagnosis can only be made by
cytological and immunohistochemical examination.Once the diagnosis has been established, the
therapy has to be started as soon as possible.
Most important in the treatment of sarcomas is a complete surgical resection, as this gives the most
successful disease-free survival. Until now, the role of chemotherapy is unclear.
Unfortunately, the prognosis of cardiac sarcomas is poor.The median time to relapse is longer in
patients with angiosarcoma than other sarcomas.
Keywords: Angiosarcoma; Cardiac malignancy; Cardiac tumor; Diagnosis; Treatment
Abbreviations
RA: Right Atrium; LA: Left Atrium; LV: Left Ventricle; RV: Right Ventricle; MRI: Magnetic Resonance Imaging; CT: Computed Tomography; FDG- PET: Fluorodeoxyglucose - Positron Emission Tomography; TTE: Transthoracic Echocardiography; TEE: Transesophageal Echocardiography; RCA: Right Coronary Artery; CABG: Coronary Artery Bypass Grafting
Introduction
Primary cardiac tumors are a rare entity (0.0017 to 0.033%, based on autopies)[1-6]. Most
cardiac tumors are metastastic locations of other primary tumors.About 75% of the primary cardiac
tumors are benign, and 75% of these benign tumors are myxomas [4,5,7].The remaining 25% of the
primary tumors of the heart are malignant, with a majority of sarcomas (75%) [2,3,5,7]. Median
survival for cardiac sarcomas is only six months [4,5].
Cardiac sarcomas can be divided into three categories, based on localization: right heart sarcoma
(as in our case), left heart sarcoma or pulmonary artery sarcoma [8]. There are several subtypes
of sarcomas; the angiosarcoma is the most common type of heart sarcoma in adults, especially in
male population [6,8]. One third of the heart sarcomas (37%) is estimated to be angiosarcomas
and male-female ratio is 2-3/1 [4,5,10]. Other types of cardiac sarcomas are rhabdomyosarcoma,
osteosarcoma, leiomyosarcoma, undifferentiated sarcoma and primary cardiac lymphoma [3].Mean
age at diagnosis of angiosarcoma is forty and 90% is right-sided [3,5,7]. The most common type of
heart sarcoma in children is rhabdomyosarcoma[6].
Angiosarcomas are endothelial cell tumors and have a poor prognosis due to their aggressive
nature (early metastatic disease and infiltration) and delay in onset and diagnosis [2,7-9].
Case Presentation
A 35-year old male presented with palpitations and progressive
dyspnea since five weeks.ECG showed atrial fibrillation and
transthoracic echocardiography (TTE) demonstrated a large right
intra-atrial mass (7.8 x 5.2 cm), infiltrating the interatrial septum
and the tricuspid valve. There were no signs of right ventricular
inflow obstruction. Initial medical treatment consisted of systemic
anticoagulation and rhythm control using amiodarone.
He was immediately referred to our hospital for further
investigation. ECG showed sinus rhythm. TEE and cardiac MRI
confirmed a large intra-atrial mass (59x 49x 68 mm) and because of
the density, the irregular shape and the localization, an angiosarcoma
was suspected (Figure 1).
In addition infiltration of the pericardium and pericardial effusion
were found. A FDG-PET/CT scan did not show signs of metastatic
disease. Coronary angiography showed normal coronary arteries. The
right filling pressures were normal.
After fourteen days, a resection was performed under general
anesthesia and full extracorporeal circulation (Figure 2).
Opening of the pericardium confirmed the effusion and there
were spot lesions on the aorta and pulmonary artery. These were
evaluated by frozen sections, ruling out malignancy before the
resection was performed. Bicaval cannulation high in the vena cava
superior and from the femoral vein allowed a macroscopic complete
resection including the right atrium, the roof of the left atrium, the
membranous atrioventricular and interventricular septum, the
tricuspid valve and the basis of the free wall of the right ventricle.
A reconstruction of the fibrous part of the septum and tricuspid
annulus allowed implantation of a tricuspid bioprosthesis (Mosaic
33). Right and left atrium and the basal part of the right ventricle were
reconstructed using pericardial patches. The vena cava superior was
reconstructed using a PTFE graft. CABG was performed on branches
of the right coronary artery using a saphenous vein graft.
Patient was weaned uneventfully from extracorporeal circulation.
The ECG showed an ectopic atrial rhythm. He was extubated twenty
hours after the operation. A permanent pacemaker was implanted
after ten days because of persistent total AV-block. After surgery
pleural punctions (temporary pigtail) were performed for relapsing
right sided pleural effusion, with a total hospitalization time of four
weeks.
Pathologic examination showed a classic angiosarcoma,
with resection margins free of tumor. CD31 and CD34
immunohistochemical staining was positive, confirming vascular
differentiation and the diagnosis of an angiosarcoma (Figure 3).
After multidisciplinary consultation between oncologists,
pathologists, radiologists and cardiac surgeons, three possible treatment options were proposed to the patient (watchful waiting,
intensive adjuvant chemotherapy (doxorubicin/ ifosphamide) or
paclitaxel monotherapy). In agreement with the patient an intensive
adjuvant chemotherapy treatment was initiated.
Preliminary evaluation using computed tomography (CT) after
three cycles of chemotherapy showed several subcentimetric liver
lesions. PET-CT showed normal metabolism in the liver, no arguments
for metastatic liver disease.Up until the moment of evaluation there is
a survival of six months, with a NYHA classification I.
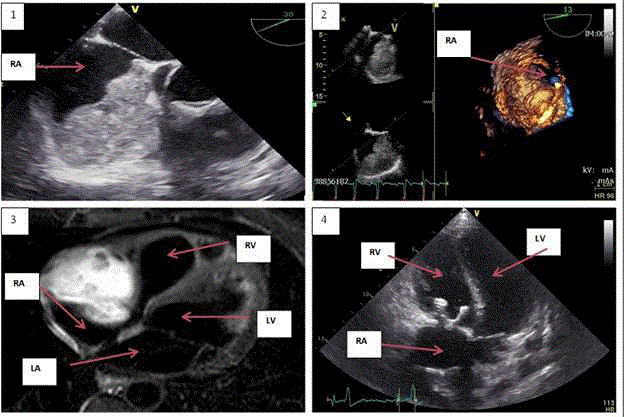
Figure 1
Figure 1
Pre- and postoperative imaging.
1 + 2. Pre-operative echocardiography (TEE): large right atrium mass.
3. Pre-operative MRI: large right atrium mass.
4. Post-operative echocardiography (TTE).
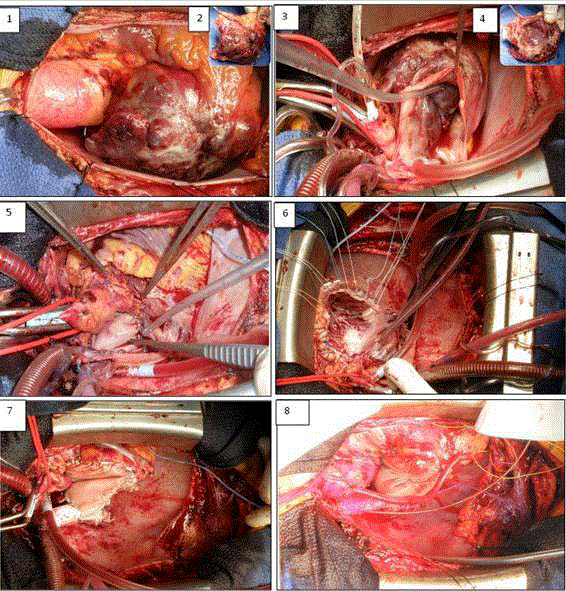
Figure 2
Figure 2
Overview of surgical procedure and reconstruction.
1. Pre-operative situation.
2. Macroscopic removement of the tumor; outside wall.
3. After removement of the tumor.
4. Macroscopic removement of the tumor; inside wall.
5. Closure of RC ostium and of closure LA.
6. Reconstruction base tricuspid by patch and placement of prosthetic valve,
followed by reconstruction VCS.
7. Patch reconstruction RA with venous CABG to branches RCA.
8. End result in reperfusion phase.
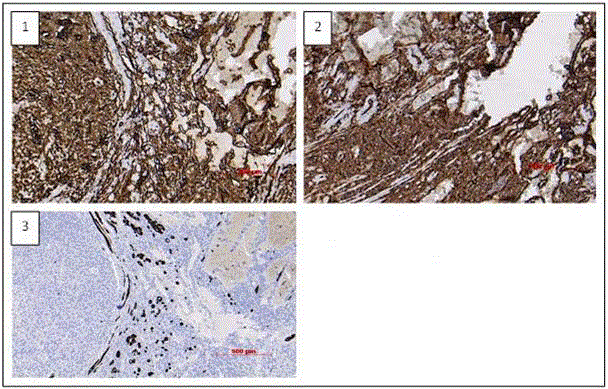
Figure 3
Figure 3
Histological evaluation
1. CD 31 positive (vessel marker).
2. CD 34 positive (vessel marker).
3. Desmine positive cells (myocard fibers), which proves it is a heart tumor.
Discussion
Symptoms
The symptoms of cardiac sarcomas are non-specific. They depend
on the size of the tumor, the anatomical localization, the myocardial
involvement and the presence of metastatic disease [3,4,7]. Dyspnea
is the most common symptom by diagnosis [3,9].
Symptoms may be systemic (e.g. anorexia, fatigue, fever, weight
loss) but also signs of obstructive cardiac invasion (e.g. pulmonary
edema, syncope, sudden cardiac death), arrhythmias (e.g. atrial
fibrillation, ventricular arrhythmias) or signs of right-sided heart
failure, pericardial effusion and cardiac tamponade may occur.
Sometimes, systemic embolization causes the first sign (e.g. stroke,
transient ischemic attack, myocardial infarction)[3,4,5,7].
Diagnosis
The number of angiosarcomas diagnosed, has increased since
non-invasive imaging (echocardiography, MRI, CT) has improved
in quality [4]. The rarity and variation and specificity in presenting
symptoms explain the delay in diagnosis [9].Other tumors that
can mimic angiosarcomas are benign entities such as myxomas or
pseudotumors (like thrombus, vegetation, and abscess.)[4]. Also
metastasis of other tumors as well as other sarcomas, mesotheliomas
or lymphomas has to be considered [9].
Diagnosis is made using echocardiography, computed
tomography (CT), magnetic resonance imaging (MRI), positron
emission tomography (PET), and catheterization. Cardiac
ultrasound is an important diagnostic method [3,5,7]. It is routinely
used, noninvasive, cheap and can give information about the size
and the localization of the tumor. Computed tomography and
magnetic resonance imaging give clues to the subtype of tumor, as
angiosarcomas are known for their irregular shape and invasion of the
pericardium [3]. Positron emission tomography is used for detection
of metastatic disease. They show the localization and relationship
with other structures. A coronary angiography evaluates the coronary
arteries before surgery, also to evaluate the possibility of resection and
reconstruction.
Criteria suggesting malignancy are size >50 mm, involvement
of more than one chamber of the heart, hemorrhagic pericardial
effusion and infiltration into the vessels or mediastinum [4].
Like in our case, there was a large intra-atrial mass of 59 mm
with infiltration of the pericardium and the presence of a pericardial
effusion.Macroscopically, the tumors are usually hemorrhagic and
necrotic, with a dark red or brown appearance [9].
Final diagnosis can only be made by cytological and
immunohistochemical examination[4]. An angiosarcoma is a
malignant tumor that contains cells with endothelial differentiation
[3]. Diagnosis is confirmed by presence of endothelial markers, such
as CD31 and CD34 [3,9]. CD 31 is positive in 90% of angiosarcomas
and is highly sensitive and specific for vascular neoplasma[9]. CD 34
is less sensitive and is positive in 50-74% of all angiosarcomas [9].
Once the diagnosis has been established, the therapy has to
be started as soon as possible. Multidisciplinary collaboration of
the cardiologist, cardiac surgeon, radiologist and oncologist is
essential[4,6]. Due to the small number of angiosarcomas, there are
currently no evidence-based treatment guidelines yet [3,5]. Most
important in the treatment of sarcomas is total surgical resection;
it gives the most successful disease-free survival [4]. Surgery can be
challenging given the localization of the tumor and infiltration in
nearby tissue, and therefore isn’t always possible.It is restricted to a
small number of patients because of the large number of metastatic
disease by diagnosis [3]. When there are extracardiac manifestations,
surgical resection has no survival benefit [7]. In many cases, an
anatomic and functional reconstruction is only possible with an atrial
patch, as in our patient.
The role of chemotherapy is unclear, given the limited experience
in these types of tumors. Sometimes neo-adjuvant chemotherapy is
given to reduce the size of the tumor [4]. Adjuvant therapy mostly
includes anthracyclines (e.g. doxorubucine) and nitrogen mustard
alkylating agents (e.g. cyclophosphamide, ifosphamide) [4,6].
Given lack of hard evidence for chemotherapy in angiosarcomas,
chemotherapy protocols from extracardiac soft tissue studies are used
[10]. Most oncologists prescribe an adriamycine based therapy [6].
The most common regimen is doxorubicin and ifosphamide [7,10].
When surgery isn’t possible, palliative chemotherapy can be given
to reduce symptoms [4]. Radiation therapy is sometimes used in
people with pulmonary artery sarcomas, but is usually not an option
in cardiac sarcomas due to complications (e.g. chronic pericarditis,
cardiomyopathy) [7,10]. The heart in itself is more sensitive to
radiation than the tumor [7].
There are no universal guidelines for treatment but complete
resection of the tumor followed by adjuvant chemotherapy is
estimated as the most optimal strategy [4,7]. Further investigation in
(neo-)adjuvant chemotherapy is necessary.
Prognosis
Prognosis of cardiac sarcomas ispoor. Most people (>80%) die
within one year after diagnosis [4,5,7].In 66-89% of cases with cardiac
angiosarcoma, there is metastatic disease at the time of diagnosis
[3,8]. Pulmonary metastases are most common. Occasionally there
can also be metastases in the lymph nodes, bone, liver, brain, bowel,
spleen, adrenal glands, diaphragm, kidneys, thyroid and skin [3].
Angiosarcomas have an aggressive biological nature and given their
rarity aren’t suspected initially [3,4,6,9].However, early detection can
improve disease free survival [3].The size and the localization of the
sarcoma are more important for prognosis than histological subtype
[4].Localization in the left heart might have a better prognosis [4,5].
Right heart sarcomas are more likely to induce late symptoms, are
more infiltrative and produce earlier metastatic disease than left
heart sarcomas [4]. Left heart sarcomas would have a lower mitotic
index [5]. The median time to relapse is greater in patients with
angiosarcoma than other sarcomas [6]. Surgical resection for cardiac
sarcomas give a median survival of twelve months [4,6].Without
treatment the survival is less than a month [4].
Learning Objectives
With this case we describe a complete surgical resection with complex reconstruction of right side of the heart after an invasive angiosarcoma of the right atrium. This case description could be a stepping stone for other surgeons and future treatments of right sided angiosarcomas. It addition, it includes an overview of the current available literature and possible additional chemotherapeutic that could be used.
References
- Meng Q, Lai H, Lima J, Tong W, Qian Y, Lai S. Echocardiographic and pathologic characteristics of primary cardiac tumors: a study of 149 cases. Int J Cardiol. 2002;84(1):69-75.
- Cadgas Baran, Serkan Durdu, Sadik Eryilmaz, Mustafa Sirlak, A Ruchan Akar. Primary left cardiac angiocsarcoma with mitral valve involvement accompanying coronary artery disease. Case rep Surg. 2015; 810306.
- Wobbe Bouma, Chris PH Lexis, Tieke P Willems, Albert H Suurmeijer, Iwan CC van der Horst, Tjark Ebels, et al. Successful surgical excision of primary right atrial angiosarcoma. J Cardiothorac Surg. 2011;6:47.
- Bartosz Hudzik, Karol Miszalski-Jamka, Jan Glowacki, Andrezej Lekston, Marek Gierlotka, Marian Zembala, et al. Malignant tumors of the heart. The international journal of cancer epidemiology, Detection and Prevention. 2015;39:665-72.
- Neragi-Miandoab S, Kim J, Vlahakes GJ. Malignant tumours of the heart: a review of tumour type, diagnosis and treatment. Clin oncol. 2007;19(10):748-56.
- Kurian KC, Weisshaar D, Parekh H, Berry GJ, Reitz B. Primary cardiac angiosarcoma: case report and review of the literature. Cardiovascular pathology. 2006;15(2):110-12.
- Reardon MJ, Walkes JC, Benjamin R. Therapy insight: malignant primary cardiac tumors. Nat Clin Pract Cardiovasc Med. 2006;3(10):548-53.
- Amonkar GP, Deshpande JR. Cardiac angiosarcoma. Cardiovasc Pathol. 2006;15(1):57-8.
- Swetal Dilip Palel, Ashley Peterson, Artur Bartczak, Sarah Lee, Slawomir Chojonwki, Piotr ajewski, et al. Primary cardiac angiosarcoma – a review. Medical science monitor. 2014;20:103-9.
- Augusto Orlandi, Amedeo Ferlosio, Mario Roselli, Luigi Chiariello, Luigi G Spagnoli. Cardiac sarcomas, an update. J Thorac Oncol. 2010;5(9):1483-89.