Research Article
Transcervical Approach for Thoracic Operations
Marcin Zieliński1*, Wojciech Czajkowski1, Sylweriusz Kosinski2, Edward Fryzlewicz2, Tomasz
Nabialek2, Juliusz Pankowski3, Mariusz Rybak1,4, Katarzyna Solarczyk-Bombik1,4 and Michal Wilkojc1,4
1Department of Thoracic Surgery, Pulmonary Hospital, Poland
2Department of Anaesthesiology and Intensive Care, Pulmonary Hospital, Poland
3Department of Pathology, Pulmonary Hospital, Poland
4Department of Surgery, Pulmonary Hospital, Zakopane, Poland
*Corresponding author: Marcin Zieliński, Department of Thoracic Surgery, Pulmonary Hospital Ul. Gładkie 1 34 500 Zakopane, Poland
Published: 28 Apr, 2017
Cite this article as: Zieliński M, Czajkowski W, Kosinski S,
Fryzlewicz E, Nabialek T, Pankowski
J, et al. Transcervical Approach for
Thoracic Operations. Clin Surg. 2017;
2: 1447.
Abstract
Aim: The aim of this study is to summarize our experience regarding thoracic operations performed
through the use of the extended transcervical approach.
Material and Methods: Transcervical extended approach utilizes a collar incision in the neck with
elevation of the sternal manubrium with a mechanical retractor. A bilateral visualization of the
laryngeal recurrent and vagus nerves is usually performed to avoid injury of these structures. The
procedures performed solely through the transcervical incision, or combined with videothoracoscopy
(VATS) or/and subxiphoid incision were analyzed.
Results: There were 1,984 transcervical operations from September 01, 2000 to September 30,
2016, including 405 transcervical-subxiphoid VATS maximal thymectomies for myasthenia
gravis, thymomas or rethymectomies, 1,224 transcervical extended mediastinal lymphadenectomy
(TEMLA) procedures for staging of non-small cell lung cancer (NSCLC), 332 resections of the
mediastinal tumors and the mediastinal metastases (mostly from thyroid cancer), 17 pulmonary
lobectomies combined with TEMLA for NSCLC and 6 attempts of closure of the right main bronchus
postpneumonectomy fistula. There were 5/1984 (0.3%) patients who had to be converted because of
technical difficulties, in no case there major bleeding, or other severe intraoperative complications
or deaths. There were 14/1984 (0.7%) patients who required revision because of postoperative
bleeding (through the original incision in all but one patient, who necessitated thoracotomy). There
was morbidity of 6.2 % (128/1984) and mortality of 0.4% (7/1984).
Conclusions: Transcervical extended approach with elevation of the sternal manubrium enables
performance of various thoracic surgical procedures with minimal invasiveness, low mortality and
morbidity and very high effectiveness.
Keywords: Thoracic operations; VATS; Thoracic surgery
Introduction
Most of general thoracic surgical operations are performed through the traditional thoracotomy,
sternotomy or videos-assisted thoracic surgery (VATS) approach. Significant severity of pain is
a common disadvantage of all these procedures, even in case of VATS. In recent years our team
developed the transcervical extended approach for various thoracic surgical procedures, originally
introduced by Cooper et al. [1] for thymectomy.
The extended transcervical approach for thoracic operations is characterized by the use of
elevation of the sternal manubrium; otherwise it would not be possible. With elevation, however the
cervical wound is like utility thoracotomy for video-assisted thoracic surgery (VATS), which enables
performance of a variety of operations. The transcervical thoracic operations are divided into two
categories. One type includes procedures performed solely through the cervical incision without
additional approaches. Such procedures might be done with preservation of the mediastinal pleura,
or may include deliberate opening of the pleural cavity. The other type of procedures combines
a transcervical approach with VATS and/or subxiphoid incision. Nevertheless, the transcervical
extended approach with elevation of the sternum is the common feature of all these procedures.
This article is based mainly on our institutional experience, with description and discussion
of the techniques we introduced or developed. Procedures such as standard mediastinoscopy,
video-mediastinoscopy, anterior mediastinotomy, the tracheal and
esophageal procedures will not be described here.
Figure 1
Figure 2
Figure 3
Surgical Technique of the Transcervical Extended Approach
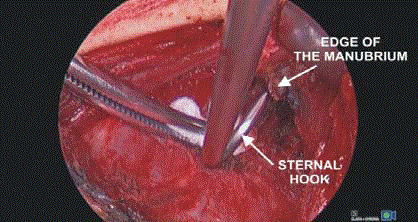
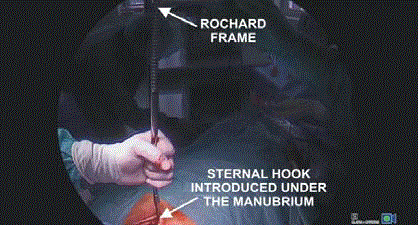
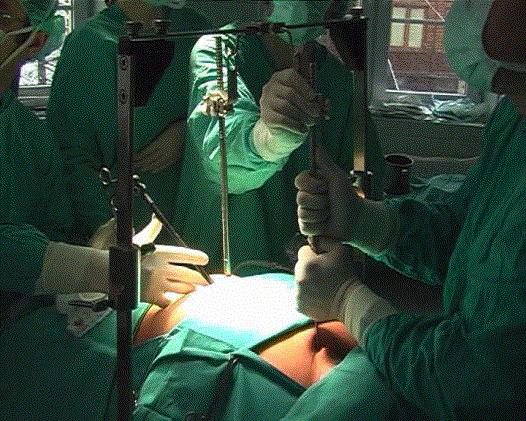
Transcervical extended approach utilizes a typical a 5 cm to 8
cm collar incision in the neck. The critical technical point enabling
a wide access to the chest is an elevation of the sternal manubrium
with a special retractor (modified Rochard frame, Asculap-Chifa,
Poland) (Figure 1 and 2). Even though the elevation of the sternum
does not create a big enlargement of the wound, nevertheless it
facilitates access to the mediastinum with the aid of the Linder-Dahan
expandable blades mediastinoscope (Richard Wolf, Germany) or/
and long narrow wound retractors. The very important maneuver is a
bilateral visualization of the laryngeal recurrent and vagus nerves are
usually performed to avoid injury of these structures [2].
The subplatysmal flaps are dissected well outside the area of skin
incision. Omission of such extensive dissection creates an obstacle for
further dissection inside the mediastinum.
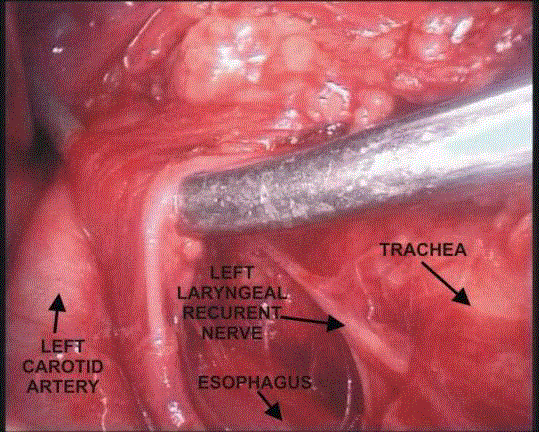
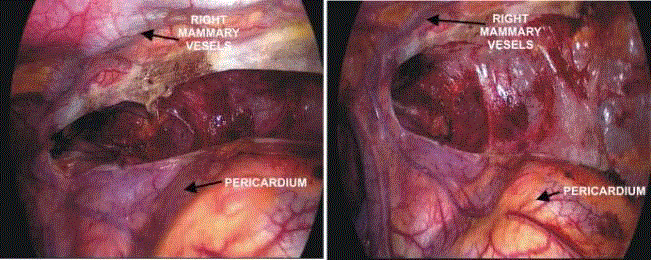
Visualization of both laryngeal recurrent and vagus nerves is
achieved with division of the fascial layers of the carotid sheath
covering these nerves (Figure 3). During visualization of the recurrent
nerves it is recommended to preserve the last, deepest fascial
membrane covering the nerve to avoid its injury. Circumferential
dissection of any nerve is not advised.
Both vagus nerves run laterally to the carotid arteries. To expose
these nerves, which are important landmarks of further dissection,
one must open the carotid sheath and dissect the vagus nerve running
between the carotid artery and the internal jugular vein.
Elevation of the sternum with a hook inserted under the
manubrium is an extremely important maneuver because it widens
the access to the mediastinum. We use a hook with sharp teeth (with
1 or 3 teeth) connected to the frame mounted to the operating table
(Rochard frame, Aesculap-Chifa, Poland). An operator stands behind
the patient’s head and the assistant stands on the operator’s right side.
The biggest part of the transcervical operation is an open surgical
procedure performed with standard surgical instruments. Only for
dissection of the structures located deep in the mediastinum dissection
is performed with aid of the Linder-Dahan mediastinoscope [3]. For
better illumination of the operating field and teaching purposes a
videothoracoscope might be used for dissection of aorta-pulmonary
window area. In some patients the mediastinal pleura is preserved,
it might be necessary however to open the pleura deliberately, or
it is done incidentally. In case of injury of the mediastinal pleura,
expansion of both lungs with high positive end expiratory pressure
(PEEP) and insertion of the fibrin sponge to seal the pleural injury is
usually suffice to manage the problem. Generally, chest tube insertion
is not necessary.
Types of Surgical Operations Performed through the Extended Transcervical Approach
The extended transcervical can be used for thymectomy, for
myasthenia gravis and thymoma, rethymectomies, resection of the
benign or early-stage malignant mediastinal tumors and resection
of the metastatic mediastinal lymph nodes. The most advanced
transcervical procedures include closure of the bronchial stump
postpneumonectomy fistula and pulmonary resections, including
wedge resection and lobectomy.
Transcervical thoracic operations performed solely
through the neck
These procedures include transcervival extended mediastinal
lyphadenectomy (TEMLA), transcervical thymectomy and
rethymectomy, resection of the priomary and metastatic
mediastinal tumors and closure of the bronchopleural fistula after
pneumonectomy.
Surgical technique of TEMLA
The technique of this procedure introduced by the first author
of this article (MZ) was described elsewhere [3] the detailed
discussion of possible pitfalls and the methods of management of
intraoperatice complications were published elsewhere [4]. In brief,
the technique of TEMLA included dissection of all mediastinal
nodal stations except for the pulmonary ligaments nodes (station 9).
Most of the procedure was performed in the open fashion, with the
subcarinal and the periesophageal nodes (stations 7 and 8) removed
in the mediastinoscopy-assisted technique and the paraaortic and
the pulmonary-window nodes (stations 6 and 5) removed in the
videothoracoscopy-assisted technique, with the videothoracoscope
inserted through the transcervical incision. Generally, the mediastinal
pleura were not violated and no drain was left in the mediastinum.
Bilateral supraclavicular lymphadenectomy and even deep cervical
lymph node dissection is possible during TEMLA through the same
incision.
Mediastinal tumors
Technique of resection of the mediastinal tumors and the
mediastinal metastases is virtually similar to the technique of
TEMLA. In case of larger tumors transcervical incision is combined
with VATS. There are four types of localization of the mediastinal
tumors that can be removed with the use of transcervical approach.
There are tumors of the superior mediastinum, located above the level
of the tracheal bifurcation. These tumors can be further differentiated
in the anterior, middle and posterior categories. The other type
is tumors located in the inferior mediastinum, below the tracheal
bifurcation. The transcervical approach can be useful in removal of all
these tumors. Radical surgery can be performed in the encapsulated
tumors, or in selected patients with limited infiltration out of the
capsule. In case of more extensive tumors a transcervical incision
is combined with VATS and subxipoid incision, or a classic open
approach through sternotomy or thoracotomy is used for complete
resection. The size of the tumor is also important. Although, there is
no specific size limit for the use of transcervical approach, however,
it would be extremely difficult to remove completely the tumors of a
diameter larger than 8 cm to 10 cm, without disruption of the tumors’
capsule.
The tumors of the superior anterior mediastinum include
mainly ectopic goiter and thymic tumors like thymomas and cysts.
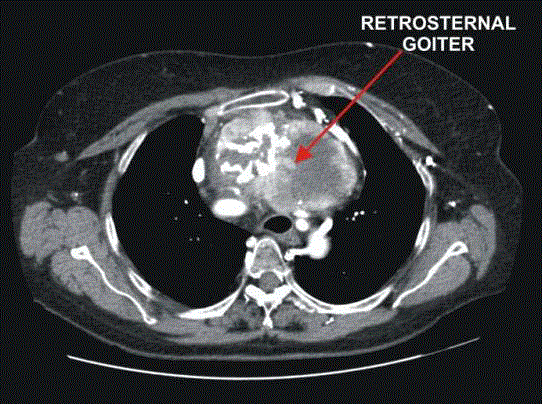
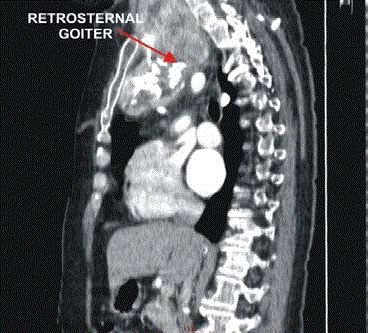
The next category is retrosternal goiters with significant part of the
mass located in the mediastinum (Figure 4 and 5). The other types
of tumors are metastatic nodules of various origin (thyroid cancer,
ectopic parathyroids and the others) and germ cell tumors (rarely
applicable for transcervical resection due to large size at presentation).
The tumors of the superior middle mediastinum include
metastatic nodes, ectopic parathyroids and mediastinal cysts (Figure
6).
Tumors located in the aorta-pulmonary area also belong to this
category. The tumors of the superior posterior mediastinum are
usually neurinomas.
There are selected tumors of the inferior mediastinum that
can be resected through the transcervical approach. These tumors
include mediastinal cysts and metastatic nodes positioned close
to the esophagus and the bronchi. The other tumors of the inferior
mediastinum cannot be removed with the transcervical technique.
Thymectomy and rethymectomy
Surgical technique of transcervical thymectomy is virtually the
same as described by Cooper et al. [1]. Contrary to the other authors
we did not use this approach for nonthymomatous myasthenia
gravis (MG), but for small cranially located thymic tumors or cysts.
However, for the majority of early-stage thymomas, however we use
the transcervical-subxiphoid-VATS or the subxipoid-right VATS
approaches, described elsewhere [5,6].
During transcervical repeated thymectomy (rethymectomy) we
a technique similar to that described by Komanapalli et al. [7]
including deliberate opening of both pleural cavities to achieve better
control of complete removal of the adipose tissue of the superior
and anterior mediastinum. We used this approach for patients who
underwent previous VATS thymectomy. In case of large amount of
fatty tissue after previous VATS thymectomy we used transcervicalsubxipid-
bilateral VATS approach.
Technique of closure of the bronchial fistula after
pneumonectomy
The approach to the main bronchus is achieved in same way as
during TEMLA. The main bronchus is dissected circumferentially,
and then the endostapler is applied and fired.
Transcervical pulmonary lobectomy
Transcervical lobectomy can be performed with the use of
the uniportal technique, or one or two additional VATS port as be
described previously [8,9].
The uniportal transcervical VATS lobectomy for NSCLC is
preceded by TEMLA to enable optimal intraoperative staging of the
mediastinal nodes and perform extensive bilateral lymphadenectomy,
which theoretically might affect survival. VATS lobectomy is the next
step after obtaining results of intraoperative examination of the nodes
performed with the imprint cytology technique [10]. Ventillation of
the operated lung is disconnected and the mediastinal pleura are
opened. Pleural adhesions are divided. The branches of the pulmonary
artery and vein and the lobar bronchus are sequentially dissected and
managed with endostaplers. The fissure is divided with endostapler
and the resected lobe is removed in an endobag.
Transcervical thoracic operations combined with VATS
and/or the subxiphoid incision
These procedures include transcervical-subxiphoid-VATS
maximal thymectomy for myasthenia gravis (MG) or/and early stage
thymoma, pulmonary resection of the right and left upper lobes,
and esophagectomy performed through transcervical-laparotomy
(laparoscopy) approach.
Technique of transcervical-subxiphoid-VATS maximal
thymectomy
The cervical incision is combined with the subxiphoid incision
and bilateral single-port VATSA. Two sternal retractor connected to
the Rochards frame are used, one for the elevation of the manubrium
and the second one is placed under the sternum, which is elevated
to facilitate access to the anterior mediastinum from below (Figure
7). An operation may be performed by two teams – one called the
“cervical team” working from above and the second one called, “the
subxiphoid team” working from below the sternum with control of
the videothoracoscope (VATS). Alternatively, the whole operation is
performed by one surgical team performing “the cervical” and “the
subxiphoid” parts of the operation sequentially. The whole thymus
with the surround fatty tissue of the areas of the neck, perithymic,
aorta-caval groove, aorta-pulmonary window and the right and left
epiphrenic fat pads is removed en-bloc.
Figure 4
Figure 5
Figure 6
Figure 7
Figure 7
The view of the mediastinum before and after elevation of the
sternum during thymectomy with significant widening of the space between
the sternum and the pericardium after elevation of the sternum.
Table 1
Table 2
Table 2
Postoperative complications in 400 patients after transcervical-subxiphoid-VATS maximal thymectomy for MG and thymomas.
Results
Starting from September 01, 2000 to September 30, 2016 there
were 1,931 transcervical operations including 392 transcervicalsubxiphoid
VATS maximal thymectomies for myasthenia gravis
(MG), 8 thymectomies for thymoma, 1,224 TEMLA procedures
for staging of non-small cell lung cancer (NSCLC), 286 resections
of the mediastinal tumors and the mediastinal metastases (mostly
from thyroid cancer), 17 pulmonary lobectomies combined with
TEMLA for NSCLC (in 7 patients TEMLA was combined with 1 or
2 intercostal ports, in the other 10 patients a uniportal transcervical
technique was used) and 6 attempts of closure of the right main
bronchus post pneumonectomy fistula.
Postoperative complications for TEMLA, transcervicalsubxiphoid
VATS maximal thymectomy, transcervical lobectomy
and resection of the mediastinal tumors are presented in Tables 1-4.
For the whole group there were 14/1,931 (0.6%) patients required
revision because of postoperative bleeding (through the original
incision in all but one patient, who necessitated thoracotomy). There
were 6 postoperative deaths with 30-day postoperative mortality
0.3% (6/1931): 5 patients died after TEMLA (unrelated causes) and 1
patient died after transcervical-VATS left upper lobectomy because of
pulmonary embolism. Complications occurred in 144/1,931 patients
(morbidity 7.5%).
In the group of the mediastinal tumors there were 3/286 (1.0%)
patients who had to be converted because of technical difficulties,
in another 2 patients packing of the mediastinum was necessary for
major bleeding; the packing was successfully removed after 2 and
3 days. There were no other severe intraoperative complications or
deaths.
In Tables 1-5, the results and complications of TEMLA,
transcervical-subxiphoid-VATS thymectomy, and pulmonary
lobectomies performed solely through the cervical approach and
resection of the mediastinal tumors are presented.
Table 3
Table 4
Table 5
Discussion
The main advantage of the transcervical approach is much lesser
postoperative pain in comparison to thoracotomy, sternotomy
and even VATS. This observation was made by us on the clinical
ground; however, we did not any specific studies comparing
severity of pain for patients undergoing operations with use of the
approaches mentioned above. Most of the transcervical procedures
need no postoperative mediastinal drainage. Recovery of patients
after transcervical operations is very fast. The rate of postoperative
respiratory insufficiency with the need of a ventilator is very low.
To get a wide and safe access to the chest two principles must be
obeyed. The first one is that the major mediastinal vessels including
the innominate artery, the common carotid arteries and the left
innominate vein must be carefully dissected free before retraction.
Dissection makes these structures more movable and therefore
protects them from traction injury. In case of severe atherosclerotic
lesions of the arteries and the aorta the retraction must be very
delicate or, in a very occasional case another approach to the chest
must be chosen. The second principle is the elevation of the sternal
manubrium with the sternal retractor, which provides the wider
access to the mediastinum, together with upwards retraction of the
mediastinal structures. Performance of operations according to these
rules enables easy access to the mediastinum down to the bifurcation
of the trachea. Operations through the transcervical approach are
feasible even in excessively obese patients; however in such cases
performance of procedure is more difficult. With use of special
retractor (Aesculap-Chifa, Poland) it is possible to retract the tracheal
bifurcation and the right main bronchus and to dissect the esophagus
down, almost to the hiatus. Opening of the mediastinal pleura and
disconnecting of the ventilation of one lung enables access to the
pleural cavity and performance of the right or left upper pulmonary
lobectomy, under control of the thoracoscope inserted through the
VATS port, with the other VATS port used for introduction of the
endostapler, while the whole dissection is performed through the
cervical incision, which has a role of the utility thoracotomy. The
advantage of this approach is the use of the classic open surgical
technique with regular surgical instruments, without necessity of the
use of fine thoracoscopic instruments.
The 30-day mortality rate for patients undergoing TEMLA was
0.5% which was slightly higher in comparison with recent publications.
The mortality rates of the largest series of mediastinoscopies reported
by Hammoud et al. [11] and Lamaire et al. [12] were 0.2% and 0.05%,
respectively. The morbidity of TEMLA was higher in comparison to
the largest series of mediastinoscopies reported recently; however
the life-threatening vascular complications reported in these studies
were completely avoided in our patients [13,14]. Most of surgical
complications of TEMLA were mild and subsided without any
treatment; the most serious complications were purely medical.
TEMLA proved to be a diagnostic procedure with an extremely
high diagnostic yield. Our recent study showed that TEMLA had
98.6% sensitivity and 99.7% negative predictive value (NPV),
significantly higher than endobronchial ultrasound/endoesophageal
ultrasound (EBUS/EUS). Similar difference between TEMLA and
EBUS/EUS was noted in regard to the mediastinal restaging after
neoadjuvant therapy. Currently, TEMLA is used for staging and
restaging of all patients with NSCLC who are possible candidates for
surgery.
The incision in the neck enables access to the tumors of the
anterior, middle and posterior mediastinum, including small
thymomas, the other thymic tumors, ectopic goiter, parathyroid
adenomas, metastatic mediastinal nodes and neurinomas of the
apex of the chest. In case of thymomas, especially with associated
myasthenia gravis (MG) the transcervical incision is combined
with the subxiphoid and bilteral port VATS approach (one port to
each pleural cavity) to get maximal completeness of removal of the
mediastinal adipose tissue, that might contain the ectopic foci of the
thymic tissue.
There was no mortality in patients undergoing thymectomy
for MG or thymomas. The morbidity rate was 5.8%, with no severe
intraoperative complications. The postoperative myasthenic crisis
rate was 3.0% and the revision rate for bleeding was 1.3%. These
results are similar to the results reported by the other authors [13,14].
Our late institutional results of presented technique of
thymectomy has been very favourable – 5-years complete remission
rates 53.1% in comparison to 20.0% complete remissions rate after
the basic trassternal thymectomy (p<0.0001), which can be only
explained by the removal of ectopic foci of the thymic tissue from the
neck and the mediastinum in these patients [5]. Due to the incidence
of the ectopic foci of the thymic tissue in all areas of the mediastinum,
including both epiphrenic fat pads we are reluctant to perform
thymectomy solely through the neck because in this procedure a large
part of the adipose tissue of the lower mediastinm is not dissected,
which might affect the final results of complete remission rates of
MG. In our opinion the extensive dissection of the fatty tissue of the
mediastinum and the lower neck is not as necessary in thymomas
without MG, because in such cases complete removal of the whole
thymus containing the thymoma is the priority.
Conclusions
Transcervical extended approach with elevation of the sternal manubrium enables performance of various thoracic surgical procedures with minimal invasiveness, low mortality and morbidity and very high effectiveness.
Author Contributions
• Marcin Zieliński (conception and design, collection and
assembly of data, final analysis and interpretation, manuscript
writing, final approval of manuscript).
• Mariusz Rybak (collection and assembly of data, manuscript
writing, final approval of manuscript).
• Katarzyna Solarczyk-Bombik (collection and assembly of
data, manuscript writing, final approval of manuscript).
• Michal Wilkojc (collection and assembly of data, manuscript
writing, final approval of manuscript).
• Wojciech Czajkowski (collection and assembly of data,
manuscript writing, final approval of manuscript).
• Sylweriusz Kosinski (collection and assembly of data,
manuscript writing, final approval of manuscript).
• Edward Fryzlewicz (collection and assembly of data,
manuscript writing, final approval of manuscript).
• Tomasz Nabialek (collection and assembly of data, manuscript
writing, final approval of manuscript).
• Juliusz Pankowski (collection and assembly of data,
manuscript writing, final approval of manuscript).
References
- Cooper JD, Al-Jilaihawa AN, Pearson FG, Humphrey JG, Humphrey HE. An improved technique to facilitate transcervical thymectomy for myasthenia gravis. Ann Thorac Surg. 1988;45(3):242-7.
- Zieliński M, KuzdzaĹ J, Szlubowski A, Soja J. A safe and reliable technique for visualization of the laryngeal recurrent nerves in the neck. Am J Surg. 2005;189(2):200-2.
- Zielinski M, Kuzdzal J, Nabialek T, Hauer L, Pankowski J, Dziadzio B. Transcervical extended mediastinal lymphadenectomy. In: Multimedia Manual of Cardiothoracic Surgery. 2005.
- Zielinski M. Technical pitfalls of transcervical extended mediastinal lymphadenectomy – how to avoid them and to manage intraooperative complications. Semin Thoracic Surg. 2010;22:236-43.
- Zielinski M, Hauer L, Hauer J, Pankowski J, Nabialek T, Szlubowski A. Comparison of complete remission rates after 5 year follow-up of three different techniques of thymectomy for myasthenia gravis. Eur J Cardiothorac Surg. 2010;37(5):1137-43.
- Zielinski M, Rybak M, Wilkojc M, Fryzlewicz E, Nabialek T, Pankowski J. Subxiphoid video-assisted thorascopic thymectomy for thymoma. Ann Cardiothorac Surg. 2015;4(6):564-6.
- Komanapalli CB, Cohen JI, Sukumar MS. Extended transcervical videoassisted thymectomy. Thorac Surg Clin. 2010;20(2):235-43.
- Zieliński M, Pankowski J, Hauer Ł, Kuzdzał J, Nabiałek T. The right upper lobe pulmonary resection performed through the transcervical approach. Eur J Cardiothorac Surg. 2007;32(5):766-9.
- Zielinski M, Rybak M, Solarczyk-Bombik K, Wilkojc M, Czajkowski W, Kosinski S, et al. Uniportal transcervical video-assisted thoracoscopic surgery (VATS) approach for pulmonary lobectomy combined with transcervical extended mediastinal lobectomy (TEMLA). J Thorac Dis 2017;9(4):878-84.
- Jakubiak M, Pankowski J, Obrochta A, Lis M, Skrobot M, Szlubowski A, et al. Fast cytological evaluation of lymphatic nodes obtained during transcervical extended mediastinal lymphadenectomy. Eur J Cardiothorac Surg. 2013;43(2):297-301.
- Hammoud ZT, Anderson RC, Meyers BF, Guthrie TJ, Roper CL, Cooper JD, et al. The current role of mediastinoscopy in the evaluation of thoracic disease. J Thorac Cardiovasc Surg. 1999;118(5):894-9.
- Lemaire A, Nikolic I, Petersen T, Haney JC, Toloza EM, Harpole DH Jr, et al. Nine-year single center experience with cervical mediastinoscopy: complications and false negative rate. Ann Thorac Surg. 2006;82(4):1185- 9.
- Tomulescu V, Ion V, Kosa A, Sgarbura O, Popescu I. Thoracoscopic thymectomy mid-term results. Ann Thorac Surg. 2006;82(3):1003-7.
- Rückert JC, Ismail M, Swierzy M, Sobel H, Rogalla P, Meisel A, et al. Thoracoscopic thymectomy with the da Vinci robotic system for myasthenia gravis. Ann N Y Acad Sci. 2008;1132:329-35.