Case Report
Long-Term Survival with Surgery for Nodal Recurrence Following Complete Response to Therapy for De-Novo, Stage IV, Liver-Limited Colorectal Cancer
Ciara M Kelly and Nancy E Kemeny*
Department of Medicine, Memorial Sloan Kettering Cancer Center, USA
*Corresponding author: Nancy E Kemeny, Department of Medicine, Memorial Sloan Kettering Cancer Center, 300 East 66th Street, 10th Floor, New York, NY 10065, USA
Published: 10 Feb, 2017
Cite this article as: Kelly CM, Kemeny NE. Long-Term
Survival with Surgery for Nodal
Recurrence Following Complete
Response to Therapy for De-Novo,
Stage IV, Liver-Limited Colorectal
Cancer. Clin Surg. 2017; 2: 1303.
Abstract
The lung and liver represent common sites of oligometastatic, recurrent colorectal cancer (CRC). The incidence of solitary nodal recurrences from CRC is low. A large volume of evidence exists to guide the management of patients with isolated recurrence to the liver or lung from which survival data supports an aggressive surgical approach. However, there is a dearth of information pertaining to the therapeutic strategy and long-term outcomes of patients with isolated nodal recurrences, particularly in the setting of previous definitive treatment for stage IV disease. This case report describes two cases whereby an aggressive surgical approach for nodal recurrence is associated with long-term survival following initial complete response to therapy for stage IV CRC to liver.
Case Presentations
Case A
A 59-year old man with a history of blood per rectum underwent a colonoscopy that found
a near obstructing sigmoid tumor. Pathology confirmed invasive adenocarcinoma. A computed
tomography (CT) scan highlighted the known sigmoid tumor and revealed innumerable liver
lesions. He underwent an open sigmoid colectomy and wedge biopsy of a liver lesion. Pathology
confirmed stage IV (pT3N1a (1/26 positive lymph nodes) M1), invasive, moderately differentiated
adenocarcinoma of the colon and liver according to the American Joint Committee on Cancer
(AJCC) TNM staging system for CRC [1]. Molecular analyses confirmed a KRAS/BRAF wild type
tumor. His serum carcinoembryonic antigen (CEA) level was 32ng/mL at diagnosis and continued
to rise after surgery to 112ng/mL. He was deemed to have inoperable, bilobar hepatic metastases
(>20 lesions). He enrolled on a phase II clinical trial exploring the conversion rate to complete
resection in patients with unresectable CRC liver metastases treated with the combination of best
systemic chemotherapy and liver directed hepatic arterial infusion (HAI) therapy with floxuridine
(FUDR) and decadron [2]. A baseline positron emission tomography (PET) scan excluded occult
extra-hepatic disease. A HAI pump was inserted and he commenced treatment. He received 6
months of combination HAI and systemic chemotherapy (5-fluorouracil, leucovorin and oxaliplatin
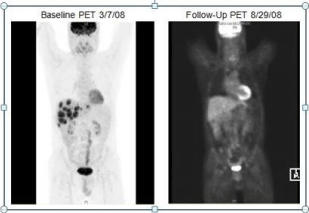
(FOLFOX)). An excellent response to treatment was observed on follow-up PET scan (Figure 1).
HAI therapy was subsequently held due to the development biliary dilatation. Oxaliplatin was
stopped because of peripheral neuropathy. In the setting of biliary dilatation, liver resection was not
performed. After a further three months of treatment PET imaging showed a complete response
within the liver. Treatment stopped and expectant management ensued. He remained off treatment
for 22 months when restaging CT and PET scan revealed a hypermetabolic, left external iliac lymph
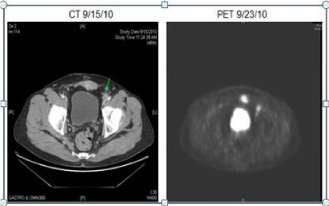
node and mass in the left lower anterior abdominal wall (Figure 2). His CEA level was elevated
(11ng/mL). He proceeded to abdominal wall resection and left pelvic lymphadenectomy. Pathology
confirmed metastatic CRC in both the abdominal wall and 1 of 4 left obturator external iliac nodes.
He received 6 months of adjuvant chemotherapy. He is now 8 years out from his original diagnosis,
of stage IV CRC, without evidence of disease.
Case B
A 61-year old man presented with weight loss and abdominal pain. A CT identified 4 right hepatic
lobe liver metastases and small lung nodules of uncertain significance. A colonoscopy revealed a
sigmoid tumor. Pathology confirmed an invasive adenocarcinoma. He commenced chemotherapy
with 5-FU, leucovorin and irinotecan (FOLFIRI) on 11/24/2003 and received 5 months of treatment.
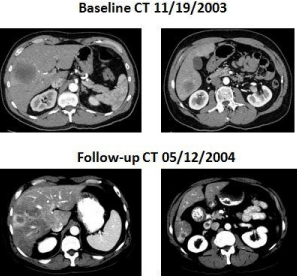
An excellent response was observed (Figure 3). The lung nodules remained stable. His CEA level fell from 184ng/mL to 4.3ng/mL. He underwent right portal venous
embolization (PVE). He proceeded to a synchronous low anterior
resection and right trisegmentectomy of the liver with placement of a
HAI pump on 05/17/2004. Pathology confirmed a stage IV (ypT3N1
(1/11 LNs) M1) moderately differentiated adenocarcinoma of colon
involving liver. He received HAI FUDR and FOLFOX chemotherapy
for 6 months in the adjuvant setting. Durable, long-term survival
has been reported in patients who underwent resection for CRC
liver metastases followed by adjuvant HAI FUDR and systemic
chemotherapy (5 and 10 year survivals of 78% and 61%, respectively)
[3]. Four months after stopping therapy he had radiological evidence
of recurrence within the peritoneum and a mesenteric lymph node
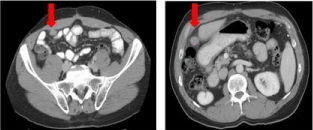
(Figure 4). His CEA was marginally elevated at 5.1ng/mL. Molecular
analysis of the primary tumor confirmed KRAS wild type disease
and he resumed chemotherapy with irinotecan and cetuximab. He
responded to 6 months of systemic therapy. On 12/15/2005, he
underwent resection of the two sites of intra-abdominal recurrent
disease. Pathology confirmed recurrent CRC. He completed 6 months
of adjuvant irinotecan and cetuximab. He continues on surveillance
and remains without evidence of disease 13 years from his original
presentation with stage IV CRC.
Figure 1
Figure 1
Case A. The baseline PET scan shows hyper-metabolic, hepatic
metastases. The follow-up PET scan, after 6 months of liver-directed and
systemic chemotherapy, reveals response to treatment with just one focus, in
segment 4A, of residual, hepatic, hypermetabolic activity, with a CT correlate,
suspicious for viable disease.
Figure 2
Figure 2
Case A. CT and PET scan performed 22 months after completing
first-line therapy with HAI and systemic chemotherapy revealed a 2cm,
hyper-metabolic, left external iliac lymph node (SUV 8.8) and a 2.3 x 2.5cm,
hyper-metabolic mass in the left lower rectus muscle (SUV 7.5).
Figure 3
Figure 3
Case B. CT 11/19/2003, revealed multiple liver metastases.
CT 05/12/2004, is status post chemotherapy and right PVE and shows a significant reduction in size of liver metastases.
Figure 4
Figure 4
Case B. CT 05/22/2005, reveals two abnormal intra-abdominal foci
(red arrows) concerning for recurrent disease.
Discussion
CRC is a significant health issue globally. In 2012, there were an estimated 1.4 million new cases diagnosed worldwide [4]. In
2016, an estimated 134,490 new cases and 49,190 deaths from CRC
will occur in the United States [5]. Despite advances in the multimodality
management of CRC, approximately 20-50% of patients
definitively treated for CRC develop recurrent disease. The majority
(>90%) of recurrences occur within 3-5 years of definitive surgery
for the primary tumor [6]. Evidence supports an aggressive surgical
approach to manage oligometastatic recurrence to liver or lung. The
incidence of solitary nodal recurrences from CRC is <10-20% [7,8]
and limited data exists to guide management particularly following
definitive therapy for stage IV CRC.
Oligometastatic disease is thought to represent an intermediate
state in the stepwise evolutionary cascade of metastatic capacity
whereby, spread may be limited to specific organs and metastases
are present in limited number [9,10]. The temporal differences in
the appearance and metastatic capacity of metastases are dependent
on tumor genetics [11,12]. Primary tumor cells may have genetically
predetermined limited capability in one or more of the necessary
biological requirements for metastasis that results in the development
of an oligometastatic state [9]. The clinical significance of this
hypothetical metastatic state is that local interventions including
surgery may represent effective therapeutic strategies. Numerous
studies have reported durable survival following surgery with and
without additional liver-directed and/or systemic chemotherapy for
the management of liver-limited metastatic CRC [2,13-15]. Similarly,
in the setting of oligometastatic lung disease of colorectal origin long-term survival may be achieved [16,17]. The rate of locoregional
recurrence following resection of colon cancer ranges between
4-34% [7]. Isolated nodal and abdominal wall recurrences from CRC
are rare. Surgery is a less widely accepted therapeutic approach for
oligometastatic CRC involving lymph nodes or the abdominal wall
than for small volume disease limited to the liver or lung. While
patients with locoregional recurrence have a poor prognosis, longterm
survival with surgical resection has been reported in a number
studies (5-year survival rates of 15-40%) [7,18]. The rarity of this clinical
scenario and the morbidity associated with surgery in this setting are
some of the reasons that explain the discrepancy in the management
of oligometastatic disease. The potential morbidity associated
with surgical resection of locoregional recurrence underscores the
importance of appropriate patient selection. A number of prognostic
factors have been identified in patients with recurrent CRC including:
location and volume of recurrence [7,19], margin status [19], site of
the primary lesion [20], nodal involvement of the primary tumor [7],
and complete R0 resection [8,18]. However, these prognostic factors
have not been consistently identified across studies. Nonetheless,
these prognostic factors reflect a logical inference that the biological
aggressiveness of both the primary and recurrent tumor has the
greatest impact on overall survival [7]. There is limited data to
guide management of nodal recurrence from CRC in the setting of
a previous definitive therapy for stage IV CRC. One study examining
the surgical management of 42 patients with loco-regional recurrent
CRC, including nodal recurrences, reported that 18 of these patients
underwent concurrent or previous resection of hepatic or pulmonary
metastases. No significant difference in outcome was observed
between these two groups. The median survival was 21 months
compared to 29 months in those without metastatic disease (p=0.315)
[7]. A few studies discuss the management of retroperitoneal nodal
recurrences from CRC. The literature suggests that isolated nodal
recurrences to the retroperitoneal area differ in terms of outcome
to non-nodal recurrences to this region. Isolated nodal recurrences
are distinguished from locoregional recurrences in the same areas by
the presence or absence of lymph node involvement in the pathology
specimen and the relationship of the lymph node to the original
primary tumor. One retrospective study, reviewed the survival data
from 31 patients following complete resection for retroperitoneal
recurrences from CRC (including 23 nodal recurrences (NR) and
8 locoregional recurrences (LR)). The median overall survival (OS)
was 18 months (range, 9-58) in the LR group, and 53 months (range,
4-258) in the NR group (p=0.033). The 3-year OS in the LR cohort was
27% versus 81% in the NR group [21]. In another study examining
patient outcomes following the multimodality management of an
intra-abdominal recurrence of CRC, nodal recurrence was associated
with a better prognosis with a 5-year OS rate of 44% compared to
28% for patients with locoregional recurrence [8]. A systematic
review examining the surgical management of retroperitoneal nodal
recurrences from CRC found in favor of an aggressive surgical
approach. No operative mortality associated with salvage resection
for retroperitoneal nodal recurrences was observed in the nine studies
reviewed. The morbidity rate ranged between 17-33% [22].
Conclusion
There is limited evidence to guide the management of nodal recurrences that develop following definitive therapy for stage IV CRC. This case report highlights that durable survival is possible when a surgical approach is undertaken in this clinical setting. Surgical resection should be considered for small volume nodal recurrences amenable to complete resection. Combining surgery with perioperative chemotherapy should also be considered. Long-term survival is a distinct possibility with this approach.
References
- Edge S, Byrd DR, Compton CC, Fritz AG, Greene FL, Trotti A. AJCC. AJCC Cancer Staging Handbook: Springer. 2010.
- DʼAngelica MI, Correa-Gallego C, Paty PB, Cercek A, Gewirtz AN, Chou JF, et al. Phase II trial of hepatic artery infusional and systemic chemotherapy for patients with unresectable hepatic metastases from colorectal cancer: conversion to resection and long-term outcomes. Ann Surg. 2015; 261: 353-360.
- Kemeny NE, Chou JF, Boucher TM, Fong YC, Cercek A, D'Angelica MI, et al. Updated long-term survival for patients with metastatic colorectal cancer treated with liver resection followed by hepatic arterial infusion and systemic chemotherapy. J Surg Oncol. 2016; 113: 477-484.
- GLOBOCAN 2012 v1.0, Cancer Incidence and Mortality Worldwide: IARC Cancer Base No. 11.
- Siegel RL, Miller KD, Jemal A. Cancer statistics, 2016. CA. A Cancer Journal for clinicians. 2016; 66: 7-30.
- Seo SI, Lim SB, Yoon YS, Kim TW, Kim JH, Kim JC, et al. Comparison of recurrence patterns between </=5 years and >5 years after curative operations in colorectal cancer patients. J Surg Oncol. 2013; 108: 9-13.
- Harji DP, Sagar PM, Boyle K, Griffiths B, McArthur DR, Evans M. Surgical resection of recurrent colonic cancer. Br J Surg. 2013; 100: 950-958.
- Taylor WE, Donohue JH, Gunderson LL, Larson DR, Rubin J, O'Connell MJ, et al. The Mayo Clinic experience with multimodality treatment of locally advanced or recurrent colon cancer. Ann Surg Oncol. 2002; 9: 177-185.
- Weichselbaum RR, Hellman S. Oligometastases revisited. Nat Rev Clin Oncol. 2011; 8: 378-382.
- Gupta GP, Massague J. Cancer metastasis: building a framework. Cell. 2006; 127: 679-695.
- Campbell PJ, Yachida S, Mudie LJ, Stephens PJ, Pleasance ED, Stebbings LA, et al. The patterns and dynamics of genomic instability in metastatic pancreatic cancer. Nature. 2010; 467: 1109-1113.
- Yachida S, Jones S, Bozic I, Antal T, Leary R, Fu B, et al. Distant metastasis occurs late during the genetic evolution of pancreatic cancer. Nature. 2010; 467: 1114-1147.
- Pawlik TM, Scoggins CR, Zorzi D, Mentha G, Capussotti L, Vauthey JN, et al. Effect of surgical margin status on survival and site of recurrence after hepatic resection for colorectal metastases. Ann Surg. 2005; 241: 715-722.
- Fong Y, Fortner J, Sun RL, Brennan MF, Blumgart LH. Clinical score for predicting recurrence after hepatic resection for metastatic colorectal cancer: analysis of 1001 consecutive cases. Ann Surg. 1999; 230: 309-318.
- Adam R, Delvart V, Pascal G, Ghémard O, Levi F, Bismuth H, et al. Rescue surgery for unresectable colorectal liver metastases downstaged by chemotherapy: a model to predict long-term survival. Ann Surg. 2004; 240: 644-657.
- Pfannschmidt J, Dienemann H, Hoffmann H. Surgical resection of pulmonary metastases from colorectal cancer: a systematic review of published series. Ann Thorac Surg. 2007; 84: 324-338.
- Onaitis MW, Petersen RP, Haney JC, Kemeny N, Rusch VW, Downey R, et al. Prognostic factors for recurrence after pulmonary resection of colorectal cancer metastases. Ann Thorac Surg. 2009; 87: 1684-1688.
- Bowne WB, Lee B, Wong WD, Guillem JG, Paty PB, Weiser MR, et al. Operative salvage for locoregional recurrent colon cancer after curative resection: an analysis of 100 cases. Dis Colon Rectum. 2005; 48: 897-909.
- Akiyoshi T, Fujimoto Y, Konishi T, Oya M, Miyata S, Yamaguchi T, et al. Prognostic factors for survival after salvage surgery for locoregional recurrence of colon cancer. Am J Surg. 2011; 201: 726-733.
- Elferink MA, Visser O, Wiggers T, Tollenaar RA, Langendijk JA, Siesling S, et al. Prognostic factors for locoregional recurrences in colon cancer. Ann Surg Oncol. 2012; 19: 2203-2211.
- Dumont F, Kothodinis K, Goere D, Ducreux M, Malka D, Elias D, et al. Central retroperitoneal recurrences from colorectal cancer: are lymph node and locoregional recurrences the same disease? Eur J Surg Oncol. 2012; 38: 611-616.
- Ho TW, Mack LA, Temple WJ. Operative salvage for retroperitoneal nodal recurrence in colorectal cancer: a systematic review. Ann Surg Oncol. 2011; 18: 697-703.