Case Report
Giant Deep Neck Lipoma: A Case Report and Review of the Literature
Ahmad Alshadwi1, Mohammed Nadershah2, Andrew Salama3 and Amr Bayoumi4*
1Department of Oral and Maxillofacial Surgery, King Faisal Specialist Hospital and Research Centre, KSA
2Department of Oral and Maxillofacial Surgery, King Abdulaziz University- Dental School, KSA
3Department of Oral and Maxillofacial Surgery, Boston University, USA
4Department of Oral and Maxillofacial Surgery, King Abdulaziz University, KSA
*Corresponding author: Amr Bayoumi, Department of Oral and Maxillofacial Surgery, King Abdulaziz University, Jeddah, KSA
Published: 10 Feb, 2017
Cite this article as: Alshadwi A, Nadershah M, Salama A,
Bayoumi A. Giant Deep Neck Lipoma:
A Case Report and Review of the
Literature. Clin Surg. 2017; 2: 1299.
Abstract
Lipomas may be located in all parts of the body and may be confused clinically with other soft tissue
masses. They infrequently occur in the head and neck. A large neck mass (greater than 10 cm) with
a rapid growth rate should raise concerns about a possible malignancy. Surgical excision of a lipoma
is often used as the definitive treatment modality and alternative treatments described for lipomas
such as liposuction have been described in the literature. In the present study a 39-year-old male
presented with an enlarging left neck mass measuring 11 cm × 8 cm that was successfully removed.
The surgery produced excellent cosmetic results and no functional impairment. An integrated
review of the literature regarding etiology, histopathology, diagnostic and treatment modalities of
lipomas is presented.
Keywords: Lipoma; Liposarcoma; Neck mass
Introduction
Lipomas are benign tumors of adipose tissues with an estimated incidence of 10% of all
mesenchymal neoplasms [1]. However, only 13% of lipomas occur in the head and neck area, most
of which arise in the posterior neck [2,3]. Rarely, they can develop in the anterior neck area, the
infratemporal fossa, or in the oral cavity, pharynx, larynx, and parotid gland. Their growth is usually
slow and limited. Most lipomas have a diameter of two centimeters and rarely grow beyond ten
centimeters [4]. Although lipomas elsewhere in the body are twice as common in females as in males,
lipomas in the head and neck region has a more balanced sex distribution [5]. Lipomas are commonly
classified based on anatomic location and histology. Benign lipomatous tumors are sub-classified
according to histologic features and growth pattern into classic lipomas, fibrolipoma, angiolipoma,
infiltrating lipoma, intramuscular lipoma, hibernoma, pleomorphic lipoma, lipoblastomatosis, and
diffuse lipoblastomatosis [6,7]. A “giant lipoma” has a size that is greater than 10 cm in at least one
dimension or weighs over 1000 grams [6]. Lipomas may be located in all parts of the body and may
be classified anatomically as superficial or deep [8]. In the head and neck region, lipomas deep to the
platysma or muscles of facial expression are considered deep [9].
The majorities of head and neck lipomas are superficial and occur in the posterior region of the
neck. On the other hand, deep lipomas in the anterior neck are rare. Only a few of such cases have
been reported in the literature [2,7,10-14]. We report a case of a giant deep lipoma of the anterior
neck.
Figure 1
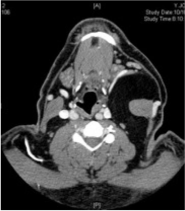
Figure 1
Axial section of the neck CT scan showing a large mass medial to the left sternocleidomastoid muscle.
Figure 2
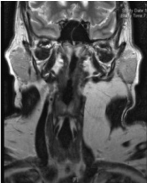
Figure 2
Coronal section of the neck MRI showing left neck lesion with a
signal consistent with fat.
Figure 3
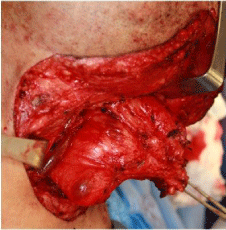
Figure 3
Intraoperative picture of the lipoma showing a close relation to the
internal jugular vein.
Figure 4
Figure 4
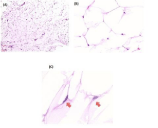
Histopathologic examination of the giant deep lipoma of the neck.
Hematoxylin and eosin stain. Original magnifications: (A) 40x, (B) 400x and (C) 600x.
Case Presentation
A 39-year-old Hispanic male was referred to the oral and maxillofacial surgery clinic at Boston Medical Center with a one-year history of progressive left sided neck swelling. The patient reported that the mass had increased in size over the preceding 2 months. He noted occasional left-side neck pain that radiated to the ipsilateral mandible. He denied both odynophagia and dysphagia. His past medical history was significant for asthma, type-two diabetes mellitus, hypertension, and obesity. He weighed 87 kilograms and his height was 167 cm. Clinical examination revealed an indiscrete soft, mobile mass in the left levels I, II, and III of the neck. There was no skin involvement, skin fixation nor lymphadenopathy. The trachea and thyroid were in the midline. Intra-orally, there was no evidence of tumor or mass. The diagnostic work up included a computed tomography scan (CT scan), a magnetic resonance imaging (MRI), and a fine needle aspiration cytology (FNAC). The CT scan (Figure 1) and MRI (Figure 2) showed a large mass media to the left sternocleidomastoid muscle extending from the level of the left mastoid tip to the level of the left clavicle. The lesion extended along the anterior and posterior aspects of the left sternocleidomastoid muscle with a distinct thin capsule and septa. It measured about 8 cm (anterior-posterior dimension) x 6.3 cm (transverse dimension) x 11 cm (cephalocaudal dimension). It was well circumscribed without evidence of invasion of adjacent structures. The mass was homogenous and had a signal consistent with fat on all sequences. It displaced the left common carotid artery and the left internal jugular vein medially without occlusion. The left submandibular gland was also anteriorly displaced. After imaging, a FNAC was attempted twice with inconclusive result. The patient underwent an incisional biopsy under general anesthesia that confirmed the diagnosis of lipoma. This giant lipoma was removed using a transcutaneous neck incision extending from the left mastoid tip toward the midline, about 4 cm above the sternal notch. The dissection was carried through the skin, subcutaneous fascia, Platysma muscle, and the superficial layer of the deep cervical fascia. A distinct capsule was identified around the lipoma, which facilitated surgical removal. The lesion was dissected bluntly from the internal jugular and common carotid artery without complications (Figure 3).
Histopathology
The surgical resection specimen consisted of grossly tan-yellow fibro-adipose tissue measuring 10.5 x 9.0 x 4.0 cm and weighing 136.2 grams. Sectioning did not show grossly abnormal areas of hemorrhage or necrosis. Microscopic examination revealed non-encapsulated mature adipose tissue (Figure 4(A); original magnification, 40×). Examination at higher magnification demonstrated typical hexagonal arrangement of mature adipocytes (Figure 4(B); original magnification, 400×) with eccentrically located small, inconspicuous oval nuclei with open chromatin configuration (Figure 4(C), red arrows; original magnification, 600×). No areas with cytologic atypia, immature adipocytes, lipoblasts, necrosis, or other atypical features were seen. These findings, together with the clinical presentation, are consistent with the diagnosis of a benign conventional lipoma. No features suggestive of a specific morphologic variant of lipoma were seen (e.g., angiolipoma or spindle cell lipoma). Focal areas of histologically unremarkable skeletal muscle and 14 benign lymph nodes were also identified in the specimen (not shown), but there was no infiltrative growth pattern or muscle fiber entrapment suggestive of an intramuscular lipoma.
Discussion
Despite the benign nature of lipomas, the distinction from welldifferentiated
liposarcomas can be challenging [11,15]. A rapidly
growing neck mass should raise suspicion of a malignancy [11].
Moreover, the mass size, location, consistency and attachment to
adjacent tissues are useful for differentiating a benign from malignant
mass. Liposarcomas are usually located in the retroperitoneum,
buttocks, lower extremity muscles, or mediastinum. They are
typically found in deeper soft tissues rather than in the subcutaneous
areas [16]. However, only 2-8% of liposarcomas occur in the head
and neck region [17,18]. Well-differentiated liposarcoma is low grade
in nature and can be divided into three subtypes, with the lipomalike
liposarcoma (the most common) mimicking the lipoma both
macroscopically and microscopically [18].
Diagnostic imaging, including computed tomography scan or
magnetic resonance imaging, is an essential step in the evaluation
of the neck mass. Simple lipomas are discrete, encapsulated, and
homogeneous [19]. Although, morphologically indistinguishable
from normal fat, lipomas’ lipids are not available for metabolism. It is
usually surrounded by a thin fibrous capsule. On MRI examination,
the more differentiated the liposarcoma, the more intense the fat
signal is. MRI findings suggestive of liposarcoma include thickened or
nodular septa (typically thicker than 2 mm), associated non-adipose
masses, and prominent foci of high T2 signal and prominent areas of
enhancement [20].
Nonetheless, CT and MRI cannot confidently differentiate
lipomas from liposarcomas. Thin capsule of the lipoma may be
perceived as an ill-defined border that blends with the surrounding
tissues thus mimicking liposarcoma [21]. Moreover, simple lipomas
may also contain muscle fibers, blood vessels, fibrous septa, and/
or areas of necrosis or inflammation. All these intralesional nonadipose
components can confound the correct imaging diagnosis
because they can mimic findings associated with well-differentiated
liposarcomas [20].
Histological examination is the only way for differentiating the
two entities. However, incisional biopsies are not reliable and many
times the final diagnosis is not reached until the lesion is completely
removed [17]. Lipomas are composed histologically of mature adipose
tissue arranged in lobules, many of which are surrounded by a delicate
fibrous capsule [22]. Liposarcomas are histologically described as
being similar to lipomas, but with scattered atypical fibroblasts or
sometimes signet ring cells present [5]. Other, soft tissue neoplasms
that may enter the differential diagnosis include lipoblastoma (of
infancy), intramuscular angioma, lipomatosis, myxoma, myxoid
liposarcoma, or pleomorphic liposarcoma, but these entities were
readily excluded morphologically in the presented case.
Surgical treatment options of lipomas include excision or
liposuction-assisted removal. Excision is more commonly used
because of its lower recurrence rate. Liposuction-assisted removal
may be advocated to avoid the resulting scar and potential damage
to adjacent structures during excision. Risks of liposuction include
skin irregularities like dimpling, parasthesia, pigmental change, and
high risks of recurrence [18]. Simple lipomas recur 5% locally [9].
Recurrence is related to incomplete excision or infiltrative type of
lipoma [7,10].
Madelung disease, also known as benign symmetric lipomatosis,
is a rare idiopathic disease, mainly reported in Mediterranean and
eastern European ethic groups. It mainly affects middle-aged males
(male-to-female ratio is 15:1) with history of alcoholism. Moreover,
about 80% of patients with HIV-1 infection treated with a protease
inhibitor developed this syndrome [23]. This disease is characterized
by multiple non-capsulated lipomas in different body areas resulting
in a significant cosmetic deformity. The typical description consists
of massive lipomatous deposits around the neck, which gives rise to
the classic description of lipoma anulare colli, “buffalo hump” and
“horse collar [24]. Surgery is the most effective treatment, especially
for those with aesthetic deformity and/or significant compression
of the aerodigestive tract. However, because these lesions are not
encapsulated, complete surgical excision is challenging and may lead
to local recurrence [25].
In summary, giant lipomas of the head and neck are uncommon.
The surgeon should be able to differentiate benign lipomas from
liposarcomas. Diagnostic aids include CT scan, MRI, FNAC, and
open biopsy. Surgical excision is the preferred treatment with low
recurrence rates.
References
- Sanchez MR, Golomb FM, Moy JA, Potozkin JR. Giant lipoma: case report and review of the literature. J Am Acad Dermatol. 1993; 28: 266-268.
- El-Monem MHA, Gaafar AH, Magdy EA. Lipomas of the head and neck: presentation variability and diagnostic work-up. J Laryngol Otol. 2006; 120: 47-55.
- Som PM, Scherl MP, Rao VM. Rare presentations of ordinary lipomas of the head and neck: a review. AJNR Am J Neuroradiol. 1986; 7: 657-664.
- Shmookler BM, Enzinger FM. Pleomorphic lipoma: a benign tumor simulating liposarcoma. A clinicopathologic analysis of 48 cases. Cancer. 1981; 47: 126-133.
- Lee CA, Damm DD, Neville BW, Allen C, Bouquot J. Oral and maxillofacial pathology. 2008.
- Lee J, Fernandes R. Neck masses: evaluation and diagnostic approach. Oral and Maxillofacial Surgery Clinics of North America. 2008; 20: 321-337.
- Pélissier A, Sawaf MH, Shabana AH. Infiltrating (intramuscular) benign lipoma of the head and neck. J Oral Maxillofac Surg. 1991; 49: 1231-1236.
- Vinay K, Abbas AL, Fauston N. Robbins and Cotran pathologic basis of disease. New York: Saunders. 2004.
- Marx RE, Stern D. Oral and maxillofacial pathology. Chicago: Quintessence. 2003.
- De Jong AL, Park A, Taylor G, Forte V. Lipomas of the head and neck in children. Int J Pediatr Otorhinolaryngol. 1998; 43: 53-60.
- Medina CR, Schneider S, Mitra A. Giant submental lipoma: Case report and review of the literature. Can J Plast Surg. Winter 2007; 15: 219-222.
- Moumoulidis I, Durvasula P, Jani P. Well-circumscribed intramuscular lipoma of the sternocleidomastoid muscle. Auris Nasus Larynx. 2004; 31: 283-285.
- Ramakantan R, Shah P. Anterior neck lipoma masquerading as an external laryngocoele. J Laryngol Otol. 1989; 103: 1087-1088.
- Wenig BM. Lipomas of the larynx and hypopharynx: a review of the literature with the addition of three new cases. J Laryngol Otol. 1995.
- Weiss SW. Lipomatous tumors. Monogr Pathol. 1996; 38: 207-239.
- Dei Tos AP. Liposarcoma: new entities and evolving concepts. Ann Diagn Pathol. 2000; 4: 252-266.
- Davis EC, Ballo MT, Luna MA, Patel SR, Roberts DB, Nong X, et al. Liposarcoma of the head and neck: The University of Texas M. D. Anderson Cancer Center experience. Head Neck. 2009; 31: 28-36.
- Nouri H, Hassani R, Aderdour L, Raji A. The well-differentiated liposarcoma of the hypopharynx. Eur Ann Otorhinolaryngol Head Neck Dis. 2011; 128: 143-145
- Cappabianca S, Colella G, Pezzullo MG, Russo A, Iaselli F, Brunese L, et al. Lipomatous lesions of the head and neck region: imaging findings in comparison with histological type. Radiol Med. 2008; 113: 758-770.
- Gaskin CM, Helms CA. Lipomas, lipoma variants, and well-differentiated liposarcomas (atypical lipomas): results of MRI evaluations of 126 consecutive fatty masses. AJR Am J Roentgenol. 2004; 182: 733-739.
- Chikui T, Yonetsu K, Yoshiura K, Miwa K, Kanda S, Ozeki S, et al. Imaging findings of lipomas in the orofacial region with CT, US, and MRI. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1995; 84: 88-95.
- Freedberg IM, Eisen AZ, Wolf K. Fitzpatrick's Dermatology in General Medicine. 5th edn. New York: McGraw-Hill, Health Professions Division. 1999; 1.
- Albu S. Madelung disease. Ear Nose Throat J. 2011; 90: 148-149.
- Ramos S, Pinheiro S, Diogo C, Cabral L, Cruzeiro C. Madelung disease: a ot-so-rare disorder. Ann Plast Surg. 2010; 64: 122-124.
- Alameda YA, Torres L, Perez-Mitchell C, Riera A. Madelung disease: a clinical diagnosis. Otolaryngol Head Neck Surg. 2009; 141: 418-419.