Review Article
Components Separation Technique Associated to a “Sandwich” Procedure in the Treatment of Large and Complex Incisional Hernias and Abdominal Wall Defects. A 30-Case Series
Martín Cartes JA*, Tamayo-López MJ and Bustos Jiménez M
Department of Surgery, Hospital Universitario Virgen del Rocio, Spain
*Corresponding author: Juan A. Martín-Cartes, Department of Surgery, Hospital Universitario Virgen del Rocio, Baños 76, 41002 Seville, Spain
Published: 08 Feb, 2017
Cite this article as: Martín Cartes JA, Tamayo-López
MJ, Bustos Jiménez M. Components
Separation Technique Associated to a
“Sandwich” Procedure in the Treatment
of Large and Complex Incisional
Hernias and Abdominal Wall Defects.
A 30-Case Series. Clin Surg. 2017; 2:
1292.
Abstract
Aim: Reconstruction of large, complex abdominal wall hernias is an interesting challenge. Primary closure of those hernias is often not possible. There is little agreement about the most appropriate
technique or prosthetic to repair these defects, in spite the fact of the prevalence of ventral hernias.
Sometimes despite being contaminated surgical fields, we are often faced to reinforce with bioprosthetic
meshes.
The components separation technique (CST) is a practical option; however, recurrence rates
remain unacceptably high. In an attempt to reduce recurrences, we frequently added a biologic
underlay mesh and a lightweight polypropylene only mesh to the traditional components separation
technique.
Our objective was to determine biologic mesh practice patterns of reconstructive surgeons with
regard to indications, most appropriate technique, election of prosthetics, and experience with
complications in order to work those large and complex hernias out.
Methods: 30 consecutive patients who underwent abdominal wall reconstruction by means of
components separations associated with non cross-linked porcine dermal scaffolds (NCPDS) or
synthetic tissue scaffolds (STS) reinforcement between October 2009 and December 2011 were
retrospectively reviewed. Analysis of demographics, indications for NCPDS or STS placement,
surgical technique, complications, and follow-up data was performed.
They underwent a “sandwich” procedure with a biologic underlay mesh and a lightweight
polypropylene only mesh added to the traditional components separation technique, we chose
NCPDS or STC underlay mesh according to the fact of the presence or absence of a contaminated
field.
Results: A “sandwich” procedure was used for abdominal wall repair in 30 patients. In all of them,
NCPDS or STC was positioned using an intraperitoneal technique associated to a lightweight
polypropylene only mesh and the components separation technique. At a mean follow-up time of
30.1 months, most patients had successful outcomes.
Complications included seroma, recurrence, and infection. One of our patients died from multiorgan
failure unrelated to hernia repair.
Conclusion: This study shows that complex abdominal wall defects can be successfully reconstructed
using a “sandwich” procedure with a low rate of recurrence and complications. Moreover, repair
of large, complex abdominal wall hernias by CST augmented with a biologic underlay mesh and
a lightweight polypropylene only mesh results in lower recurrence rates compared to historical
reports of CST alone.
Keywords: Contaminated hernia repair; Sublay mesh; Biologic mesh; Biologic scaffolds; Noncross- linked porcine dermis; Components separation technique; “Sandwich” procedure
Introduction
Abdominal wall defects caused by trauma, tumor resection, and
incisional hernias are a commonly encountered and challenging
problem for surgeons. Incisional hernias occur in 1% to 11% of
patients after midline laparotomy, and their repair is the most
common major surgical procedure performed by general surgeons
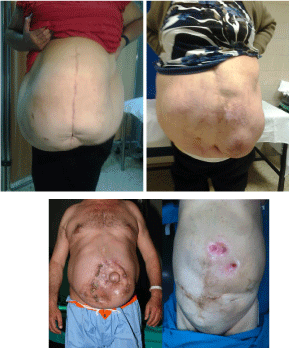
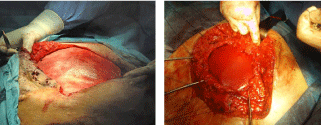
[1]. Operative repair of abdominal wall defects can be complicated by
their size and the presence of contamination (Figure 1).
Despite the high prevalence of this problem, there is little
agreement as to the most appropriate technique or prosthetic to
repair these defects. Reconstruction of large, complex abdominal
wall hernias is an interesting challenge for the practicing surgeon.
Furthermore, operative repair of abdominal wall defects can be
complicated by their size and the presence of contamination.
Unlikely any single technique or mesh will adequately address
all patients with incisional hernias because of the broad spectrum
of diseases associated with ventral hernias makes it. Additionally,
the absence of a clear classification system to standardize all reports
makes comparative analysis of publications limited. Several groups
have attempted to classify incisional hernias based on different factors
and or standards [1,2].
Some years ago, in 2010, were made recommendations as to the
most appropriate prosthetic selection (synthetic versus biologic) based
on the presence of underlying patient comorbidities and perioperative
wound contamination (Figure 2). However, this was only based on
expert opinion and was not validated with outcomes data. This group
recommended synthetic mesh for otherwise healthy individuals and
biologic grafts for those patients with active contamination during
abdominal wall reconstruction. There was little consensus as to the
ideal prosthetic for high-risk patients (diabetics, obese, COPD, and
smokers) without the presence of contamination.
Unfortunately, primary closure of such hernias is often not
possible due to the extensive size of the fascial defect encountered,
bigger than conventional meshes, and even when possible, the repair
often fails due to excessive tension at the suture line. These obstacles
often leave patients with few options as they are commonly refused
surgical treatment.
This subset of patients represents a large percentage of incisional
hernia patients, as these comorbidities are inherent risk factors to the
formation of hernias [3]. The introduction of biologic mesh to the
repertoire of the reconstructive surgeon has enabled one-stage repairs
of contaminated and infected abdominal wall hernias [4].
The actual utilization of these materials in non-contaminated
abdominal wall hernia repair remains unknown. The lack of clear
guidelines as to the most appropriate usage of these expensive
products has resulted in inconsistent practice patterns among
reconstructive surgeons. We hypothesized that practice patterns of
reconstructive surgeons with regard to indications, most appropriate
technique, choice of prosthetic, and experience with complications
vary significantly. We have though up we could combine the CST with
the use of prosthetic biomaterials (NCPDS or STS) would allow for a
dynamic abdominal wall closure in most of cases as well as keeping the
hernia recurrence acceptably low. A biologic underlay has been used
to allow for the incorporation of the product into the patient’s own
collagen to create a neofascia and avoid the complications observed
with the permanent prosthetic meshes. Closure of the midline, if
possible, adds to the repair while the only mesh reinforces the entire
abdominal wall that has been rebuilt.
Figure 1
Figure 2
Figure 2
Contaminated surgical fields, including contaminated meshes in
association with enterocutaneous fistulas, we had to deal with.
Figure 3
Material and Methods
From October 2009 until December 2013, 30 consecutive complex
abdominal wall defects were repaired by CST using a biologic mesh
underlay (Gore BioA Tissue Reinforcement®; Gore, Flagstaff, AZ
or Permacol® Covidien, 15 Hampshire Street, Mansfield, MA) in
conjunction with a lightweight polypropylene (Optilene® Mesh
Elastic, B. Braun, Melsungen, AG, Carl-Braun-Straße 1 Melsungen,
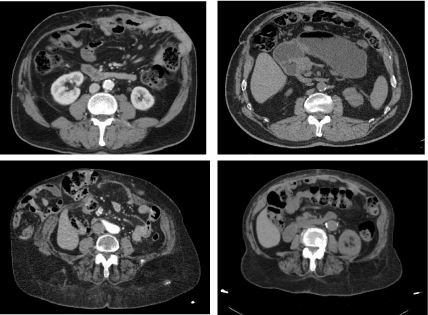
Germany) only mesh [5]. Briefly, all patients underwent preoperative
imaging including computed tomography of the abdomen and pelvis
with no oral contrast (Figure 3). 27 cases in our series suffered from
complex incisional hernias; the three others from desmoid tumors.
The construction of porcine dermal collagen is very similar to
that of human tissue and because Permacol® in sheet form is not
a reconstructed form of collagen, its 3-D matrix is maintained. A
precisely controlled degree of cross-linking is introduced into the
structure, making it resistant to collagenase enzymes responsible
for the breakdown and reabsorption of implanted collagen [5].
This unique feature enables surgeons to complete operations and
procedures involving tissue reconstruction, re-contouring and repair,
with permanent results.
As the finished biomaterial is rendered acellular, it contains no
material capable of provoking an immunogenic reaction which is a
very important feature in a product designed for implantation into
human tissue. Permacol® surgical implant is able to support host cell
infiltration and revascularisation and within a few months becomes
an integral part of the body (Figure 4).
Permacol differs from cheaper synthetic meshes in that it can be
used in instances where they cannot be used for example against the
bowel. Should infection occur it can be treated while Permacol is
in place and need not be removed as would other implants or mesh.
Permacol® permanent surgical implant is presented in the form
of a flat, off white sheet of acellular porcine collagen. Tough but
flexible its constituent elastin fibres are presented moist in sterile
saline. Sizes we employed were Gore® Bio-A® Tissue Reinforcement
is a uniquely designed web of biocompatible synthetic polymers that
is gradually absorbed by the body, while its 3D matrix of open highly
interconnected pores facilitates tissue generation and healing. As
a synthetic tissue scaffold, it is not derived from human or animal
tissue but engineered for uniformity, consistency and versatility.
Clinical evidence demonstrates that the scaffold is replaced with type
I collagen.
Optilene® Mesh Elastic is a light-weight large pore monofilament
polypropylene mesh. Due to the exact elasticity of the abdominal wall
it is able to adapt to all movements taking place. The new honeycomb
like structure, with one of the largest pores available on the market,
permits an ideal healing and the formation of an elastic scar. Optilene®
Mesh Elastic is ideal for incisional hernia repair. Optilene® Mesh
Elastic helps to maintain an excellent abdominal wall physiology
resulting in a greater convenience and comfort for the patient.
We chose Permacol® to be used in contaminated fields and Bio-
A if we had to deal with a clean one.
Nasogastric tubes were not routinely employed, only if necessary.
Urinary catheters were inserted to drain the bladder, monitor
urine output and, if warranted, to measure bladder pressures. The
placement and length of the skin incision was determined by prior
incisions. So they were specific for each hernia in order to allow an
adequate exposure of the fascial defect.
Our patients had undergone from 1 to 11 surgical procedures in
order to get their incisional hernias repaired, with an average of 4, 5.
After having made the skin incision, the abdominal cavity was
explored, adhesiolysis was performed and the size of the fascial defect
was measured. Done that, we started the components separation
procedure by elevation of skin and subcutaneous fat off the rectus
fascia and external oblique muscle and fascia. Division of the external
oblique aponeurosis was performed one cm lateral to the lateral
border of the rectus sheath along the defect to be repaired.
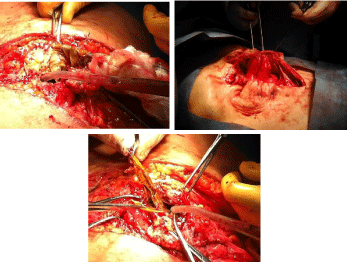
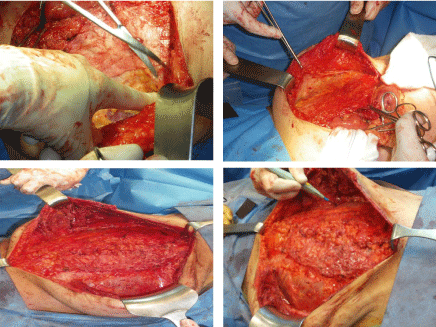
The underlay reinforcement (Permacol® or Bio-A®) sheet were
fixed, after having been cut out, using a transparietal technique
(Figure 5). Due to the complexity and large extent of their abdominal
wall defects, and according to the presence or absence of bacterial
contamination, combination of intraperitoneal Permacol® (14
patients) insertion and ‘‘components separation’’ technique (Figure
6) while Bio-A® was used in 16 cases (53, 33).
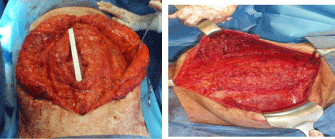
Full closure of the defect was achieved in 11 (36, 66%) of these cases
(Figure 7). In the other 19 cases (63, 33%) combining intraperitoneal
mesh with separation of components, medial approximation of the
recti muscles was not possible due to the large extent of the initial
defect. Permacol® and Bio-A® were sutured under moderate tension
in order to distribute the stress of closure evenly between this
fixation, and final recti muscle fascial closure when possible. Sizes of
Permacol® mesh used in this series varied widely between patients;
the most usual were 30 x 20 and 40 x 20 cm, and Bio-A® prostheses
were 20 x 30 and 20 x 20cm. However, both, Permacol®> and Bio-A®
used meshes were always larger than the resulting defect after having
performed a CST, so that we could provide a minimum of 3-5 cm
overlap with the posterior fascia (Figure 8).
In case the midline fascia could not be re-approximated, we
usually closed the redundant hernia sac over the biologic mesh to
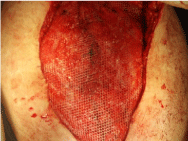
provide vascularized tissue coverage for mesh in growth. The next
step, a large-pore, lightweight polypropylene mesh (Optilene® Mesh
Elastic) was fixed to the abdominal fascia in an only position. The
most frequent size we used was 30 x 30 cm.
The skin and subcutaneous tissue were then closed over two
closed suction drains. At the time of skin closure, generous resection
of excessive skin and subcutaneous tissue was performed, leaving
only the amount necessary for closure.
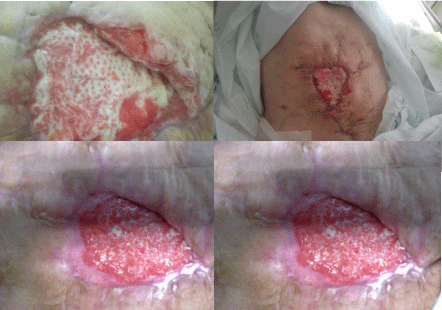
Figure 4
Figure 4
Those pictures show how host cells infiltrate NCPDS and so, within
a few months, it becomes an integral part of the body.
Figure 5
Figure 6
Figure 7
Figure 8
Figure 8
An achieved “sandwich” procedure with a full closure of the abdominal wall; a biologic underlay mesh and a lightweight polypropylene only mesh are added to the traditional components separation technique.
Results
Most of patients in our series had successful outcomes at a
mean follow-up time of 30.1 months (range, 13–42 months). One
patient developed an abdominal compartment syndrome following
hernia repair and was returned to the operating room some days
later following his hernia repair for decompression. This patient had
significant comorbidities (ASA score of 4), had undergone multiple
laparotomies and suffered from a severe chronic respiratory disease.
Despite having been thoroughly informed and cautioned regarding
his high risk of serious postoperative complications due to significant
associated medical comorbidities, he requested to proceed due to the
severity of his obstructive symptoms associated with the hernia.
The polypropylene mesh was removed, and the intraperitoneal
Permacol® mesh was liberated from its fixations on the patient’s right
side and left in place to relieve the intraabdominal pressure. The defect
was then patched with Dual Mesh Plus (W.L. Gore & Associates,
Flagstaff, AZ) to allow for normal intra-abdominal pressure. The
patient was subsequently returned to the operating room multiple
times. Unfortunately, in the end, he passed away.
Thirty patients (17 males and 13 females) underwent a meshreinforced
CST from October 2009 until December 2011, the average
follow-up of 236±2.3 months. The average age of the study population
was 59.9±1.8 years, with an average BMI of 37, 96 (23, 12–53) kg/
m2 and ASA score of 2.92±0.17. Thirty-nine percent were smokers,
32% were diabetic, and 87% had at least one previous abdominal wall
hernia repair.
Operative time for the described CST averaged 176.5, the average
blood loss 258 ml and hernia defect size of 21 x 17 cm. Patients were
discharged from the hospital on average 9 days following a meshreinforced
CST.
Surgical site occurrences were identified in 10 patients (33%) most
commonly from skin necrosis. Five of these patients were treated with
negative pressure dressings for local wound care, and the two other
surgical sites improved with antibiotics alone. Seven patients (14%)
required re-operation and partial polypropylene mesh excision. This
excision involved only the portion of mesh that was grossly infected
and unincorporated into surrounding tissues. Two other patients
were treated outside our hospital with a Streptokinase cream; it
resulted in a local destruction of the Permacol® sheet following new
recurrences, so using those creams was strictly forbidden in case of
patients after having been placed a biologic mesh.
Wounds were then treated with a negative pressure dressing until
resolution of the infection. None of the patients who experienced a
surgical site occurrence were found to have a fascial defect during
wound exploration, unless those above mentioned patients, other
patient suffered from a recurrence, having been re-operated
satisfactorily.
Moreover, no bowel complications or leaks were encountered as a
consequence of having placed the intraperitoneal biologic mesh.
Seroma formation was the most common postoperative
complication, affecting eight of the 30 patients (26, 66%). Average
time from surgery to seroma formation was 29 days.
Twelve patients (40%) underwent NCPDS placement to repair a
giant ventral hernia complicated with enterocutaneous fistulas. They
were taken down at the time of mesh implantation.
The 3 patients with post-ostomal hernias experienced
postoperative courses without complications according to the fact we
reinforced the whole area by means of a big underlay prostheses.
We have not found association between surgical technique
(underlay mesh, the only one, etc) and type of complication.
Discussion
Incisional hernias usually recur because the tensile strength of the
healed fascial scar is lower than that of normal fascia.
Repair of these complex hernias has been managed with the
insertion of mesh either via an open or laparoscopic technique. The
incidence of incisional hernia after abdominal surgery ranges from 9
to 20%, which may also result in large, complex hernias with loss of
domain [6]. However, patients with massive hernias that are larger
than 12 cm in transverse dimension are difficult to approach either
laparoscopically or via an open laparotomy [7].
Our findings suggest that Permacol® or Bio-A® sheets are effective
in the reconstruction of complex abdominal wall defects, resulting in
satisfactory outcomes at an average follow-up time of 30.1 months
and yielding a low rate of surgical complications. Despite the short
follow-up time, recurrence rates lower than those reported with mesh
repair have been achieved [8].
Furthermore, there was no incidence of small bowel obstruction
in this patient population. The most commonly encountered
complication was seroma, a benign problem. Our rate of 40% seroma
formation is higher than other series we found on medical [9]
Reinforcement of tense midline repair with intraperitoneal
prostheses has significantly reduced the incidence of this type of
hernias in our experience. It is likely that our low recurrence rates are
due to the combination of both material and surgical technique. An
added benefit of using an intraperitoneal biologic mesh is its ability
to resist infection [10,11]. The abdominal cavity can be left open for
extended periods of time during the extensive lysis of adhesions that
are often required during a CST, thus increasing the risk of wound
infection. The surgical undermining that also occurs to release the
external oblique adds to the risk of wound infection as well. For these
reasons, wound occurrences are frequent and would therefore place a
permanent prosthetic mesh at high risk of infection and subsequent
need for removal. Removing the permanent underlay mesh would
require an extended operation likely requiring the removal of the
only mesh as well, resulting in hernia recurrence. The placement
of an intraperitoneal biologic mesh obviates the need for future
removal, in nearly all cases, and allows for successful treatment of a
large majority of wound infections with negative pressure dressings
alone, as was the case in our series. In patients with clean wounds,
the rate of recurrence is also lower than that of our entire sample
population (6, 66 vs. 12, 5%). Although long-term outcomes for
primary hernia repair with biologic materials are under investigation,
there is strong data supporting its use in infected and contaminated
fields [12,13]. For this reason, we initially restricted the use of biologic
meshes to patients presenting with difficult, contaminated wounds.
However, the evidence-based recommendations of the Ventral
Hernia Working Group highlight the growing role of biologic mesh
in the reconstruction of a wide variety of abdominal wall defects [14].
As a result of the low incidence of complications observed, we then
proceeded to use Bio-A mesh in non-contaminated yet complex
abdominal defects, where there was often insufficient omentum,
thus precluding use of prosthetic mesh. It is well known that the cost
of biologic materials such as NCPDS is higher than synthetic mesh
products [15].
We feel that prosthetic mesh plays a significant role in hernia
repair and should be used whenever deemed safe. However, when
compared to the foreign body implantation mechanism of synthetic
mesh, implanted Permacol or Bio-A did not result in complications
like bowel perforation in our series, and may be better suited than
mesh whenever an intraperitoneal repair is necessary.
Byrnes explained that a faithful cost-effective analysis of biologic
mesh repair is very complex due to the afore-mentioned price
variability between institutions [16]. Nonetheless, we believe that this
clear reduction in recurrence rates and postoperative complications
justifies the use of the more expensive in non-contaminated complex
ventral hernias whenever intraperitoneal repair is indicated. The
individual rates of seroma (25%), recurrence (10%), and infection
(3, 3%) in patients with clean wounds are similar to the rates of
these same complications in our entire patient sample. Statistical
analysis (Fisher test) determined that no association exists between
wound class and type of complication. The trend of complications is
however indicating that a larger series may confirm a higher rate of
complications in clean cases [17].
In this study, we have reported our increased experience using
Permacol® or Bio-A® mesh to rebuild abdominal wall defects in a
large patient population over longer follow-up times. We have been
able to reproduce the desirable outcomes and minimal complications
reported in our initial study. Our work continues to be limited by
its single-institution, retrospective nature and its lack of controls.
Furthermore, we are a tertiary care hospital dealing with large defects
that represent abdominal wall reconstruction rather than routine
hernia repairs that are performed by our general surgery colleagues.
A prospective, multi-center, randomized trial on abdominal wall
reconstruction using Permacol® or Bio-A® should be carried out to
compare various products and their efficiency. Despite having been
good outcomes, according to the latest articles [17] published on
medical literature, we changed our minds about the best way of those
patients suffering from enterocutaneous fistulas or infected meshes.
So we gave up placing them a second (only) large-pore, lightweight
polypropylene mesh (Optilene® Mesh Elastic) in association with
an underlay reinforcement (Permacol®) in order to place the lesser
amount of foreign bodies on those contaminated fields. In addition
it is an evidence of our full confidence in its abilities, such as strength
and resistance so that they can reinforce or substitute abdominal wall
efficiently. Those new strategies will be the matter of our next work
about complex incisional hernias, we hope. To sum up, despite the
fact that these materials might be useful in certain conditions, the
evidence from latest studies is low. Moreover, although the use of
synthetic meshes has really decreased the recurrence rate after the
treatment of hernias of the abdominal wall, we know that their use
in a contaminated surgical field or in certain locations can lead to
specific complications such as mesh infection or erosion. To get over
these problems, a completely new generation of so-called remodeling
biological scaffolds from human or animal origin or even new synthetic
constructs have been promoted in recent years. This study shows that
complex abdominal wall defects can be successfully reconstructed
using a “sandwich” procedure with a low rate of recurrence and
complications. Moreover, repair of large, complex abdominal wall
hernias by CST augmented with a biologic underlay mesh and a
lightweight polypropylene only mesh results in lower recurrence
rates compared to historical reports of CST alone. Although our
analysis shows that there was no association between indication for
reconstruction and type of complications, a larger patient population
studied in a multi-center trial may identify statistically significant
association between indications and complications.
References
- Burger J, Luijendijk R, Hop W, Halm JA, Emiel GGV, Jeekel J. Long-term follow-up of a randomized controlled trial of suture versus mesh repair of incisional hernia. Ann Surg. 2004; 240: 578-585.
- Millikan K. Incisional hernia repair. Surg Clin N Amer. 2003; 83: 1223- 1234.
- Matthews B, Kercher K. Bioprosthetic materials in hernia epair. Problems Gen Surg. 2002; 19: 7-13.
- Alaedeen DI, Lipman J, Medalie D, Rosen MJ. The single staged approach to the surgical management of abdominal wall hernias in contaminated fields. Hernia. 2007; 11: 41-45.
- http://www.covidien.com/hernia/biologics/permacol
- Nasajpour H, LeBlanc KA, Steele MH. Complex hernia repair using component separation technique paired with intraperitoneal acellular porcine dermis and synthetic mesh overlay. Ann Plast Surg. 2011; 66: 280- 284.
- Kim H, Bruen K, Vargo D. Acellular dermal matrix in the management of high-risk abdominal wall defects. Am J Surg. 2006; 192: 705-709.
- Zheng F, Lin Y, Verbeken E, Claerhout F, Fastrez M, De Ridder D, et al. Host response after reconstruction of abdominal wall defects with porcine dermal collagen in a rat model. Am J Obstet Gynecol. 2004; 191: 1961- 1970.
- Pomahac B, Aflaki P. Use of a non-cross-linked porcine dermal scaffold in abdominal wall reconstruction. Am J Surg. 2010; 199: 22-27.
- Saettele TM, Bachman SL, Costello CR, Grant SA, Cleveland DS, Loy TS, et al. Use of porcine dermal collagen as a prosthetic mesh in a contaminated field for ventral hernia repair: a case report. Hernia. 2007; 11: 279-285.
- Franklin ME Jr, Gonzalez JJ Jr, Glass JL. Use of porcine small intestinal submucosa as a prosthetic device for laparoscopic repair of hernias in contaminated fields: 2-year follow-up. Hernia. 2004; 8: 186-189.
- Schuster R, Singh J, Safadi BY, Wren SM. The use of acellular dermal matrix for contaminated abdominal wall defects: wound status predicts success. Am J Surg. 2006; 192: 594-597.
- Diaz JJ Jr, Guy J, Berkes MB, Guillamondegui O, Miller RS. Acellular dermal allograft for ventral hernia repair in the compromised surgical field. Am Surg. 2006; 72: 1181-1187.
- Breuing K, Butler CE, Ferzoco S, Franz M, Hultman CS, Kilbridge JF, et al. Incisional ventral hernias: review of the literature and recommendations regarding the grading and technique of repair. Surgery. 2010; 148: 544-558.
- Shankaran V, Weber DJ, Reed RL, Luchette FA. A review of available prosthetics for ventral hernia repair. Ann Surg. 2011; 253: 16-26.
- Byrnes MC, Irwin E, Carlson D, Campeau A, Gipson JC, Beal A, et al, Repair of high-risk incisional hernias and traumatic abdominal wall defects with porcine mesh. Am Surg. 2011; 77: 144-150.
- Turnage RH, Badgwell B. Abdominal wall, umbilicus, peritoneum, mesenteries, omentum, and retroperitoneum. Chapter 45 in Townsend: Sabiston Textbook of Surgery. The Biological Basis of Modern Surgical Practice. 1088-1113, 19th edition. 2012 Elsevier Saunders, Philadelphia, PA. ISBN: 978-1-4557-1146-1148.