Review Article
Ulcerative Colitis and the Surgeon
Nisar Ahmad Chowdri*
Department of Colorectal Surgery, Sheri Kashmir Institute of Medical Sciences, India
*Corresponding author: Nisar Ahmad Chowdri, Department of Colorectal Surgery, Sheri Kashmir Institute of Medical Sciences, Jammu and Kashmir, 190011, PO Box: 27, India
Published: 30 Dec, 2016
Cite this article as: Chowdri NA. Ulcerative Colitis and the
Surgeon. Clin Surg. 2016; 1: 1280.
Abstract
Patients of ulcerative colitis are mostly managed by physicians. Surgeons play a very pivotal role in curative treatment and in dealing with complications of ulcerative colitis. Various technical advances made in the field have reduced surgical morbidity and mortality in these patients with improvement in the quality of life. The article discusses the role of surgery and various surgical options available for ulcerative colitis.
Introduction
Ulcerative colitis (UC) is common in developed countries with an incidence of 10-15 per 100,000
populations and a prevalence of 40-100 per 100,000 populations [1]. Though exact figures are not
available from this part of the world, a good number of patients do suffer from ulcerative colitis.
Although treatment of ulcerative colitis primarily remains medical (though not curative), the
surgeon continues to have a major role in saving patients life and in eliminating cancer and its long
term risk (3.5% which increases to 12% after 20 years of disease) 1 and abolish large intestinal disease.
Previously surgery was often delayed because of fear of ileostomy and its social and psychological
consequences. With the various technical advances in surgery, understanding timing and proper
patient selection, surgeons have been able to preserve sphincters and fecal continence in most of
the patients. There have been improvements in stomal care reflecting in improved quality of life, so
more and more patients are benefited by surgery.
Surgical Treatment
The rationale of surgical treatment in ulcerative colitis is to remove diseased bowel completely,
maintain voluntary transanal defecation with reasonable fecal continence, avoidance of permanent
ileostomy with minimal complications. Therefore, patients show overall improvement in health.
Elective indications
Failure of medical treatment: About 87-92% of patients with mild to moderate disease respond
to medical treatment. Some patients with partial response continue to live with mild to moderate
symptoms but patients with complete failure should be advised surgery. In patients with severe
disease response rates are low and they need large doses of medications which may be unacceptable
because of intolerable side effects, such patients opt for surgery. Patients with poor nutritional status
and failure to grow despite medical treatment do better with surgery.
Recurrent intestinal obstruction: Intestinal obstruction is almost always due to malignancy.
Even if investigations including biopsy favour benign stricture, still proctocolectomy is
recommended.
Chronic bleeding: Chronic blood loss necessitating frequent admissions for transfusion is also
an indication for elective surgery.
Cancer: Patients with disease for more than 10 years, involvement of entire colon and onset
in childhood are at risk of developing cancer and should be offered prophylactic proctocolectomy.
Alternatively they should be kept under close and vigorous surveillance which may be difficult
especially in mild to moderate disease. Colonoscopy should be advised every second year after 9th
year of disease with sigmoidoscopy in intervening year upto 15 years after which colonoscopy should
be done yearly. Dysplasia does not always precede carcinoma and carcinoma may be already present
when dysplasia is first detected. Patients with colonic mucosal dysplasia have more than 50% chance
of developing invasive cancer and proctocolectomy should be recommended to them [2].
Extraintestinal manifestations: Approximately 30% patients of ulcerative colitis have at least
one extraintestinal manifestation [3]. Cutaneous, joint and vascular manifestations usually regress
and do not recur after resection of entire colon and rectal mucosa.
Other manifestations like ankylosing spondylitis and rheumatoid
arthritis have separate disease pattern and genetic predisposition
in common with ulcerative colitis and usually do not respond to
surgical treatment. Patients with primary biliary cholangitis may
progress to cirrhosis and cholangiocarcinoma after surgery. Many
of the extracolonic manifestations improve as the severity of disease
decreases with medical treatment, but if these continue to cause
considerable symptoms, surgery should be considered.
Emergency indications
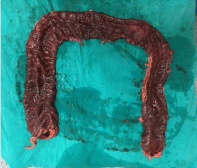
Fulminant colitis: Nearly 10% of ulcerative colitis patients present
with fulminant colitis (Figure 1). These patients present with severe
abdominal pain, fever, tachycardia, severe diarrhea, dehydration,
weight loss and increased leucocyte count. Sometimes fulminant
colitis may be the initial presentation of the disease. Though ulcerative
colitis is primarily a mucosal or submucosal disease, inflammation
in fulminant colitis has gone through all the layers of colon. These
patients are treated aggressively with medication but failure to
improve within 72 hours and continued deterioration warrants
prompt surgical intervention. With aggressive medical treatment and
early surgical intervention mortality is reduced to less than 3% [4].
Toxic megacolon: It may be initial presentation of the disease
and develops in 6% of hospitalized patients of ulcerative colitis. These
patients have colonic diameter of more than 6 cm in addition to signs
and symptoms of fulminant colitis. So patients with severe colitis
should have serial daily radiographs of the abdomen. Hypokalemia,
anticholinergics and barium sulphate enema are the precipitating
factors. Dysentery, typhoid and amoebic colitis should be considered
in differential diagnosis of toxic megacolon. Surgery is indicated
if there is no improvement in 24 hours with medical treatment,
deteriorating general condition and progressive increase in colonic
diameter. Early operative intervention is better. Mortality of toxic
megacolon without perforation is 4% and it increases to 20-40% in
patients with perforation [5].
Perforation: It is usually rare for colonic perforation to occur in
absence of toxic megacolon. In such cases, crohn’s disease should be
ruled out. High doses of steroids may mask symptoms. Early surgical
intervention reduces mortality in these patients.
Acute massive bleed: Less than 4% of patients of ulcerative colitis
present with massive bleed but it accounts for 10% of emergency
colectomies performed in such patients [2]. It is often associated
with toxic megacolon. Excessive need for transfusion is an indication
for emergency near total proctocolectomy with ileal pouch anal
anastamosis in young patients; however, restorative procedure may
not be possible in elderly patients.
Indeterminate and crohn’s colitis
Sometimes pelvic pouches are made with incorrect diagnosis in
a patient with crohn’s colitis. However failure rates and fistula rates
are higher (19% vs. 8% and 31% vs. 9% respectively) in indeterminate
colitis vs. patients with ulcerative colitis [6]. Such patients should be
offered restorative surgery only if they desire so and cannot live with
permanent ileostomy, provided they understand risks and are aware
of removal of pouch with loss of two feet of small gut, if needed.
Preoperative preparation
The patient should be well prepared to reduce the complications
with improved surgical results.
Patient counseling and education: All patients should be
educated and explained the various surgical options available, risks
and benefits of different procedures, the need for stoma and follow
up.
Nutrition: These patients usually have low nutritional status.
Fluid and electrolyte imbalance, anemia, coagulation deficiencies and
hypoproteinemia should be corrected first. Sometimes patient may
need parenteral nutrition.
Medical measures: Patient receiving or who have recently (within
1 year) received steroids should have additional stress dose therapy of
100 mg of hydrocortisone 8 hrly in the perioperative period to ensure
adequate hormonal support during surgery. Preferably patient should
be off steroids for two months or on a very low dose (10 mg per day)
before extensive restorative surgery. Similarly aspirin compounds
are withdrawn a week before elective surgery. Immunosuppressants
should also be withdrawn for as long as possible before surgery.
Prevention of thromboembolic: Prophylaxis for thromboembolic
in the form of elastic stocking and pneumatic compression should be
provided. However, heparinization is withheld.
Bowel preparation: Conventional bowel preparation in the form
of clear liquids a day before surgery, whole gut irrigation a night
before surgery, neomycin (1 gm) and metronidazole (500 mg) orally
a day before procedure at 5 pm and 11 pm are advice.
Surgical options
The surgical procedures currently in use for ulcerative colitis are
Total proctocolectomy with ileal pouch anal anastamosis (TPC
with IPAA): Restorative proctocolectomy with pouch formation has
become the procedure of choice for many patients of ulcerative colitis
[7]. The operation is attractive because it avoids permanent ileostomy,
cures the patient of disease while preserving the anorectal function.
The indications for TPC with IPAA are:
a. Ulcerative Colitis: Most cases of ulcerative colitis (surgery
indicated) who are well motivated, are less than 50 years of age, have
good sphincter function, without any significant comorbidity or low
rectal or perianal pathology are candidates for this procedure.
b. This procedure is also indicated for Familial adenomatous
polyposis, some cases of colorectal tumours and Hirschprung’s
disease. Crohn’s disease is a contraindication.
In this procedure total proctocolectomy is done with mucosectomy
of upper anal canal and distal rectum with anastamosis of ileal pouch
with dentate anal. In an alternative technique TPC with IPAA is
performed by using staplers without mucosectomy. The advantages
of this technique are precision, no tension on anastamosis with
preservation of good blood supply to the stump. However, retained
anorectal mucosa has a risk of colitis, dysplasia and malignancy and
these patients should be kept under surveillance, though malignancy
has been reported even after mucosectomy probably because of
regeneration of mucosa. Temporary fecal diversion is done in most
of the centers to allow anastamosis to heal well and reduce septic
complications; however, diversion can be avoided in selected patients.
The complications of ileal pouch anal anastamosis procedure
include small bowel obstruction (13%), pelvic sepsis (3-6%),
anastamotic leaks (10-14%), wound sepsis (3%), urinary dysfunction
(5%), stoma related (5-25%), fecal incontinence (usually nocturnal in
20-30%), pouchitis (18% at 1 yr and 40% at 10 yrs), stricture, fistula
(9%), sexual dysfunction (11-12%), cancer, pouch failure (75% at 1 yr
and 9% at 10yrs). The mortality following TPC with IPAA is less than
2% with morbidity ranging from 13-58%. However, inspite of high
morbidity majority of patients (80-90%) are satisfied and the overall
consensus at present is that the pouch anal procedure offers the best
quality of life when compared with alternatives [8-13].
Proctocolectomy with ileal pouch distal rectal anastamosis:
The rationale of this procedure is that it is easy to perform and
preserves transitional mucosa (anal sensation, sphincter function
and continence). However, the concern with this procedure is that
the diseased mucosa that is left behind can undergo dysplasia and
malignant change.
Proctocolectomy with end ileostomy (Brooke): This procedure
is indicated in elderly patients, those with incontinent sphincter,
synchronous low rectal cancer, significant comorbidity and prohibitive
concern about outcome of pelvic or Kock’s pouch. Toxic colitis, toxic
megacolon and significant comorbidity are contraindications for this
procedure. In these patients subtotal colectomy with end ileostomy
should be done. The advantages of this procedure are that it is one
stage operation, least complex and with good social support 90%
of these patients adapt to limitations of ileostomy. The drawbacks
include complete fecal incontinence, problems related to stoma, ever
present threat of leakage of stools and gas, psychological factors,
appliance cost, urinary and sexual dysfunction and perineal wound
[14].
Proctocolectomy with continent ileostomy (Kock’s Pouch):
The rationale of this procedure is making an internal reservoir for
storage of faces which can be voluntarily emptied by a catheter (30
Fr with big holes) with internal valve for continence. Incisions for
making pouch are made on antimesentric border which reduces
contractions and keeps the pressure low in the pouch. This type of
operation is indicated in all those patients who are candidates for
conventional Brooke ileostomy but want to improve quality of life,
preserve fecal continence, avoid external appliance and for those with
non availability of bathroom facilities and failed ileoanal anastamosis.
The contraindications include old patients (more prone to valve
dysfunction), crohn’s (risk of recurrence in small bowel), obese
patients (more chance of nipple valve failure), critically ill patients,
toxic megacolon (staged procedure better), psychologically unfit
(unable to intubate and cannot tolerate reoperation if required) and
those with multiple abdominal operations (due to adhesions).
The procedure avoids external bag (95%) and offers improved
quality of life. It is effective with no peristomal odour, social, sexual
or psychological problems. However, it is complex with risk of
pouchitis, valve complications (5-25%) and needs expert surgeon to
fashion pouch [15,16].
Colectomy with ileorectal anastamosis: This type of operation is
indicated in patients who are not suitable for IPAA or Kock’s pouch,
young patients who want to avoid any type of ileostomy and its
disability and risks related to rectal excision, if crohn’s disease cannot
be excluded and if ulcerative colitis is associated with metastatic
malignancy of colon. However, this procedure is avoided in patients
with severe rectal disease, dysplastic changes in rectum, emergency
situation (anastomotic breakdown- it is better to close distal rectal
stump or make a mucous fistula if stump is friable with proximal
ileostomy).
The procedure maintains anal route of defecation and is safe with
minimum complications. But, it leaves the disease in the stump with
6% cumulative risk of cancer after 20 years (15% at 30 yrs) and needs
continuous endoscopic surveillance. The procedure is performed
as a single stage electively but should be performed as a two stage
procedure in emergency conditions [17].
This type of operation has a limited role at present and only 55%
have satisfactory functional results. Approximately 36% of these
patients require proctectomy within few years. However, this is the
safest procedure for seriously ill patients (severe colitis, leucocytosis,
toxic megacolon, massive hemorrhage, severe anemia and
hypoalbuminemia). Proctectomy should be avoided in these patients.
It reduces blood loss and avoids transfusion. Patient can be weaned
off steroids slowly (over a period of 4-6 wks), anemia and nutritional
status improves. Patient also gains experience to live with ileostomy
for comparison with pelvic pouch. The pouch can be constructed later
and rectum dissected under best possible conditions.
Figure 1
Conclusion
With the advances made in surgical technique, anesthesia, antibacterial therapy the morbidity and mortality in expert hands has significantly reduced in patients with ulcerative colitis. Therefore, surgery should be offered to all suitable patients in whom it is indicated.
References
- Corman ML. Ulcerative colitis in Colon and Rectal surgery. 3rd Edn. JB Lippincott company, Philadelphia. 1993; 901-1011.
- Kelly KA, Dozois RR. Chronic ulcerative colitis. In: Mayo Clinic Gastrointestinal Surgery. Kelly KA, Sarr MG, Hinder RA, editors. Philadelphia, WB Saunders Company. 2004; 533-552.
- Goudet P, Dozois RR, Kelly KA, Ilstrup DM, Phillips SF. Characteristics and evolution of extraintestinal manifestations associated with ulcerative colitis after proctocolectomy. Dig Surg. 2001; 18: 51-55.
- Dozois RR, Kelly KA. The surgical management of ulcerative colitis. In: Inflammatory Bowel Disease. 5th Edn. Kirsner JB, editor. Philadelphia, WB Saunders Company. 2000; 626-657.
- Banner JJ. Total abdominal colectomy with mucosal proctectomy and ileal J (or S) reservoir. In: Colorectal Surgery Illustrated. Ist edn. Mos by –year book, Inc. 1993; 209-222.
- Wexner SD, Rothenberger DA, Jensen L, Goldberg SM, Balcos EG, Belliveau P, et al. Ileal pouch vaginal fistulas: incidence, etiology and management. Dis Colon Rectum. 1989; 32: 460-465.
- Parks AG, Nicholls RJ, Bellveau P. Proctocolectomy with Ileal reservoir and anal anastomosis. Br J Surg. 1980; 67: 533-538.
- Pemberton JH, Kelly KA, Beart RW Jr, Dozois RR, Wolff BG, Ilstrup DM. Ileal pouch – anal anastomosis for chronic ulcerative colitis: Long term results. Ann Surg. 1987; 206: 504-513.
- Chapman JR, Larson DW, Wolff BG, Dozois EJ, Cima RR, Larson DR, et al. Ileal pouch – anal anastomosis: does age at the time of surgery affect outcome. Arch Surg. 2005; 140: 534-539.
- Farouk R, Dozois RR, Pemberton JH, Larson D. Incidence and subsequent impact of pelvic abscess after ileal pouch anal anastomosis for chronic ulcerative colitis. Dis Colon Rectum. 1998; 41: 1239-1243.
- Metcalf AM, Dozois RR, Beart RW Jr, Kelly KA, Wollf BG. Temporary ileostomy for ileal pouch – anal anastomosis: Function and complications. Dis Colon Rectum. 1986; 29: 300-303.
- Feinberg SM, McLeod RS, Cohen Z. Complications of loop ileostomy. Am J Surg. 1987; 153: 102-107.
- Metcalf AM, Dozois RR, Kelly KA. Sexual function in women after proctocolectomy. Ann Surg. 1986; 204: 624-627.
- Pemberton JH, Phillips SF, Ready RR, Zinsmeister AR, Beahrs OH. Quality of life after Brooke ileostomy and ileal pouch-anal anastomosis: comparision of performance status. Ann Surg. 1989; 209: 620-626.
- Dozois RR, Dozois EJ. Continent ileostomy. In: Mastery of Surgery. 4th edn. Baker RJ, Fischer JE, editor. Philadelphia, Lippincott Williams & Wilkins. 2001; 1425-1434.
- Kohler LW, Pemberton JH, Zinsmeister AR, Kelly KA. Quality of life after prostocolectomy: comparison of Brooke ileostomy, Kock pouch, and ileal pouch-anal anastomosis. Gastroenterology. 1991; 101: 679-684.
- Kelly KA. Anal sphincter-saving operations for chronic ulcerative colitis. Am J Surg. 1992; 163: 5-11.