Case Report
An Axillary-Popliteal Artery Bypass Using PROPATEN® for Critical Limb Ischemia Due to an Extremely Long Chronic Total Occlusion: A Case Report
Soichiro Fukushima1*, Naoki Toya1, Kota Shukuzawa1, Tadashi Akiba2, Yuji Kanaoka3 and Takao Ohki3
1Department of Vascular Surgery, Jikei University Kashiwa Hospital, Japan
2Department of Surgery, Jikei University Kashiwa Hospital, Japan
3Department of Vascular Surgery, Jikei University School of Medicine, Japan
*Corresponding author: Soichiro Fukushima, Department of Vascular Surgery, Jikei University Kashiwa Hospital, 163-1, Kashiwashita, Kashiwa-Si, Chiba 277-8567, Japan
Published: 22 Dec, 2016
Cite this article as: Fukushima S, Toya N, Shukuzawa
K, Akiba T, Kanaoka Y, Ohki T. An
Axillary-Popliteal Artery Bypass Using
PROPATEN® for Critical Limb Ischemia
Due to an Extremely Long Chronic Total
Occlusion: A Case Report. Clin Surg.
2016; 1: 1253.
Abstract
Background: Extra-anatomic bypass is a less invasive treatment option of surgical revascularization for high risk critical limb ischemia (CLI), but it is thought to be difficult to keep the patency for
longer term. We experienced a CLI case due to an extremely long chronic total occlusion extending
from the infrarenal abdominal aorta to the superficial femoral artery, and succeeded limb salvage by
an axillary-popliteal artery bypass using a PROPATEN®, heparin bonded ePTFE graft, with double
antiplatelet therapy. A long extra-anatomic bypass has low patency rate for longer term, but we can
maintain the patency over 20 months without any target lesion revascularization. We report a rare
case with some literatures.
Case Presentation: An 83 years-old man complained of rest leg pain, and he was diagnosed as
CLI due to a long chronic total occlusion extending from the infrarenal abdominal aorta to the
superficial femoral artery. Because he had received several times of surgeries for cancers, and also
he had poor vein graft conditions, we selected an extra-anatomic bypass using a PROPATEN®. We
succeeded limb salvage, and are able to keep the patency without any target lesion revascularization
over 20 months.
Conclusion: An extremely long axillary-popliteal bypass using a PROPATEN® is not a gold standard
treatment for CLI, but it may be one of an alternative option only for high risk patient.
Keywords: CLI; Surgical revascularization; Aortic occlusive disease; Axillary-popliteal artery bypass; PROPATEN®
Introduction
The standard treatment for critical limb ischemia (CLI) is surgical revascularization (SR) using autologous vein grafts. However, it can be difficult to actually perform standard SR with autologous veins for CLI patients, because they have often already undergone coronary revascularization using autologous veins, or they often have poor vein graft conditions. We experienced a CLI case due to an extremely long chronic total occlusion (CTO) extending from the infrarenal abdominal aorta to the superficial femoral artery, with poor vein graft condition. An anatomical revascularization by laparotomy, or the surgical revascularization using autologous vein graft could not be applicable because of the patient’s conditions, we treated by an axillary-popliteal artery bypass using a PROPATEN® (W.L.Gore & Associates, Inc. Arizona, USA) heparin-bonded ePTFE graft. Although it seems to be difficult to keep the patency in such extremely long extra-anatomical bypass, the PROPATEN® maintain the patency over 20 months after procedure without any target lesion revascularization (TLR) with double antiplatelet therapy. It may be one of an alternative option only for high risk CLI patient to use the PROPATEN® for long extra anatomical bypass instead of the standard SR. We report the case with discussion of the relevant literature.
Case Presentation
In November 2014, an 83-year-old man consulted to our department with coldness, pallor, and
rest pain of the left leg. He had a past medical histories of the bladder cancer (total cystectomy and iliac
conduit diversion), rectal cancer (low anterior resection), and lung cancer (right upper lobectomy),
and also he had a smoking history of 20 cigarettes/day × 60 years. His
ankle brachial pressure index (ABI) was 0.47 in the right, and 0.35
in the left. Hematology and biochemistry tests revealed no abnormal
data. Contrast-enhanced computed tomography scans (CT) revealed
chronic total occlusion (CTO) of the infrarenal abdominal aorta,
bilateral common and external iliac arteries, common and superficial
femoral arteries with severe calcifications. Because radiological
examination showed a decrease in enhancement of the deep femoral
artery via collateral flow into the left leg, we decided to perform
angiography and prompt revascularization.
Pre-operative angiograph via the left brachial artery showed a
long CTO as previous enhanced CT scans. In the left limb, the deep
femoral artery was occluded at its origin, and the above-knee popliteal
artery was visualized via the collateral blood flow in the delayed
phase, and distal run-off was relatively maintained (Figures 1A-1C).
This patient was elderly, and his backgrounds strongly demanded
that the less invasive treatment should be selected. Therefore, we did
not attempt anatomical revascularization by laparotomy, but instead
performed non-anatomical revascularization using the left axillary
artery and the left above-knee popliteal artery as the inflow and
outflow vessels, respectively. Because the condition of the saphenous
vein was poor in both legs, we decided to use a ringed PROPATEN®
graft for revascularization.
The axillary artery and the above knee popliteal artery were
exposed as usual manner, and the bypass surgery was done using a
single 8 mm × 80 cm PROPATEN® graft. The graft was passed through
a subcutaneous tunnel from below the pectoral major muscle to the
inguinal ligament, while it ran under the femoral fascia below the
inguinal ligament. After anastomosis, angiography showed the blood
flow through the bypass was satisfactory and blood flow in the leg
had improved (Figure 2). His postoperative course was uneventful.
Coldness and rest pain in the left leg resolved. The ABI of the
treated leg improved to 0.61, and the patient was ambulatory when
discharged from hospital at 8 days postoperatively. Postoperative
CT clearly visualized distal blood flow in the left foot via the bypass
(Figure 3), and the revascularized graft is still patent more than 20
months after surgery.
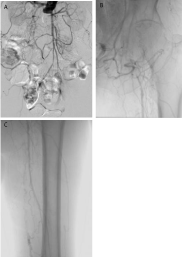
Figure 1
Figure 1
A. Angiography showing chronic total occlusion from the infrarenal abdominal aorta.
B. Angiography displaying total occlusion and severe calcification of the femoral artery.
C. Angiography revealing distal flow in the above-knee popliteal artery from collaterals.
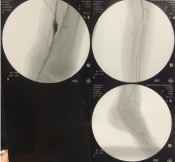
Figure 2
Figure 2
Intraoperative angiography displaying distal anastomosis of the left popliteal artery and PROPATEN
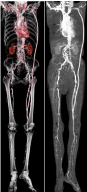
Figure 3
Figure 3
Postoperative CT angiography showing the patent bypass with distal blood flow below the ankle more than 18 months after the procedure.
Discussion
In the treatment of PAD, the indications for endovascular therapy
(EVT) have continued to increase over time. SR used to be the
treatment of first choice for TASC C-D lesions of the femoropopliteal
region, but in July 2012, based on the results of a Japan-U.S.
collaborative international study, a paclitaxel-eluting superficial
femoral artery stent (Zilver PTX®) [1-2] was approved in Japan in
compliance with the Pharmaceutical Affairs Law. And various devices
for treating leg lesions, such as Viabahn® heparin-bonded covered
stent for long/diffuse lesions of the superficial femoral artery [3,4],
drug-eluting balloons, [5,6] have also been developed. According to
these new devices, better results have been obtained by EVT and this
therapy is now indicated for a wider range of conditions.
However, SR is still the gold standard for revascularization in
CLI patients with PAD. The BASIL trial [7]d a similar
cost-benefit ratio were suggested by the early results at 12 months
postoperatively, but these results were subsequently reversed to some
extent after longer follow up until 36 months [8]. It was found that
the frequency of early failure was higher after EVT and that SR was
superior to EVT with respect to primary graft patency and avoiding
leg amputation. In the SR group, the results of revascularization were
even better when autologous veins were used and the amputation-free
rate was 60% or more from 36 months postoperatively, emphasizing
again that performing SR with autologous veins is a useful first-line
approach to the treatment of CLI.
On the other hand, it has been reported in recent years that
favorable therapeutic results can be obtained by leg revascularization
using a heparin-bonded ePTFE graft (PROPATEN®) [9]. Dorigo
et al [10]. Performed a multicenter prospective study comparing
the outcome of bypass surgery (femoral artery to the below-knee
popliteal artery) for CLI associated with diabetes between patients
treated with PROPATEN® grafts and those treated with autologous
vein grafts. They found that there was no significant difference of
the leg amputation-free rate between the PROPATEN® group and
the autologous vein group (59.9% vs. 64.4%). The results of their
study suggested that the PROPATEN® graft is also a useful option for
revascularization second to autologous veins in patients requiring
bypass surgery to the leg.
The PROPATEN® is an ePTFE graft that is manufactured
using porcine low-molecular-weight heparin. Because heparin
immobilized to the graft is not readily eluted, it produces no systemic
anticoagulant effect, but its antithrombotic activity has been reported
to be maintained topically even after surgery. It has been proven in
vitro that the beneficial effect of heparin lasts for at least 12 weeks
[11,12]. Because there is a risk of thrombotic occlusion in the acute
to sub-acute phase after revascularization and because most of the
target lesions for CLI are not single or short but diffuse or long, the
PROPATEN®, a vascular graft which itself has an antithrombotic
effect, may be superior to conventional ePTFE with respect to patency.
In the present patient, we had planned to perform poplitealfemoral
artery bypass surgery and combined with femoral
endarterectomy and then perform a separate bypass procedure
(sequential bypass surgery) from the femoral artery to the above-knee
popliteal artery. However, the patient was elderly, had undergone
surgery for several cancers, and also had coronary stenosis and COPD.
Considering these points, we decided to perform more rapid and less
invasive surgical revascularization by using a single 8 mm × 80 cm
PROPATEN® graft. After revascularization, angiography revealed a
definite improvement of blood flow to the popliteal artery and leg
arteries below the distal anastomosis, and rest pain and coldness of
the left foot resolved from early after surgery.
Conclusion
CLI patients requiring revascularization of the leg often have preoperative coronary artery disease, and their condition of vein graft is often unfavorable. The postoperative course in this patient suggests that the revascularization by an extra-anatomical bypass using the PROPATEN® graft with double antiplatelet therapy can be a useful alternative to SR for CLI patients, in whom it is difficult to perform revascularization with autologous veins. However, it is necessary to conduct further studies of long-term postoperative graft patency in CLI patients to confirm the findings obtained in the present case.
Acknowledgement
The author would like to thank Dr. Takao Ohki and Dr. Tadashi Akiba and Dr. Yuji Kanaoka for helpful discussions.
References
- Ohki T, Yokoi H, Kichikawa K, Kimura T, Snyder SA, Ragheb AO, et al. Two-year analysis of the Japanese cohort from the Zilver PTX randomized controlled trial supports the validity of multinational clinical trials. J Endovasc Ther. 2014; 21: 644-653.
- Dake MD, Ansel GM, Jaff MR, Ohki T, Saxon RR, Smouse HB, et al. Paclitaxel-eluting stents show superiority to balloon angioplasty and bare metal stents in femoropopliteal disease: twelve-month Zilver PTX randomized study results. Circ Cardiovasc Interv. 2011; 4: 495-504.
- Lammer J, Zeller T, Hausegger KA, Schaefer PJ, Gschwendtner M, Mueller-Huelsbeck S, et al. Heparin-bonded covered stents versus bare-metal stents for complex femoropopliteal artery lesions: the randomized VIASTAR trial (Viabahn endoprosthesis with PROPATEN bioactive surface [VIA] versus bare nitinol stent in the treatment of long lesions in superficial femoral artery occlusive disease). J Am Coll Cardiol. 2013; 62: 1320-1327.
- Zeller T, Peeters P, Bosiers M, Lammer J, Brechtel K, Scheinert D, et al. Heparin-bonded stent-graft for the treatment of TASC II C and D femoropopliteal lesions: the Viabahn-25 cm trial. J Endovasc Ther. 2014; 21: 765-774.
- Liistro F, Porto I, Angioli P, Grotti S, Ricci L, Ducci K, et al. Drugeluting balloon in peripheral intervention for below the knee angioplasty evaluation (DEBATE-BTK): a randomized trial in diabetic patients with critical limb ischemia. Circulation. 2013; 128: 615-621.
- Zeller T, Baumgartner I, Scheinert D, Brodmann M, Bosiers M, Micari A, et al. Drug-eluting balloon versus standard balloon angioplasty for infrapopliteal arterial revascularization in critical limb ischemia: 12-month results from the IN.PACT DEEP randomized trial. J Am Coll Cardiol. 2014; 64: 1568-1576.
- Adam DJ, Beard JD, Cleveland T, Bell J, Bradbury AW, Forbes JF, et al. Bypass versus angioplasty in severe ischaemia of the leg (BASIL): multicentre, randomised controlled trial. Lancet. 2005; 366: 1925-1934.
- Bradbury AW, Adam DJ, Bell J, Forbes JF, Fowkes FG, Gillespie I, et al. Bypass versus Angioplasty in Severe Ischaemia of the Leg (BASIL) trial: Analysis of amputation free and overall survival by treatment received. J Vasc Surg. 2010; 51: 18-31.
- Lindholt JS, Gottschalksen B, Johannesen N, Dueholm D, Ravn H, Christensen ED, et al. The Scandinavian Propaten(®) trial - 1-year patency of PTFE vascular prostheses with heparin-bonded luminal surfaces compared to ordinary pure PTFE vascular prostheses - a randomised clinical controlled multi-centre trial. Eur J Vasc Endovasc Surg. 2011; 41: 668-673.
- Dorigo W, Pulli R, Castelli P, Dorrucci V, Ferilli F, De Blasis G, et al. A multicenter comparison between autologous saphenous vein and heparinbonded expanded polytetrafluoroethylene (ePTFE) graft in the treatment of critical limb ischemia in diabetics. J Vasc Surg. 2011; 54: 1332-1338.
- Begovac PC, Thomson RC, Fisher JL, Hughson A, Gällhagen A. Improvements in GORE-TEX® Vascular Graft performance by Carmeda® bioactive surface heparin immobilization. Eur J Vasc Endovasc Surg 2003; 25: 432-437.
- Heyligers JM, Verhagen HJ, Rotmans JI, Weeterings C, de Groot PG, Moll FL, et al. Heparin immobilization reduces thrombogenicity of small-caliber expanded polytetrafluoroethylene grafts. J Vasc Surg. 2006; 43: 587-591.