Case Report
Simultaneous Cochlear Implantation with Translabyrinthine Removal of Vestibular Schwannoma
Katsumi Doi*,Ko SHiraishi, Takeshi Fujita, Takamitsu Kobayashi, Mitsuo Sato, Kazuya Saito, Toru Seo, Kumi Kohama and Daisuke Nagatomi
Department of Otolaryngology, Kindai University School of Medicine, Japan
*Corresponding author: Katsumi Doi, Department of Otolaryngology, Kindai University, 377-2 Oono-Higashi, Osaka-Sayama, Osaka 589-8511, Japan
Published: 08 Dec, 2016
Cite this article as: Doi K, SHiraishi K, Fujita T, Kobayashi
T, Sato M, Saito K, et al. Simultaneous
Cochlear Implantation with
Translabyrinthine Removal of Vestibular
Schwannoma. Clin Surg. 2016; 1: 1241.
Abstract
Decision making in patients with a vestibular schwannoma (VS) in the only hearing ear is challenging. Restoration of hearing when they become deaf will depend on the status of the remaining cochlear
and the integrity and function of the cochlear nerve. In terms of hearing restoration, cochlear
implantation (CI) is the most effective option if the cochlear nerve could be preserved intact and the
cochlea could be remained responsive to electrical stimulation. Auditory Brainstem Implantation
(ABI) would be another option for the patients in which the cochlear nerve could not be spared
during VS removal, while the hearing results with ABI are still far poor than those with CI. If CI
is being considered, it should be performed near the time of the surgery for VS removal, because
cochlear fibrosis and/or ossification might occur in a short time after the surgery. When the
translabyrinthine surgery (TLS) for VS removal is selected, CI surgery should be completed as close
as possible to the procedure.
Simultaneous CI with TLS removal of VS was considered for the patient who suffered from a severe
sensorineural hearing loss on the same side with VS and a profound deafness on the opposite side
due to the past idiopathic sudden deafness. The first CI was preceded on the opposite side, and the
second CI was performed on the tumor side one year after. Simultaneous CI with TLS VS removal
is a good option that should be considered when discussing and planning the most appropriate
strategy.
Introduction
Hearing preservation is often difficult to achieve despite treatment of VS removal with surgery
even with hearing preservation techniques are employed [1]. Therefore, the resection of VS for
the patients with only hearing or better hearing on the tumor side ear is still controversial. In
profoundly deaf patients or patients where treatment is likely to cause severe hearing deterioration,
cochlear implantation (CI) or auditory brainstem implantation (ABI) provide the best two options
for hearing outcomes [1-3]. CI surgery may be of benefit if the cochlear nerve could be preserved
after tumor removal, while ABI should be considered if the cochlear nerve preservation would not
be predicted. Some authors reported that VS removal with simultaneous CI is another option for
those cases and the hearing results with CI were shown to be excellent mostly [1-5] .
We present a case in which L-CI was firstly performed on the opposite side, and then R-VS
removal surgery via translabyrinthine approach with simultaneous R-CI on the tumor side was
conducted one year later.
Case Presentation
A 50-year-old woman presented in our hospital suffering from sudden onset hearing loss on the
left ear in 2005. A pure tone audiogram showed 91.7 dB SNHL on the left side and 36.7 dB SNHL on
the right. Despite conservative treatments, her left hearing did not recovered.MRI scan revealed VS
on the right side, which might cause R-SNHL.
Follow-up with MRI scans and PTA evaluations confirmed that the tumor continued to grow
up to 16.1 mm x 8.6 mm x 9.2 mm (Figure 1A) and the hearing deterioration in the right ear became
worsened (Figure1B).Finally, she could not communicate even with R-HA (hearing aid; HA) in her
daily life in 2012.
CI Surgery in the Left Ear
As the first stage, CI was performed on the left side with the round window approach (RWA)
in 2012 (Figure 2A). Neural Telemetry test (NRT) showed good
responses at all electrode arrays and dexamethasone was administered
intra- and post-operatively for preservation of both hearing and
vestibular functions. Free-field PTA with L-CI is stable around 30 dB
after 3 months (Figure 2A). Speech discrimination test on the left side
showed 45% correct in sentences at 6 months after the surgery, while
that on the tumor side further deteriorated (Figure 2B). She became
to be able to communicate even only with L-CI. The caloric test after
the surgery indicated good preservation of the vestibular function in
the left ear (Figure 2B).
CI Surgery in the Right Ear
As the second stage, translabyrinthine removal of VS with
simultaneous CI surgery on the tumor side was performed in 2013
(Figure 3A). The tumor was totally removed, while anatomical
preservation of the cochlear nerve was confirmed. Full and smooth
insertion of the electrode arrays was done again via RWM. NRT
test showed poor but positive responses at a few electrodes.
Dexamethasone was again used to preserve the cochlear function
as the same manner. No peri- and post-operative complication was
noted.
Speech test in the right ear showed 15% correct in sentences at
6 months after the surgery and it had continued to improve up to
36% correct in words and 46% correct in sentences at 1 year after the
surgery. Free-field PTA with CI is stable at 30-40 dB on both sides
(Figure 3B). NRT responses were successfully detected more than 10
electrodes on the tumor side with R-CI, and it remained stable on the
opposite side thereafter.
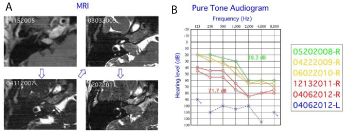
Figure 1
Figure 1
Figure 1A: MRI scans demonstrated relative rapid tumor growth.
Figure 1B: PTA indicated a profound deafness in the left ear and a progressive hearing deterioration in the right ear.
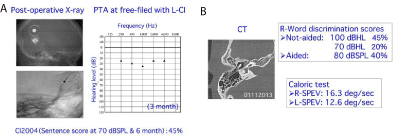
Figure 2
Figure 2
Figure 2A: CI surgery was successfully completed on the left side and free-field PTA was stable after 3 months.
Figure 2B: Speech discrimination test on the tumor side further deteriorated, while the caloric test showed positive responses on both sides.
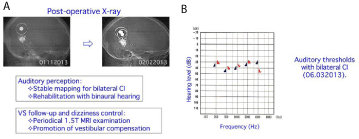
Figure 3
Figure 3
Figure 3A: Second CI was simultaneously performed with TLS tumor removal. Auditory rehabilitations and MRI and CT scans have been conducted.
Figure 3B: Free-field PTA was stable around 30-40 dB on both sides.
Discussion
The natural history of vestibular schwannoma (VS) leads to
profound deafness that is one of the most important predictors of
quality of life [1,2]. Therefore, the optimal hearing preservation is one
of the priorities in management of VS. The traditional approach has
been to wait for hearing loss before surgery to preserve function for
as long as possible. While this might allow continuous tumor growth,
increase the risk of surgery and should lost a chance of preservation of
hearing as well as the cochlear nerve. In such cases, auditory brainstem
implantation (ABI) would be adopted, however, hearing outcomes
using ABI are known to be usually poor [1-3]. Another option is early
intervention to remove the tumor while small. This should reduce the
risk of surgery, and offer the opportunity to attempt for preservation
of the cochlear nerve as well as good hearing outcomes with cochlear
implantation (CI) [1-5].
The present study demonstrates that it is possible to remove
the tumor completely, preserve the cochlear nerve, and successfully
restore hearing with CI in the operated ear. According to this strategy,
translabyrinthine surgery (TLS) should be favorable, because with
this approach the entire length of the cochlear nerve is visualized
from the fundus of internal auditory canal (IAC) to the brainstem,
therefore, the procedure should avoid unvisualized manipulation of
the cochlear nerve [1-5]. The previous reports suggest that the tumor
size of cerebellopontine angle (CPA) should be 10 mm or less for the
cochlear nerve preservation with TLS as the cochlear nerve is difficult
to preserve beyond this size [1,2]. TLS with CI should be considered
if the tumor is growing and the hearing is unserviceable or becoming
worse. The same strategy should be considered to prevent the tumor
extension deep into the cochlea if the small intralabyrinthine VS were
found. In some cases, just like ABI, CI implanted on the operated side
might serve as the sleeper until the hearing loss on the opposite side
became unserviceable due to some pathology such as VS, idiopathic
sensorineural hearing loss, presbyacusis, and Meniere’s disease [1,2].
On the contrary, CI implanted on the opposite side might also serve
as the sleeper or the reservoir even after the hearing on the tumor
side would be gradually worse or lost as the result of surgery. In our
case, the CPA component of the tumor was still within 10 mm, while
the tumor continued to grow up relative rapidly. The hearing level
on the opposite side was already profoundly deaf, and the hearing
deterioration on the tumor side was becoming more apparent
There is a rapid accumulation of the evidence that the outcomes
with ABI are much more variable than with CI, and CI after TLS
could be much more successful, with hearing outcomes similar to
the best postlingual ordinary CI adult cases [1-3]. According to the
peer-reviewed literatures, the relative high scores (at least more than
50%) in the open-set speech discrimination were confirmed among
the patients who have undertaken TLS with CI [2,3,5]. One factor
associated with poor outcomes would be absence of hearing sensation
on pre- & post-operative promontory stimulation testing and/or
intra-operative electrical auditory brainstem responses (eABR), ABR,
and the cochlear nerve compound action potential (CNAP). A good
quality eABR and CNAP is a reasonable indicator of good outcomes,
while a poor responses is less predicative of poor outcomes [1,2].
In our case, intra-operative neural telemetry testing (NRT) after
insertion of the electrode arrays into the cochlea was performed to
monitor the function of the cochlear nerve on both sides during the
surgery. We could detect excellent NRT responses on the opposite
side and poor but positive responses at least at some electrodes even
after total removal of the tumor, indicating the preservation of the
cochlear nerve even on the tumor side. We sometimes experience
poor NRT responses even during the ordinary CI surgery, presumably
due to functional changes of the cochlear nerve, too. However, these
functional changes would be temporal and reversible in most cases,
because we usually could get vivid NRT responses after initiation of
CI system even in those cases, just as in our case.
Another factor associated poor outcomes with CI should be a
delay in CI surgery after tumor removal, which may result in cochlear
fibrosis and/or ossification [1-5]. It is well recognized that TLS is
highly destructive method and cochlear fibrosis and/or ossification
might occur in a relative short time. The delay in decision making
of CI insertion would allow total fibrosis and/or ossification which
means CI placement might be no longer possible. In our case,
simultaneous CI surgery with TLS was performed where full insertion
of the electrode arrays was completed without any difficulties, resulted
in successful hearing outcomes.
Today, we have two options for the hearing preservation in
VS surgery, one is CI and another one is ABI [1-5]. Even though
CI requires the preservation of the cochlear nerve after the tumor
removal, hearing outcomes seem better with CI than with ABI.
Whether CI or ABI was implanted, an important issue is the necessity
of follow-up with MRI test in all VS cases. The patients are known
to have potential risks such as device failure, device and magnet
displacements, and local heating during the MRI scans [1,2]. The
progress in devices of both CI and AB now makes it possible to
have 1.5 T MRI safely, although there should be some precautions
such as the use of a compression bandage over the implant [1,2].
Combination of MRI with high-resolution computed tomography
(CT) scans would be of benefit and also recommended.
Conclusion
Decision making in patients with VS in the only hearing ear is challenging. Restoration of hearing when they become deaf will depend on the status of the remaining cochlear and the integrity and function of the cochlear nerve. In terms of hearing restoration, CI is the most effective option if the cochlear nerve could be preserved intact and the cochlea could be remained responsive to electrical stimulation. ABI would be another option for the patients in which the cochlear nerve could not be spared during VS removal, while the hearing results with an ABI are still far poor than those with a CI. If CI is being considered, it should be performed near the time of the surgery for VS removal, because cochlear fibrosis and/or ossification in the cochlea might occur in a short time after the surgery. When the TLS for tumor removal is selected, CI surgery should be done as close as possible to the procedure.
References
- Tysome JR, Axon PR, Donnelly NP, Evans DG, Ferner RE, O’Connor AFF, et al. English consensus protocol evaluating candidacy for auditory brainstem and cochlear implantation in neurofibromatosis type 2. Otol & Neurotol. 2013; 34: 1743-1747.
- SKW Lloyd, Glynn FJ, Rutherford SA, King AT, Mawman DJ, O'Driscoll MP, et al. Ipsilateral cochlear implantation after cochlear nerve preservation vestibular schwannoma surgery in patients with neurofibromatosis type 2. Otol & Neurotol. 2013; 35: 43-51.
- Ozdek A, Bayir O, Donmez T, Ozisik P, Safin M, Tulgar M, et al. Hearing restoration in NF2 patients and patients with vestibular schwannoma in the only hearing ear. Report of two cases. Am J Otolaryngol. 2014; 35: 538- 541.
- Schutt CA, Kventon JF. Cochlear implantation after resection of an intralabyrinthine schwannoma. Am J Otolaryngol. 2014; 35: 257-260.
- Di-Lella F, Merkus P, Di-Trapani G, Taibah A, Guida M, Sanna M, et al. Vestibular schwannoma in the only hearing ear: role of cochlear implants. Ann Otol Rhinol Laryngol. 2013; 122: 91-99.